The Troubling Reason I Obsessively Researched My Pregnancy

A pregnant woman in her third trimester.
At the end of my second trimester of pregnancy, I answered a call from an unknown number.
To be pregnant is to exist on a never-ending receiving line of advice, whether we want it or not.
"I know your due date is approaching," said a stranger at the other end of the line, completely freaking me out. She identified herself as being from Natera, a company that my doctor had used for genetic testing I had consented to months ago.
"Excuse me?" I said.
"Have you considered cord-blood banking?" she said.
"No, I'm not doing that," I said. I had read enough about cord-blood banking, the process of saving stem cell-containing blood from your baby's umbilical cord, to understand that my family was in the vast majority of those that would with extremely high likelihood derive no medical benefit from it. Of course, in the societally sanctioned spending spree that accompanies new parenthood, plenty of companies are happy to charge anyone hundreds if not thousands of dollars plus annual storage fees to collect and manage your cord blood.
"Why not? Have you considered all the bene—"
"I'm not doing it and I don't want to explain my decision," I said before hanging up. I would later learn I neglected to check a miniscule box on my testing consent forms at the doctor to opt out of solicitations. Still, I was angry that I was being telemarketed unnecessary and costly medical services by someone who had been trained to immediately call my judgment into question. I was annoyed that my doctor's office would allow such intrusions at all. When I asked my OB about it at my next visit, she told me there's no way Natera would have gotten my information from them. Apparently even she didn't realize what was on those forms.
The incident with Natera did nothing to heighten my trust of the medical establishment during my pregnancy. I was hardly alone. Almost every mom I knew had expressed a similar sentiment.
"I don't trust doctors," read the text of a loved one when I told her I would probably get an epidural after my doctor recommended getting one because, she said, it can help relax the pelvic muscles during labor. But this friend, a highly educated woman who had had done her research and had two unmedicated births, believed firmly otherwise. "Look it up," she said. Thus commenced more of the furious Googling I found myself doing multiple times a day since deciding I wanted to become pregnant.
To be pregnant is to exist on a never-ending receiving line of advice, whether we want it or not. Information presents to us from Google's never-out-of-reach search bar, friends and family eager to use our pregnancies as an excuse to recall their own, and the doctor's office, where the wisdom of medical professionals neatly comingles with brochures and free samples from myriad companies that would really, really like our business as new moms. Separating the "good" advice from the rest is a Herculean task that many pregnant women manage only with vigorous fact-finding missions of their own.
The medical community in America is poorly equipped to help women navigate the enormous pressures that come with birth and transitioning to motherhood.
Doing my research during pregnancy felt like a defense against the scary unknowns, overabundance of opinions, and disturbing marketing schemes that come with entering parenthood. The medical community in America is poorly equipped to help women navigate the enormous emotional and societal pressures that come with birth and transitioning to motherhood. Too much of what pregnant women experience at the doctor has to do with dated ideas about our care, mandated by tradition or a fear of being sued rather than medical necessity. These practices, like weigh-ins at every appointment or medically unnecessary C-sections (which are estimated to account, horrifically, for almost 50 percent of all C-sections performed in the U.S.), only heighten anxiety.
Meanwhile, things that might alleviate stress – like having thorough discussions about the kinds of interventions we might be asked to accept at the hospital during labor and delivery – are left to outside educators and doulas that insurance plans typically don't cover. The net effect isn't better health outcomes for mom and baby, but rather a normalized sense of distrust many American women feel toward their OBGYNs, and the burden of going to every appointment and the delivery room on the defensive. Instead of being wed to dated medical practices and tangled in America's new motherhood industrial complex, shouldn't our doctors, of all people, be our biggest advocates?
As soon as I found out I was pregnant, I devoured Expecting Better, by Emily Oster, an economist who embarked on her own fact-finding mission during her first pregnancy, predicated on the belief that the advice OBGYNs have been giving pregnant women for decades is out of date and unnecessarily restrictive. The book includes controversial stances, like that having small amounts of alcohol while pregnant is OK. (More recent research has called this view into question.) Oster writes that for the vast majority of pregnant women, it's perfectly fine to lie on your back, do sit-ups, and eat Brie — all things I was relieved to learn I wouldn't have to give up for nine months, despite the traditional advice, which my doctor also gave to me.
Oster recommends hiring a doula, based both on research and personal experience. It's a worthwhile investment for those who can afford it: according to one study, 20.4 percent of laboring women with doulas had C-sections compared with 34.2 percent of women without them. A doula can do many things for a pregnant client, including helping her write a birth plan, massaging her back in labor, and cheering her on, which is especially useful for women who plan to labor without pain medication. Use of doulas is on the rise; according to DONA International, the world's largest and oldest doula association, the number of doulas who have been certified to date is over 12,000, up from 2,000 in 2002.
But the most significant role a doula plays is that of patient advocate in the hospital. This is a profound commentary on the way the medical establishment handles childbirth, a medical event that 86 percent of women aged 40 to 44 had gone through as of 2016. Recognizing the maternal mortality crisis in the U.S., where women are far more likely to die as a result of childbirth than anywhere else in the developed world and black women are three times more likely to die in childbirth than white women, a few states now allow Medicaid to cover doulas. Can you imagine feeling the need to hire an independent non-medical care provider to help you run interference with your doctors and nurses for something like an appendectomy?
I wouldn't have been aware of all the imminent interventions during my labor if my doula hadn't told me about them. Things happen fast in the hospital and doctors and nurses may rush patients to consent before proceeding with things like breaking their water or hooking them up to an IV of Pitocin. Only because my husband and I had spent six hours in birth class — a suggestion by my doula — did I realize that I was empowered to say "no" to such procedures.
Expecting more trustworthy advice to come from my doctor than books or Google or even a doula hardly seems unreasonable.
Of course, we all feel immense pressure to become good parents, and questioning conventional medical wisdom is a natural response to that pressure. "Looking around at the world and saying, who am I as a parent? What is important to me? Who are the wise people? What do I think wisdom is? What is a good decision? If you're a certain type of introspective person, if you're really asking those questions, that's going to include like taking a second look at things that doctors, for example, say," says Koyuki Smith, a doula and birth educator.
Expecting more trustworthy advice to come from my doctor than books or Google or even a doula hardly seems unreasonable. Yet my doctor's office seemed more concerned with checking off a list of boxes rather than providing me with personalized care that might have relieved my understandable anxiety about my first birth. When I still hadn't gone into labor around the time of my due date, my doctor encouraged me to be induced because my baby appeared to be large. I declined but scheduled an induction to "hold my spot" around the 42-week mark.
When I asked what medication would be used for an induction if I had one and she said Cytotec, I told her I had read that drug could cause serious complications, but she dismissed my concerns after I told her they stemmed from a book I read on natural childbirth. The FDA's page on Cytotec isn't exactly reassuring.
The nurse who took me in triage after I went into labor a week past my due date practically scolded me for waiting to go into labor naturally instead of opting for induction sooner. My doula told her while I was struggling to speak through labor pains to get off my case about it. I hadn't even become a mom and I was already doing so many things "wrong." Because I had done my own reading, I felt confident that my choices weren't harming my baby or me.
Becoming a mom would be less daunting if the medical community found a way to help women navigate the pressures of motherhood instead of adding to them. "Our culture at large doesn't support women enough in the complicated emotions that are a part of this process," said Alexandra Saks, a reproductive psychologist and author of What No One Tells You: A Guide to Your Emotions From Pregnancy to Motherhood. "I hope that every practitioner that works with women around reproductive health prioritizes her emotions around her experience."
For many of us, that will mean doctors who help us understand the pros and cons of conventional advice, don't use their offices as marketing channels, and don't pressure women into medically unnecessary inductions. Moms should also receive more attention after delivery both in the hospital and after they get home; a single, quick postpartum visit at six weeks is not an adequate way to care for women recovering from the trauma of childbirth, nor is it an adequate way to ensure women are emotionally supported during the transition. While several people interrogated me about my mental health at the hospital and my doctor's office just before and after birth, if I had been concerned about postpartum depression, I can't imagine feeling comfortable enough in those moments to tell strangers filling out obligatory worksheets.
It also means figuring out how to talk to patients who are prone to Googling their pregnancies with gusto every single day. It would be impossible for many women to shun independent research during pregnancy altogether. But it would also be nice if our doctors didn't add to our impulse to do it.
Urinary tract infections account for more than 8 million trips to the doctor each year.
Few things are more painful than a urinary tract infection (UTI). Common in men and women, these infections account for more than 8 million trips to the doctor each year and can cause an array of uncomfortable symptoms, from a burning feeling during urination to fever, vomiting, and chills. For an unlucky few, UTIs can be chronic—meaning that, despite treatment, they just keep coming back.
But new research, presented at the European Association of Urology (EAU) Congress in Paris this week, brings some hope to people who suffer from UTIs.
Clinicians from the Royal Berkshire Hospital presented the results of a long-term, nine-year clinical trial where 89 men and women who suffered from recurrent UTIs were given an oral vaccine called MV140, designed to prevent the infections. Every day for three months, the participants were given two sprays of the vaccine (flavored to taste like pineapple) and then followed over the course of nine years. Clinicians analyzed medical records and asked the study participants about symptoms to check whether any experienced UTIs or had any adverse reactions from taking the vaccine.
The results showed that across nine years, 48 of the participants (about 54%) remained completely infection-free. On average, the study participants remained infection free for 54.7 months—four and a half years.
“While we need to be pragmatic, this vaccine is a potential breakthrough in preventing UTIs and could offer a safe and effective alternative to conventional treatments,” said Gernot Bonita, Professor of Urology at the Alta Bro Medical Centre for Urology in Switzerland, who is also the EAU Chairman of Guidelines on Urological Infections.
The news comes as a relief not only for people who suffer chronic UTIs, but also to doctors who have seen an uptick in antibiotic-resistant UTIs in the past several years. Because UTIs usually require antibiotics, patients run the risk of developing a resistance to the antibiotics, making infections more difficult to treat. A preventative vaccine could mean less infections, less antibiotics, and less drug resistance overall.
“Many of our participants told us that having the vaccine restored their quality of life,” said Dr. Bob Yang, Consultant Urologist at the Royal Berkshire NHS Foundation Trust, who helped lead the research. “While we’re yet to look at the effect of this vaccine in different patient groups, this follow-up data suggests it could be a game-changer for UTI prevention if it’s offered widely, reducing the need for antibiotic treatments.”
MILESTONE: Doctors have transplanted a pig organ into a human for the first time in history
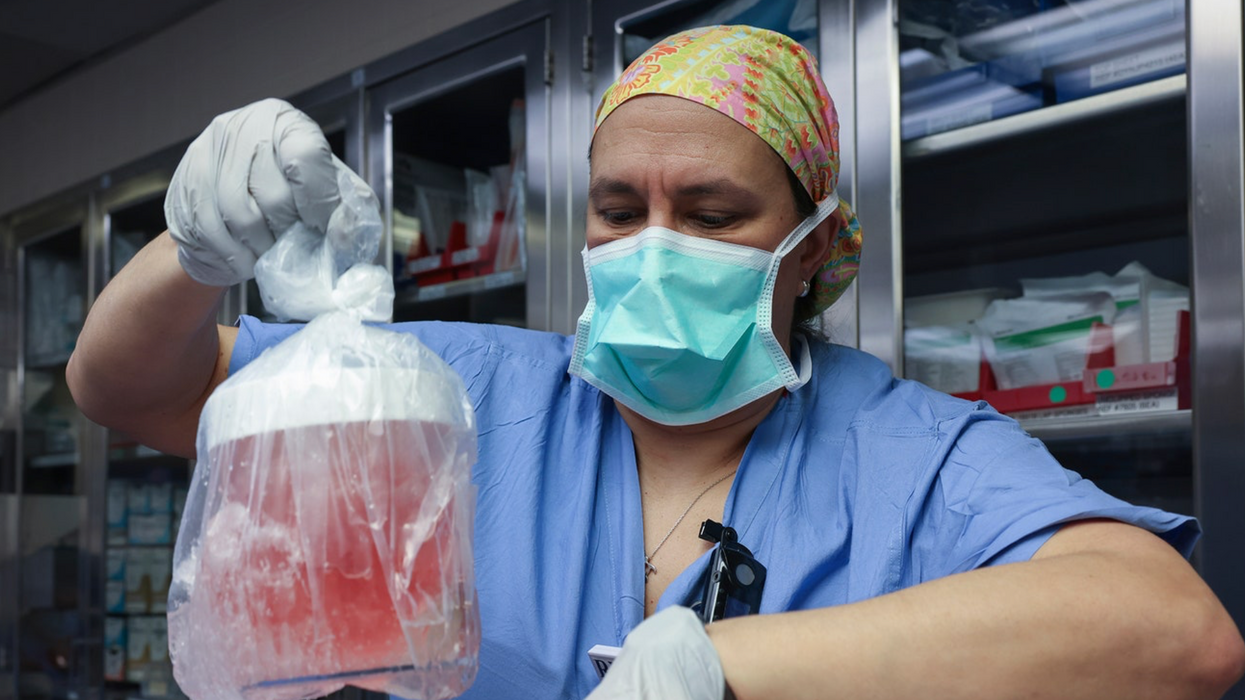
A surgeon at Massachusetts General Hospital prepares a pig organ for transplant.
Surgeons at Massachusetts General Hospital made history last week when they successfully transplanted a pig kidney into a human patient for the first time ever.
The recipient was a 62-year-old man named Richard Slayman who had been living with end-stage kidney disease caused by diabetes. While Slayman had received a kidney transplant in 2018 from a human donor, his diabetes ultimately caused the kidney to fail less than five years after the transplant. Slayman had undergone dialysis ever since—a procedure that uses an artificial kidney to remove waste products from a person’s blood when the kidneys are unable to—but the dialysis frequently caused blood clots and other complications that landed him in the hospital multiple times.
As a last resort, Slayman’s kidney specialist suggested a transplant using a pig kidney provided by eGenesis, a pharmaceutical company based in Cambridge, Mass. The highly experimental surgery was made possible with the Food and Drug Administration’s “compassionate use” initiative, which allows patients with life-threatening medical conditions access to experimental treatments.
The new frontier of organ donation
Like Slayman, more than 100,000 people are currently on the national organ transplant waiting list, and roughly 17 people die every day waiting for an available organ. To make up for the shortage of human organs, scientists have been experimenting for the past several decades with using organs from animals such as pigs—a new field of medicine known as xenotransplantation. But putting an animal organ into a human body is much more complicated than it might appear, experts say.
“The human immune system reacts incredibly violently to a pig organ, much more so than a human organ,” said Dr. Joren Madsen, director of the Mass General Transplant Center. Even with immunosuppressant drugs that suppress the body’s ability to reject the transplant organ, Madsen said, a human body would reject an animal organ “within minutes.”
So scientists have had to use gene-editing technology to change the animal organs so that they would work inside a human body. The pig kidney in Slayman’s surgery, for instance, had been genetically altered using CRISPR-Cas9 technology to remove harmful pig genes and add human ones. The kidney was also edited to remove pig viruses that could potentially infect a human after transplant.
With CRISPR technology, scientists have been able to prove that interspecies organ transplants are not only possible, but may be able to successfully work long term, too. In the past several years, scientists were able to transplant a pig kidney into a monkey and have the monkey survive for more than two years. More recently, doctors have transplanted pig hearts into human beings—though each recipient of a pig heart only managed to live a couple of months after the transplant. In one of the patients, researchers noted evidence of a pig virus in the man’s heart that had not been identified before the surgery and could be a possible explanation for his heart failure.
So far, so good
Slayman and his medical team ultimately decided to pursue the surgery—and the risk paid off. When the pig organ started producing urine at the end of the four-hour surgery, the entire operating room erupted in applause.
Slayman is currently receiving an infusion of immunosuppressant drugs to prevent the kidney from being rejected, while his doctors monitor the kidney’s function with frequent ultrasounds. Slayman is reported to be “recovering well” at Massachusetts General Hospital and is expected to be discharged within the next several days.