Can You Trust Your Gut for Food Advice?
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.

Which foods are actually healthy for your individual gut microbiome? Several companies are offering personalized dietary guidance based on your test results, but their answers in one experiment turned up with some conflicting advice.
I recently got on the scale to weigh myself, thinking I've got to eat better. With so many trendy diets today claiming to improve health, from Keto to Paleo to Whole30, it can be confusing to figure out what we should and shouldn't eat for optimal nutrition.
A number of companies are now selling the concept of "personalized" nutrition based on the genetic makeup of your individual gut bugs.
My next thought was: I've got to lose a few pounds.
Consider a weird factoid: In addition to my fat, skin, bone and muscle, I'm carrying around two or three pounds of straight-up bacteria. Like you, I am the host to trillions of micro-organisms that live in my gut and are collectively known as my microbiome. An explosion of research has occurred in the last decade to try to understand exactly how these microbial populations, which are unique to each of us, may influence our overall health and potentially even our brains and behavior.
Lots of mysteries still remain, but it is established that these "bugs" are crucial to keeping our body running smoothly, performing functions like stimulating the immune system, synthesizing important vitamins, and aiding digestion. The field of microbiome science is evolving rapidly, and a number of companies are now selling the concept of "personalized" nutrition based on the genetic makeup of your individual gut bugs. The two leading players are Viome and DayTwo, but the landscape includes the newly launched startup Onegevity Health and others like Thryve, which offers customized probiotic supplements in addition to dietary recommendations.
The idea has immediate appeal – if science could tell you exactly what to make for lunch and what to avoid, you could forget about the fad diets and go with your own bespoke food pyramid. Wondering if the promise might be too good to be true, I decided to perform my own experiment.
Last fall, I sent the identical fecal sample to both Viome (I paid $425, but the price has since dropped to $299) and DayTwo ($349). A couple of months later, both reports finally arrived, and I eagerly opened each app to compare their recommendations.
First, I examined my results from Viome, which was founded in 2016 in Cupertino, Calif., and declares without irony on its website that "conflicting food advice is now obsolete."
I learned I have "average" metabolic fitness and "average" inflammatory activity in my gut, which are scores that the company defines based on a proprietary algorithm. But I have "low" microbial richness, with only 62 active species of bacteria identified in my sample, compared with the mean of 157 in their test population. I also received a list of the specific species in my gut, with names like Lactococcus and Romboutsia.
But none of it meant anything to me without actionable food advice, so I clicked through to the Recommendations page and found a list of My Superfoods (cranberry, garlic, kale, salmon, turmeric, watermelon, and bone broth) and My Foods to Avoid (chickpeas, kombucha, lentils, and rice noodles). There was also a searchable database of many foods that had been categorized for me, like "bell pepper; minimize" and "beef; enjoy."
"I just don't think sufficient data is yet available to make reliable personalized dietary recommendations based on one's microbiome."
Next, I looked at my results from DayTwo, which was founded in 2015 from research out of the Weizmann Institute of Science in Israel, and whose pitch to consumers is, "Blood sugar made easy. The algorithm diet personalized to you."
This app had some notable differences. There was no result about my metabolic fitness, microbial richness, or list of the species in my sample. There was also no list of superfoods or foods to avoid. Instead, the app encouraged me to build a meal by searching for foods in their database and combining them in beneficial ways for my blood sugar. Two slices of whole wheat bread received a score of 2.7 out of 10 ("Avoid"), but if combined with one cup of large curd cottage cheese, the score improved to 6.8 ("Limit"), and if I added two hard-boiled eggs, the score went up to 7.5 ("Good").
Perusing my list of foods with "Excellent" scores, I noticed some troubling conflicts with the other app. Lentils, which had been a no-no according to Viome, received high marks from DayTwo. Ditto for Kombucha. My purported superfood of cranberry received low marks. Almonds got an almost perfect score (9.7) while Viome told me to minimize them. I found similarly contradictory advice for foods I regularly eat, including navel oranges, peanuts, pork, and beets.
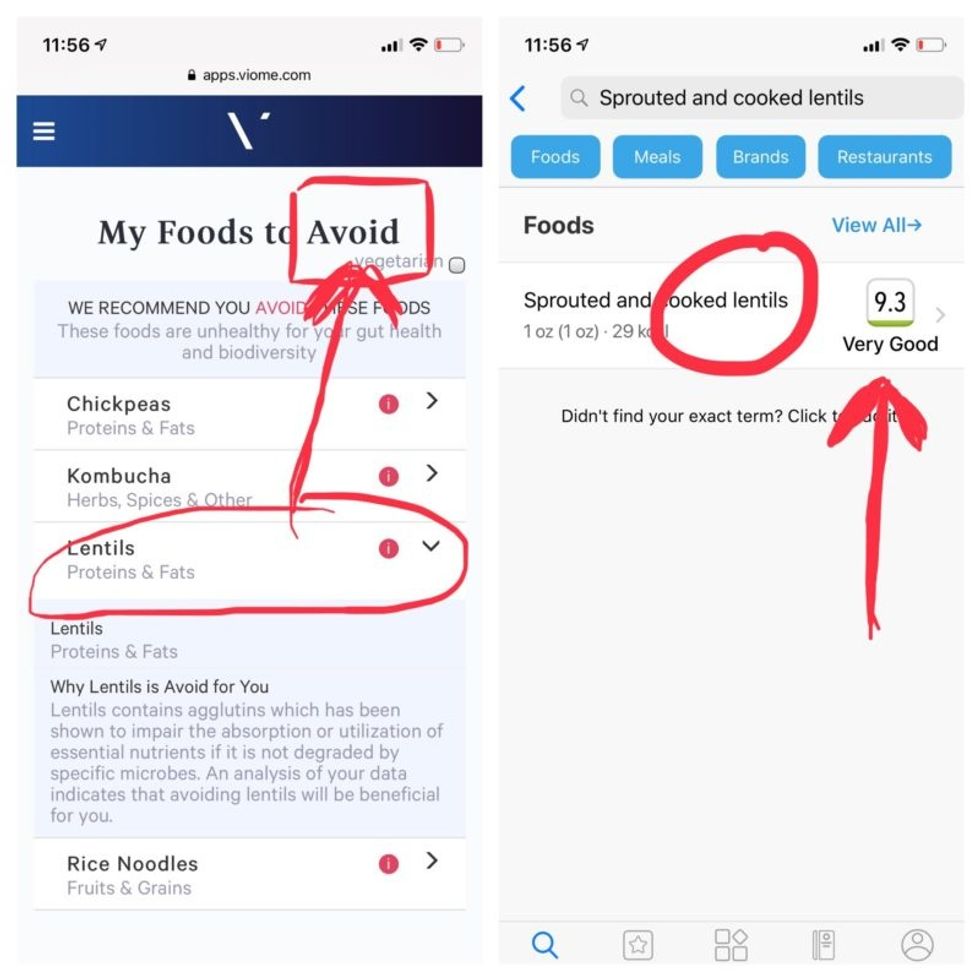
Contradictory dietary guidance that Kira Peikoff received from Viome (left) and DayTwo from an identical sample.
To be sure, there was some overlap. Both apps agreed on rice noodles (bad), chickpeas (bad), honey (bad), carrots (good), and avocado (good), among other foods.
But still, I was left scratching my head. Which set of recommendations should I trust, if either? And what did my results mean for the accuracy of this nascent field?
I called a couple of experts to find out.
"I have worked on the microbiome and nutrition for the last 20 years and I would be absolutely incapable of finding you evidence in the scientific literature that lentils have a detrimental effect based on the microbiome," said Dr. Jens Walter, an Associate Professor and chair for Nutrition, Microbes, and Gastrointestinal Health at the University of Alberta. "I just don't think sufficient data is yet available to make reliable personalized dietary recommendations based on one's microbiome. And even if they would have proprietary algorithms, at least one of them is not doing it right."
There is definite potential for personalized nutrition based on the microbiome, he said, but first, predictive models must be built and standardized, then linked to clinical endpoints, and tested in a large sample of healthy volunteers in order to enable extrapolations for the general population.
"It is mindboggling what you would need to do to make this work," he observed. "There are probably hundreds of relevant dietary compounds, then the microbiome has at least a hundred relevant species with a hundred or more relevant genes each, then you'd have to put all this together with relevant clinical outcomes. And there's a hundred-fold variation in that information between individuals."
However, Walter did acknowledge that the companies might be basing their algorithms on proprietary data that could potentially connect all the dots. I reached out to them to find out.
Amir Golan, the Chief Commercial Officer of DayTwo, told me, "It's important to emphasize this is a prediction, as the microbiome field is in a very early stage of research." But he added, "I believe we are the only company that has very solid science published in top journals and we can bring very actionable evidence and benefit to our uses."
He was referring to pioneering work out of the Weizmann Institute that was published in 2015 in the journal Cell, which logged the glycemic responses of 800 people in response to nearly 50,000 meals; adding information about the subjects' microbiomes enabled more accurate glycemic response predictions. Since then, Golan said, additional trials have been conducted, most recently with the Mayo Clinic, to duplicate the results, and other studies are ongoing whose results have not yet been published.
He also pointed out that the microbiome was merely one component that goes into building a client's profile, in addition to medical records, including blood glucose levels. (I provided my HbA1c levels, a measure of average blood sugar over the previous several months.)
"We are not saying we want to improve your gut microbiome. We provide a dynamic tool to help guide what you should eat to control your blood sugar and think about combinations," he said. "If you eat one thing, or with another, it will affect you in a different way."
Viome acknowledged that the two companies are taking very different approaches.
"DayTwo is primarily focused on the glycemic response," Naveen Jain, the CEO, told me. "If you can only eat butter for rest of your life, you will have no glycemic response but will probably die of a heart attack." He laughed. "Whereas we came from very different angle – what is happening inside the gut at a microbial level? When you eat food like spinach, how will that be metabolized in the gut? Will it produce the nutrients you need or cause inflammation?"
He said his team studied 1000 people who were on continuous glucose monitoring and fed them 45,000 meals, then built a proprietary data prediction model, looking at which microbes existed and how they actively broke down the food.
Jain pointed out that DayTwo sequences the DNA of the microbes, while Viome sequences the RNA – the active expression of DNA. That difference, in his opinion, is key to making accurate predictions.
"DNA is extremely stable, so when you eat any food and measure the DNA [in a fecal sample], you get all these false positives--you get DNA from plant food and meat, and you have no idea if those organisms are dead and simply transient, or actually exist. With RNA, you see what is actually alive in the gut."
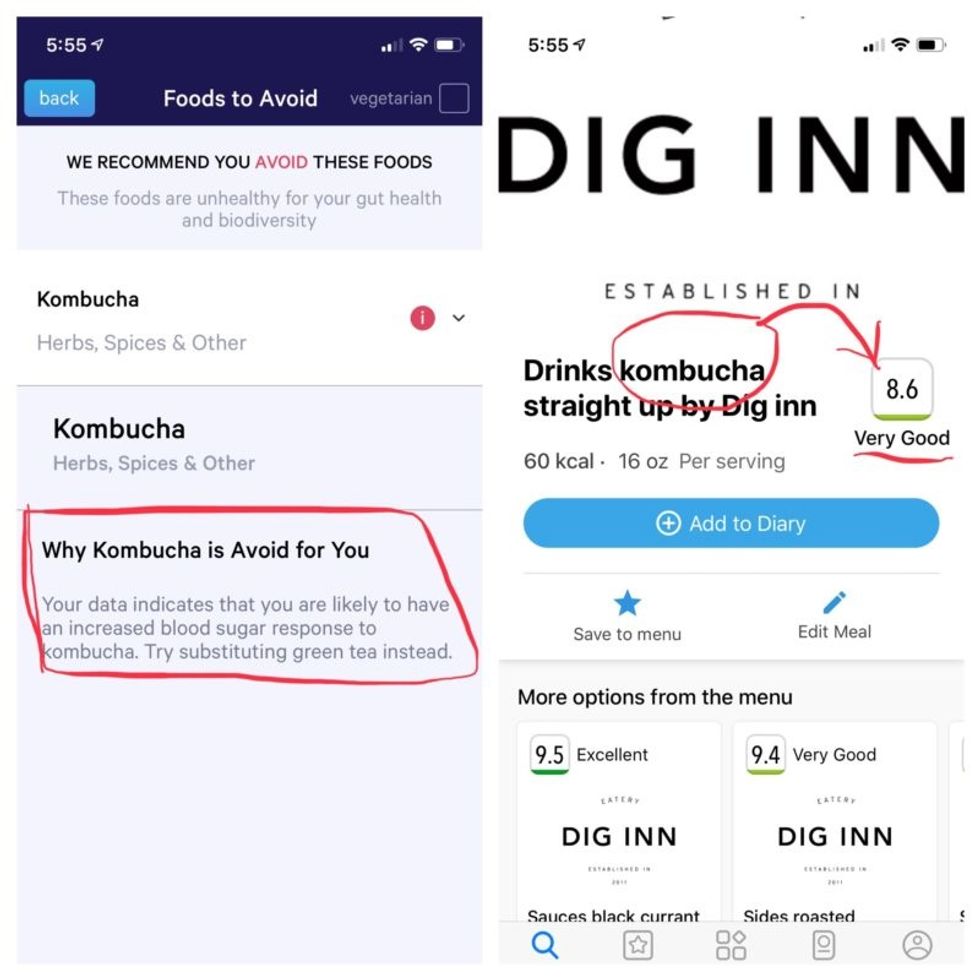
More contradictory food advice from Viome (left) and DayTwo.
Note that controversy exists over how it is possible with a fecal sample to effectively measure RNA, which degrades within minutes, though Jain said that his company has the technology to keep RNA stable for fourteen days.
Viome's approach, Jain maintains, is 90 percent accurate, based on as-yet unpublished data; a patent was filed just last week. DayTwo's approach is 66 percent accurate according to the latest published research.
Natasha Haskey, a registered dietician and doctoral student conducting research in the field of microbiome science and nutrition, is skeptical of both companies. "We can make broad statements, like eat more fruits and vegetables and fiber, but when it comes to specific foods, the science is just not there yet," she said. "I think there is a future, and we will be doing that someday, but not yet. Maybe we will be closer in ten years."
Professor Walter wholeheartedly agrees with Haskey, and suggested that if people want to eat a gut-healthy diet, they should focus on beneficial oils, fruits and vegetables, fish, a variety of whole grains, poultry and beans, and limit red meat and cheese, as well as avoid processed meats.
"These services are far over the tips of their science skis," Arthur Caplan, the founding head of New York University's Division of Medical Ethics, said in an email. "We simply don't know enough about the gut microbiome, its fluctuations and variability from person to person to support general [direct-to-consumer] testing. This is simply premature. We need standards for accuracy, specificity, and sensitivity, plus mandatory competent counseling for all such testing. They don't exist. Neither should DTC testing—yet."
Meanwhile, it's time for lunch. I close out my Viome and DayTwo apps and head to the kitchen to prepare a peanut butter sandwich. My gut tells me I'll be just fine.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
Tapping into the Power of the Placebo Effect
When Wayne Jonas was in medical school 40 years ago, doctors would write out a prescription for placebos, spelling it out backwards in capital letters, O-B-E-C-A-L-P. The pharmacist would fill the prescription with a sugar pill, recalls Jonas, now director of integrative health programs at the Samueli Foundation. It fulfilled the patient's desire for the doctor to do something when perhaps no drug could help, and the sugar pills did no harm.
Today, that deception is seen as unethical. But time and time again, studies have shown that placebos can have real benefits. Now, researchers are trying to untangle the mysteries of placebo effect in an effort to better treat patients.
The use of placebos took off in the post-WWII period, when randomized controlled clinical trials became the gold standard for medical research. One group in a study would be treated with a placebo, a supposedly inert pill or procedure that would not affect normal healing and recovery, while another group in the study would receive an "active" component, most commonly a pill under investigation. Presumably, the group receiving the active treatment would have a better response and the difference from the placebo group would represent the efficacy of the drug being tested. That was the basis for drug approval by the U.S. Food and Drug Administration.
"Placebo responses were marginalized," says Ted Kaptchuk, director of the Program in Placebo Studies & Therapeutic Encounters at Harvard Medical School. "Doctors were taught they have to overcome it when they were thinking about using an effective drug."
But that began to change around the turn of the 21st century. The National Institutes of Health held a series of meetings to set a research agenda and fund studies to answer some basic questions, led by Jonas who was in charge of the office of alternative medicine at the time. "People spontaneously get better all the time," says Kaptchuk. The crucial question was, is the placebo effect real? Is it more than just spontaneous healing?
Brain mechanisms
A turning point came in 2001 in a paper in Science that showed physical evidence of the placebo effect. It used positron emission tomography (PET) scans to measure release patterns of dopamine — a chemical messenger involved in how we feel pleasure — in the brains of patients with Parkinson's disease. Surprisingly, the placebo activated the same patterns that were activated by Parkinson's drugs, such as levodopa. It proved the placebo effect was real; now the search was on to better understand and control it.
A key part of the effect can be the beliefs, expectations, context, and "rituals" of the encounter between doctor and patient. Belief by the doctor and patient that the treatment would work, and the formalized practices of administering the treatment can all contribute to a positive outcome.
Conditioning can be another important component in generating a response, as Pavlov demonstrated more than a century ago in his experiments with dogs. They were trained with a bell prior to feeding such that they would begin to salivate in anticipation at the sound of a bell even with no food present.
Translating that to humans, studies with pain medications and sleeping aids showed that patients who had a positive response with a certain dose of those medications could have the same response if the doses was reduced and a dummy pill substituted, even to the point where there was no longer any active ingredient.
Researchers think placebo treatments can work particularly well in helping people deal with pain and psychological disorders.
Those types of studies troubled Kaptchuk because they often relied on deception; patients weren't told they were receiving a placebo, or at best there was a possibility that they might be randomized to receive a placebo. He believed the placebo effect could work even if patients were told upfront that they were going to receive a placebo. More than a dozen so call "open-label placebo" studies across numerous medical conditions, by Kaptchuk and others, have shown that you don't have to lie to patients for a placebo to work.
Jonas likes to tell the story of a patient who used methotrexate, a potent immunosuppressant, to control her rheumatoid arthritis. She was planning a long trip and didn't want to be bothered with the injections and monitoring required in using the drug, So she began to drink a powerful herbal extract of anise, a licorice flavor that she hated, prior to each injection. She reduced the amount of methotrexate over a period of months and finally stopped, but continued to drink the anise. That process had conditioned her body "to alter her immune function and her autoimmunity" as if she were taking the drug, much like Pavlov's dogs had been trained. She has not taken methotrexate for more than a year.
An intriguing paper published in May 2021 found that mild, non-invasive electric stimulation to the brain could not only boost the placebo effect on pain but also reduce the "nocebo" effect — when patients report a negative effect to a sham treatment. While the work is very preliminary, it may open the door to directly manipulating these responses.
Researchers think placebo treatments can work particularly well in helping people deal with pain and psychological disorders, areas where drugs often are of little help. Still, placebos aren't a cure and only a portion of patients experience a placebo effect.
Nocebo
If medicine were a soap opera, the nocebo would be the evil twin of the placebo. It's what happens when patients have adverse side effects because of the expectation that they will. It's commonly seem when patients claims to experience pain or gastric distress that can occur with a drug even when they've received a placebo. The side effects were either imagined or caused by something else.
"Up to 97% of reported pharmaceutical side effects are not caused by the drug itself but rather by nocebo effects and symptom misattribution," according to one 2019 paper.
One way to reduce a nocebo response is to simply not tell patients that specific side effects might occur. An example is a liver biopsy, in which a large-gauge needle is used to extract a tissue sample for examination. Those told ahead of time that they might experience some pain were more likely to report pain and greater pain than those who weren't offered this information.
Interestingly, a nocebo response plays out in the hippocampus, a part of the brain that is never activated in a placebo response. "I think what we are dealing with with nocebo is anxiety," says Kaptchuk, but he acknowledges that others disagree.
Distraction may be another way to minimize the nocebo effect. Pediatricians are using virtual reality (VR) to engage children and distract them during routine procedures such as blood draws and changing wound dressings, and burn patients of all ages have found relief with specially created VRs.
Treatment response
Jonas argues that what we commonly call the placebo effect is misnamed and leading us astray. "The fact is people heal and that inherent healing capacity is both powerful and influenced by mental, social, and contextual factors that are embedded in every medical encounter since the idea of treatment began," he wrote in a 2019 article in the journal Frontiers in Psychiatry. "Our understanding of healing and ability to enhance it will be accelerated if we stop using the term 'placebo response' and call it what it is—the meaning response, and its special application in medicine called the healing response."
He cites evidence that "only 15% to 20% of the healing of an individual or a population comes from health care. The rest—nearly 80%—comes from other factors rarely addressed in the health care system: behavioral and lifestyle choices that people make in their daily life."
To better align treatments and maximize their effectiveness, Jonas has created HOPE (Healing Oriented Practices & Environments) Note, "a patient-guided process designed to identify the patient's values and goals in their life and for healing." Essentially, it seeks to make clear to both doctor and patient what the patient's goals are in seeking treatment. In an extreme example of terminal cancer, some patients may choose to extend life despite the often brutal treatments, while others might prefer to optimize quality of life in the remaining time that they have. It builds on practices already taught in medical schools. Jonas believes doctors and patients can use tools like these to maximize the treatment response and achieve better outcomes.
Much of the medical profession has been resistant to these approaches. Part of that is simply tradition and limited data on their effectiveness, but another very real factor is the billing process for how they are reimbursed. Jonas says a new medical billing code added this year gives doctors another way to be compensated for the extra time and effort that a more holistic approach to medicine may initially require. Other moves away from fee-for-service payments to bundling and payment for outcomes, and the integrated care provided by the Veterans Affairs, Kaiser Permanente and other groups offer longer term hope for the future of approaches that might enhance the healing response.
This article was first published by Leaps.org on July 7, 2021.
New tech helps people of all ages stay social
Sonja Bauman, 39, and Mariela Florez, 83, taking one of their regular walks in Plantation, Fla. The pair met through an online platform called Papa that provides "family on demand." (Photo by Sonja Bauman)
In March, Sonja Bauman, 39, used an online platform called Papa, which offers “family on demand,” to meet Mariela Florez, an 83-year-old retiree. Despite living with her adult children, Florez was bored and lonely when they left for work, and her recoveries from a stroke and broken hip were going slowly. That's when Bauman began visiting twice per week. They take walks, strengthening Florez’s hip, and play games like Connect Four for mental stimulation. “It’s very important for me so I don’t feel lonely all day long,” said Florez. Her memories, blurred by the stroke, are gradually returning.
Papa is one of a growing number of tech approaches that are bringing together people of all ages. In addition to platforms like Papa that connect people in real life, other startups use virtual reality and video, with some of them focusing especially on deepening social connections between the generations — relationships that support the health of older and younger people alike. “I enjoy seeing Mariela as much as she enjoys seeing me,” Bauman said.
Connecting in real life
Telehealth expert Andrew Parker founded Papa in 2017 to improve the health outcomes of older adults and families. Seniors can meet people — some their grandkids’ age — for healthy activities, while working parents find retirees to watch their children. These “Papa Pals” are provided as a benefit through Medicare, Medicaid and some employer health plans.
In 2020, Papa connected Bauman, the 39-year-old Floridian, with another woman in her mid-70s who lives alone and has very limited mobility. Bauman began driving her to doctor’s appointments and helping her with chores around the house. “When I’m not there, she doesn’t leave her apartment,” said Bauman. The two have gone to the gym together, and they walk slowly through the neighborhood, chatting so it feels less like exercise.
Parker was driven to start Papa by the problem of social isolation among seniors, exacerbated by the pandemic, but he believes users of all ages can benefit. “Many of our Pals feel more comfortable opening up with older members than their same-aged friends,” he said.
Other platforms aim for similar, in-person connections. Generation Tech unites teens with seniors for technology training. And Mon Ami, which provides case management software for aging and disability service providers, has an app that connects isolated older people with college-age volunteers.
Making new connections through video
Several new sites match you with strangers for real-time video chatting on various topics, such as finding common ground on political issues. Other video platforms focus on intergenerational connections.
S. Jay Olshansky, a gerontology professor at the University of Illinois-Chicago, recalls the first time he saw Hyunseung Lee, an 11-year-old from Seoul, through his computer screen. The kid was shy, but Olshansky, 67, encouraged him to ask questions. “Turns out, he was thirsting for this kind of interaction.”
They’d connected through Eldera, a platform that pairs mentors age 60 and up with mentees, using an algorithm, for video conversations. “The time and wisdom of older adults is the most important natural resource we can give future generations,” said Dana Griffin, Eldera's CEO. “Connecting through a screen is the opposite of social media.”
In weekly meetings, Olshansky noticed Lee’s unique interest in math. “There’s something special in you,” Olshansky told him. “How do we bring it to the surface?” He suggested Lee write a book on his favorite subject, and the preteen ran with it, cranking out 70 pages in two weeks. Lee has published his love letter to theorems on Amazon.
Hyunseung Lee, age 11, of Korea, and U.S. college professor Jay Olshanksy, 67, discuss math, strategy and Hyunsung's budding career as a book author during their video chats through a platform called Eldera. (Photo by Dana Palmer/Eldera)
Lee’s parents told Olshansky that their son has become more assertive — a recurring theme, Griffin said. “Confidence is the number one thing parents tell us about.” Since Eldera’s inception last year, the number of mentors has grown exponentially. Even so, Griffin said the waitlist for mentors typically numbers 200 kids.
Another site, Big and Mini, hosts video interactions between seniors and young adults; about 10,000 active users have joined since 2019, said co-founder Aditi Merchant.
Users often bring the benefits of their video interactions to their real-world relationships. Olshansky views Lee as an older version of his grandkids. “Eldera teaches me how to interact with them.” Lee, high on confidence, began instructing his classmates in math. Griffin noted that a group of Eldera mentors in Memphis, who met initially on Eldera, now take walks together in-person to trade ideas for helping each other’s Eldera kids solve problems in their schools and communities.
“We’ve evolved into a community for older adults who want to give back to the world,” said Griffin. Other new tools for connection take the form of virtual reality apps.
Connecting in virtual reality
During pandemic isolation, record numbers of people bought devices for virtual and augmented reality. Such gadgets can convince you that you’re hanging out with friends, even if they’re in another hemisphere. Lifelike simulations from miles away could be especially useful for meaningful interactions between people of different generations, since they’re often geographically segregated.
VR’s benefits require further study, but users report less social isolation and depression, according to MIT research. The immersive, 3-D experience is more compelling than FaceTime or Zoom. “It’s like the difference between a phone call and video call,” said Rick Robinson, Vice President of AARP’s Innovation Labs.
“When VR is designed right, the medium disappears,” said Jeremy Bailenson of Stanford.
Dana Pierce, a 56-year-old government employee in Indiana, got Meta's VR headset in May, 2021, thinking she’d enjoy it more than a new laptop. After many virtual group tours of exotic destinations, she has no regrets. Her adventures occur on Alcove, an app made by Robinson’s Innovation Labs. He co-created it with VR-company Rendever and sought input from people over age 50 to tailor it to their interests. “I’m an introvert,” said Pierce. “I’ve been more socially active since getting my headset than I am in real life.”
Tagging along with her to places like Paris are avatars representing real people around the world. She’s gotten to know VR users in their 70s, 80s and 90s, as well as younger people and some her own age. One is a new friend she plays chess with in relaxing nature settings. Another is her oldest son. He lives 90 minutes away but, earlier this year, Pierce welcomed him and his girlfriend to her virtual house on Alcove. They chatted in the living room decorated with family photos uploaded by Pierce. Then they took out a boat to go VR fishing — because why not — until 2 a.m.
“When VR is designed right, the medium disappears,” said Jeremy Bailenson, a communications professor who directs Stanford’s Virtual Human Interaction Lab. He’s teaching a class of 175 students entirely in VR. After months of covid isolation, the first time the class met, “there was a big catharsis. It really feels like you’re in a big crowd.” Like-minded people meet in VR for events such as comedy shows and creative writing meetups, while the Swedish pop group ABBA has performed this year as digital versions of themselves (“ABBA-tars”) during a virtual concert tour.
Karen Fingerman, a psychologist and director of the Texas Aging and Longevity Center at the University of Texas-Austin, supports the idea of VR for social connection, though she added that some people need it more than others. Hospitals and assisted-living facilities are using products such as Penumbra’s REAL I-Series and MyndVR to bring VR excursions to isolated patients and seniors. “If you’re in a bed or facility, this gives you something to talk about,” said Gita Barry, Penumbra’s executive vice president.
Pierce uses it on most days. She may see another adult son, who lives with her, less often as a result. But VR helps her manage real-world stressors, more than escaping them. After a long workday, she visits her back porch on Alcove, which overlooks a pond. “It’s my little retreat,” she said. “VR improves my mood. It’s added a lot to my life.”
Some seniors are using more than one technology. Olshansky and Lee discuss strategy while playing Internet chess. And Olshansky recently began using VR. He sees his sister, who lives far away, in a virtual beach house. “It’d be a great way to interact with Hyunseung,” he said. “I should get him a headset.”
A version of this article first appeared in The Washington Post on December 3, 2021.

