In 2010, a 67-year-old former executive assistant for a Fortune 500 company was diagnosed with mild cognitive impairment. By 2014, her doctors confirmed she had Alzheimer's disease.
As her disease progressed, she continued to live independently but wasn't able to drive anymore. Today, she can manage most of her everyday tasks, but her two daughters are considering a live-in caregiver. Despite her condition, the woman may represent a beacon of hope for the approximately 44 million people worldwide living with Alzheimer's disease. The now 74-year-old is among a small cadre of Alzheimer's patients who have undergone an experimental ultrasound procedure aimed at slowing cognitive decline.
In November 2020, Elisa Konofagou, a professor of biomedical engineering and director of the Ultrasound and Elasticity Imaging Laboratory at Columbia University, and her team used ultrasound to noninvasively open the woman's blood-brain barrier. This barrier is a highly selective membrane of cells that prevents toxins and pathogens from entering the brain while allowing vital nutrients to pass through. This regulatory function means the blood-brain barrier filters out most drugs, making treating Alzheimer's and other brain diseases a challenge.
Ultrasound uses high-frequency sound waves to produce live images from the inside of the human body. But scientists think it could also be used to boost the effectiveness of Alzheimer's drugs, or potentially even improve brain function in dementia patients without the use of drugs.
The procedure, which involves a portable ultrasound system, is the culmination of 17 years of lab work. As part of a small clinical trial, scientists positioned a sensor transmitting ultrasound waves on top of the woman's head while she sat in a chair. The sensor sends ultrasound pulses throughout the target region. Meanwhile, investigators intravenously infused microbubbles into the woman to boost the effects of the ultrasound. Three days after the procedure, scientists scanned her brain so that they could measure the effects of the treatments. Five months later, they took more images of her brain to see if the effects of the treatment lasted.
Promising Signs
After the first brain scan, Konofagou and her team found that amyloid-beta, the protein that clumps together in the brains of Alzheimer's patients and disrupts cell function, had declined by 14%. At the woman's second scan, amyloid levels were still lower than before the experimental treatment, but only by 10% this time. Konofagou thinks repeat ultrasound treatments given early on in the development of Alzheimer's may have the best chance at keeping amyloid plaques at bay.
This reduction in amyloid appeared to halt the woman's cognitive decline, at least temporarily. Following the ultrasound treatment, the woman took a 30-point test used to measure cognitive impairment in Alzheimer's. Her score — 22, indicating mild cognitive impairment — remained the same as before the intervention. Konofagou says this was actually a good sign.
"Typically, every six months an Alzheimer's patient scores two to three points lower, so this is highly encouraging," she says.
Konofagou speculates that the results might have been even more impressive had they applied the ultrasound on a larger section of the brain at a higher frequency. The selected site was just 4 cubic centimeters. Current safety protocols set by the U.S. Food and Drug Administration stipulate that investigators conducting such trials only treat one brain region with the lowest pressure possible.
The Columbia trial is aided by microbubble technology. During the procedure, investigators infused tiny, gas-filled spheres into the woman's veins to enhance the ultrasound reflection of the sound waves.
The big promise of ultrasound is that it could eventually make drugs for Alzheimer's obsolete.
"Ultrasound with microbubbles wakes up immune cells that go on to discard amyloid-beta," Konofagou says. "In this way, we can recover the function of brain neurons, which are destroyed by Alzheimer's in a sort of domino effect." What's more, a drug delivered alongside ultrasound can penetrate the brain at a dose up to 10 times higher.
Costas Arvanitis, an assistant professor at Georgia Institute of Technology who studies ultrasonic biophysics and isn't involved in the Columbia trial, is excited about the research. "First, by applying ultrasound you can make larger drugs — picture an antibody — available to the brain," he says. Then, you can use ultrasound to improve the therapeutic index, or the ratio of the effectiveness of a drug versus the ratio of adverse effects. "Some drugs might be effective but because we have to provide them in high doses to see significant responses they tend to come with side effects. By improving locally the concentration of a drug, you open up the possibility to reduce the dose."
The Columbia trial will enroll just six patients and is designed to test the feasibility and safety of the approach, not its efficacy. Still, Arvantis is hopeful about the potential benefits of the technique. "The technology has already been demonstrated to be safe, its components are now tuned to the needs of this specific application, and it's safe to say it's only a matter of time before we are able to develop personalized treatments," he says.
Konofagou and her colleagues recently presented their findings at the 20th Annual International Symposium for Therapeutic Ultrasound and intend to publish them in a scientific journal later this year. They plan to recruit more participants for larger trials, which will determine how effective the therapy is at improving memory and brain function in Alzheimer's patients. They're also in talks with pharmaceutical companies about ways to use their therapeutic approach to improve current drugs or even "create new drugs," says Konofagou.
A New Treatment Approach
On June 7, the FDA approved the first Alzheimer's disease drug in nearly two decades. Aducanumab, a drug developed by Biogen, is an antibody designed to target and reduce amyloid plaques. The drug has already sparked immense enthusiasm — and controversy. Proponents say the drug is a much-needed start in the fight against the disease, but others argue that the drug doesn't substantially improve cognition. They say the approval could open the door to the FDA greenlighting more Alzheimer's drugs that don't have a clear benefit, giving false hope to both patients and their families.
Konofagou's ultrasound approach could potentially boost the effects of drugs like aducanumab. "Our technique can be seamlessly combined with aducanumab in early Alzheimer's, where it has shown the most promise, to further enhance both its amyloid load reduction and further reduce cognitive deficits while using exactly the same drug regimen otherwise," she says. For the Columbia team, the goal is to use ultrasound to maximize the effects of aducanumab, as they've done with other drugs in animal studies.
But Konofagou's approach could transcend drug controversies, and even drugs altogether. The big promise of ultrasound is that it could eventually make drugs for Alzheimer's obsolete.
"There are already indications that the immune system is alerted each time ultrasound is exerted on the brain or when the brain barrier is being penetrated and gets activated, which on its own may have sufficient therapeutic effects," says Konofagou. Her team is now working with psychiatrists in hopes of using brain stimulation to treat patients with depression.
The potential to modulate the brain without drugs is huge and untapped, says Kim Butts Pauly, a professor of radiology, electrical engineering and bioengineering at Stanford University, who's not involved in the Columbia study. But she admits that scientists don't know how to fully control ultrasound in the brain yet. "We're only at the starting point of getting the tools to understand and harness how ultrasound microbubbles stimulate an immune response in the brain."
Meanwhile, the 74-year-old woman who received the ultrasound treatment last year, goes on about her life, having "both good days and bad days," her youngest daughter says. COVID-19's isolation took a toll on her, but both she and her daughters remain grateful for the opportunity to participate in the ultrasound trial.
"My mother wants to help, if not for herself, then for those who will follow her," the daughter says. She hopes her mother will be able to join the next phase of the trial, which will involve a drug in conjunction with the ultrasound treatment. "This may be the combination where the magic will happen," her daughter says.
Artificial Wombs Are Getting Closer to Reality for Premature Babies
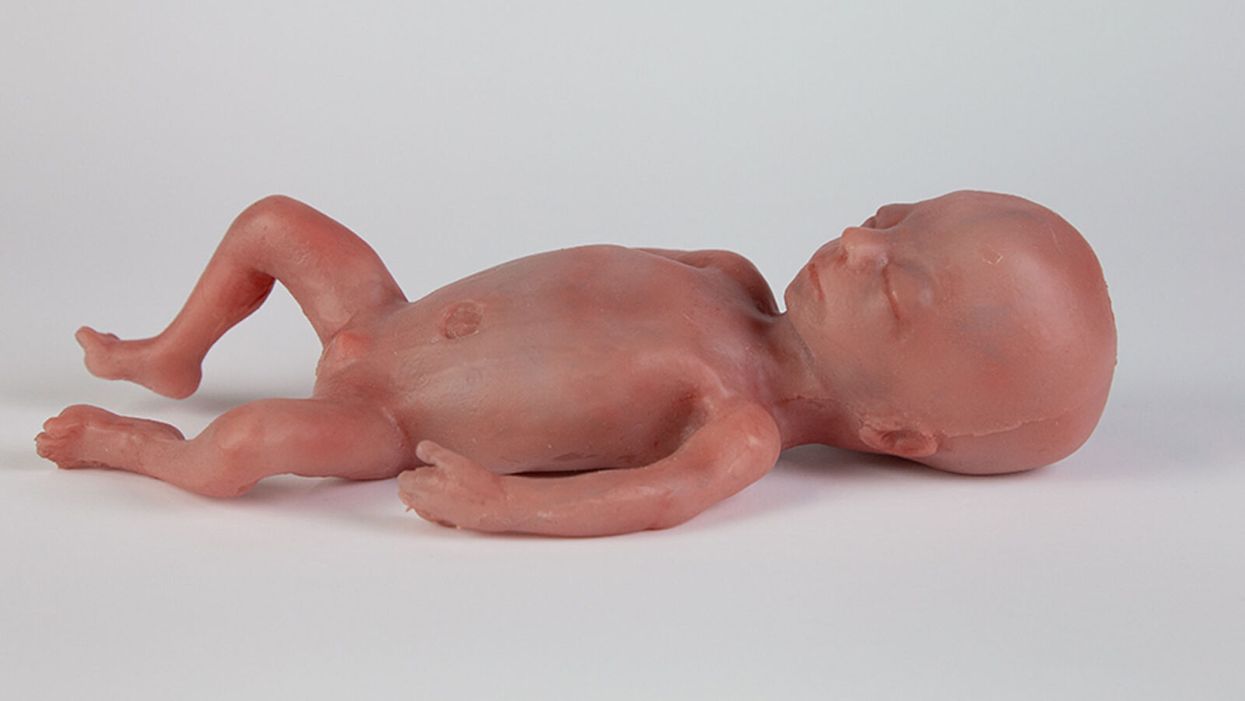
A mannequin of a 24-week-old fetus replicated from MR imaging. Created by: Juliette van Haren, Mark Thielen, Jasper Sterk, Chet Bangaru, and Frank Delbressine, Department of Industrial Design, Eindhoven University of Technology.
In 2017, researchers at the Children's Hospital of Philadelphia grew extremely preterm lambs from hairless to fluffy inside a "biobag," a dark, fluid-filled bag designed to mimic a mother's womb.
"There could be quite a lot of infants that would benefit from artificial womb technologies."
This happened over the course of a month, across a delicate period of fetal development that scientists consider the "edge of viability" for survival at birth.
In 2019, Australian and Japanese scientists repeated the success of keeping extremely premature lambs inside an artificial womb environment until they were ready to survive on their own. Those researchers are now developing a treatment strategy for infants born at "the hard limit of viability," between 20 and 23 weeks of gestation. At the same time, Dutch researchers are going so far as to replicate the sound of a mother's heartbeat inside a biobag. These developments signal exciting times ahead--with a touch of science fiction--for artificial womb technologies. But is there a catch?
"There could be quite a lot of infants that would benefit from artificial womb technologies," says Josephine Johnston, a bioethicist and lawyer at The Hastings Center, an independent bioethics research institute in New York. "These technologies can decrease morbidity and mortality for infants at the edge of viability and help them survive without significant damage to the lungs or other problems," she says.
It is a viewpoint shared by Frans van de Vosse, leader of the Cardiovascular Biomechanics research group at Eindhoven University of Technology in the Netherlands. He participates in a university project that recently received more than $3 million in funding from the E.U. to produce a prototype artificial womb for preterm babies between 24 and 28 weeks of gestation by 2024.
The Eindhoven design comes with a fluid-based environment, just like that of the natural womb, where the baby receives oxygen and nutrients through an artificial placenta that is connected to the baby's umbilical cord. "With current incubators, when a respiratory device delivers oxygen into the lungs in order for the baby to breathe, you may harm preterm babies because their lungs are not yet mature for that," says van de Vosse. "But when the lungs are under water, then they can develop, they can mature, and the baby will receive the oxygen through the umbilical cord, just like in the natural womb," he says.
His research team is working to achieve the "perfectly natural" artificial womb based on strict mathematical models and calculations, van de Vosse says. They are even employing 3D printing technology to develop the wombs and artificial babies to test in them--the mannequins, as van de Vosse calls them. These mannequins are being outfitted with sensors that can replicate the environment a fetus experiences inside a mother's womb, including the soothing sound of her heartbeat.
"The Dutch study's artificial womb design is slightly different from everything else we have seen as it encourages a gestateling to experience the kind of intimacy that a fetus does in pregnancy," says Elizabeth Chloe Romanis, an assistant professor in biolaw at Durham Law School in the U.K. But what is a "gestateling" anyway? It's a term Romanis has coined to describe neither a fetus nor a newborn, but an in-between artificial stage.
"Because they aren't born, they are not neonates," Romanis explains. "But also, they are not inside a pregnant person's body, so they are not fetuses. In an artificial womb the fetus is still gestating, hence why I call it gestateling."
The terminology is not just a semantic exercise to lend a name to what medical dictionaries haven't yet defined. "Gestatelings might have a slightly different psychology," says Romanis. "A fetus inside a mother's womb interacts with the mother. A neonate has some kind of self-sufficiency in terms of physiology. But the gestateling doesn't do either of those things," she says, urging us to be mindful of the still-obscure effects that experiencing early life as a gestateling might have on future humans. Psychology aside, there are also legal repercussions.
The Universal Declaration of Human Rights proclaims the "inalienable rights which everyone is entitled to as a human being," with "everyone" including neonates. However, such a legal umbrella is absent when it comes to fetuses, which have no rights under the same declaration. "We might need a new legal category for a gestateling," concludes Romanis.
But not everyone agrees. "However well-meaning, a new legal category would almost certainly be used to further erode the legality of abortion in countries like the U.S.," says Johnston.
The "abortion war" in the U.S. has risen to a crescendo since 2019, when states like Missouri, Mississippi, Kentucky, Louisiana and Georgia passed so-called "fetal heartbeat bills," which render an abortion illegal once a fetal heartbeat is detected. The situation is only bound to intensify now that Justice Ruth Bader Ginsburg, one of the Supreme Court's fiercest champions for abortion rights, has passed away. If President Trump appoints Ginsburg's replacement, he will probably grant conservatives on the Court the votes needed to revoke or weaken Roe v. Wade, the milestone decision of 1973 that established women's legal right to an abortion.
"A gestateling with intermediate status would almost certainly be considered by some in the U.S. (including some judges) to have at least certain legal rights, likely including right-to-life," says Johnston. This would enable a fetus on the edge of viability to make claims on the mother, and lead either to a shortening of the window in which abortion is legal—or a practice of denying abortion altogether. Instead, Johnston predicts, doctors might offer to transfer the fetus to an artificial womb for external gestation as a new standard of care.
But the legal conundrum does not stop there. The viability threshold is an estimate decided by medical professionals based on the clinical evidence and the technology available. It is anything but static. In the 1970s when Roe v. Wade was decided, for example, a fetus was considered legally viable starting at 28 weeks. Now, with improved technology and medical management, "the hard limit today is probably 20 or 21 weeks," says Matthew Kemp, associate professor at the University of Western Australia and one of the Australian-Japanese artificial womb project's senior researchers.
The changing threshold can result in situations where lots of people invested in the decision disagree. "Those can be hard decisions, but they are case-by-case decisions that families make or parents make with the key providers to determine when to proceed and when to let the infant die. Usually, it's a shared decision where the parents have the final say," says Johnston. But this isn't always the case.
On May 9th 2016, a boy named Alfie Evans was born in Liverpool, UK. Suffering seizures a few months after his birth, Alfie was diagnosed with an unknown neurodegenerative disorder and soon went into a semi-vegetative state, which lasted for more than a year. Alfie's medical team decided to withdraw his ventilation support, suggesting further treatment was unlawful and inhumane, but his parents wanted permission to fly him to a hospital in Rome and attempt to prolong his life there. In the end, the case went all the way up to the Supreme Court, which ruled that doctors could stop providing life support for Alfie, saying that the child required "peace, quiet and privacy." What happened to little Alfie raised huge publicity in the UK and pointedly highlighted the dilemma of whether parents or doctors should have the final say in the fate of a terminally-ill child in life-support treatment.
"In a few years from now, women who cannot get pregnant because of uterine infertility will be able to have a fully functional uterus made from their own tissue."
Alfie was born and, thus had legal rights, yet legal and ethical mayhem arose out of his case. When it comes to gestatelings, the scenarios will be even more complicated, says Romanis. "I think there's a really big question about who has parental rights and who doesn't," she says. "The assisted reproductive technology (ART) law in the U.K. hasn't been updated since 2008....It certainly needs an update when you think about all the things we have done since [then]."
This June, for instance, scientists from the Wake Forest Institute for Regenerative Medicine in North Carolina published research showing that they could take a small sample of tissue from a rabbit's uterus and create a bioengineered uterus, which then supported both fertilization and normal pregnancy like a natural uterus does.
"In [a number of] years from now, women who cannot get pregnant because of uterine infertility will be able to have a fully functional uterus made from their own tissue," says Dr. Anthony Atala, the Institute's director and a pioneer in regenerative medicine. These bioengineered uteri will eventually be covered by insurance, Atala expects. But when it comes to artificial wombs that externally gestate premature infants, will all mothers have equal access?
Medical reports have already shown racial and ethnic disparities in infertility treatments and access to assisted reproductive technologies. Costs on average total $12,400 per cycle of treatment and may require several cycles to achieve a live birth. "There's no indication that artificial wombs would be treated any differently. That's what we see with almost every expensive new medical technology," says Johnston. In a much more dystopian future, there is even a possibility that inequity in healthcare might create disturbing chasms in how women of various class levels bear children. Romanis asks us to picture the following scenario:
We live in a world where artificial wombs have become mainstream. Most women choose to end their pregnancies early and transfer their gestatelings to the care of machines. After a while, insurers deem full-term pregnancy and childbirth a risky non-necessity, and are lobbying to stop covering them altogether. Wealthy white women continue opting out of their third trimesters (at a high cost), since natural pregnancy has become a substandard route for poorer women. Those women are strongly judged for any behaviors that could risk their fetus's health, in contrast with the machine's controlled environment. "Why are you having a coffee during your pregnancy?" critics might ask. "Why are you having a glass of red wine? If you can't be perfect, why don't you have it the artificial way?"
Problem is, even if they want to, they won't be able to afford it.
In a more sanguine version, however, the artificial wombs are only used in cases of prematurity as a life-saving medical intervention rather than as a lifestyle accommodation. The 15 million babies who are born prematurely each year and may face serious respiratory, cardiovascular, visual and hearing problems, as well as learning disabilities, instead continue their normal development in artificial wombs. After lots of deliberation, insurers agree to bear the cost of external wombs because they are cheaper than a lifetime of medical care for a disabled or diseased person. This enables racial and ethnic minority women, who make up the majority of women giving premature birth, to access the technology.
Even extremely premature babies, those babies (far) below the threshold of 28 weeks of gestation, half of which die, could now discover this thing called life. In this scenario, as the Australian researcher Kemp says, we are simply giving a good shot at healthy, long-term survival to those who were unfortunate enough to start too soon.