Elizabeth Holmes Through the Director’s Lens
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.

Elizabeth Holmes.
"The Inventor," a chronicle of Theranos's storied downfall, premiered recently on HBO. Leapsmag reached out to director Alex Gibney, whom The New York Times has called "one of America's most successful and prolific documentary filmmakers," for his perspective on Elizabeth Holmes and the world she inhabited.
Do you think Elizabeth Holmes was a charismatic sociopath from the start — or is she someone who had good intentions, over-promised, and began the lies to keep her business afloat, a "fake it till you make it" entrepreneur like Thomas Edison?
I'm not qualified to say if EH was or is a sociopath. I don't think she started Theranos as a scam whose only purpose was to make money. If she had done so, she surely would have taken more money for herself along the way. I do think that she had good intentions and that she, as you say, "began the lies to keep her business afloat." ([Reporter John] Carreyrou's book points out that those lies began early.) I think that the Edison comparison is instructive for a lot of reasons.
First, Edison was the original "fake-it-till-you-make-it" entrepreneur. That puts this kind of behavior in the mainstream of American business. By saying that, I am NOT endorsing the ethic, just the opposite. As one Enron executive mused about the mendacity there, "Was it fraud or was it bad marketing?" That gives you a sense of how baked-in the "fake it" sensibility is.
"Having a thirst for fame and a noble cause enabled her to think it was OK to lie in service of those goals."
I think EH shares one other thing with Edison, which is a huge ego coupled with a talent for storytelling as long as she is the heroic, larger-than-life main character. It's interesting that EH calls her initial device "Edison." Edison was the world's most famous "inventor," both because of the devices that came out of his shop and and for his ability for "self-invention." As Randall Stross notes in "The Wizard of Menlo Park," he was the first celebrity businessman. In addition to her "good intentions," EH was certainly motivated by fame and glory and many of her lies were in service to those goals.
Having a thirst for fame and a noble cause enabled her to think it was OK to lie in service of those goals. That doesn't excuse the lies. But those noble goals may have allowed EH to excuse them for herself or, more perniciously, to make believe that they weren't lies at all. This is where we get into scary psychological territory.
But rather than thinking of it as freakish, I think it's more productive to think of it as an exaggeration of the way we all lie to others and to ourselves. That's the point of including the Dan Ariely experiment with the dice. In that experiment, most of the subjects cheated more when they thought they were doing it for a good cause. Even more disturbing, that "good cause" allowed them to lie much more effectively because they had come to believe they weren't doing anything wrong. As it turns out, economics isn't a rational practice; it's the practice of rationalizing.
Where EH and Edison differ is that Edison had a firm grip on reality. He knew he could find a way to make the incandescent lightbulb work. There is no evidence that EH was close to making her "Edison" work. But rather than face reality (and possibly adjust her goals) she pretended that her dream was real. That kind of "over-promising" or "bold vision" is one thing when you are making a prototype in the lab. It's a far more serious matter when you are using a deeply flawed system on real patients. EH can tell herself that she had to do that (Walgreens was ready to walk away if she hadn't "gone live") or else Theranos would have run out of money.
But look at the calculation she made: she thought it was worth putting lives at risk in order to make her dream come true. Now we're getting into the realm of the sociopath. But my experience leads me to believe that -- as in the case of the Milgram experiment -- most people don't do terrible things right away, they come to crimes gradually as they become more comfortable with bigger and bigger rationalizations. At Theranos, the more valuable the company became, the bigger grew the lies.
The two whistleblowers come across as courageous heroes, going up against the powerful and intimidating company. The contrast between their youth and lack of power and the old elite backers of Theronos is staggering, and yet justice triumphed. Were the whistleblowers hesitant or afraid to appear in the film, or were they eager to share their stories?
By the time I got to them, they were willing and eager to tell their stories, once I convinced them that I would honor their testimony. In the case of Erika and Tyler, they were nudged to participate by John Carreyrou, in whom they had enormous trust.
"It's simply crazy that no one demanded to see an objective demonstration of the magic box."
Why do you think so many elite veterans of politics and venture capitalism succumbed to Holmes' narrative in the first place, without checking into the details of its technology or financials?
The reasons are all in the film. First, Channing Robertson and many of the old men on her board were clearly charmed by her and maybe attracted to her. They may have rationalized their attraction by convincing themselves it was for a good cause! Second, as Dan Ariely tells us, we all respond to stories -- more than graphs and data -- because they stir us emotionally. EH was a great storyteller. Third, the story of her as a female inventor and entrepreneur in male-dominated Silicon Valley is a tale that they wanted to invest in.
There may have been other factors. EH was very clever about the way she put together an ensemble of credibility. How could Channing Robertson, George Shultz, Henry Kissinger and Jim Mattis all be wrong? And when Walgreens put the Wellness Centers in stores, investors like Rupert Murdoch assumed that Walgreens must have done its due diligence. But they hadn't!
It's simply crazy that no one demanded to see an objective demonstration of the magic box. But that blind faith, as it turns out, is more a part of capitalism than we have been taught.
Do you think that Roger Parloff deserves any blame for the glowing Fortune story on Theranos, since he appears in the film to blame himself? Or was he just one more victim of Theranos's fraud?
He put her on the cover of Fortune so he deserves some blame for the fraud. He still blames himself. That willingness to hold himself to account shows how seriously he takes the job of a journalist. Unlike Elizabeth, Roger has the honesty and moral integrity to admit that he made a mistake. He owned up to it and published a mea culpa. That said, Roger was also a victim because Elizabeth lied to him.
Do you think investors in Silicon Valley, with their FOMO attitudes and deep pockets, are vulnerable to making the same mistake again with a shiny new startup, or has this saga been a sober reminder to do their due diligence first?
Many of the mistakes made with Theranos were the same mistakes made with Enron. We must learn to recognize that we are, by nature, trusting souls. Knowing that should lead us to a guiding slogan: "trust but verify."
The irony of Holmes dancing to "I Can't Touch This" is almost too perfect. How did you find that footage?
It was leaked to us.
"Elizabeth Holmes is now famous for her fraud. Who better to host the re-boot of 'The Apprentice.'"
Holmes is facing up to 20 years in prison for federal fraud charges, but Vanity Fair recently reported that she is seeking redemption, taking meetings with filmmakers for a possible documentary to share her "real" story. What do you think will become of Holmes in the long run?
It's usually a mistake to handicap a trial. My guess is that she will be convicted and do some prison time. But maybe she can convince jurors -- the way she convinced journalists, her board, and her investors -- that, on account of her noble intentions, she deserves to be found not guilty. "Somewhere, over the rainbow…"
After the trial, and possibly prison, I'm sure that EH will use her supporters (like Tim Draper) to find a way to use the virtual currency of her celebrity to rebrand herself and launch something new. Fitzgerald famously said that "there are no second acts in American lives." That may be the stupidest thing he ever said.
Donald Trump failed at virtually every business he ever embarked on. But he became a celebrity for being a fake businessman and used that celebrity -- and phony expertise -- to become president of the United States. Elizabeth Holmes is now famous for her fraud. Who better to host the re-boot of "The Apprentice." And then?
"You Can't Touch This!"
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
Although Jonas Salk has gone down in history for helping rid the world (almost) of polio, his revolutionary vaccine wouldn't have been possible without the world’s largest clinical trial – and the bravery of thousands of kids.
Exactly 67 years ago, in 1955, a group of scientists and reporters gathered at the University of Michigan and waited with bated breath for Dr. Thomas Francis Jr., director of the school’s Poliomyelitis Vaccine Evaluation Center, to approach the podium. The group had gathered to hear the news that seemingly everyone in the country had been anticipating for the past two years – whether the vaccine for poliomyelitis, developed by Francis’s former student Jonas Salk, was effective in preventing the disease.
Polio, at that point, had become a household name. As the highly contagious virus swept through the United States, cities closed their schools, movie theaters, swimming pools, and even churches to stop the spread. For most, polio presented as a mild illness, and was usually completely asymptomatic – but for an unlucky few, the virus took hold of the central nervous system and caused permanent paralysis of muscles in the legs, arms, and even people’s diaphragms, rendering the person unable to walk and breathe. It wasn’t uncommon to hear reports of people – mostly children – who fell sick with a flu-like virus and then, just days later, were relegated to spend the rest of their lives in an iron lung.
For two years, researchers had been testing a vaccine that would hopefully be able to stop the spread of the virus and prevent the 45,000 infections each year that were keeping the nation in a chokehold. At the podium, Francis greeted the crowd and then proceeded to change the course of human history: The vaccine, he reported, was “safe, effective, and potent.” Widespread vaccination could begin in just a few weeks. The nightmare was over.
The road to success
Jonas Salk, a medical researcher and virologist who developed the vaccine with his own research team, would rightfully go down in history as the man who eradicated polio. (Today, wild poliovirus circulates in just two countries, Afghanistan and Pakistan – with only 140 cases reported in 2020.) But many people today forget that the widespread vaccination campaign that effectively ended wild polio across the globe would have never been possible without the human clinical trials that preceded it.
As with the COVID-19 vaccine, skepticism and misinformation around the polio vaccine abounded. But even more pervasive than the skepticism was fear. The consequences of polio had arguably never been more visible.
The road to human clinical trials – and the resulting vaccine – was a long one. In 1938, President Franklin Delano Roosevelt launched the National Foundation for Infantile Paralysis in order to raise funding for research and development of a polio vaccine. (Today, we know this organization as the March of Dimes.) A polio survivor himself, Roosevelt elevated awareness and prevention into the national spotlight, even more so than it had been previously. Raising funds for a safe and effective polio vaccine became a cornerstone of his presidency – and the funds raked in by his foundation went primarily to Salk to fund his research.
The Trials Begin
Salk’s vaccine, which included an inactivated (killed) polio virus, was promising – but now the researchers needed test subjects to make global vaccination a possibility. Because the aim of the vaccine was to prevent paralytic polio, researchers decided that they had to test the vaccine in the population that was most vulnerable to paralysis – young children. And, because the rate of paralysis was so low even among children, the team required many children to collect enough data. Francis, who led the trial to evaluate Salk’s vaccine, began the process of recruiting more than one million school-aged children between the ages of six and nine in 272 counties that had the highest incidence of the disease. The participants were nicknamed the “Polio Pioneers.”
Double-blind, placebo-based trials were considered the “gold standard” of epidemiological research back in Francis's day - and they remain the best approach we have today. These rigorous scientific studies are designed with two participant groups in mind. One group, called the test group, receives the experimental treatment (such as a vaccine); the other group, called the control, receives an inactive treatment known as a placebo. The researchers then compare the effects of the active treatment against the effects of the placebo, and every researcher is “blinded” as to which participants receive what treatment. That way, the results aren’t tainted by any possible biases.
But the study was controversial in that only some of the individual field trials at the county and state levels had a placebo group. Researchers described this as a “calculated risk,” meaning that while there were risks involved in giving the vaccine to a large number of children, the bigger risk was the potential paralysis or death that could come with being infected by polio. In all, just 200,000 children across the US received a placebo treatment, while an additional 725,000 children acted as observational controls – in other words, researchers monitored them for signs of infection, but did not give them any treatment.
As with the COVID-19 vaccine, skepticism and misinformation around the polio vaccine abounded. But even more pervasive than the skepticism was fear. President Roosevelt, who had made many public and televised appearances in a wheelchair, served as a perpetual reminder of the consequences of polio, as an infection at age 39 had rendered him permanently unable to walk. The consequences of polio had arguably never been more visible, and parents signed up their children in droves to participate in the study and offer them protection.
The Polio Pioneer Legacy
In a little less than a year, roughly half a million children received a dose of Salk’s polio vaccine. While plenty of children were hesitant to get the shot, many former participants still remember the fear surrounding the disease. One former participant, a Polio Pioneer named Debbie LaCrosse, writes of her experience: “There was no discussion, no listing of pros and cons. No amount of concern over possible side effects or other unknowns associated with a new vaccine could compare to the terrifying threat of polio.” For their participation, each kid received a certificate – and sometimes a pin – with the words “Polio Pioneer” emblazoned across the front.
When Francis announced the results of the trial on April 12, 1955, people did more than just breathe a sigh of relief – they openly celebrated, ringing church bells and flooding into the streets to embrace. Salk, who had become the face of the vaccine at that point, was instantly hailed as a national hero – and teachers around the country had their students to write him ‘thank you’ notes for his years of diligent work.
But while Salk went on to win national acclaim – even accepting the Presidential Medal of Freedom for his work on the polio vaccine in 1977 – his success was due in no small part to the children (and their parents) who took a risk in order to advance medical science. And that risk paid off: By the early 1960s, the yearly cases of polio in the United States had gone down to just 910. Where before the vaccine polio had caused around 15,000 cases of paralysis each year, only ten cases of paralysis were recorded in the entire country throughout the 1970s. And in 1979, the virus that once shuttered entire towns was declared officially eradicated in this country. Thanks to the efforts of these brave pioneers, the nation – along with the majority of the world – remains free of polio even today.
Why you should (virtually) care
Virtual-first care, or V1C, could increase the quality of healthcare and make it more patient-centric by letting patients combine in-person visits with virtual options such as video for seeing their care providers.
As the pandemic turns endemic, healthcare providers have been eagerly urging patients to return to their offices to enjoy the benefits of in-person care.
But wait.
The last two years have forced all sorts of organizations to be nimble, adaptable and creative in how they work, and this includes healthcare providers’ efforts to maintain continuity of care under the most challenging of conditions. So before we go back to “business as usual,” don’t we owe it to those providers and ourselves to admit that business as usual did not work for most of the people the industry exists to help? If we’re going to embrace yet another period of change – periods that don’t happen often in our complex industry – shouldn’t we first stop and ask ourselves what we’re trying to achieve?
Certainly, COVID has shown that telehealth can be an invaluable tool, particularly for patients in rural and underserved communities that lack access to specialty care. It’s also become clear that many – though not all – healthcare encounters can be effectively conducted from afar. That said, the telehealth tactics that filled the gap during the pandemic were largely stitched together substitutes for existing visit-based workflows: with offices closed, patients scheduled video visits for help managing the side effects of their blood pressure medications or to see their endocrinologist for a quarterly check-in. Anyone whose children slogged through the last year or two of remote learning can tell you that simply virtualizing existing processes doesn’t necessarily improve the experience or the outcomes!
But what if our approach to post-pandemic healthcare came from a patient-driven perspective? We have a fleeting opportunity to advance a care model centered on convenient and equitable access that first prioritizes good outcomes, then selects approaches to care – and locations – tailored to each patient. Using the example of education, imagine how effective it would be if each student, regardless of their school district and aptitude, received such individualized attention.
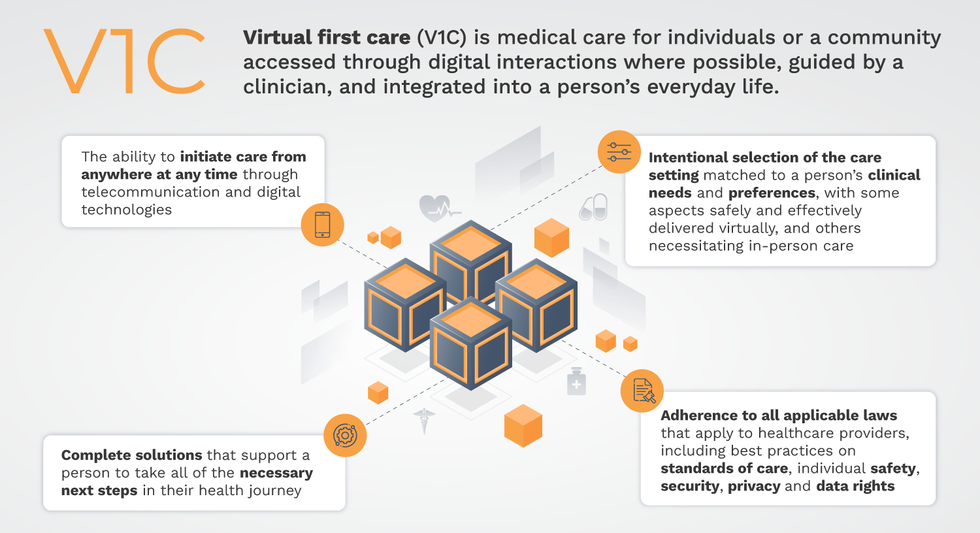
That’s the idea behind virtual-first care (V1C), a new care model centered on convenient, customized, high-quality care that integrates a full suite of services tailored directly to patients’ clinical needs and preferences. This package includes asynchronous communication such as texting; video and other live virtual modes; and in-person options.
V1C goes beyond what you might think of as standard “telehealth” by using evidence-based protocols and tools that include traditional and digital therapeutics and testing, personalized care plans, dynamic patient monitoring, and team-based approaches to care. This could include spit kits mailed for laboratory tests and complementing clinical care with health coaching. V1C also replaces some in-person exams with ongoing monitoring, using sensors for more ‘whole person’ care.
Amidst all this momentum, we have the opportunity to rethink the goals of healthcare innovation, but that means bringing together key stakeholders to demonstrate that sustainable V1C can redefine healthcare.
Established V1C healthcare providers such as Omada, Headspace, and Heartbeat Health, as well as emerging market entrants like Oshi, Visana, and Wellinks, work with a variety of patients who have complicated long-term conditions such as diabetes, heart failure, gastrointestinal illness, endometriosis, and COPD. V1C is comprehensive in ways that are lacking in digital health and its other predecessors: it has the potential to integrate multiple data streams, incorporate more frequent touches and check-ins over time, and manage a much wider range of chronic health conditions, improving lives and reducing disease burden now and in the future.
Recognizing the pandemic-driven interest in virtual care, significant energy and resources are already flowing fast toward V1C. Some of the world’s largest innovators jumped into V1C early on: Verily, Alphabet’s Life Sciences Company, launched Onduo in 2016 to disrupt the diabetes healthcare market, and is now well positioned to scale its solutions. Major insurers like Aetna and United now offer virtual-first plans to members, responding as organizations expand virtual options for employees. Amidst all this momentum, we have the opportunity to rethink the goals of healthcare innovation, but that means bringing together key stakeholders to demonstrate that sustainable V1C can redefine healthcare.
That was the immediate impetus for IMPACT, a consortium of V1C companies, investors, payers and patients founded last year to ensure access to high-quality, evidence-based V1C. Developed by our team at the Digital Medicine Society (DiMe) in collaboration with the American Telemedicine Association (ATA), IMPACT has begun to explore key issues that include giving patients more integrated experiences when accessing both virtual and brick-and-mortar care.
Digital Medicine Society
V1C is not, nor should it be, virtual-only care. In this new era of hybrid healthcare, success will be defined by how well providers help patients navigate the transitions. How do we smoothly hand a patient off from an onsite primary care physician to, say, a virtual cardiologist? How do we get information from a brick-and-mortar to a digital portal? How do you manage dataflow while still staying HIPAA compliant? There are many complex regulatory implications for these new models, as well as an evolving landscape in terms of privacy, security and interoperability. It will be no small task for groups like IMPACT to determine the best path forward.
None of these factors matter unless the industry can recruit and retain clinicians. Our field is facing an unprecedented workforce crisis. Traditional healthcare is making clinicians miserable, and COVID has only accelerated the trend of overworked, disenchanted healthcare workers leaving in droves. Clinicians want more interactions with patients, and fewer with computer screens – call it “More face time, less FaceTime.” No new model will succeed unless the industry can more efficiently deploy its talent – arguably its most scarce and precious resource. V1C can help with alleviating the increasing burden and frustration borne by individual physicians in today’s status quo.
In healthcare, new technological approaches inevitably provoke no shortage of skepticism. Past lessons from Silicon Valley-driven fixes have led to understandable cynicism. But V1C is a different breed of animal. By building healthcare around the patient, not the clinic, V1C can make healthcare work better for patients, payers and providers. We’re at a fork in the road: we can revert back to a broken sick-care system, or dig in and do the hard work of figuring out how this future-forward healthcare system gets financed, organized and executed. As a field, we must find the courage and summon the energy to embrace this moment, and make it a moment of change.

