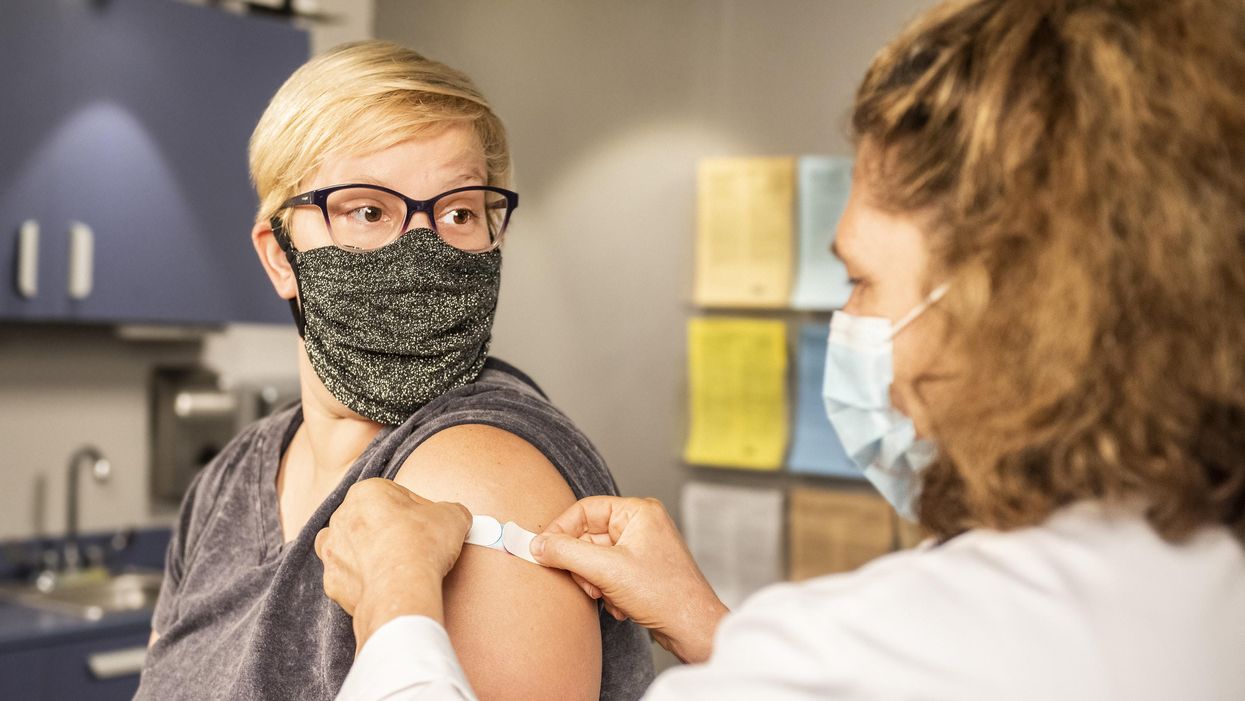
Clever Firm Predicts Patients Most at Risk, Then Tries to Intervene Before They Get Sicker

Health firm Populytics tracks and analyzes patient data, and makes care suggestions based on that data.
The diabetic patient hit the danger zone.
Ideally, blood sugar, measured by an A1C test, rests at 5.9 or less. A 7 is elevated, according to the Diabetes Council. Over 10, and you're into the extreme danger zone, at risk of every diabetic crisis from kidney failure to blindness.
In three months of working with a case manager, Jen's blood sugar had dropped to 7.2, a much safer range.
This patient's A1C was 10. Let's call her Jen for the sake of this story. (Although the facts of her case are real, the patient's actual name wasn't released due to privacy laws.).
Jen happens to live in Pennsylvania's Lehigh Valley, home of the nonprofit Lehigh Valley Health Network, which has eight hospital campuses and various clinics and other services. This network has invested more than $1 billion in IT infrastructure and founded Populytics, a spin-off firm that tracks and analyzes patient data, and makes care suggestions based on that data.
When Jen left the doctor's office, the Populytics data machine started churning, analyzing her data compared to a wealth of information about future likely hospital visits if she did not comply with recommendations, as well as the potential positive impacts of outreach and early intervention.
About a month after Jen received the dangerous blood test results, a community outreach specialist with psychological training called her. She was on a list generated by Populytics of follow-up patients to contact.
"It's a very gentle conversation," says Cathryn Kelly, who manages a care coordination team at Populytics. "The case manager provides them understanding and support and coaching." The goal, in this case, was small behavioral changes that would actually stick, like dietary ones.
In three months of working with a case manager, Jen's blood sugar had dropped to 7.2, a much safer range. The odds of her cycling back to the hospital ER or veering into kidney failure, or worse, had dropped significantly.
While the health network is extremely localized to one area of one state, using data to inform precise medical decision-making appears to be the wave of the future, says Ann Mongovern, the associate director of Health Care Ethics at the Markkula Center for Applied Ethics at Santa Clara University in California.
"Many hospitals and hospital systems don't yet try to do this at all, which is striking given where we're at in terms of our general technical ability in this society," Mongovern says.
How It Happened
While many hospitals make money by filling beds, the Lehigh Valley Health Network, as a nonprofit, accepts many patients on Medicaid and other government insurances that don't cover some of the costs of a hospitalization. The area's population is both poorer and older than national averages, according to the U.S. Census data, meaning more people with higher medical needs that may not have the support to care for themselves. They end up in the ER, or worse, again and again.
In the early 2000s, LVHN CEO Dr. Brian Nester started wondering if his health network could develop a way to predict who is most likely to land themselves a pricey ICU stay -- and offer support before those people end up needing serious care.
Embracing data use in such specific ways also brings up issues of data security and patient safety.
"There was an early understanding, even if you go back to the (federal) balanced budget act of 1997, that we were just kicking the can down the road to having a functional financial model to deliver healthcare to everyone with a reasonable price," Nester says. "We've got a lot of people living longer without more of an investment in the healthcare trust."
Popultyics, founded in 2013, was the result of years of planning and agonizing over those population numbers and cost concerns.
"We looked at our own health plan," Nester says. Out of all the employees and dependants on the LVHN's own insurance network, "roughly 1.5 percent of our 25,000 people — under 400 people — drove $30 million of our $130 million on insurance costs -- about 25 percent."
"You don't have to boil the ocean to take cost out of the system," he says. "You just have to focus on that 1.5%."
Take Jen, the diabetic patient. High blood sugar can lead to kidney failure, which can mean weekly expensive dialysis for 20 years. Investing in the data and staff to reach patients, he says, is "pennies compared to $100 bills."
For most doctors, "there's no awareness for providers to know who they should be seeing vs. who they are seeing. There's no incentive, because the incentive is to see as many patients as you can," he says.
To change that, first the LVHN invested in the popular medical management system, Epic. Then, they negotiated with the top 18 insurance companies that cover patients in the region to allow access to their patient care data, which means they have reams of patient history to feed the analytics machine in order to make predictions about outcomes. Nester admits not every hospital could do that -- with 52 percent of the market share, LVHN had a very strong negotiating position.
Third party services take that data and churn out analytics that feeds models and care management plans. All identifying information is stripped from the data.
"We can do predictive modeling in patients," says Populytics President and CEO Gregory Kile. "We can identify care gaps. Those care gaps are noted as alerts when the patient presents at the office."
Kile uses himself as a hypothetical patient.
"I pull up Gregory Kile, and boom, I see a flag or an alert. I see he hasn't been in for his last blood test. There is a care gap there we need to complete."
"There's just so much more you can do with that information," he says, envisioning a future where follow-up for, say, knee replacement surgery and outcomes could be tracked, and either validated or changed.
Ethical Issues at the Forefront
Of course, embracing data use in such specific ways also brings up issues of security and patient safety. For example, says medical ethicist Mongovern, there are many touchpoints where breaches could occur. The public has a growing awareness of how data used to personalize their experiences, such as social media analytics, can also be monetized and sold in ways that benefit a company, but not the user. That's not to say data supporting medical decisions is a bad thing, she says, just one with potential for public distrust if not handled thoughtfully.
"You're going to need to do this to stay competitive," she says. "But there's obviously big challenges, not the least of which is patient trust."
So far, a majority of the patients targeted – 62 percent -- appear to embrace the effort.
Among the ways the LVHN uses the data is monthly reports they call registries, which include patients who have just come in contact with the health network, either through the hospital or a doctor that works with them. The community outreach team members at Populytics take the names from the list, pull their records, and start calling. So far, a majority of the patients targeted – 62 percent -- appear to embrace the effort.
Says Nester: "Most of these are vulnerable people who are thrilled to have someone care about them. So they engage, and when a person engages in their care, they take their insulin shots. It's not rocket science. The rocket science is in identifying who the people are — the delivery of care is easy."
Vaccine passports, if required by businesses and universities, may give people a false sense of security, one expert cautions.
Vaccines are one of the greatest public health accomplishments of all time. For centuries, public health has relied on vaccinations to prevent and control disease outbreaks for a plethora of infectious scourges, with our crowning achievement being the successful eradication of smallpox.
The purpose of vaccine documentation is to provide proof of an individual's protection from either becoming infected or transmitting a vaccine-preventable disease. Vouching for these protections requires a firm knowledge about the epidemiology of the disease, as well as scientific knowledge concerning the efficacy of the vaccine. The vaccines we currently require be documented have met these tests; the vaccine for COVID-19 has not yet been proven to do so.
Let's acknowledge that the term "vaccine passport" is a poor choice of words. Passports are a legal travel document created by nations and governed by law for identification of the bearer to control entry and exit from nation states. They often serve as legal forms of identification and as a record of international travel. They are generally very sophisticated documents that have been created in a secure manner and may include a range of electronic and, in some cases, biometric measures such as fingerprints to ensure the holder is indeed who they say they are. Vaccine passports are medical documents used to document the vaccination status of an individual. They do not undergo the same level of administrative scrutiny and cannot be used to verify that the presenter is indeed the vaccinated individual. Some companies do have electronic methods to address concerns about verification; however, most people currently have paper records that can be easily falsified.
"Vaccine passports" as currently proposed risk giving people a false sense of security.
Successful disease control from vaccination programs relies on the ability to vaccinate at a level that prevents large-scale disease spread and the ability to rapidly identify the presence of disease outbreaks. It requires reliable, safe, and effective vaccines that are easily delivered in clinical and nonclinical settings. Keeping vaccination information as a part of the medical record, and even having a separate specialized vaccine record for personal use, is a time-honored tradition.
Keeping a vaccination record provides a method to keep track of the many shots one receives and serves as a visual reminder to help ensure the appropriate vaccine shot schedule is maintained for vaccines requiring multiple doses. The vaccine record, when combined with vaccine safety monitoring systems, serves as a mechanism to track adverse events to monitor and ensure the safety of vaccines as a consumer product. The record also serves as the official record of vaccination when required for administrative or legally prescribed purposes.
"Vaccine passports" as currently proposed risk giving people a false sense of security. In the case of the COVID-19 vaccines currently approved for use, many of the essential questions remain unanswered. While we do know the current three vaccines are highly protective against severe disease and death, and there is some evidence that these vaccinations do reduce infections and virus transmission of SARS-CoV-2, we do not yet know the full degree to which this occurs.
For example, we know there have been some cases of people that have been infected in close proximity to getting their full vaccination and rare cases of breakthrough reinfections. A breakthrough infection in a restaurant is a challenge for contact tracing, but an outbreak from a movie theater exposure or a baseball game could spark a major outbreak at our current level of vaccination. Current CDC guidance recommends continued mask wearing in order to address these concerns.
We also do not yet know how long the protections will last and if or when a booster or revaccination is required. In effect, it is too soon to know. Should an annual booster shot be required, then a vaccine passport would require annual updating, a process more frequent than renewal of a driver's license.
We also know that the current SARS-CoV-2 virus is mutating briskly. While the current approved vaccines have remained effective overall, there is evidence of some degree of degradation in vaccine effectiveness against some of the circulating strains. We also have sparse data on many of the other emerging strains of concern because we have not had the surveillance capacity in the U.S. to gain an adequate sense of how the virus is changing to fully align vaccine effectiveness with viral capabilities.
The risk of people misusing these "passports" is troubling. The potential for using these documents for hiring, firing or job limitation is a serious concern. Unvaccinated workers are at risk of this form of discrimination even from well-meaning employers or supervisors. Health insurers are prohibited by the Affordable Care Act from discriminating based on preexisting conditions, but they could probably charge a higher premium for unvaccinated individuals. There also is a risk of stigmatizing individuals who are not vaccinated or have left their vaccine documentation at home. Another concern: the opportunity to discriminate based on race, gender, sexual orientation, or religion, using one's vaccination status as an excuse.
These "passports" are being discussed as a "ticket verification" for entry to many activities, including dining at restaurants, flying domestically and/or internationally, going to movie theaters and sporting events, etc. These are all activities we already are doing at reduced levels and for which wearing a mask, hand hygiene and physical distancing are effective disease control practices. COVID-19 vaccines are indeed the measure that will make the ability to totally reopen our society complete, but we are not there yet. Documentation of one's COVID-19 vaccine status may be useful in selected situations in the future. That remains to be seen.
Finally, inadequate vaccine supply and disparities in vaccine delivery have created enormous challenges in providing equal access to vaccination. Also, the amount of misinformation, disinformation, and lingering vaccine hesitancy continue to limit the speed at which we will reach the level of vaccination of the population that would make this documentation meaningful. The requirement for "vaccine passports" is already alienating people who are opposed to vaccinations for a variety of reasons, paradoxically risking reduced vaccine uptake. This politicization of the vaccination effort is of concern. There are indeed people who, due to medical contraindications or legal exemptions, will not be vaccinated, and we do not yet have a national framework on how to address this.
Vaccine passports are not the solution for reopening our society — a robust vaccination program is. The requirement to document one's vaccination status for COVID-19 may one day have its place. For now, it is an idea whose time has not yet come.
Editor's Note: This op/ed is part of a "Big Question" series on the ethics of vaccine passports. Read the flip side argument here.
A digital health passport required by businesses and universities could help us get back to normal more quickly, one expert argues.
"Vaccine passports" are a system that requires proof of a COVID-19 vaccination as a condition of engaging in activities that pose a risk of transmitted SARS-CoV-2. Digital Health Passes (DHPs) are typically a smartphone application with a code that verifies whether someone has been vaccinated.
Vaccine passports could very much be in our future. Many businesses are implementing or planning to require proof of vaccination as a condition of returning to the workplace. Colleges and universities have announced vaccine requirements for students, staff, and faculty. It may not be long before the private sector requires a vaccination card or image to attend an entertainment or sporting event, to travel, or even to dine or shop indoors, at least in some venues.
But it's unlikely the federal government or the states will launch DHPs, at least not in the near-term. President Biden announced the White House has no intention of requiring proof of vaccination. While no state has mandated DHPs, New York is piloting its Excelsior Pass on a voluntary basis, partnering with IBM. Other nations are not so hesitant. Israel's "Green Pass" has gotten the nation back to normal in record time. And various countries and regions are planning DHPs, including the European Union and the United Kingdom. Foreign airlines are likely to require proof of vaccination as a condition of flying internationally.
DHPs could emerge as a way to get us back to normal more quickly, but are they ethical? Let's start with the law. The US Equal Opportunity Commission (EEOC) has specifically said that employers have the legal right to require proof of vaccination as a condition of returning to work. Colleges and universities already require several vaccines for students living in dorms. Hospitals and nursing homes often mandate influenza vaccinations. And, of course, all states require childhood vaccinations for school attendance. Vaccine passports are lawful but are they ethical? The short answer is "yes" but only if we ensure no one is left behind.
Vaccine passports "don't force anyone to be vaccinated against his or her will. They simply say to individuals that if you choose not to be vaccinated, you can't work or recreate in public spaces that risk transmission of the virus."
Why are vaccine passports ethical? Vaccines are a miracle of modern science, but they have become a political symbol, and a significant part of the population doesn't want to get a jab. The rare cases of blood clots associated with the Johnson & Johnson and AstraZeneca vaccines have only created more distrust.
Most opposition to vaccine passports hinges on the claim that they infringe personal autonomy and liberty. But this argument misses the point. Of course, every competent adult has the right to make decisions that affect his or her own health and safety. But no one has a right to infringe on the rights of others, such as by exposing them to a potentially serious or deadly infectious disease. An individual can't claim the right to attend a crowded event mask-less and unvaccinated. This was once accepted across the political spectrum. Conservative economists called it an "externality," that is a person has no right to harm others. The U.S. has lost the tradition of the common good. We have become so focused on our own individual rights that we forget about our ethical obligations to our neighbors and to our community.
In fact, DHPs actually don't force anyone to be vaccinated against his or her will. They simply say to individuals that if you choose not to be vaccinated, you can't work or recreate in public spaces that risk transmission of the virus.
DHPs also don't infringe on privacy. Again, everyone has the choice whether to show proof of vaccination. It isn't required. Moreover, DHPs may actually protect privacy because all they do is show whether or not you have been vaccinated. They don't disclose any other personal medical information. All of us actually have already had to show proof of vaccination as a condition of going to school. Thus, DHPs are well established in the United States.
But there is one ethical argument against DHPs that I find to be powerful, and that is equity. If we require proof of vaccination while doses are scarce, we will give the already privileged even more privilege. And that would be unconscionable. Thus, DHPs should not be implemented until everyone who wants a vaccine is able to get a vaccine. Equity isn't a side issue. It needs to be front and center.
As of today, all adults in the U.S. are eligible to get vaccinated, and President Biden has pledged that by the end of May there will be enough doses to vaccinate the entire U.S. population. It is a realistic promise. Once vaccines become plentiful, everyone should get their shot. All Food and Drug Administration authorized vaccines are highly safe and effective, even the Johnson & Johnson vaccine that the FDA has just put on pause.
Businesses have an economic incentive to require proof of vaccination. Very few of us would feel comfortable returning to our jobs, shops, theaters, or restaurants unless we feel safe. Businesses understand the duty to create safer places for work, recreation, and commerce.
One question has dominated national conversation since the pandemic began. "When will we get back to normal?" There is a deep human yearning to hug family and friends, see our work colleagues, recreate, and be entertained. One day we will have defeated this wily virus and get back to normal. But vaccine passports can help us get back to the things we love faster and more safely. As long as we don't leave anyone behind, using this miracle of modern science to make our lives better is both lawful and ethical.
Editor's Note: This op/ed is part of a "Big Question" series on the ethics of vaccine passports. Read the flip-side argument here.