A Single Blood Test May Soon Replace Your Annual Physical
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
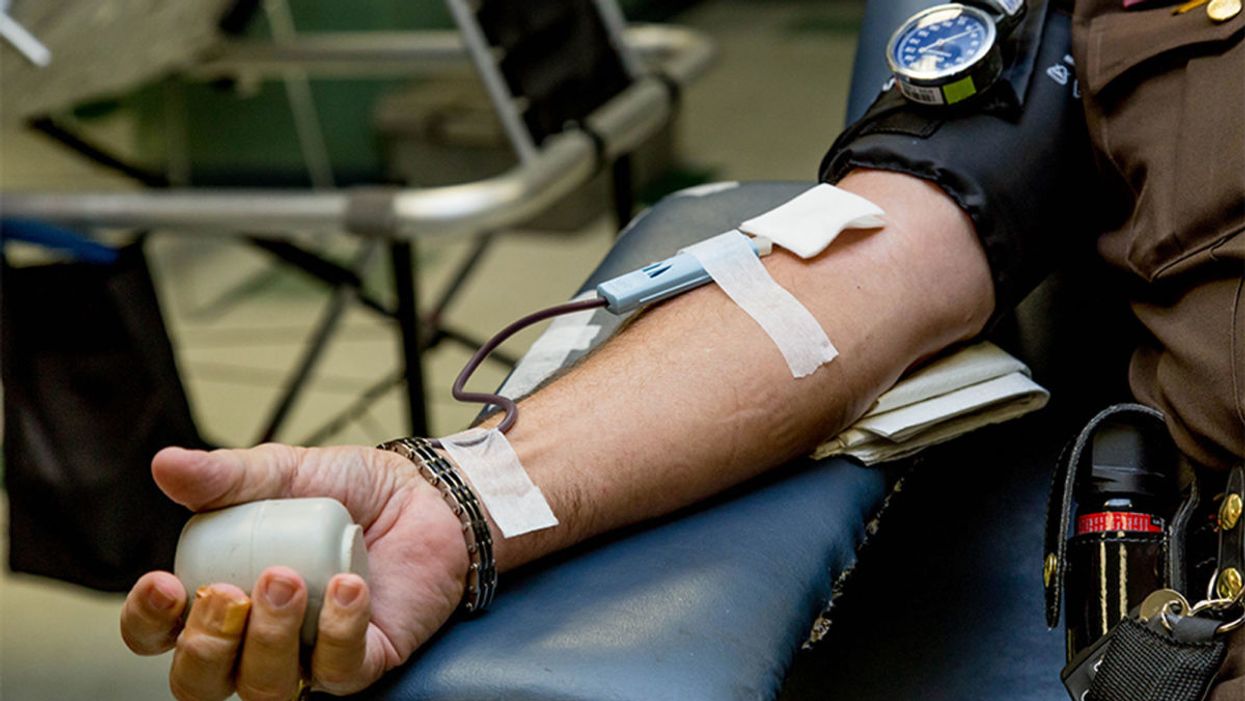
The measurement of proteins in one blood test could provide a comprehensive snapshot of a person's health in the near future.
For all the excitement over "personalized medicine" in the last two decades, its promise has not fully come to pass. Consider your standard annual physical.
Scientists have measured thousands of proteins from a single blood test to assess many individualized health conditions at once.
Your doctor still does a blood test to check your cholesterol and gauge your risk for heart disease by considering traditional risk factors (like smoking, diabetes, blood pressure) — an evaluation that has not changed in decades.
But a high-risk number alone is not enough to tell accurately whether you will suffer from heart disease. It just reflects your risk compared to population-level averages. In other words, not every person with elevated "bad" cholesterol will have a heart attack, so how can doctors determine who truly needs to give up the cheeseburgers and who doesn't?
Now, an emerging area of research may unlock some real-time answers. For the first time, as reported in the journal Nature Medicine last week, scientists have measured thousands of proteins from a single blood test to assess many individualized health conditions at once, including liver and kidney function, diabetes risk, body fat, cardiopulmonary fitness, and even smoking and alcohol consumption. Proteins can give a clear snapshot of how your body is faring at any given moment, as well as a sneak preview at what diseases may be lurking under the surface.
"Years from now," says study co-author Peter Ganz of UCSF, "we will probably be looking back on this paper as a milestone in personalized medicine."
We spoke to Ganz about the significance of this milestone. Our interview has been edited and condensed.
Is this the first study of its kind?
Yes, it is. This is a study where we measured 5,000 proteins at once to look for patterns that could either predict the risk of future diseases or inform the current state of health. Previous to this, people have measured typically one protein at a time, and some of these individual proteins have made it into clinical practice.
An example would be a protein called C-reactive protein, which is a measure of inflammation and is used sometimes in cardiology to predict the risk of future heart attacks. But what's really new is this scale. We wanted to get away from just focusing on one problem that the patient may have at a time, whether it's heart disease or kidney disease, and by measuring a much greater number of proteins, the hope is that we could inform the health of ultimately just about every organ in the body or every tissue. It's a step forward for what I would call "a one-stop shop."
"I'm very excited about personalized medicine through proteins as opposed to genes because you get both the nature and nurture."
Three things get me excited about this. One is the convenience for the patient of a single test to determine many different diseases. The second thing is the healthcare cost savings. We estimated what the cost would be to get these 11 healthcare measures that we reported on using traditional testing and the cost was upwards of 3,000 British pounds. And even though I don't know for sure what the cost of the protein tests would ultimately be, [it could come down to about $50 to $100].
The last thing is that the measurement of proteins is part of what people have called personalized medicine or precision medicine. If you look at risk factors across the population, it may not apply to individuals. In contrast, proteins are downstream of risk factors. So proteins actually tell us whether the traditional risk factors have set in motion the necessary machinery to cause disease. Proteins are the worker bees that regulate what the human body does, and so if you can find some anomalies in the proteins, that may inform us if a disease is likely to be ongoing even in its earliest stages.
Does protein testing have advantages over genetic testing for predicting future health risks?
The problem with genomics is that genes usually don't take care of the environment. It's a blueprint, but your blueprint has no idea what you will be exposed to during your lifetime in terms of the environment and lifestyle that you may choose and medications that you may be on. These are things that proteins can account for. I'm very excited about personalized medicine through proteins as opposed to genes because you get both the nature and nurture as opposed to genomics, which only gives you nature but doesn't account for anything else.
Proteins can also be tracked over time and that's not something you can do with genes. So if your behavior improves, your genes won't change, but your proteins will.
Could this new test become a regular feature of your annual physical?
That's the idea. This would be basically almost a standalone test that you could have done every year. And hopefully you wouldn't need other tests to complement this. This could be your yearly physical.
How much more does it need to be validated before it can enter the clinic and patients can trust the results?
This was a proof-of concept study. To really make this useful, we need to expand from 11 measures of health to a hundred or more health insights, to cover the whole body. And we need to expand this to all racial groups. Three of the five centers in the study were European – all Caucasian – so it's one of our high priorities to find groups of patients with better representation of minorities.
When do you expect doctors to be routinely giving this test to patients?
Much closer to five years than 20 years. We're scaling up from 11 disease states to 100, and many of those studies are underway. Results should be done within three to five years.
Do you think insurance will cover it?
Good question. I have been approached by an insurance company that wanted to understand the product better – a major insurer, with the possibility that this could actually be cost saving.
I have to ask you a curveball -- do you think that the downfall of Theranos will make consumers hesitant to trust a new technology that relies on using a single blood sample to screen for multiple health risks?
[Laughs] You're not the first person to ask me that today. I actually got a call from Elizabeth Holmes [in 2008 when I was at Harvard]. I met with her for an afternoon and met her team two more times. I gave them advice that they completely disregarded.
In many ways, what we do is diametrically opposite to Theranos. They had a culture of secrecy, and what we do is about openness. We publish, like this paper in Nature Medicine, to show the scientific details. Our supplement is much longer than the typical academic paper. We reveal everything we know. A lot of the research we do is funded by [the National Institutes of Health], and they have strict expectations about data sharing. So we agree to make the data available on a public website. If there is something we haven't done with the data, others can do it.
So you're saying that this is not another Theranos.
No, God forbid. We hope to be the opposite.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
Often called the window to the soul, the eyes are more sacred than other body parts, at least for some.
Awash in a fluid finely calibrated to keep it alive, a human eye rests inside a transparent cubic device. This ECaBox, or Eyes in a Care Box, is a one-of-a-kind system built by scientists at Barcelona’s Centre for Genomic Regulation (CRG). Their goal is to preserve human eyes for transplantation and related research.
In recent years, scientists have learned to transplant delicate organs such as the liver, lungs or pancreas, but eyes are another story. Even when preserved at the average transplant temperature of 4 Centigrade, they last for 48 hours max. That's one explanation for why transplanting the whole eye isn’t possible—only the cornea, the dome-shaped, outer layer of the eye, can withstand the procedure. The retina, the layer at the back of the eyeball that turns light into electrical signals, which the brain converts into images, is extremely difficult to transplant because it's packed with nerve tissue and blood vessels.
These challenges also make it tough to research transplantation. “This greatly limits their use for experiments, particularly when it comes to the effectiveness of new drugs and treatments,” said Maria Pia Cosma, a biologist at Barcelona’s Centre for Genomic Regulation (CRG), whose team is working on the ECaBox.
Eye transplants are desperately needed, but they're nowhere in sight. About 12.7 million people worldwide need a corneal transplant, which means that only one in 70 people who require them, get them. The gaps are international. Eye banks in the United Kingdom are around 20 percent below the level needed to supply hospitals, while Indian eye banks, which need at least 250,000 corneas per year, collect only around 45 to 50 thousand donor corneas (and of those 60 to 70 percent are successfully transplanted).
As for retinas, it's impossible currently to put one into the eye of another person. Artificial devices can be implanted to restore the sight of patients suffering from severe retinal diseases, but the number of people around the world with such “bionic eyes” is less than 600, while in America alone 11 million people have some type of retinal disease leading to severe vision loss. Add to this an increasingly aging population, commonly facing various vision impairments, and you have a recipe for heavy burdens on individuals, the economy and society. In the U.S. alone, the total annual economic impact of vision problems was $51.4 billion in 2017.
Even if you try growing tissues in the petri dish route into organoids mimicking the function of the human eye, you will not get the physiological complexity of the structure and metabolism of the real thing, according to Cosma. She is a member of a scientific consortium that includes researchers from major institutions from Spain, the U.K., Portugal, Italy and Israel. The consortium has received about $3.8 million from the European Union to pursue innovative eye research. Her team’s goal is to give hope to at least 2.2 billion people across the world afflicted with a vision impairment and 33 million who go through life with avoidable blindness.
Their method? Resuscitating cadaveric eyes for at least a month.
If we succeed, it will be the first intact human model of the eye capable of exploring and analyzing regenerative processes ex vivo. -- Maria Pia Cosma.
“We proposed to resuscitate eyes, that is to restore the global physiology and function of human explanted tissues,” Cosma said, referring to living tissues extracted from the eye and placed in a medium for culture. Their ECaBox is an ex vivo biological system, in which eyes taken from dead donors are placed in an artificial environment, designed to preserve the eye’s temperature and pH levels, deter blood clots, and remove the metabolic waste and toxins that would otherwise spell their demise.

Scientists work on resuscitating eyes in the lab of Maria Pia Cosma.
Courtesy of Maria Pia Cosma.
“One of the great challenges is the passage of the blood in the capillary branches of the eye, what we call long-term perfusion,” Cosma said. Capillaries are an intricate network of very thin blood vessels that transport blood, nutrients and oxygen to cells in the body’s organs and systems. To maintain the garland-shaped structure of this network, sufficient amounts of oxygen and nutrients must be provided through the eye circulation and microcirculation. “Our ambition is to combine perfusion of the vessels with artificial blood," along with using a synthetic form of vitreous, or the gel-like fluid that lets in light and supports the the eye's round shape, Cosma said.
The scientists use this novel setup with the eye submersed in its medium to keep the organ viable, so they can test retinal function. “If we succeed, we will ensure full functionality of a human organ ex vivo. It will be the first intact human model of the eye capable of exploring and analyzing regenerative processes ex vivo,” Cosma added.
A rapidly developing field of regenerative medicine aims to stimulate the body's natural healing processes and restore or replace damaged tissues and organs. But for people with retinal diseases, regenerative medicine progress has been painfully slow. “Experiments on rodents show progress, but the risks for humans are unacceptable,” Cosma said.
The ECaBox could boost progress with regenerative medicine for people with retinal diseases, which has been painfully slow because human experiments involving their eyes are too risky. “We will test emerging treatments while reducing animal research, and greatly accelerate the discovery and preclinical research phase of new possible treatments for vision loss at significantly reduced costs,” Cosma explained. Much less time and money would be wasted during the drug discovery process. Their work may even make it possible to transplant the entire eyeball for those who need it.
“It is a very exciting project,” said Sanjay Sharma, a professor of ophthalmology and epidemiology at Queen's University, in Kingston, Canada. “The ability to explore and monitor regenerative interventions will increasingly be of importance as we develop therapies that can regenerate ocular tissues, including the retina.”
Seemingly, there's no sacred religious text or a holy book prohibiting the practice of eye donation.
But is the world ready for eye transplants? “People are a bit weird or very emotional about donating their eyes as compared to other organs,” Cosma said. And much can be said about the problem of eye donor shortage. Concerns include disfigurement and healthcare professionals’ fear that the conversation about eye donation will upset the departed person’s relatives because of cultural or religious considerations. As just one example, Sharma noted the paucity of eye donations in his home country, Canada.
Yet, experts like Sharma stress the importance of these donations for both the recipients and their family members. “It allows them some psychological benefit in a very difficult time,” he said. So why are global eye banks suffering? Is it because the eyes are the windows to the soul?
Seemingly, there's no sacred religious text or a holy book prohibiting the practice of eye donation. In fact, most major religions of the world permit and support organ transplantation and donation, and by extension eye donation, because they unequivocally see it as an “act of neighborly love and charity.” In Hinduism, the concept of eye donation aligns with the Hindu principle of daan or selfless giving, where individuals donate their organs or body after death to benefit others and contribute to society. In Islam, eye donation is a form of sadaqah jariyah, a perpetual charity, as it can continue to benefit others even after the donor's death.
Meanwhile, Buddhist masters teach that donating an organ gives another person the chance to live longer and practice dharma, the universal law and order, more meaningfully; they also dismiss misunderstandings of the type “if you donate an eye, you’ll be born without an eye in the next birth.” And Christian teachings emphasize the values of love, compassion, and selflessness, all compatible with organ donation, eye donation notwithstanding; besides, those that will have a house in heaven, will get a whole new body without imperfections and limitations.
The explanation for people’s resistance may lie in what Deepak Sarma, a professor of Indian religions and philosophy at Case Western Reserve University in Cleveland, calls “street interpretation” of religious or spiritual dogmas. Consider the mechanism of karma, which is about the causal relation between previous and current actions. “Maybe some Hindus believe there is karma in the eyes and, if the eye gets transplanted into another person, they will have to have that karmic card from now on,” Sarma said. “Even if there is peculiar karma due to an untimely death–which might be interpreted by some as bad karma–then you have the karma of the recipient, which is tremendously good karma, because they have access to these body parts, a tremendous gift,” Sarma said. The overall accumulation is that of good karma: “It’s a beautiful kind of balance,” Sarma said.
For the Jews, Christians, and Muslims who believe in the physical resurrection of the body that will be made new in an afterlife, the already existing body is sacred since it will be the basis of a new refashioned body in an afterlife.---Omar Sultan Haque.
With that said, Sarma believes it is a fallacy to personify or anthropomorphize the eye, which doesn’t have a soul, and stresses that the karma attaches itself to the soul and not the body parts. But for scholars like Omar Sultan Haque—a psychiatrist and social scientist at Harvard Medical School, investigating questions across global health, anthropology, social psychology, and bioethics—the hierarchy of sacredness of body parts is entrenched in human psychology. You cannot equate the pinky toe with the face, he explained.
“The eyes are the window to the soul,” Haque said. “People have a hierarchy of body parts that are considered more sacred or essential to the self or soul, such as the eyes, face, and brain.” In his view, the techno-utopian transhumanist communities (especially those in Silicon Valley) have reduced the totality of a person to a mere material object, a “wet robot” that knows no sacredness or hierarchy of human body parts. “But for the Jews, Christians, and Muslims who believe in the physical resurrection of the body that will be made new in an afterlife, the [already existing] body is sacred since it will be the basis of a new refashioned body in an afterlife,” Haque said. “You cannot treat the body like any old material artifact, or old chair or ragged cloth, just because materialistic, secular ideologies want so,” he continued.
For Cosma and her peers, however, the very definition of what is alive or not is a bit semantic. “As soon as we die, the electrophysiological activity in the eye stops,” she said. “The goal of the project is to restore this activity as soon as possible before the highly complex tissue of the eye starts degrading.” Cosma’s group doesn’t yet know when they will be able to keep the eyes alive and well in the ECaBox, but the consensus is that the sooner the better. Hopefully, the taboos and fears around the eye donations will dissipate around the same time.
As Our AI Systems Get Better, So Must We
In order to build the future we want, we must also become ever better humans, explains the futurist Jamie Metzl in this opinion essay.
As the power and capability of our AI systems increase by the day, the essential question we now face is what constitutes peak human. If we stay where we are while the AI systems we are unleashing continually get better, they will meet and then exceed our capabilities in an ever-growing number of domains. But while some technology visionaries like Elon Musk call for us to slow down the development of AI systems to buy time, this approach alone will simply not work in our hyper-competitive world, particularly when the potential benefits of AI are so great and our frameworks for global governance are so weak. In order to build the future we want, we must also become ever better humans.
The list of activities we once saw as uniquely human where AIs have now surpassed us is long and growing. First, AI systems could beat our best chess players, then our best Go players, then our best champions of multi-player poker. They can see patterns far better than we can, generate medical and other hypotheses most human specialists miss, predict and map out new cellular structures, and even generate beautiful, and, yes, creative, art.
A recent paper by Microsoft researchers analyzing the significant leap in capabilities in OpenAI’s latest AI bot, ChatGPT-4, asserted that the algorithm can “solve novel and difficult tasks that span mathematics, coding, vision, medicine, law, psychology and more, without needing any special prompting.” Calling this functionality “strikingly close to human-level performance,” the authors conclude it “could reasonably be viewed as an early (yet still incomplete) version of an artificial general intelligence (AGI) system.”
The concept of AGI has been around for decades. In its common use, the term suggests a time when individual machines can do many different things at a human level, not just one thing like playing Go or analyzing radiological images. Debating when AGI might arrive, a favorite pastime of computer scientists for years, now has become outdated.
We already have AI algorithms and chatbots that can do lots of different things. Based on the generalist definition, in other words, AGI is essentially already here.
Unfettered by the evolved capacity and storage constraints of our brains, AI algorithms can access nearly all of the digitized cultural inheritance of humanity since the dawn of recorded history and have increasing access to growing pools of digitized biological data from across the spectrum of life.
Once we recognize that both AI systems and humans have unique superpowers, the essential question becomes what each of us can do better than the other and what humans and AIs can best do in active collaboration. The future of our species will depend upon our ability to safely, dynamically, and continually figure that out.
With these ever-larger datasets, rapidly increasing computing and memory power, and new and better algorithms, our AI systems will keep getting better faster than most of us can today imagine. These capabilities have the potential to help us radically improve our healthcare, agriculture, and manufacturing, make our economies more productive and our development more sustainable, and do many important things better.
Soon, they will learn how to write their own code. Like human children, in other words, AI systems will grow up. But even that doesn’t mean our human goose is cooked.
Just like dolphins and dogs, these alternate forms of intelligence will be uniquely theirs, not a lesser or greater version of ours. There are lots of things AI systems can't do and will never be able to do because our AI algorithms, for better and for worse, will never be human. Our embodied human intelligence is its own thing.
Our human intelligence is uniquely ours based on the capacities we have developed in our 3.8-billion-year journey from single cell organisms to us. Our brains and bodies represent continuous adaptations on earlier models, which is why our skeletal systems look like those of lizards and our brains like most other mammals with some extra cerebral cortex mixed in. Human intelligence isn’t just some type of disembodied function but the inextricable manifestation of our evolved physical reality. It includes our sensory analytical skills and all of our animal instincts, intuitions, drives, and perceptions. Disembodied machine intelligence is something different than what we have evolved and possess.
Because of this, some linguists including Noam Chomsky have recently argued that AI systems will never be intelligent as long as they are just manipulating symbols and mathematical tokens without any inherent understanding. Nothing could be further from the truth. Anyone interacting with even first-generation AI chatbots quickly realizes that while these systems are far from perfect or omniscient and can sometimes be stupendously oblivious, they are surprisingly smart and versatile and will get more so… forever. We have little idea even how our own minds work, so judging AI systems based on their output is relatively close to how we evaluate ourselves.
Anyone not awed by the potential of these AI systems is missing the point. AI’s newfound capacities demand that we work urgently to establish norms, standards, and regulations at all levels from local to global to manage the very real risks. Pausing our development of AI systems now doesn’t make sense, however, even if it were possible, because we have no sufficient ways of uniformly enacting such a pause, no plan for how we would use the time, and no common framework for addressing global collective challenges like this.
But if all we feel is a passive awe for these new capabilities, we will also be missing the point.
Human evolution, biology, and cultural history are not just some kind of accidental legacy, disability, or parlor trick, but our inherent superpower. Our ancestors outcompeted rivals for billions of years to make us so well suited to the world we inhabit and helped build. Our social organization at scale has made it possible for us to forge civilizations of immense complexity, engineer biology and novel intelligence, and extend our reach to the stars. Our messy, embodied, intuitive, social human intelligence is roughly mimicable by AI systems but, by definition, never fully replicable by them.
Once we recognize that both AI systems and humans have unique superpowers, the essential question becomes what each of us can do better than the other and what humans and AIs can best do in active collaboration. We still don't know. The future of our species will depend upon our ability to safely, dynamically, and continually figure that out.
As we do, we'll learn that many of our ideas and actions are made up of parts, some of which will prove essentially human and some of which can be better achieved by AI systems. Those in every walk of work and life who most successfully identify the optimal contributions of humans, AIs, and the two together, and who build systems and workflows empowering humans to do human things, machines to do machine things, and humans and machines to work together in ways maximizing the respective strengths of each, will be the champions of the 21st century across all fields.
The dawn of the age of machine intelligence is upon us. It’s a quantum leap equivalent to the domestication of plants and animals, industrialization, electrification, and computing. Each of these revolutions forced us to rethink what it means to be human, how we live, and how we organize ourselves. The AI revolution will happen more suddenly than these earlier transformations but will follow the same general trajectory. Now is the time to aggressively prepare for what is fast heading our way, including by active public engagement, governance, and regulation.
AI systems will not replace us, but, like these earlier technology-driven revolutions, they will force us to become different humans as we co-evolve with our technology. We will never reach peak human in our ongoing evolutionary journey, but we’ve got to manage this transition wisely to build the type of future we’d like to inhabit.
Alongside our ascending AIs, we humans still have a lot of climbing to do.

