How dozens of men across Alaska (and their dogs) teamed up to save one town from a deadly outbreak

In 1925, health officials in Alaska came up with a creative solution to save a remote fishing town from a deadly disease outbreak.
During the winter of 1924, Curtis Welch – the only doctor in Nome, a remote fishing town in northwest Alaska – started noticing something strange. More and more, the children of Nome were coming to his office with sore throats.
Initially, Welch dismissed the cases as tonsillitis or some run-of-the-mill virus – but when more kids started getting sick, with some even dying, he grew alarmed. It wasn’t until early 1925, after a three-year-old boy died just two weeks after becoming ill, that Welch realized that his worst suspicions were true. The boy – and dozens of other children in town – were infected with diphtheria.
A DEADLY BACTERIA
Diphtheria is nearly nonexistent and almost unheard of in industrialized countries today. But less than a century ago, diphtheria was a household name – one that struck fear in the heart of every parent, as it was extremely contagious and particularly deadly for children.
Diphtheria – a bacterial infection – is an ugly disease. When it strikes, the bacteria eats away at the healthy tissues in a patient’s respiratory tract, leaving behind a thick, gray membrane of dead tissue that covers the patient's nose, throat, and tonsils. Not only does this membrane make it very difficult for the patient to breathe and swallow, but as the bacteria spreads through the bloodstream, it causes serious harm to the heart and kidneys. It sometimes also results in nerve damage and paralysis. Even with treatment, diphtheria kills around 10 percent of people it infects. Young children, as well as adults over the age of 60, are especially at risk.
Welch didn’t suspect diphtheria at first. He knew the illness was incredibly contagious and reasoned that many more people would be sick – specifically, the family members of the children who had died – if there truly was an outbreak. Nevertheless, the symptoms, along with the growing number of deaths, were unmistakable. By 1925 Welch knew for certain that diphtheria had come to Nome.
In desperation, Welch tried treating an infected seven-year-old girl with some expired antitoxin – but she died just a few hours after he administered it.
AN INACCESSIBLE CURE
A vaccine for diphtheria wouldn’t be widely available until the mid-1930s and early 1940s – so an outbreak of the disease meant that each of the 10,000 inhabitants of Nome were all at serious risk.
One option was to use something called an antitoxin – a serum consisting of anti-diphtheria antibodies – to treat the patients. However, the town’s reserve of diphtheria antitoxin had expired. Welch had ordered a replacement shipment of antitoxin the previous summer – but the shipping port that was set to deliver the serum had been closed due to ice, and no new antitoxin would arrive before spring of 1925. In desperation, Welch tried treating an infected seven-year-old girl with some expired antitoxin – but she died just a few hours after he administered it.
Welch radioed for help to all the major towns in Alaska as well as the US Public Health Service in Washington, DC. His telegram read: An outbreak of diphtheria is almost inevitable here. I am in urgent need of one million units of diphtheria antitoxin. Mail is the only form of transportation.
FOUR-LEGGED HEROES
When the Alaskan Board of Health learned about the outbreak, the men rushed to devise a plan to get antitoxin to Nome. Dropping the serum in by airplane was impossible, as the available planes were unsuitable for flying during Alaska’s severe winter weather, where temperatures were routinely as cold as -50 degrees Fahrenheit.
In late January 1925, roughly 30,000 units of antitoxin were located in an Anchorage hospital and immediately delivered by train to a nearby city, Nenana, en route to Nome. Nenana was the furthest city that was reachable by rail – but unfortunately it was still more than 600 miles outside of Nome, with no transportation to make the delivery. Meanwhile, Welch had confirmed 20 total cases of diphtheria, with dozens more at high risk. Diphtheria was known for wiping out entire communities, and the entire town of Nome was in danger of suffering the same fate.
It was Mark Summer, the Board of Health superintendent, who suggested something unorthodox: Using a relay team of sled-racing dogs to deliver the antitoxin serum from Nenana to Nome. The Board quickly voted to accept Summer’s idea and set up a plan: The thousands of units of antitoxin serum would be passed along from team to team at different towns along the mail route from Nenana to Nome. When it reached a town called Nulato, a famed dogsled racer named Leonhard Seppala and his experienced team of huskies would take the serum more than 90 miles over the ice of Norton Sound, the longest and most treacherous part of the journey. Past the sound, the serum would change hands several times more before arriving in Nome.
Between January 27 and 31, the serum passed through roughly a dozen drivers and their dog sled teams, each of them carrying the serum between 20 and 50 miles to the next destination. Though each leg of the trip took less than a day, the sub-zero temperatures – sometimes as low as -85 degrees – meant that every driver and dog risked their lives. When the first driver, Bill Shannon, arrived at his checkpoint in Tolovana on January 28th, his nose was black with frostbite, and three of his dogs had died. The driver who relieved Bill Shannon, named Edgar Kalland, needed the owner of a local roadhouse to pour hot water over his hands to free them from the sled’s metal handlebar. Two more dogs from another relay team died before the serum was passed to Seppala at a town called Ungalik.
THE FINAL STRETCHES
Seppala and his team raced across the ice of the Norton Sound in the dead of night on January 31, with wind chill temperatures nearing an astonishing -90 degrees. The team traveled 84 miles in a single day before stopping to rest – and once rested, they set off again in the middle of the night through a raging winter storm. The team made it across the ice, as well as a 5,000-foot ascent up Little McKinley Mountain, to pass the serum to another driver in record time. The serum was now just 78 miles from Nome, and the death toll in town had reached 28.
The serum reached Gunnar Kaasen and his team of dogs on February 1st. Balto, Kaasen’s lead dog, guided the team heroically through a winter storm that was so severe Kaasen later reported not being able to see the dogs that were just a few feet ahead of him.
Visibility was so poor, in fact, that Kaasen ran his sled two miles past the relay point before noticing – and not wanting to lose a minute, he decided to forge on ahead rather than doubling back to deliver the serum to another driver. As they continued through the storm, the hurricane-force winds ripped past Kaasen’s sled at one point and toppled the sled – and the serum – overboard. The cylinder containing the antitoxin was left buried in the snow – and Kaasen tore off his gloves and dug through the tundra to locate it. Though it resulted in a bad case of frostbite, Kaasen eventually found the cylinder and kept driving.
Kaasen arrived at the next relay point on February 2nd, hours ahead of schedule. When he got there, however, he found the relay driver of the next team asleep. Kaasen took a risk and decided not to wake him, fearing that time would be wasted with the next driver readying his team. Kaasen, Balto, and the rest of the team forged on, driving another 25 miles before finally reaching Nome just before six in the morning. Eyewitnesses described Kaasen pulling up to the town’s bank and stumbling to the front of the sled. There, he collapsed in exhaustion, telling onlookers that Balto was “a damn fine dog.”
A LIVING LEGACY
Just a few hours after Balto’s heroic arrival in Nome, the serum had been thawed and was ready to administer to the patients with diphtheria. Amazingly, the relay team managed to complete the entire journey in just 127 hours – a world record at the time – without one serum vial damaged or destroyed. The serum shipment that arrived by dogsled – along with additional serum deliveries that followed in the next several weeks – were successful in stopping the outbreak in its tracks.
Balto and several other dogs – including Togo, the lead dog on Seppala’s team – were celebrated as local heroes after the race. Balto died in 1933, while the last of the human serum runners died in 1999 – but their legacy lives on: In early 2021, an all-female team of healthcare workers made the news by braving the Alaskan winter to deliver COVID-19 vaccines to people in rural North Alaska, traveling by bobsled and snowmobile – a heroic journey, and one that would have been unthinkable had Balto, Togo, and the 1925 sled runners not first paved the way.
New Device Can Detect Peanut Allergens on a Plate in 30 Seconds
Peanuts on a plate can be deadly for those with severe allergies, but an Israeli startup company wants to alleviate that fear.
People with life-threatening allergies live in constant fear of coming into contact with deadly allergens. Researchers estimate that about 32 million Americans have food allergies, with the most severe being milk, egg, peanut, tree nuts, wheat, soy, fish, and shellfish.
"It is important to understand that just several years ago, this would not have been possible."
Every three minutes, a food allergy reaction sends someone to the emergency room, and 200,000 people in the U.S. require emergency medical care each year for allergic reactions, according to Food Allergy Research and Education.
But what if there was a way you could easily detect if something you were about to eat contains any harmful allergens? Thanks to Israeli scientists, this will soon be the case — at least for peanuts. The team has been working to develop a handheld device called Allerguard, which analyzes the vapors in your meal and can detect allergens in 30 seconds.
Leapsmag spoke with the founder and CTO of Allerguard, Guy Ayal, about the groundbreaking technology, how it works, and when it will be available to purchase.
What prompted you to create this device? Do you have a personal connection with severe food allergies?
Guy Ayal: My eldest daughter's best friend suffers from a severe food allergy, and I experienced first-hand the effect it has on the person and their immediate surroundings. Most notable for me was the effect on the quality of life – the experience of living in constant fear. Everything we do at Allerguard is basically to alleviate some of that fear.
How exactly does the device work?
The device is built on two main pillars. The first is the nano-chemical stage, in which we developed specially attuned nanoparticles that selectively adhere only to the specific molecules that we are looking for. Those molecules, once bound to the nanoparticles, induce a change in their electrical behavior, which is measured and analyzed by the second main pillar -- highly advanced machine learning algorithms, which can surmise which molecules were collected, and thus whether or not peanuts (or in the future, other allergens) were detected.
It is important to understand that just several years ago, this would not have been possible, because both the nano-chemistry, and especially the entire world of machine learning, big data, and what is commonly known as AI only started to exist in the '90s, and reached applicability for handheld devices only in the past few years.
Where are you at in the development process and when will the device be available to consumers?
We have concluded the proof of concept and proof of capability phase, when we demonstrated successful detection of the minimal known clinical amount that may cause the slightest effect in the most severely allergic person – less than 1 mg of peanut (actually it is 0.7 mg). Over the next 18 months will be productization, qualification, and validation of our device, which should be ready to market in the latter half of 2021. The sensor will be available in the U.S., and after a year in Europe and Canada.

The Allerguard was made possible through recent advances in machine learning, big data, and AI.
(Courtesy)
How much will it cost?
Our target price is about $200 for the device, with a disposable SenseCard that will run for at least a full day and cost about $1. That card is for a specific allergen and will work for multiple scans in a day, not just one time.
[At a later stage, the company will have sensors for other allergens like tree nuts, eggs, and milk, and they'll develop a multi-SenseCard that works for a few allergens at once.]
Are there any other devices on the market that do something similar to Allerguard?
No other devices are even close to supplying the level of service that we promise. All known methods for allergen detection rely on sampling of the food, which is a viable solution for homogenous foodstuffs, such as a factory testing their raw ingredients, but not for something as heterogenous as an actual dish – especially not for solid allergens such as peanuts, treenuts, or sesame.
If there is a single peanut in your plate, and you sample from anywhere on that plate which is not where that peanut is located, you will find that your sample is perfectly clean – because it is. But the dish is not. That dish is a death trap for an allergic person. Allerguard is the only suggested solution that could indeed detect that peanut, no matter where in that plate it is hiding.
Anything else readers should know?
Our first-generation product will be for peanuts only. You have to understand, we are still a start-up company, and if we don't concentrate our limited resources to one specific goal, we will not be able to achieve anything at all. Once we are ready to market our first device, the peanut detector, we will be able to start the R&D for the 2nd product, which will be for another allergen – most likely tree nuts and/or sesame, but that will probably be in debate until we actually start it.
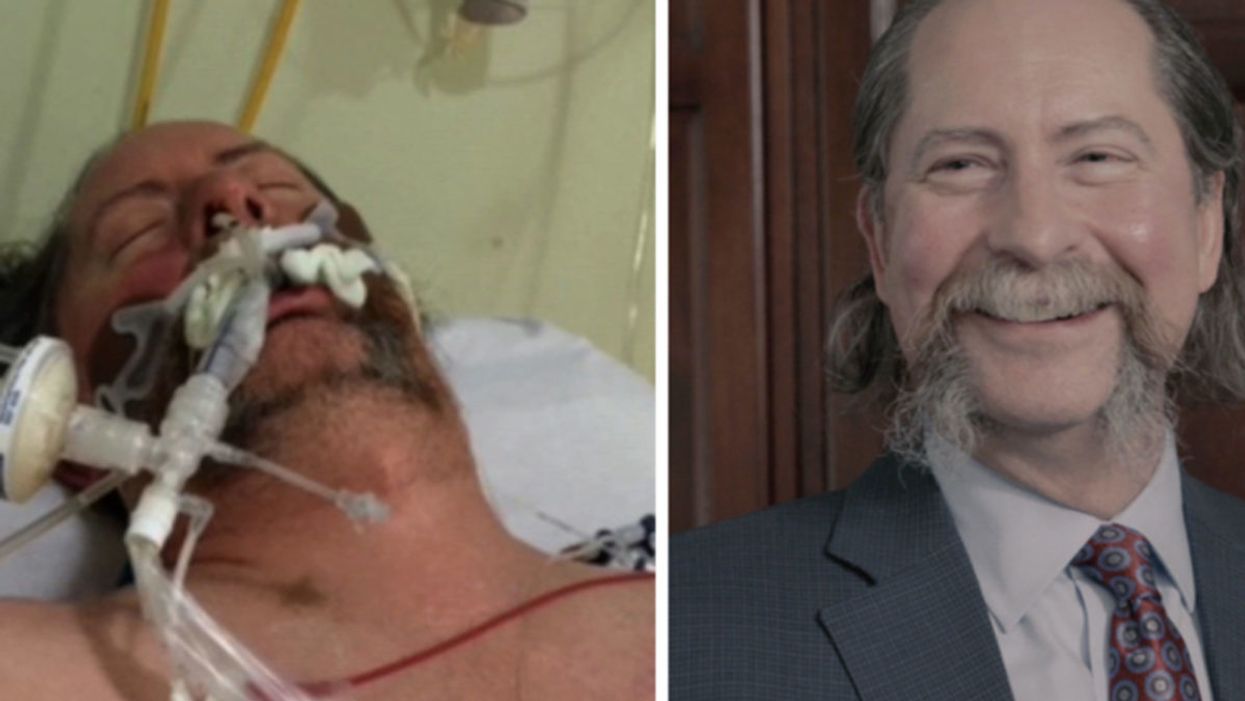
Dr. Robert Montgomery, the director of NYU Langone's Transplant Institute, is ironically the recipient of a heart transplant.
[Ed. Note: This is the fourth episode in our Moonshot series, which explores four cutting-edge scientific developments that stand to fundamentally transform our world.]
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.