Scientists want the salamander's secret: how they regenerate tissue

All organisms can repair damaged tissue, but none do it better than salamanders and newts. A surprising area of science could tell us how they manage this feat - and perhaps even help us develop a similar ability.
All organisms have the capacity to repair or regenerate tissue damage. None can do it better than salamanders or newts, which can regenerate an entire severed limb.
That feat has amazed and delighted man from the dawn of time and led to endless attempts to understand how it happens – and whether we can control it for our own purposes. An exciting new clue toward that understanding has come from a surprising source: research on the decline of cells, called cellular senescence.
Senescence is the last stage in the life of a cell. Whereas some cells simply break up or wither and die off, others transition into a zombie-like state where they can no longer divide. In this liminal phase, the cell still pumps out many different molecules that can affect its neighbors and cause low grade inflammation. Senescence is associated with many of the declining biological functions that characterize aging, such as inflammation and genomic instability.
Oddly enough, newts are one of the few species that do not accumulate senescent cells as they age, according to research over several years by Maximina Yun. A research group leader at the Center for Regenerative Therapies Dresden and the Max Planck Institute of Molecular and Cell Biology and Genetics, in Dresden, Germany, Yun discovered that senescent cells were induced at some stages of regeneration of the salamander limb, “and then, as the regeneration progresses, they disappeared, they were eliminated by the immune system,” she says. “They were present at particular times and then they disappeared.”
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states.
Previous research on senescence in aging had suggested, logically enough, that applying those cells to the stump of a newly severed salamander limb would slow or even stop its regeneration. But Yun stood that idea on its head. She theorized that senescent cells might also play a role in newt limb regeneration, and she tested it by both adding and removing senescent cells from her animals. It turned out she was right, as the newt limbs grew back faster than normal when more senescent cells were included.
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states, which could then be turned into progenitors, a cell type in between stem cells and specialized cells, needed to regrow the muscle tissue of the missing limb. “We think that this ability to dedifferentiate is intrinsically a big part of why salamanders can regenerate all these very complex structures, which other organisms cannot,” she explains.
Yun sees regeneration as a two part problem. First, the cells must be able to sense that their neighbors from the lost limb are not there anymore. Second, they need to be able to produce the intermediary progenitors for regeneration, , to form what is missing. “Molecularly, that must be encoded like a 3D map,” she says, otherwise the new tissue might grow back as a blob, or liver, or fin instead of a limb.
Wound healing
Another recent study, this time at the Mayo Clinic, provides evidence supporting the role of senescent cells in regeneration. Looking closely at molecules that send information between cells in the wound of a mouse, the researchers found that senescent cells appeared near the start of the healing process and then disappeared as healing progressed. In contrast, persistent senescent cells were the hallmark of a chronic wound that did not heal properly. The function and significance of senescence cells depended on both the timing and the context of their environment.
The paper suggests that senescent cells are not all the same. That has become clearer as researchers have been able to identify protein markers on the surface of some senescent cells. The patterns of these proteins differ for some senescent cells compared to others. In biology, such physical differences suggest functional differences, so it is becoming increasingly likely there are subsets of senescent cells with differing functions that have not yet been identified.
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes.
Scientists initially thought that senescent cells couldn’t play a role in regeneration because they could no longer reproduce, says Anthony Atala, a practicing surgeon and bioengineer who leads the Wake Forest Institute for Regenerative Medicine in North Carolina. But Yun’s study points in the other direction. “What this paper shows clearly is that these cells have the potential to be involved in tissue regeneration [in newts]. The question becomes, will these cells be able to do the same in humans.”
As our knowledge of senescent cells increases, Atala thinks we need to embrace a new analogy to help understand them: humans in retirement. They “have acquired a lot of wisdom throughout their whole life and they can help younger people and mentor them to grow to their full potential. We're seeing the same thing with these cells,” he says. They are no longer putting energy into their own reproduction, but the signaling molecules they secrete “can help other cells around them to regenerate.”
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes. If so, it seems that our genes are unable to express this ability, perhaps as part of a tradeoff in acquiring other traits. It is a fertile area of research.
Dedifferentiation is likely to become an important process in the field of regenerative medicine. One extreme example: a lab has been able to turn back the clock and reprogram adult male skin cells into female eggs, a potential milestone in reproductive health. It will be more difficult to control just how far back one wishes to go in the cell's dedifferentiation – part way or all the way back into a stem cell – and then direct it down a different developmental pathway. Yun is optimistic we can learn these tricks from newts.
Senolytics
A growing field of research is using drugs called senolytics to remove senescent cells and slow or even reverse disease of aging.
“Senolytics are great, but senolytics target different types of senescence,” Yun says. “If senescent cells have positive effects in the context of regeneration, of wound healing, then maybe at the beginning of the regeneration process, you may not want to take them out for a little while.”
“If you look at pretty much all biological systems, too little or too much of something can be bad, you have to be in that central zone” and at the proper time, says Atala. “That's true for proteins, sugars, and the drugs that you take. I think the same thing is true for these cells. Why would they be different?”
Our growing understanding that senescence is not a single thing but a variety of things likely means that effective senolytic drugs will not resemble a single sledge hammer but more a carefully manipulated scalpel where some types of senescent cells are removed while others are added. Combinations and timing could be crucial, meaning the difference between regenerating healthy tissue, a scar, or worse.
New Device Can Detect Peanut Allergens on a Plate in 30 Seconds
Peanuts on a plate can be deadly for those with severe allergies, but an Israeli startup company wants to alleviate that fear.
People with life-threatening allergies live in constant fear of coming into contact with deadly allergens. Researchers estimate that about 32 million Americans have food allergies, with the most severe being milk, egg, peanut, tree nuts, wheat, soy, fish, and shellfish.
"It is important to understand that just several years ago, this would not have been possible."
Every three minutes, a food allergy reaction sends someone to the emergency room, and 200,000 people in the U.S. require emergency medical care each year for allergic reactions, according to Food Allergy Research and Education.
But what if there was a way you could easily detect if something you were about to eat contains any harmful allergens? Thanks to Israeli scientists, this will soon be the case — at least for peanuts. The team has been working to develop a handheld device called Allerguard, which analyzes the vapors in your meal and can detect allergens in 30 seconds.
Leapsmag spoke with the founder and CTO of Allerguard, Guy Ayal, about the groundbreaking technology, how it works, and when it will be available to purchase.
What prompted you to create this device? Do you have a personal connection with severe food allergies?
Guy Ayal: My eldest daughter's best friend suffers from a severe food allergy, and I experienced first-hand the effect it has on the person and their immediate surroundings. Most notable for me was the effect on the quality of life – the experience of living in constant fear. Everything we do at Allerguard is basically to alleviate some of that fear.
How exactly does the device work?
The device is built on two main pillars. The first is the nano-chemical stage, in which we developed specially attuned nanoparticles that selectively adhere only to the specific molecules that we are looking for. Those molecules, once bound to the nanoparticles, induce a change in their electrical behavior, which is measured and analyzed by the second main pillar -- highly advanced machine learning algorithms, which can surmise which molecules were collected, and thus whether or not peanuts (or in the future, other allergens) were detected.
It is important to understand that just several years ago, this would not have been possible, because both the nano-chemistry, and especially the entire world of machine learning, big data, and what is commonly known as AI only started to exist in the '90s, and reached applicability for handheld devices only in the past few years.
Where are you at in the development process and when will the device be available to consumers?
We have concluded the proof of concept and proof of capability phase, when we demonstrated successful detection of the minimal known clinical amount that may cause the slightest effect in the most severely allergic person – less than 1 mg of peanut (actually it is 0.7 mg). Over the next 18 months will be productization, qualification, and validation of our device, which should be ready to market in the latter half of 2021. The sensor will be available in the U.S., and after a year in Europe and Canada.

The Allerguard was made possible through recent advances in machine learning, big data, and AI.
(Courtesy)
How much will it cost?
Our target price is about $200 for the device, with a disposable SenseCard that will run for at least a full day and cost about $1. That card is for a specific allergen and will work for multiple scans in a day, not just one time.
[At a later stage, the company will have sensors for other allergens like tree nuts, eggs, and milk, and they'll develop a multi-SenseCard that works for a few allergens at once.]
Are there any other devices on the market that do something similar to Allerguard?
No other devices are even close to supplying the level of service that we promise. All known methods for allergen detection rely on sampling of the food, which is a viable solution for homogenous foodstuffs, such as a factory testing their raw ingredients, but not for something as heterogenous as an actual dish – especially not for solid allergens such as peanuts, treenuts, or sesame.
If there is a single peanut in your plate, and you sample from anywhere on that plate which is not where that peanut is located, you will find that your sample is perfectly clean – because it is. But the dish is not. That dish is a death trap for an allergic person. Allerguard is the only suggested solution that could indeed detect that peanut, no matter where in that plate it is hiding.
Anything else readers should know?
Our first-generation product will be for peanuts only. You have to understand, we are still a start-up company, and if we don't concentrate our limited resources to one specific goal, we will not be able to achieve anything at all. Once we are ready to market our first device, the peanut detector, we will be able to start the R&D for the 2nd product, which will be for another allergen – most likely tree nuts and/or sesame, but that will probably be in debate until we actually start it.
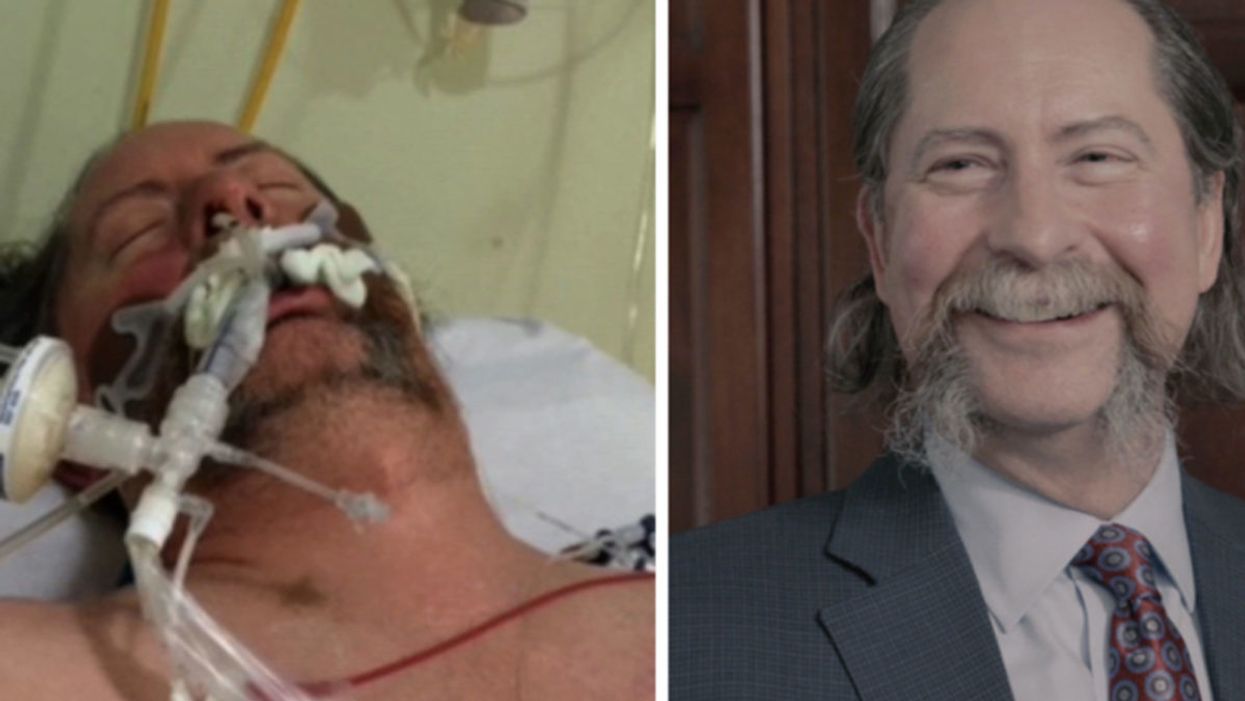
Dr. Robert Montgomery, the director of NYU Langone's Transplant Institute, is ironically the recipient of a heart transplant.
[Ed. Note: This is the fourth episode in our Moonshot series, which explores four cutting-edge scientific developments that stand to fundamentally transform our world.]
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.