Scientists redesign bacteria to tackle the antibiotic resistance crisis
Probiotic bacteria can be engineered to fight antibiotic-resistant superbugs by releasing chemicals that kill them.
In 1945, almost two decades after Alexander Fleming discovered penicillin, he warned that as antibiotics use grows, they may lose their efficiency. He was prescient—the first case of penicillin resistance was reported two years later. Back then, not many people paid attention to Fleming’s warning. After all, the “golden era” of the antibiotics age had just began. By the 1950s, three new antibiotics derived from soil bacteria — streptomycin, chloramphenicol, and tetracycline — could cure infectious diseases like tuberculosis, cholera, meningitis and typhoid fever, among others.
Today, these antibiotics and many of their successors developed through the 1980s are gradually losing their effectiveness. The extensive overuse and misuse of antibiotics led to the rise of drug resistance. The livestock sector buys around 80 percent of all antibiotics sold in the U.S. every year. Farmers feed cows and chickens low doses of antibiotics to prevent infections and fatten up the animals, which eventually causes resistant bacterial strains to evolve. If manure from cattle is used on fields, the soil and vegetables can get contaminated with antibiotic-resistant bacteria. Another major factor is doctors overprescribing antibiotics to humans, particularly in low-income countries. Between 2000 to 2018, the global rates of human antibiotic consumption shot up by 46 percent.
In recent years, researchers have been exploring a promising avenue: the use of synthetic biology to engineer new bacteria that may work better than antibiotics. The need continues to grow, as a Lancet study linked antibiotic resistance to over 1.27 million deaths worldwide in 2019, surpassing HIV/AIDS and malaria. The western sub-Saharan Africa region had the highest death rate (27.3 people per 100,000).
Researchers warn that if nothing changes, by 2050, antibiotic resistance could kill 10 million people annually.
To make it worse, our remedy pipelines are drying up. Out of the 18 biggest pharmaceutical companies, 15 abandoned antibiotic development by 2013. According to the AMR Action Fund, venture capital has remained indifferent towards biotech start-ups developing new antibiotics. In 2019, at least two antibiotic start-ups filed for bankruptcy. As of December 2020, there were 43 new antibiotics in clinical development. But because they are based on previously known molecules, scientists say they are inadequate for treating multidrug-resistant bacteria. Researchers warn that if nothing changes, by 2050, antibiotic resistance could kill 10 million people annually.
The rise of synthetic biology
To circumvent this dire future, scientists have been working on alternative solutions using synthetic biology tools, meaning genetically modifying good bacteria to fight the bad ones.
From the time life evolved on earth around 3.8 billion years ago, bacteria have engaged in biological warfare. They constantly strategize new methods to combat each other by synthesizing toxic proteins that kill competition.
For example, Escherichia coli produces bacteriocins or toxins to kill other strains of E.coli that attempt to colonize the same habitat. Microbes like E.coli (which are not all pathogenic) are also naturally present in the human microbiome. The human microbiome harbors up to 100 trillion symbiotic microbial cells. The majority of them are beneficial organisms residing in the gut at different compositions.
The chemicals that these “good bacteria” produce do not pose any health risks to us, but can be toxic to other bacteria, particularly to human pathogens. For the last three decades, scientists have been manipulating bacteria’s biological warfare tactics to our collective advantage.
In the late 1990s, researchers drew inspiration from electrical and computing engineering principles that involve constructing digital circuits to control devices. In certain ways, every cell in living organisms works like a tiny computer. The cell receives messages in the form of biochemical molecules that cling on to its surface. Those messages get processed within the cells through a series of complex molecular interactions.
Synthetic biologists can harness these living cells’ information processing skills and use them to construct genetic circuits that perform specific instructions—for example, secrete a toxin that kills pathogenic bacteria. “Any synthetic genetic circuit is merely a piece of information that hangs around in the bacteria’s cytoplasm,” explains José Rubén Morones-Ramírez, a professor at the Autonomous University of Nuevo León, Mexico. Then the ribosome, which synthesizes proteins in the cell, processes that new information, making the compounds scientists want bacteria to make. “The genetic circuit remains separated from the living cell’s DNA,” Morones-Ramírez explains. When the engineered bacteria replicates, the genetic circuit doesn’t become part of its genome.
Highly intelligent by bacterial standards, some multidrug resistant V. cholerae strains can also “collaborate” with other intestinal bacterial species to gain advantage and take hold of the gut.
In 2000, Boston-based researchers constructed an E.coli with a genetic switch that toggled between turning genes on and off two. Later, they built some safety checks into their bacteria. “To prevent unintentional or deleterious consequences, in 2009, we built a safety switch in the engineered bacteria’s genetic circuit that gets triggered after it gets exposed to a pathogen," says James Collins, a professor of biological engineering at MIT and faculty member at Harvard University’s Wyss Institute. “After getting rid of the pathogen, the engineered bacteria is designed to switch off and leave the patient's body.”
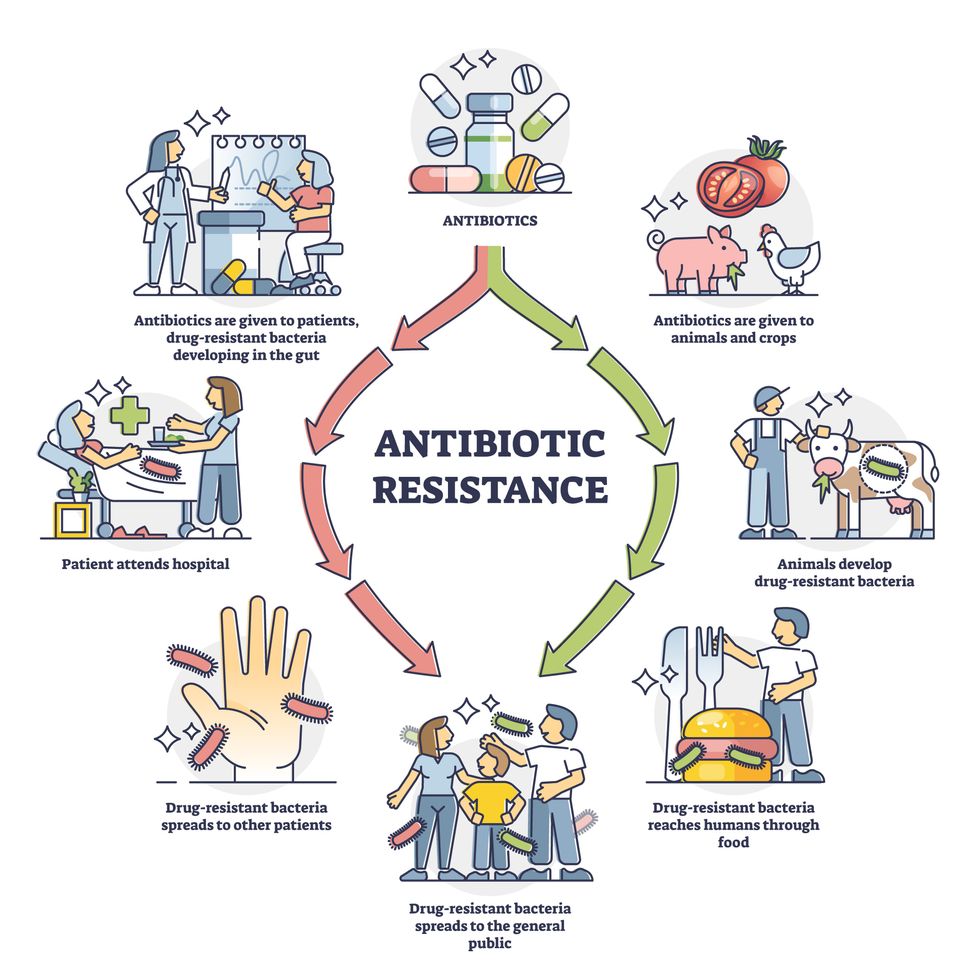
Overuse and misuse of antibiotics causes resistant strains to evolve
Adobe Stock
Seek and destroy
As the field of synthetic biology developed, scientists began using engineered bacteria to tackle superbugs. They first focused on Vibrio cholerae, which in the 19th and 20th century caused cholera pandemics in India, China, the Middle East, Europe, and Americas. Like many other bacteria, V. cholerae communicate with each other via quorum sensing, a process in which the microorganisms release different signaling molecules, to convey messages to its brethren. Highly intelligent by bacterial standards, some multidrug resistant V. cholerae strains can also “collaborate” with other intestinal bacterial species to gain advantage and take hold of the gut. When untreated, cholera has a mortality rate of 25 to 50 percent and outbreaks frequently occur in developing countries, especially during floods and droughts.
Sometimes, however, V. cholerae makes mistakes. In 2008, researchers at Cornell University observed that when quorum sensing V. cholerae accidentally released high concentrations of a signaling molecule called CAI-1, it had a counterproductive effect—the pathogen couldn’t colonize the gut.
So the group, led by John March, professor of biological and environmental engineering, developed a novel strategy to combat V. cholerae. They genetically engineered E.coli to eavesdrop on V. cholerae communication networks and equipped it with the ability to release the CAI-1 molecules. That interfered with V. cholerae progress. Two years later, the Cornell team showed that V. cholerae-infected mice treated with engineered E.coli had a 92 percent survival rate.
These findings inspired researchers to sic the good bacteria present in foods like yogurt and kimchi onto the drug-resistant ones.
Three years later in 2011, Singapore-based scientists engineered E.coli to detect and destroy Pseudomonas aeruginosa, an often drug-resistant pathogen that causes pneumonia, urinary tract infections, and sepsis. Once the genetically engineered E.coli found its target through its quorum sensing molecules, it then released a peptide, that could eradicate 99 percent of P. aeruginosa cells in a test-tube experiment. The team outlined their work in a Molecular Systems Biology study.
“At the time, we knew that we were entering new, uncharted territory,” says lead author Matthew Chang, an associate professor and synthetic biologist at the National University of Singapore and lead author of the study. “To date, we are still in the process of trying to understand how long these microbes stay in our bodies and how they might continue to evolve.”
More teams followed the same path. In a 2013 study, MIT researchers also genetically engineered E.coli to detect P. aeruginosa via the pathogen’s quorum-sensing molecules. It then destroyed the pathogen by secreting a lab-made toxin.
Probiotics that fight
A year later in 2014, a Nature study found that the abundance of Ruminococcus obeum, a probiotic bacteria naturally occurring in the human microbiome, interrupts and reduces V.cholerae’s colonization— by detecting the pathogen’s quorum sensing molecules. The natural accumulation of R. obeum in Bangladeshi adults helped them recover from cholera despite living in an area with frequent outbreaks.
The findings from 2008 to 2014 inspired Collins and his team to delve into how good bacteria present in foods like yogurt and kimchi can attack drug-resistant bacteria. In 2018, Collins and his team developed the engineered probiotic strategy. They tweaked a bacteria commonly found in yogurt called Lactococcus lactis to treat cholera.
Engineered bacteria can be trained to target pathogens when they are at their most vulnerable metabolic stage in the human gut. --José Rubén Morones-Ramírez.
More scientists followed with more experiments. So far, researchers have engineered various probiotic organisms to fight pathogenic bacteria like Staphylococcus aureus (leading cause of skin, tissue, bone, joint and blood infections) and Clostridium perfringens (which causes watery diarrhea) in test-tube and animal experiments. In 2020, Russian scientists engineered a probiotic called Pichia pastoris to produce an enzyme called lysostaphin that eradicated S. aureus in vitro. Another 2020 study from China used an engineered probiotic bacteria Lactobacilli casei as a vaccine to prevent C. perfringens infection in rabbits.
In a study last year, Ramírez’s group at the Autonomous University of Nuevo León, engineered E. coli to detect quorum-sensing molecules from Methicillin-resistant Staphylococcus aureus or MRSA, a notorious superbug. The E. coli then releases a bacteriocin that kills MRSA. “An antibiotic is just a molecule that is not intelligent,” says Ramírez. “On the other hand, engineered bacteria can be trained to target pathogens when they are at their most vulnerable metabolic stage in the human gut.”
Collins and Timothy Lu, an associate professor of biological engineering at MIT, found that engineered E. coli can help treat other conditions—such as phenylketonuria, a rare metabolic disorder, that causes the build-up of an amino acid phenylalanine. Their start-up Synlogic aims to commercialize the technology, and has completed a phase 2 clinical trial.
Circumventing the challenges
The bacteria-engineering technique is not without pitfalls. One major challenge is that beneficial gut bacteria produce their own quorum-sensing molecules that can be similar to those that pathogens secrete. If an engineered bacteria’s biosensor is not specific enough, it will be ineffective.
Another concern is whether engineered bacteria might mutate after entering the gut. “As with any technology, there are risks where bad actors could have the capability to engineer a microbe to act quite nastily,” says Collins of MIT. But Collins and Ramírez both insist that the chances of the engineered bacteria mutating on its own are virtually non-existent. “It is extremely unlikely for the engineered bacteria to mutate,” Ramírez says. “Coaxing a living cell to do anything on command is immensely challenging. Usually, the greater risk is that the engineered bacteria entirely lose its functionality.”
However, the biggest challenge is bringing the curative bacteria to consumers. Pharmaceutical companies aren’t interested in antibiotics or their alternatives because it’s less profitable than developing new medicines for non-infectious diseases. Unlike the more chronic conditions like diabetes or cancer that require long-term medications, infectious diseases are usually treated much quicker. Running clinical trials are expensive and antibiotic-alternatives aren’t lucrative enough.
“Unfortunately, new medications for antibiotic resistant infections have been pushed to the bottom of the field,” says Lu of MIT. “It's not because the technology does not work. This is more of a market issue. Because clinical trials cost hundreds of millions of dollars, the only solution is that governments will need to fund them.” Lu stresses that societies must lobby to change how the modern healthcare industry works. “The whole world needs better treatments for antibiotic resistance.”
Entomologist Jessica Ware is using new technologies to identify insect species in a changing climate. She shares her suggestions for how we can live harmoniously with creeper crawlers everywhere.
Jessica Ware is obsessed with bugs.
My guest today is a leading researcher on insects, the president of the Entomological Society of America and a curator at the American Museum of Natural History. Learn more about her here.
You may not think that insects and human health go hand-in-hand, but as Jessica makes clear, they’re closely related. A lot of people care about their health, and the health of other creatures on the planet, and the health of the planet itself, but researchers like Jessica are studying another thing we should be focusing on even more: how these seemingly separate areas are deeply entwined. (This is the theme of an upcoming event hosted by Leaps.org and the Aspen Institute.)
Listen to the Episode
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google

Entomologist Jessica Ware
D. Finnin / AMNH
Maybe it feels like a core human instinct to demonize bugs as gross. We seem to try to eradicate them in every way possible, whether that’s with poison, or getting out our blood thirst by stomping them whenever they creep and crawl into sight.
But where did our fear of bugs really come from? Jessica makes a compelling case that a lot of it is cultural, rather than in-born, and we should be following the lead of other cultures that have learned to live with and appreciate bugs.
The truth is that a healthy planet depends on insects. You may feel stung by that news if you hate bugs. Reality bites.
Jessica and I talk about whether learning to live with insects should include eating them and gene editing them so they don’t transmit viruses. She also tells me about her important research into using genomic tools to track bugs in the wild to figure out why and how we’ve lost 50 percent of the insect population since 1970 according to some estimates – bad news because the ecosystems that make up the planet heavily depend on insects. Jessica is leading the way to better understand what’s causing these declines in order to start reversing these trends to save the insects and to save ourselves.
They received retinal implants to restore their vision. Then the company turned its back on them.
A company called Second Sight made an implant that partially restored vision to people who'd been blind for decades. But when Second Sight pivoted, it stopped servicing its product, leaving many in the dark.
The first thing Jeroen Perk saw after he partially regained his sight nearly a decade ago was the outline of his guide dog Pedro.
“There was a white floor, and the dog was black,” recalls Perk, a 43-year-old investigator for the Dutch customs service. “I was crying. It was a very nice moment.”
Perk was diagnosed with retinitis pigmentosa as a child and had been blind since early adulthood. He has been able to use the implant placed into his retina in 2013 to help identify street crossings, and even ski and pursue archery. A video posted by the company that designed and manufactured the device indicates he’s a good shot.
Less black-and-white has been the journey Perk and others have been on after they were implanted with the Argus II, a second-generation device created by a Los Angeles-based company called Second Sight Medical Devices.
The Argus II uses the implant and a video camera embedded in a special pair of glasses to provide limited vision to those with retinitis pigmentosa, a genetic disease that causes cells in the retina to deteriorate. The camera feeds information to the implant, which sends electrical impulses into the retina to recapitulate what the camera sees. The impulses appear in the Argus II as a 60-pixel grid of blacks, grays and whites in the user’s eye that can render rough outlines of objects and their motion.
Smartphone and computer manufacturers typically stop issuing software upgrades to their devices after two or three years, eventually rendering them bricks. But is the smartphone approach acceptable for a device that helps restore the most crucial sense a human being possesses?
Ross Doerr, a retired disability rights attorney in Maine who received an Argus II in 2019, describes the field of vision as the equivalent of an index card held at arm’s length. Perk often brings objects close to his face to decipher them. Moreover, users must swivel their heads to take in visual data; moving their eyeballs does not work.
Despite its limitations, the Argus II beats the alternative. Perk no longer relies on his guide dog. Doerr was uplifted when he was able to see the outlines of Christmas trees at a holiday show.
“The fairy godmother department sort of reaches out and taps you on the shoulder once in a while,” Doerr says of his implant, which came about purely by chance. A surgeon treating his cataracts was partnered with the son of another surgeon who was implanting the devices, and he was referred.
Doerr had no reason to believe the shower of fairy dust wouldn’t continue. Second Sight held out promises that the Argus II recipients’ vision would gradually improve through upgrades to much higher pixel densities. The ability to recognize individual faces was even touted as a possibility. In the winter of 2020, Doerr was preparing to travel across the U.S. to Second Sight’s headquarters to receive an upgrade. But then COVID-19 descended, and the trip was canceled.
The pandemic also hit Second Sight’s bottom line. Doerr found out about its tribulations only from one of the company’s vision therapists, who told him the entire department was being laid off. Second Sight cut nearly 80% of its workforce in March 2020 and announced it would wind down operations.

Ross Doerr has mostly stopped using his Argus II, the result of combination of fear of losing its assistance from wear and tear and disdain for the company that brought it to market.
Jan Doerr
Second Sight’s implosion left some 350 Argus recipients in the metaphorical dark about what to do if their implants failed. Skeleton staff seem to have rarely responded to queries from their customers, at least based on the experiences of Perk and Doerr. And some recipients have unfortunately returned to the actual dark as well, as reports have surfaced of Argus II failures due to aging or worn-down parts.
Product support for complex products is remarkably uneven. Although the iconic Ford Mustang ceased production in the late 1960s, its parts market is so robust that it’s theoretically possible to assemble a new vehicle from recently crafted components. Conversely, smartphone and computer manufacturers typically stop issuing software upgrades to their devices after two or three years, eventually rendering them bricks. Consumers have accepted both extremes.
But is the smartphone approach acceptable for a device that helps restore the most crucial sense a human being possesses?
Margaret McLean, a senior fellow at the Markkula Center for Applied Ethics at Santa Clara University in California, notes companies like Second Sight have a greater obligation for product support than other consumer product ventures.
“In this particular case, you have a great deal of risk that is involved in using this device, the implant, and the after care of this device,” she says. “You cannot, like with your car, decide that ‘I don’t like my Mustang anymore,’ and go out and buy a Corvette.”
And, whether the Argus II implant works or not, its physical presence can impact critical medical decisions. Doerr’s doctor wanted him to undergo an MRI to assist in diagnosing attacks of vertigo. But the physician was concerned his implant might interfere. With the latest available manufacturer advisories on his implant nearly a decade old, the procedure was held up. Doerr spent months importuning Second Sight through phone calls, emails and Facebook postings to learn if his implant was contraindicated with MRIs, which he never received. Although the cause of his vertigo was found without an MRI, Doerr was hardly assured.
“Put that into context for a minute. I get into a serious car accident. I end up in the emergency room, and I have a tag saying I have an implanted medical device,” he says. “You can’t do an MRI until you get the proper information from the company. Who’s going to answer the phone?”
Second Sight’s management did answer the call to revamp its business. It netted nearly $78 million through a private stock placement and an initial public offering last year. At the end of 2021, Second Sight had nearly $70 million in cash on hand, according to a recent filing with the Securities and Exchange Commission.
And while the Argus II is still touted at length on Second Sight’s home page, it appears little of its corporate coffers are earmarked toward its support. These days, the company is focused on obtaining federal approvals for Orion, a new implant that would go directly into the recipient’s brain and could be used to remedy blindness from a variety of causes. It obtained a $6.4 million grant from the National Institutes of Health in May 2021 to help develop Orion.
Presented with a list of written questions by email, Second Sight’s spokesperson, Dave Gentry of the investor relations firm Red Chip Companies, copied a subordinate with an abrupt message to “please handle.” That was the only response from a company representative. A call to Second Sight acting chief executive officer Scott Dunbar went unreturned.
Whether or not the Orion succeeds remains to be seen. The company’s SEC filings suggest a viable and FDA-approved device is years away, and that operational losses are expected for the “foreseeable future.” Second Sight reported zero revenue in 2020 or 2021.
Moreover, the experiences of the Argus II recipients could color the reception of future Second Sight products. Doerr notes that his insurer paid nearly $500,000 to implant his device and for training on how to use it.
“What’s the insurance industry going to say the next time this crops up?” Doerr asks, noting that the company’s reputation is “completely shot” with the recipients of its implants.
Perk, who made speeches to praise the Argus II and is still featured in a video on the Second Sight website, says he also no longer supports the company.

Jeroen Perk, an investigator for the Dutch customs service, cried for joy after partially regaining his sight, but he no longer trusts Second Sight, the company that provided his implant.
Nanda Perk
Nevertheless, Perk remains highly reliant on the technology. When he dropped an external component of his device in late 2020 and it broke, Perk briefly debated whether to remain blind or find a way to get his Argus II working again. Three months later, he was able to revive it by crowdsourcing parts, primarily from surgeons with spare components or other Argus II recipients who no longer use their devices. Perk now has several spare parts in reserve in case of future breakdowns.
Despite the frantic efforts to retain what little sight he has, Perk has no regrets about having the device implanted. And while he no longer trusts Second Sight, he is looking forward to possibly obtaining more advanced implants from companies in the Netherlands and Australia working on their own products.
Doerr suggests that biotech firms whose implants are distributed globally be bound to some sort of international treaty requiring them to service their products in perpetuity. Such treaties are still applied to the salvage rights for ships that sunk centuries ago, he notes.
“I think that in a global tech economy, that would be a good thing,” says McLean, the fellow at Santa Clara, “but I am not optimistic about it in the near term. Business incentives push toward return on share to stockholders, not to patients and other stakeholders. We likely need to rely on some combination of corporately responsibility…and [international] government regulation. It’s tough—the Paris Climate Accord implementation at a slow walk comes to mind.”
Unlike Perk, Doerr has mostly stopped using his Argus II, the result of combination of fear of losing its assistance from wear and tear and disdain for the company that brought it to market. At 70, Doerr says he does not have the time or energy to hold the company more accountable. And with Second Sight having gone through a considerable corporate reorganization, Doerr believes a lawsuit to compel it to better serve its Argus recipients would be nothing but an extremely costly longshot.
“It’s corporate America at its best,” he observes.

