“Disinfection Tunnels” Are Popping Up Around the World, Fueled By Misinformation and Fear

A screenshot of a video published by The Guardian of a tunnel used in a Mexican border town to "disinfect" U.S. visitors in an attempt to prevent them from spreading the coronavirus.
In an incident that sparked widespread outrage across India in late March, officials in the north Indian state of Uttar Pradesh sprayed hundreds of migrant workers, including women and children, with a chemical solution to sanitize them, in a misguided attempt to contain the spread of the novel coronavirus.
Since COVID-19 is a respiratory disorder, disinfecting a person's body or clothes cannot protect them from contracting the novel coronavirus, or help in containing the pathogen's spread.
Health officials reportedly doused the group with a diluted mixture of sodium hypochlorite – a bleaching agent harmful to humans, which led to complaints of skin rashes and eye irritation. The opposition termed the instance 'inhuman', compelling the state government to order an investigation into the mass 'chemical bath.'
"I don't think the officials thought this through," says Thomas Abraham, a professor with The University of Hong Kong, and a former consultant for the World Health Organisation (WHO) on risk communication. "Spraying people with bleach can prove to be harmful, and there is no guideline … that recommends it. This was some sort of a kneejerk reaction."
Although spraying individuals with chemicals led to a furor in the South Asian nation owing to its potential dangers, so-called "disinfection tunnels" have sprung up in crowded public places around the world, including malls, offices, airports, railway stations and markets. Touted as mass disinfectants, these tunnels spray individuals with chemical disinfectant liquids, mists or fumes through nozzles for a few seconds, purportedly to sanitize them -- though experts strongly condemn their use. The tunnels have appeared in at least 16 countries: India, Malaysia, Scotland, Albania, Argentina, Colombia, Singapore, China, Pakistan, France, Vietnam, Bosnia and Herzegovina, Chile, Mexico, Sri Lanka and Indonesia. Russian President Vladimir Putin even reportedly has his own tunnel at his residence.
While U.S. visitors to Mexico are "disinfected" through these sanitizing tunnels, there is no evidence that the mechanism is currently in use within the United States. However, the situation could rapidly change with international innovators like RD Pack, an Israeli start-up, pushing for their deployment. Many American and multinational companies like Stretch Structures, Guilio Barbieri and Inflatable Design Works are also producing these systems. As countries gradually ease lockdown restrictions, their demand is on the rise -- despite a stringent warning from the WHO against their potential health hazards.
"Spraying individuals with disinfectants (such as in a tunnel, cabinet, or chamber) is not recommended under any circumstances," the WHO warned in a report on May 15. "This could be physically and psychologically harmful and would not reduce an infected person's ability to spread the virus through droplets or contact. Moreover, spraying individuals with chlorine and other toxic chemicals could result in eye and skin irritation, bronchospasm due to inhalation, and gastrointestinal effects such as nausea and vomiting."
Disinfection tunnels largely spray a diluted mixture of sodium hypochlorite, a chlorine compound commonly known as bleach, often used to disinfect inanimate surfaces. Known for its hazardous properties, the WHO, in a separate advisory on COVID-19, warns that spraying bleach or any other disinfectant on individuals can prove to be poisonous if ingested, and that such substances should be used only to disinfect surfaces.
Considering the effect of sodium hypochlorite on mucous membranes, the European Centre for Disease Prevention and Control, an EU agency focussed on infectious diseases, recommends limited use of the chemical compound even when disinfecting surfaces – only 0.05 percent for cleaning surfaces, and 0.1 percent for toilets and bathroom sinks. The Indian health ministry also cautioned against spraying sodium hypochlorite recently, stating that its inhalation can lead to irritation of mucous membranes of the nose, throat, and respiratory tract.
In addition to the health hazards that such sterilizing systems pose, they have little utility, argues Indian virologist T. Jacob John. Since COVID-19 is a respiratory disorder, disinfecting a person's body or clothes cannot protect them from contracting the novel coronavirus, or help in containing the pathogen's spread.
"It's a respiratory infection, which means that you have the virus in your respiratory tract, and of course, that shows in your throat, therefore saliva, etc.," says John. "The virus does not survive outside the body for a long time, unless it is in freezing temperatures. Disinfecting a person's clothes or their body makes no sense."
Disinfection tunnels have limited, if any, impact on the main modes of coronavirus transmission, adds Craig Janes, director, School of Public Health and Health Systems at Canada's University of Waterloo. He explains that the nature of COVID-19 transmission is primarily from person-to-person, either directly, or via an object that is shared between two individuals. Measures like physical distancing and handwashing take care of these transmission risks.
"My view of these kinds of actions are that they are principally symbolic, indicating to a concerned population that 'something is being done,' to martial support for government or health system efforts," says Janes. "So perhaps a psychological benefit, but I'm not sure that this benefit would outweigh the risks."
"They may make people feel that their risk of infection has been reduced, and also that they do not have to worry about infecting others."
A recent report by Health Care Without Harm (HCWH), an international not-for-profit organization focused on sustainable health care around the world, states that disinfection tunnels have little evidence to demonstrate their efficacy or safety.
"If the goal is to reduce the spread of the virus by decontaminating the exterior clothing, shoes, and skin of the general public, there is no evidence that clothes are an important vector for transmission. If the goal is to attack the virus in the airways, what is the evidence that a 20-30 second external application is efficacious and safe?" the report questions. "The World Health Organization recommends more direct and effective ways to address hand hygiene, with interventions known to be effective."
If an infected person walks through a disinfection tunnel, he would still be infectious, as the chemicals will only disinfect the surfaces, says Gerald Keusch, a professor of medicine and international health at Boston University's Schools of Medicine and Public Health.
"While we know that viruses can be "disinfected" from surfaces and hands, disinfectants can be harmful to health if ingested or inhaled. The underlying principle of medicine is to do no harm, and we always measure benefit against risk when approving interventions. I don't know if this has been followed and assessed with respect to these devices," says Keusch. "It's a really bad idea."
Experts warn that such tunnels may also create a false sense of security, discouraging people from adopting best practice methods like handwashing, social distancing, avoiding crowded places, and using masks to combat the spread of COVID-19.
"They may make people feel that their risk of infection has been reduced, and also that they do not have to worry about infecting others," says Janes. "These are false assumptions, and may lead to increasing rather than reducing transmission."
Urinary tract infections account for more than 8 million trips to the doctor each year.
Few things are more painful than a urinary tract infection (UTI). Common in men and women, these infections account for more than 8 million trips to the doctor each year and can cause an array of uncomfortable symptoms, from a burning feeling during urination to fever, vomiting, and chills. For an unlucky few, UTIs can be chronic—meaning that, despite treatment, they just keep coming back.
But new research, presented at the European Association of Urology (EAU) Congress in Paris this week, brings some hope to people who suffer from UTIs.
Clinicians from the Royal Berkshire Hospital presented the results of a long-term, nine-year clinical trial where 89 men and women who suffered from recurrent UTIs were given an oral vaccine called MV140, designed to prevent the infections. Every day for three months, the participants were given two sprays of the vaccine (flavored to taste like pineapple) and then followed over the course of nine years. Clinicians analyzed medical records and asked the study participants about symptoms to check whether any experienced UTIs or had any adverse reactions from taking the vaccine.
The results showed that across nine years, 48 of the participants (about 54%) remained completely infection-free. On average, the study participants remained infection free for 54.7 months—four and a half years.
“While we need to be pragmatic, this vaccine is a potential breakthrough in preventing UTIs and could offer a safe and effective alternative to conventional treatments,” said Gernot Bonita, Professor of Urology at the Alta Bro Medical Centre for Urology in Switzerland, who is also the EAU Chairman of Guidelines on Urological Infections.
The news comes as a relief not only for people who suffer chronic UTIs, but also to doctors who have seen an uptick in antibiotic-resistant UTIs in the past several years. Because UTIs usually require antibiotics, patients run the risk of developing a resistance to the antibiotics, making infections more difficult to treat. A preventative vaccine could mean less infections, less antibiotics, and less drug resistance overall.
“Many of our participants told us that having the vaccine restored their quality of life,” said Dr. Bob Yang, Consultant Urologist at the Royal Berkshire NHS Foundation Trust, who helped lead the research. “While we’re yet to look at the effect of this vaccine in different patient groups, this follow-up data suggests it could be a game-changer for UTI prevention if it’s offered widely, reducing the need for antibiotic treatments.”
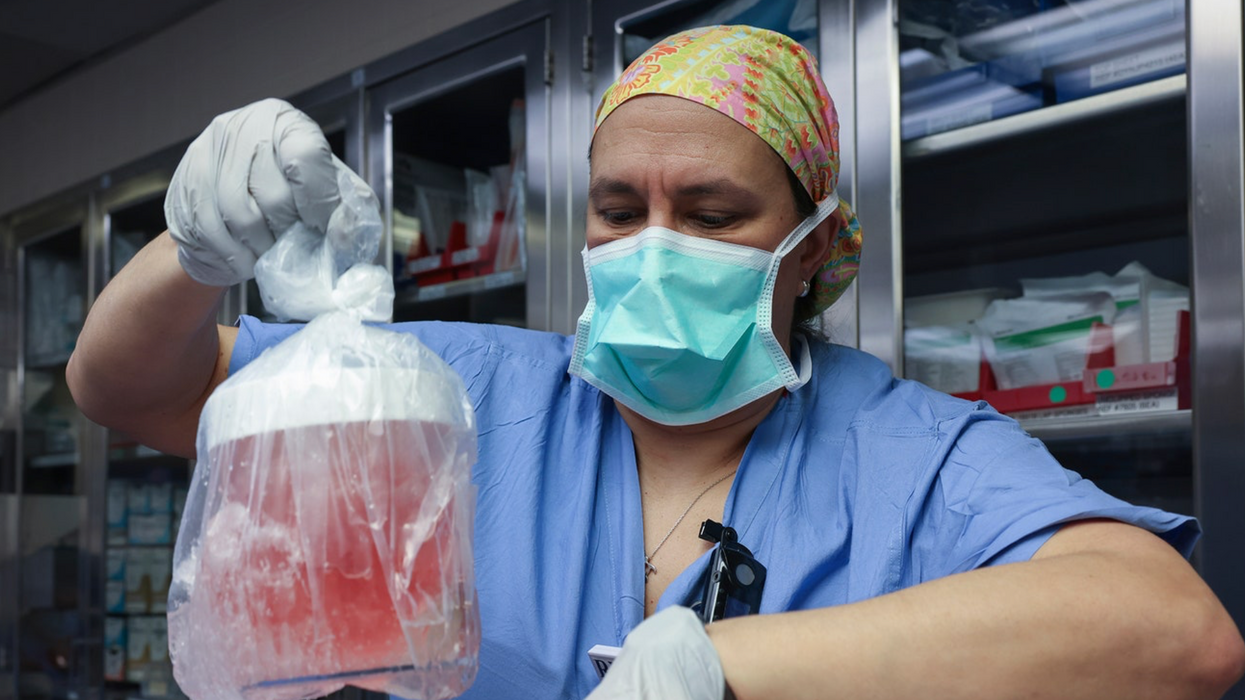
MILESTONE: Doctors have transplanted a pig organ into a human for the first time in history
A surgeon at Massachusetts General Hospital prepares a pig organ for transplant.
Surgeons at Massachusetts General Hospital made history last week when they successfully transplanted a pig kidney into a human patient for the first time ever.
The recipient was a 62-year-old man named Richard Slayman who had been living with end-stage kidney disease caused by diabetes. While Slayman had received a kidney transplant in 2018 from a human donor, his diabetes ultimately caused the kidney to fail less than five years after the transplant. Slayman had undergone dialysis ever since—a procedure that uses an artificial kidney to remove waste products from a person’s blood when the kidneys are unable to—but the dialysis frequently caused blood clots and other complications that landed him in the hospital multiple times.
As a last resort, Slayman’s kidney specialist suggested a transplant using a pig kidney provided by eGenesis, a pharmaceutical company based in Cambridge, Mass. The highly experimental surgery was made possible with the Food and Drug Administration’s “compassionate use” initiative, which allows patients with life-threatening medical conditions access to experimental treatments.
The new frontier of organ donation
Like Slayman, more than 100,000 people are currently on the national organ transplant waiting list, and roughly 17 people die every day waiting for an available organ. To make up for the shortage of human organs, scientists have been experimenting for the past several decades with using organs from animals such as pigs—a new field of medicine known as xenotransplantation. But putting an animal organ into a human body is much more complicated than it might appear, experts say.
“The human immune system reacts incredibly violently to a pig organ, much more so than a human organ,” said Dr. Joren Madsen, director of the Mass General Transplant Center. Even with immunosuppressant drugs that suppress the body’s ability to reject the transplant organ, Madsen said, a human body would reject an animal organ “within minutes.”
So scientists have had to use gene-editing technology to change the animal organs so that they would work inside a human body. The pig kidney in Slayman’s surgery, for instance, had been genetically altered using CRISPR-Cas9 technology to remove harmful pig genes and add human ones. The kidney was also edited to remove pig viruses that could potentially infect a human after transplant.
With CRISPR technology, scientists have been able to prove that interspecies organ transplants are not only possible, but may be able to successfully work long term, too. In the past several years, scientists were able to transplant a pig kidney into a monkey and have the monkey survive for more than two years. More recently, doctors have transplanted pig hearts into human beings—though each recipient of a pig heart only managed to live a couple of months after the transplant. In one of the patients, researchers noted evidence of a pig virus in the man’s heart that had not been identified before the surgery and could be a possible explanation for his heart failure.
So far, so good
Slayman and his medical team ultimately decided to pursue the surgery—and the risk paid off. When the pig organ started producing urine at the end of the four-hour surgery, the entire operating room erupted in applause.
Slayman is currently receiving an infusion of immunosuppressant drugs to prevent the kidney from being rejected, while his doctors monitor the kidney’s function with frequent ultrasounds. Slayman is reported to be “recovering well” at Massachusetts General Hospital and is expected to be discharged within the next several days.