Scientists Are Devising Clever Solutions to Feed Astronauts on Mars Space Flights

Astronaut and Expedition 64 Flight Engineer Soichi Noguchi of the Japan Aerospace Exploration Agency displays Extra Dwarf Pak Choi plants growing aboard the International Space Station. The plants were grown for the Veggie study which is exploring space agriculture as a way to sustain astronauts on future missions to the Moon or Mars.
Astronauts at the International Space Station today depend on pre-packaged, freeze-dried food, plus some fresh produce thanks to regular resupply missions. This supply chain, however, will not be available on trips further out, such as the moon or Mars. So what are astronauts on long missions going to eat?
Going by the options available now, says Christel Paille, an engineer at the European Space Agency, a lunar expedition is likely to have only dehydrated foods. “So no more fresh product, and a limited amount of already hydrated product in cans.”
For the Mars mission, the situation is a bit more complex, she says. Prepackaged food could still constitute most of their food, “but combined with [on site] production of certain food products…to get them fresh.” A Mars mission isn’t right around the corner, but scientists are currently working on solutions for how to feed those astronauts. A number of boundary-pushing efforts are now underway.
The logistics of growing plants in space, of course, are very different from Earth. There is no gravity, sunlight, or atmosphere. High levels of ionizing radiation stunt plant growth. Plus, plants take up a lot of space, something that is, ironically, at a premium up there. These and special nutritional requirements of spacefarers have given scientists some specific and challenging problems.
To study fresh food production systems, NASA runs the Vegetable Production System (Veggie) on the ISS. Deployed in 2014, Veggie has been growing salad-type plants on “plant pillows” filled with growth media, including a special clay and controlled-release fertilizer, and a passive wicking watering system. They have had some success growing leafy greens and even flowers.
"Ideally, we would like a system which has zero waste and, therefore, needs zero input, zero additional resources."
A larger farming facility run by NASA on the ISS is the Advanced Plant Habitat to study how plants grow in space. This fully-automated, closed-loop system has an environmentally controlled growth chamber and is equipped with sensors that relay real-time information about temperature, oxygen content, and moisture levels back to the ground team at Kennedy Space Center in Florida. In December 2020, the ISS crew feasted on radishes grown in the APH.
“But salad doesn’t give you any calories,” says Erik Seedhouse, a researcher at the Applied Aviation Sciences Department at Embry-Riddle Aeronautical University in Florida. “It gives you some minerals, but it doesn’t give you a lot of carbohydrates.” Seedhouse also noted in his 2020 book Life Support Systems for Humans in Space: “Integrating the growing of plants into a life support system is a fiendishly difficult enterprise.” As a case point, he referred to the ESA’s Micro-Ecological Life Support System Alternative (MELiSSA) program that has been running since 1989 to integrate growing of plants in a closed life support system such as a spacecraft.
Paille, one of the scientists running MELiSSA, says that the system aims to recycle the metabolic waste produced by crew members back into the metabolic resources required by them: “The aim is…to come [up with] a closed, sustainable system which does not [need] any logistics resupply.” MELiSSA uses microorganisms to process human excretions in order to harvest carbon dioxide and nitrate to grow plants. “Ideally, we would like a system which has zero waste and, therefore, needs zero input, zero additional resources,” Paille adds.
Microorganisms play a big role as “fuel” in food production in extreme places, including in space. Last year, researchers discovered Methylobacterium strains on the ISS, including some never-seen-before species. Kasthuri Venkateswaran of NASA’s Jet Propulsion Laboratory, one of the researchers involved in the study, says, “[The] isolation of novel microbes that help to promote the plant growth under stressful conditions is very essential… Certain bacteria can decompose complex matter into a simple nutrient [that] the plants can absorb.” These microbes, which have already adapted to space conditions—such as the absence of gravity and increased radiation—boost various plant growth processes and help withstand the harsh physical environment.
MELiSSA, says Paille, has demonstrated that it is possible to grow plants in space. “This is important information because…we didn’t know whether the space environment was affecting the biological cycle of the plant…[and of] cyanobacteria.” With the scientific and engineering aspects of a closed, self-sustaining life support system becoming clearer, she says, the next stage is to find out if it works in space. They plan to run tests recycling human urine into useful components, including those that promote plant growth.
The MELiSSA pilot plant uses rats currently, and needs to be translated for human subjects for further studies. “Demonstrating the process and well-being of a rat in terms of providing water, sufficient oxygen, and recycling sufficient carbon dioxide, in a non-stressful manner, is one thing,” Paille says, “but then, having a human in the loop [means] you also need to integrate user interfaces from the operational point of view.”
Growing food in space comes with an additional caveat that underscores its high stakes. Barbara Demmig-Adams from the Department of Ecology and Evolutionary Biology at the University of Colorado Boulder explains, “There are conditions that actually will hurt your health more than just living here on earth. And so the need for nutritious food and micronutrients is even greater for an astronaut than for [you and] me.”
Demmig-Adams, who has worked on increasing the nutritional quality of plants for long-duration spaceflight missions, also adds that there is no need to reinvent the wheel. Her work has focused on duckweed, a rather unappealingly named aquatic plant. “It is 100 percent edible, grows very fast, it’s very small, and like some other floating aquatic plants, also produces a lot of protein,” she says. “And here on Earth, studies have shown that the amount of protein you get from the same area of these floating aquatic plants is 20 times higher compared to soybeans.”
Aquatic plants also tend to grow well in microgravity: “Plants that float on water, they don’t respond to gravity, they just hug the water film… They don’t need to know what’s up and what’s down.” On top of that, she adds, “They also produce higher concentrations of really important micronutrients, antioxidants that humans need, especially under space radiation.” In fact, duckweed, when subjected to high amounts of radiation, makes nutrients called carotenoids that are crucial for fighting radiation damage. “We’ve looked at dozens and dozens of plants, and the duckweed makes more of this radiation fighter…than anything I’ve seen before.”
Despite all the scientific advances and promising leads, no one really knows what the conditions so far out in space will be and what new challenges they will bring. As Paille says, “There are known unknowns and unknown unknowns.”
One definite “known” for astronauts is that growing their food is the ideal scenario for space travel in the long term since “[taking] all your food along with you, for best part of two years, that’s a lot of space and a lot of weight,” as Seedhouse says. That said, once they land on Mars, they’d have to think about what to eat all over again. “Then you probably want to start building a greenhouse and growing food there [as well],” he adds.
And that is a whole different challenge altogether.
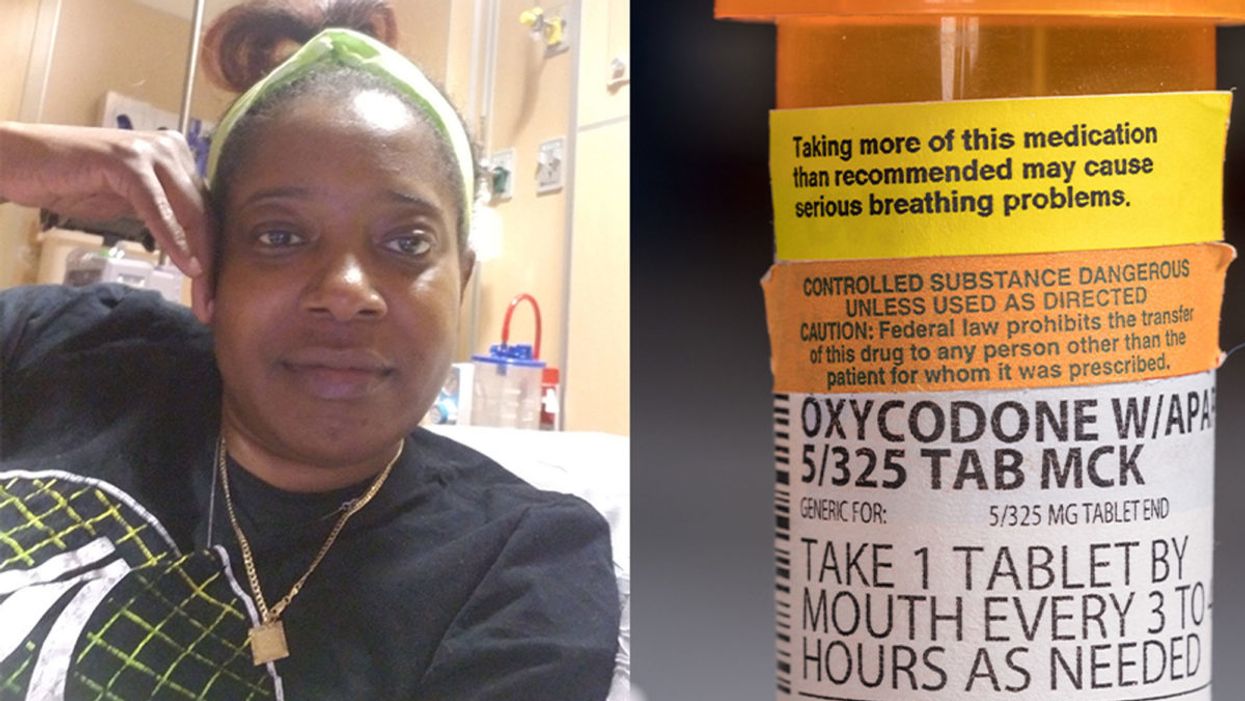
A New Test Aims to Objectively Measure Pain. It Could Help Legitimate Sufferers Access the Meds They Need.
Sickle cell patient Bridgett Willkie found herself being labeled an addict when she sought an opioid prescription to control her pain.
"That throbbing you feel for the first minute after a door slams on your finger."
This is how Central Florida resident Bridgett Willkie describes the attacks of pain caused by her sickle cell anemia – a genetic blood disorder in which a patient's red blood cells become shaped like sickles and get stuck in blood vessels, thereby obstructing the flow of blood and oxygen.
"I found myself being labeled as an addict and I never was."
Willkie's lifelong battle with the condition has led to avascular necrosis in both of her shoulders, hips, knees and ankles. This means that her bone tissue is dying due to insufficient blood supply (sickle cell anemia is among the medical conditions that can decrease blood flow to one's bones).
"That adds to the pain significantly," she says. "Every time my heart beats, it hurts. And the pain moves. It follows the path of circulation. I liken it to a traffic jam in my veins."
For more than a decade, she received prescriptions for Oxycontin. Then, four years ago, her hematologist – who had been her doctor for 18 years – suffered a fatal heart attack. She says her longtime doctor's replacement lacked experience treating sickle cell patients and was uncomfortable writing her a prescription for opioids. What's more, this new doctor wanted to place her in a drug rehab facility.
"Because I refused to go, he stopped writing my scripts," she says. The ensuing three months were spent at home, detoxing. She describes the pain as unbearable. "Sometimes I just wanted to die."
One of the effects of the opioid epidemic is that many legitimate pain patients have seen their opioids significantly reduced or downright discontinued because of their doctors' fears of over-prescribing addictive medications.
"I found myself being labeled as an addict and I never was...Being treated like a drug-seeking patient is degrading and humiliating," says Willkie, who adds that when she is at the hospital, "it's exhausting arguing with the doctors...You dread them making their rounds because every day they come in talking about weaning you off your meds."
Situations such as these are fraught with tension between patients and doctors, who must remain wary about the risk of over-prescribing powerful and addictive medications. Adding to the complexity is that it can be very difficult to reliably assess a patient's level of physical pain.
However, this difficulty may soon decline, as Indiana University School of Medicine researchers, led by Dr. Alexander B. Niculescu, have reportedly devised a way to objectively assess physical pain by analyzing biomarkers in a patient's blood sample. The results of a study involving more than 300 participants were published earlier this year in the journal Molecular Psychiatry.
Niculescu – who is both a professor of psychiatry and medical neuroscience at the IU School of Medicine – explains that, when someone is in severe physical pain, a blood sample will show biomarkers related to intracellular adhesion and cell-signaling mechanisms. He adds that some of these biomarkers "have prior convergent evidence from animal or human studies for involvement in pain."
Aside from reliably measuring pain severity, Niculescu says blood biomarkers can measure the degree of one's response to treatment and also assess the risk of future recurrences of pain. He believes this new method's greatest benefit, however, might be the ability to identify a number of non-opioid medications that a particular patient is likely to respond to, based on his or her biomarker profile.
Clearly, such a method could be a gamechanger for pain patients and the professionals who treat them. As of yet, health workers have been forced to make crucial decisions based on their clinical impressions of patients; such impressions are invariably subjective. A method that enables people to prove the extent of their pain could remove the stigma that many legitimate pain patients face when seeking to obtain their needed medicine. It would also improve their chances of receiving sufficient treatment.
Niculescu says it's "theoretically possible" that there are some conditions which, despite being severe, might not reveal themselves through his testing method. But he also says that, "even if the same molecular markers that are involved in the pain process are not reflected in the blood, there are other indirect markers that should reflect the distress."
Niculescu expects his testing method will be available to the medical community at large within one to three years.
Willkie says she would welcome a reliable pain assessment method. Well-aware that she is not alone in her plight, she has more than 500 Facebook friends with sickle cell disease, and she says that "all of their opioid meds have been restricted or cut" as a result of the opioid crisis. Some now feel compelled to find their opioids "on the streets." She says she personally has never obtained opioids this way. Instead, she relies on marijuana to mitigate her pain.
Niculescu expects his testing method will be available to the medical community at large within one to three years: "It takes a while for things to translate from a lab setting to a commercial testing arena."
In the meantime, for Willkie and other patients, "we have to convince doctors and nurses that we're in pain."
Some people can eat red meat without negative health consequences, which may be due to variability between people's gut microbes.
In different countries' national dietary guidelines, red meats (beef, pork, and lamb) are often confined to a very small corner. Swedish officials, for example, advise the population to "eat less red and processed meat". Experts in Greece recommend consuming no more than four servings of red meat — not per week, but per month.
"Humans 100% rely on the microbes to digest this food."
Yet somehow, the matter is far from settled. Quibbles over the scientific evidence emerge on a regular basis — as in a recent BMJ article titled, "No need to cut red meat, say new guidelines." News headlines lately have declared that limiting red meat may be "bad advice," while carnivore diet enthusiasts boast about the weight loss and good health they've achieved on an all-meat diet. The wildly successful plant-based burgers? To them, a gimmick. The burger wars are on.
Nutrition science would seem the best place to look for answers on the health effects of specific foods. And on one hand, the science is rather clear: in large populations, people who eat more red meat tend to have more health problems, including cardiovascular disease, colorectal cancer, and other conditions. But this sort of correlational evidence fails to settle the matter once and for all; many who look closely at these studies cite methodological shortcomings and a low certainty of evidence.
Some scientists, meanwhile, are trying to cut through the noise by increasing their focus on the mechanisms: exactly how red meat is digested and the step-by-step of how this affects human health. And curiously, as these lines of evidence emerge, several of them center around gut microbes as active participants in red meat's ultimate effects on human health.
Dr. Stanley Hazen, researcher and medical director of preventive cardiology at Cleveland Clinic, was one of the first to zero in on gut microorganisms as possible contributors to the health effects of red meat. In looking for chemical compounds in the blood that could predict the future development of cardiovascular disease, his lab identified a molecule called trimethylamine-N-oxide (TMAO). Little by little, he and his colleagues began to gather both human and animal evidence that TMAO played a role in causing heart disease.
Naturally, they tried to figure out where the TMAO came from. Hazen says, "We found that animal products, and especially red meat, were a dietary source that, [along with] gut microbes, would generate this product that leads to heart disease development." They observed that the gut microbes were essential for making TMAO out of dietary compounds (like red meat) that contained its precursor, trimethylamine (TMA).
So in linking red meat to cardiovascular disease through TMAO, the surprising conclusion, says Hazen, was that, "Without a doubt, [the microbes] are the most important aspect of the whole pathway."
"I think it's just a matter of time [before] we will have therapeutic interventions that actually target our gut microbes, just like the way we take drugs that lower cholesterol levels."
Other researchers have taken an interest in different red-meat-associated health problems, like colorectal cancer and the inflammation that accompanies it. This was the mechanistic link tackled by the lab of professor Karsten Zengler of the UC San Diego Departments of Pediatrics and Bioengineering—and it also led straight back to the gut microbes.
Zengler and colleagues recently published a paper in Nature Microbiology that focused on the effects of a red meat carbohydrate (or sugar) called Neu5Gc.
He explains, "If you eat animal proteins in your diet… the bound sugars in your diet are cleaved off in your gut and they get recycled. Your own cells will not recognize between the foreign sugars and your own sugars, because they look almost identical." The unsuspecting human cells then take up these foreign sugars — spurring antibody production and creating inflammation.
Zengler showed, however, that gut bacteria use enzymes to cleave off the sugar during digestion, stopping the inflammation and rendering the sugar harmless. "There's no enzyme in the human body that can cleave this [sugar] off. Humans 100% rely on the microbes to digest this food," he says.
Both researchers are quick to caution that the health effects of diet are complex. Other work indicates, for example, that while intake of red meat can affect TMAO levels, so can intake of fish and seafood. But these new lines of evidence could help explain why some people, ironically, seem to be in perfect health despite eating a lot of red meat: their ideal frequency of meat consumption may depend on their existing community of gut microbes.
"It helps explain what accounts for inter-person variability," Hazen says.
These emerging mechanisms reinforce overall why it's prudent to limit red meat, just as the nutritional guidelines advised in the first place. But both Hazen and Zengler predict that interventions to buffer the effects of too many ribeyes may be just around the corner.
Zengler says, "Our idea is that you basically can help your own digestive system detoxify these inflammatory compounds in meat, if you continue eating red meat or you want to eat a high amount of red meat." A possibly strategy, he says, is to use specific pre- or probiotics to cultivate an inflammation-reducing gut microbial community.
Hazen foresees the emergence of drugs that act not on the human, but on the human's gut microorganisms. "I think it's just a matter of time [before] we will have therapeutic interventions that actually target our gut microbes, just like the way we take drugs that lower cholesterol levels."
He adds, "It's a matter of 'stay tuned', I think."