Scientists redesign bacteria to tackle the antibiotic resistance crisis
Probiotic bacteria can be engineered to fight antibiotic-resistant superbugs by releasing chemicals that kill them.
In 1945, almost two decades after Alexander Fleming discovered penicillin, he warned that as antibiotics use grows, they may lose their efficiency. He was prescient—the first case of penicillin resistance was reported two years later. Back then, not many people paid attention to Fleming’s warning. After all, the “golden era” of the antibiotics age had just began. By the 1950s, three new antibiotics derived from soil bacteria — streptomycin, chloramphenicol, and tetracycline — could cure infectious diseases like tuberculosis, cholera, meningitis and typhoid fever, among others.
Today, these antibiotics and many of their successors developed through the 1980s are gradually losing their effectiveness. The extensive overuse and misuse of antibiotics led to the rise of drug resistance. The livestock sector buys around 80 percent of all antibiotics sold in the U.S. every year. Farmers feed cows and chickens low doses of antibiotics to prevent infections and fatten up the animals, which eventually causes resistant bacterial strains to evolve. If manure from cattle is used on fields, the soil and vegetables can get contaminated with antibiotic-resistant bacteria. Another major factor is doctors overprescribing antibiotics to humans, particularly in low-income countries. Between 2000 to 2018, the global rates of human antibiotic consumption shot up by 46 percent.
In recent years, researchers have been exploring a promising avenue: the use of synthetic biology to engineer new bacteria that may work better than antibiotics. The need continues to grow, as a Lancet study linked antibiotic resistance to over 1.27 million deaths worldwide in 2019, surpassing HIV/AIDS and malaria. The western sub-Saharan Africa region had the highest death rate (27.3 people per 100,000).
Researchers warn that if nothing changes, by 2050, antibiotic resistance could kill 10 million people annually.
To make it worse, our remedy pipelines are drying up. Out of the 18 biggest pharmaceutical companies, 15 abandoned antibiotic development by 2013. According to the AMR Action Fund, venture capital has remained indifferent towards biotech start-ups developing new antibiotics. In 2019, at least two antibiotic start-ups filed for bankruptcy. As of December 2020, there were 43 new antibiotics in clinical development. But because they are based on previously known molecules, scientists say they are inadequate for treating multidrug-resistant bacteria. Researchers warn that if nothing changes, by 2050, antibiotic resistance could kill 10 million people annually.
The rise of synthetic biology
To circumvent this dire future, scientists have been working on alternative solutions using synthetic biology tools, meaning genetically modifying good bacteria to fight the bad ones.
From the time life evolved on earth around 3.8 billion years ago, bacteria have engaged in biological warfare. They constantly strategize new methods to combat each other by synthesizing toxic proteins that kill competition.
For example, Escherichia coli produces bacteriocins or toxins to kill other strains of E.coli that attempt to colonize the same habitat. Microbes like E.coli (which are not all pathogenic) are also naturally present in the human microbiome. The human microbiome harbors up to 100 trillion symbiotic microbial cells. The majority of them are beneficial organisms residing in the gut at different compositions.
The chemicals that these “good bacteria” produce do not pose any health risks to us, but can be toxic to other bacteria, particularly to human pathogens. For the last three decades, scientists have been manipulating bacteria’s biological warfare tactics to our collective advantage.
In the late 1990s, researchers drew inspiration from electrical and computing engineering principles that involve constructing digital circuits to control devices. In certain ways, every cell in living organisms works like a tiny computer. The cell receives messages in the form of biochemical molecules that cling on to its surface. Those messages get processed within the cells through a series of complex molecular interactions.
Synthetic biologists can harness these living cells’ information processing skills and use them to construct genetic circuits that perform specific instructions—for example, secrete a toxin that kills pathogenic bacteria. “Any synthetic genetic circuit is merely a piece of information that hangs around in the bacteria’s cytoplasm,” explains José Rubén Morones-Ramírez, a professor at the Autonomous University of Nuevo León, Mexico. Then the ribosome, which synthesizes proteins in the cell, processes that new information, making the compounds scientists want bacteria to make. “The genetic circuit remains separated from the living cell’s DNA,” Morones-Ramírez explains. When the engineered bacteria replicates, the genetic circuit doesn’t become part of its genome.
Highly intelligent by bacterial standards, some multidrug resistant V. cholerae strains can also “collaborate” with other intestinal bacterial species to gain advantage and take hold of the gut.
In 2000, Boston-based researchers constructed an E.coli with a genetic switch that toggled between turning genes on and off two. Later, they built some safety checks into their bacteria. “To prevent unintentional or deleterious consequences, in 2009, we built a safety switch in the engineered bacteria’s genetic circuit that gets triggered after it gets exposed to a pathogen," says James Collins, a professor of biological engineering at MIT and faculty member at Harvard University’s Wyss Institute. “After getting rid of the pathogen, the engineered bacteria is designed to switch off and leave the patient's body.”
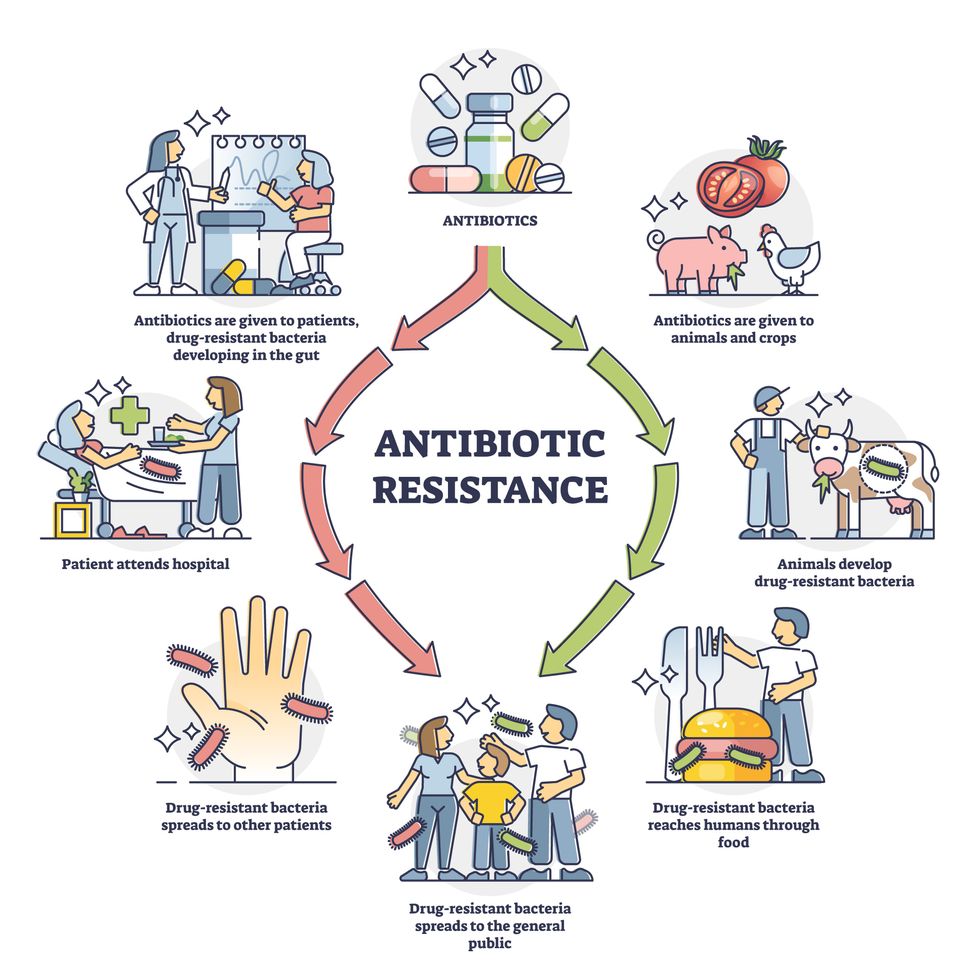
Overuse and misuse of antibiotics causes resistant strains to evolve
Adobe Stock
Seek and destroy
As the field of synthetic biology developed, scientists began using engineered bacteria to tackle superbugs. They first focused on Vibrio cholerae, which in the 19th and 20th century caused cholera pandemics in India, China, the Middle East, Europe, and Americas. Like many other bacteria, V. cholerae communicate with each other via quorum sensing, a process in which the microorganisms release different signaling molecules, to convey messages to its brethren. Highly intelligent by bacterial standards, some multidrug resistant V. cholerae strains can also “collaborate” with other intestinal bacterial species to gain advantage and take hold of the gut. When untreated, cholera has a mortality rate of 25 to 50 percent and outbreaks frequently occur in developing countries, especially during floods and droughts.
Sometimes, however, V. cholerae makes mistakes. In 2008, researchers at Cornell University observed that when quorum sensing V. cholerae accidentally released high concentrations of a signaling molecule called CAI-1, it had a counterproductive effect—the pathogen couldn’t colonize the gut.
So the group, led by John March, professor of biological and environmental engineering, developed a novel strategy to combat V. cholerae. They genetically engineered E.coli to eavesdrop on V. cholerae communication networks and equipped it with the ability to release the CAI-1 molecules. That interfered with V. cholerae progress. Two years later, the Cornell team showed that V. cholerae-infected mice treated with engineered E.coli had a 92 percent survival rate.
These findings inspired researchers to sic the good bacteria present in foods like yogurt and kimchi onto the drug-resistant ones.
Three years later in 2011, Singapore-based scientists engineered E.coli to detect and destroy Pseudomonas aeruginosa, an often drug-resistant pathogen that causes pneumonia, urinary tract infections, and sepsis. Once the genetically engineered E.coli found its target through its quorum sensing molecules, it then released a peptide, that could eradicate 99 percent of P. aeruginosa cells in a test-tube experiment. The team outlined their work in a Molecular Systems Biology study.
“At the time, we knew that we were entering new, uncharted territory,” says lead author Matthew Chang, an associate professor and synthetic biologist at the National University of Singapore and lead author of the study. “To date, we are still in the process of trying to understand how long these microbes stay in our bodies and how they might continue to evolve.”
More teams followed the same path. In a 2013 study, MIT researchers also genetically engineered E.coli to detect P. aeruginosa via the pathogen’s quorum-sensing molecules. It then destroyed the pathogen by secreting a lab-made toxin.
Probiotics that fight
A year later in 2014, a Nature study found that the abundance of Ruminococcus obeum, a probiotic bacteria naturally occurring in the human microbiome, interrupts and reduces V.cholerae’s colonization— by detecting the pathogen’s quorum sensing molecules. The natural accumulation of R. obeum in Bangladeshi adults helped them recover from cholera despite living in an area with frequent outbreaks.
The findings from 2008 to 2014 inspired Collins and his team to delve into how good bacteria present in foods like yogurt and kimchi can attack drug-resistant bacteria. In 2018, Collins and his team developed the engineered probiotic strategy. They tweaked a bacteria commonly found in yogurt called Lactococcus lactis to treat cholera.
Engineered bacteria can be trained to target pathogens when they are at their most vulnerable metabolic stage in the human gut. --José Rubén Morones-Ramírez.
More scientists followed with more experiments. So far, researchers have engineered various probiotic organisms to fight pathogenic bacteria like Staphylococcus aureus (leading cause of skin, tissue, bone, joint and blood infections) and Clostridium perfringens (which causes watery diarrhea) in test-tube and animal experiments. In 2020, Russian scientists engineered a probiotic called Pichia pastoris to produce an enzyme called lysostaphin that eradicated S. aureus in vitro. Another 2020 study from China used an engineered probiotic bacteria Lactobacilli casei as a vaccine to prevent C. perfringens infection in rabbits.
In a study last year, Ramírez’s group at the Autonomous University of Nuevo León, engineered E. coli to detect quorum-sensing molecules from Methicillin-resistant Staphylococcus aureus or MRSA, a notorious superbug. The E. coli then releases a bacteriocin that kills MRSA. “An antibiotic is just a molecule that is not intelligent,” says Ramírez. “On the other hand, engineered bacteria can be trained to target pathogens when they are at their most vulnerable metabolic stage in the human gut.”
Collins and Timothy Lu, an associate professor of biological engineering at MIT, found that engineered E. coli can help treat other conditions—such as phenylketonuria, a rare metabolic disorder, that causes the build-up of an amino acid phenylalanine. Their start-up Synlogic aims to commercialize the technology, and has completed a phase 2 clinical trial.
Circumventing the challenges
The bacteria-engineering technique is not without pitfalls. One major challenge is that beneficial gut bacteria produce their own quorum-sensing molecules that can be similar to those that pathogens secrete. If an engineered bacteria’s biosensor is not specific enough, it will be ineffective.
Another concern is whether engineered bacteria might mutate after entering the gut. “As with any technology, there are risks where bad actors could have the capability to engineer a microbe to act quite nastily,” says Collins of MIT. But Collins and Ramírez both insist that the chances of the engineered bacteria mutating on its own are virtually non-existent. “It is extremely unlikely for the engineered bacteria to mutate,” Ramírez says. “Coaxing a living cell to do anything on command is immensely challenging. Usually, the greater risk is that the engineered bacteria entirely lose its functionality.”
However, the biggest challenge is bringing the curative bacteria to consumers. Pharmaceutical companies aren’t interested in antibiotics or their alternatives because it’s less profitable than developing new medicines for non-infectious diseases. Unlike the more chronic conditions like diabetes or cancer that require long-term medications, infectious diseases are usually treated much quicker. Running clinical trials are expensive and antibiotic-alternatives aren’t lucrative enough.
“Unfortunately, new medications for antibiotic resistant infections have been pushed to the bottom of the field,” says Lu of MIT. “It's not because the technology does not work. This is more of a market issue. Because clinical trials cost hundreds of millions of dollars, the only solution is that governments will need to fund them.” Lu stresses that societies must lobby to change how the modern healthcare industry works. “The whole world needs better treatments for antibiotic resistance.”
Your phone could show if a bridge is about to collapse
Researchers have tested a new smartphone app that could gather data about whether bridges are "structurally deficient" —a low-cost citizen-scientist alternative to current methods that are expensive and complex.
In summer 2017, Thomas Matarazzo, then a postdoctoral researcher at the Massachusetts Institute of Technology, landed in San Francisco with a colleague. They rented two cars, drove up to the Golden Gate bridge, timing it to the city’s rush hour, and rode over to the other side in heavy traffic. Once they reached the other end, they turned around and did it again. And again. And again.
“I drove over that bridge 100 times over five days, back and forth,” says Matarazzo, now an associate director of High-Performance Computing in the Center for Innovation in Engineering at the United States Military Academy, West Point. “It was surprisingly stressful, I never anticipated that. I had to maintain the speed of about 30 miles an hour when the speed limit is 45. I felt bad for everybody behind me.”
Matarazzo had to drive slowly because the quality of data they were collecting depended on it. The pair was designing and testing a new smartphone app that could gather data about the bridge’s structural integrity—a low-cost citizen-scientist alternative to the current industrial methods, which aren’t always possible, partly because they’re expensive and complex. In the era of aging infrastructure, when some bridges in the United States and other countries are structurally unsound to the point of collapsing, such an app could inform authorities about the need for urgent repairs, or at least prompt closing the most dangerous structures.
There are 619,588 bridges in the U.S., and some of them are very old. For example, the Benjamin Franklin Bridge connecting Philadelphia to Camden, N.J., is 96-years-old while the Brooklyn Bridge is 153. So it’s hardly surprising that many could use some upgrades. “In the U.S., a lot of them were built in the post-World War II period to accommodate the surge of motorization,” says Carlo Ratti, architect and engineer who directs the Senseable City Lab at Massachusetts Institute of Technology. “They are beginning to reach the end of their life.”
According to the 2022 American Road & Transportation Builders Association’s report, one in three U.S. bridges needs repair or replacement. The Department of Transportation (DOT) National Bridge Inventory (NBI) database reveals concerning numbers. Thirty-six percent of U.S. bridges need repair work and over 78,000 bridges should be replaced. More than 43,500 bridges are rated in poor condition and classified as “structurally deficient” – an alarming description. Yet, people drive over them 167.5 million times a day. The Pittsburgh bridge which collapsed in January this year—only hours before President Biden arrived to discuss the new infrastructure law—was on the “poor” rating list.
Assessing the structural integrity of a bridge is not an easy endeavor. Most of the time, these are visual inspections, Matarazzo explains. Engineers check cracks, rust and other signs of wear and tear. They also check for wildlife—birds which may build nests or even small animals that make homes inside the bridge structures, which can slowly chip at the structure. However, visual inspections may not tell the whole story. A more sophisticated and significantly more expensive inspection requires placing special sensors on the bridge that essentially listen to how the bridge vibrates.
“Some bridges can afford expensive sensors to do the job, but that comes at a very high cost—hundreds of thousands of dollars per bridge per year,” Ratti says.
We may think of bridges as immovable steel and concrete monoliths, but they naturally vibrate, oscillating slightly. That movement can be influenced by the traffic that passes over them, and even by wind. Bridges of different types vibrate differently—some have longer vibrational frequencies and others shorter ones. A good way to visualize this phenomenon is to place a ruler over the edge of a desk and flick it slightly. If the ruler protrudes far off the desk, it will vibrate slowly. But if you shorten the end that hangs off, it will vibrate much faster. It works similarly with bridges, except there are more factors at play, including not only the length, but also the design and the materials used.
The long suspension bridges such as the Golden Gate or Verrazano Narrows, which hang on a series of cables, are more flexible, and their vibration amplitudes are longer. The Golden Gate Bridge can vibrate at 0.106 Hertz, where one Hertz is one oscillation per second. “Think about standing on the bridge for about 10 seconds—that's how long it takes for it to move all the way up and all the way down in one oscillation,” Matarazzo says.
On the contrary, the concrete span bridges that rest on multiple columns like Brooklyn Bridge or Manhattan Bridge, are “stiffer” and have greater vibrational frequencies. A concrete bridge can have a frequency of 10 Hertz, moving 10 times in one second—like that shorter stretch of a ruler.
The special devices that can pick up and record these vibrations over time are called accelerometers. A network of these devices for each bridge can cost $20,000 to $50,000, and more—and require trained personnel to place them. The sensors also must stay on the bridge for some time to establish what’s a healthy vibrational baseline for a given bridge. Maintaining them adds to the cost. “Some bridges can afford expensive sensors to do the job, but that comes at a very high cost—hundreds of thousands of dollars per bridge per year,” Ratti says.
Making sense of the readouts they gather is another challenge, which requires a high level of technical expertise. “You generally need somebody, some type of expert capable of doing the analysis to translate that data into information,” says Matarazzo, which ticks up the price, so doing visual inspections often proves to be a more economical choice for state-level DOTs with tight budgets. “The existing systems work well, but have downsides,” Ratti says. The team thought the old method could use some modernizing.
Smartphones, which are carried by millions of people, contain dozens of sensors, including the accelerometers capable of picking up the bridges’ vibrations. That’s why Matarazzo and his colleague drove over the bridge 100 times—they were trying to pick up enough data. Timing it to rush hour supported that goal because traffic caused more “excitation,” Matarazzo explains. “Excitation is a big word we use when we talk about what drives the vibration,” he says. “When there's a lot of traffic, there's more excitation and more vibration.” They also collaborated with Uber, whose drivers made 72 trips across the bridge to gather data in different cars.
The next step was to clean the data from “noise”—various vibrations that weren’t relevant to the bridge but came from the cars themselves. “It could be jumps in speed, it could be potholes, it could be a bunch of other things," Matarazzo says. But as the team gathered more data, it became easier to tell the bridge vibrational frequencies from all others because the noises generated by cars, traffic and other things tend to “cancel out.”
The team specifically picked the Golden Gate bridge because the civil structural engineering community had studied it extensively over the years and collected a host of vibrational data, using traditional sensors. When the researchers compared their app-collected frequencies with those gathered by 240 accelerometers formerly placed on the Golden Gate, the results were the same—the data from the phones converged with that from the bridge’s sensors. The smartphone-collected data were just as good as those from industry devices.
The study authors estimate that officials could use crowdsourced data to make key improvements that would help new bridges to last about 14 years longer.
The team also tested their method on a different type of bridge—not a suspension one like the Golden Gate, but a concrete span bridge in Ciampino, Italy. There they compared 280 car trips over the bridge to the six sensors that had been placed on the bridge for seven months. The results were slightly less matching, but a larger volume of trips would fix the divergence, the researchers wrote in their study, titled Crowdsourcing bridge dynamic monitoring with smartphone vehicle trips, published last month in Nature Communications Engineering.
Although the smartphones proved effective, the app is not quite ready to be rolled out commercially for people to start using. “It is still a pilot version,” so there’s room for improvement, says Ratti, who co-authored the study. “But on a more optimistic note, it has really low barriers to entry—all you need is smartphones on cars—so that makes the system easy to reach a global audience.” And the study authors estimate that the use of crowdsourced data would result in a new bridge lasting about 14 years longer.
Matarazzo hopes that the app could be eventually accessible for your average citizen scientist to collect the data and supply it to their local transportation authorities. “I hope that this idea can spark a different type of relationship with infrastructure where people think about the data they're collecting as some type of contribution or investment into their communities,” he says. “So that they can help their own department of transportation, their own municipality to support that bridge and keep it maintained better, longer and safer.”
Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.
The Friday Five: Sugar could help catch cancer early
In this week's Friday Five, catching cancer early could depend on sugar, how to boost memory in a flash, a tiny sandwich cake could help the heart, and meet the top banana in the fight against Covid.
The Friday Five covers five stories in research that you may have missed this week. There are plenty of controversies and troubling ethical issues in science – and we get into many of them in our online magazine – but this news roundup focuses on scientific creativity and progress to give you a therapeutic dose of inspiration headed into the weekend.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
Here are the promising studies covered in this week's Friday Five:
- Catching cancer early could depend on sugar
- How to boost memory in a flash
- This is your brain on books
- A tiny sandwich cake could help the heart
- Meet the top banana for fighting Covid variants

