Elizabeth Holmes Through the Director’s Lens
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.

Elizabeth Holmes.
"The Inventor," a chronicle of Theranos's storied downfall, premiered recently on HBO. Leapsmag reached out to director Alex Gibney, whom The New York Times has called "one of America's most successful and prolific documentary filmmakers," for his perspective on Elizabeth Holmes and the world she inhabited.
Do you think Elizabeth Holmes was a charismatic sociopath from the start — or is she someone who had good intentions, over-promised, and began the lies to keep her business afloat, a "fake it till you make it" entrepreneur like Thomas Edison?
I'm not qualified to say if EH was or is a sociopath. I don't think she started Theranos as a scam whose only purpose was to make money. If she had done so, she surely would have taken more money for herself along the way. I do think that she had good intentions and that she, as you say, "began the lies to keep her business afloat." ([Reporter John] Carreyrou's book points out that those lies began early.) I think that the Edison comparison is instructive for a lot of reasons.
First, Edison was the original "fake-it-till-you-make-it" entrepreneur. That puts this kind of behavior in the mainstream of American business. By saying that, I am NOT endorsing the ethic, just the opposite. As one Enron executive mused about the mendacity there, "Was it fraud or was it bad marketing?" That gives you a sense of how baked-in the "fake it" sensibility is.
"Having a thirst for fame and a noble cause enabled her to think it was OK to lie in service of those goals."
I think EH shares one other thing with Edison, which is a huge ego coupled with a talent for storytelling as long as she is the heroic, larger-than-life main character. It's interesting that EH calls her initial device "Edison." Edison was the world's most famous "inventor," both because of the devices that came out of his shop and and for his ability for "self-invention." As Randall Stross notes in "The Wizard of Menlo Park," he was the first celebrity businessman. In addition to her "good intentions," EH was certainly motivated by fame and glory and many of her lies were in service to those goals.
Having a thirst for fame and a noble cause enabled her to think it was OK to lie in service of those goals. That doesn't excuse the lies. But those noble goals may have allowed EH to excuse them for herself or, more perniciously, to make believe that they weren't lies at all. This is where we get into scary psychological territory.
But rather than thinking of it as freakish, I think it's more productive to think of it as an exaggeration of the way we all lie to others and to ourselves. That's the point of including the Dan Ariely experiment with the dice. In that experiment, most of the subjects cheated more when they thought they were doing it for a good cause. Even more disturbing, that "good cause" allowed them to lie much more effectively because they had come to believe they weren't doing anything wrong. As it turns out, economics isn't a rational practice; it's the practice of rationalizing.
Where EH and Edison differ is that Edison had a firm grip on reality. He knew he could find a way to make the incandescent lightbulb work. There is no evidence that EH was close to making her "Edison" work. But rather than face reality (and possibly adjust her goals) she pretended that her dream was real. That kind of "over-promising" or "bold vision" is one thing when you are making a prototype in the lab. It's a far more serious matter when you are using a deeply flawed system on real patients. EH can tell herself that she had to do that (Walgreens was ready to walk away if she hadn't "gone live") or else Theranos would have run out of money.
But look at the calculation she made: she thought it was worth putting lives at risk in order to make her dream come true. Now we're getting into the realm of the sociopath. But my experience leads me to believe that -- as in the case of the Milgram experiment -- most people don't do terrible things right away, they come to crimes gradually as they become more comfortable with bigger and bigger rationalizations. At Theranos, the more valuable the company became, the bigger grew the lies.
The two whistleblowers come across as courageous heroes, going up against the powerful and intimidating company. The contrast between their youth and lack of power and the old elite backers of Theronos is staggering, and yet justice triumphed. Were the whistleblowers hesitant or afraid to appear in the film, or were they eager to share their stories?
By the time I got to them, they were willing and eager to tell their stories, once I convinced them that I would honor their testimony. In the case of Erika and Tyler, they were nudged to participate by John Carreyrou, in whom they had enormous trust.
"It's simply crazy that no one demanded to see an objective demonstration of the magic box."
Why do you think so many elite veterans of politics and venture capitalism succumbed to Holmes' narrative in the first place, without checking into the details of its technology or financials?
The reasons are all in the film. First, Channing Robertson and many of the old men on her board were clearly charmed by her and maybe attracted to her. They may have rationalized their attraction by convincing themselves it was for a good cause! Second, as Dan Ariely tells us, we all respond to stories -- more than graphs and data -- because they stir us emotionally. EH was a great storyteller. Third, the story of her as a female inventor and entrepreneur in male-dominated Silicon Valley is a tale that they wanted to invest in.
There may have been other factors. EH was very clever about the way she put together an ensemble of credibility. How could Channing Robertson, George Shultz, Henry Kissinger and Jim Mattis all be wrong? And when Walgreens put the Wellness Centers in stores, investors like Rupert Murdoch assumed that Walgreens must have done its due diligence. But they hadn't!
It's simply crazy that no one demanded to see an objective demonstration of the magic box. But that blind faith, as it turns out, is more a part of capitalism than we have been taught.
Do you think that Roger Parloff deserves any blame for the glowing Fortune story on Theranos, since he appears in the film to blame himself? Or was he just one more victim of Theranos's fraud?
He put her on the cover of Fortune so he deserves some blame for the fraud. He still blames himself. That willingness to hold himself to account shows how seriously he takes the job of a journalist. Unlike Elizabeth, Roger has the honesty and moral integrity to admit that he made a mistake. He owned up to it and published a mea culpa. That said, Roger was also a victim because Elizabeth lied to him.
Do you think investors in Silicon Valley, with their FOMO attitudes and deep pockets, are vulnerable to making the same mistake again with a shiny new startup, or has this saga been a sober reminder to do their due diligence first?
Many of the mistakes made with Theranos were the same mistakes made with Enron. We must learn to recognize that we are, by nature, trusting souls. Knowing that should lead us to a guiding slogan: "trust but verify."
The irony of Holmes dancing to "I Can't Touch This" is almost too perfect. How did you find that footage?
It was leaked to us.
"Elizabeth Holmes is now famous for her fraud. Who better to host the re-boot of 'The Apprentice.'"
Holmes is facing up to 20 years in prison for federal fraud charges, but Vanity Fair recently reported that she is seeking redemption, taking meetings with filmmakers for a possible documentary to share her "real" story. What do you think will become of Holmes in the long run?
It's usually a mistake to handicap a trial. My guess is that she will be convicted and do some prison time. But maybe she can convince jurors -- the way she convinced journalists, her board, and her investors -- that, on account of her noble intentions, she deserves to be found not guilty. "Somewhere, over the rainbow…"
After the trial, and possibly prison, I'm sure that EH will use her supporters (like Tim Draper) to find a way to use the virtual currency of her celebrity to rebrand herself and launch something new. Fitzgerald famously said that "there are no second acts in American lives." That may be the stupidest thing he ever said.
Donald Trump failed at virtually every business he ever embarked on. But he became a celebrity for being a fake businessman and used that celebrity -- and phony expertise -- to become president of the United States. Elizabeth Holmes is now famous for her fraud. Who better to host the re-boot of "The Apprentice." And then?
"You Can't Touch This!"
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
Beyond Henrietta Lacks: How the Law Has Denied Every American Ownership Rights to Their Own Cells
A 2017 portrait of Henrietta Lacks.
The common perception is that Henrietta Lacks was a victim of poverty and racism when in 1951 doctors took samples of her cervical cancer without her knowledge or permission and turned them into the world's first immortalized cell line, which they called HeLa. The cell line became a workhorse of biomedical research and facilitated the creation of medical treatments and cures worth untold billions of dollars. Neither Lacks nor her family ever received a penny of those riches.
But racism and poverty is not to blame for Lacks' exploitation—the reality is even worse. In fact all patients, then and now, regardless of social or economic status, have absolutely no right to cells that are taken from their bodies. Some have called this biological slavery.
How We Got Here
The case that established this legal precedent is Moore v. Regents of the University of California.
John Moore was diagnosed with hairy-cell leukemia in 1976 and his spleen was removed as part of standard treatment at the UCLA Medical Center. On initial examination his physician, David W. Golde, had discovered some unusual qualities to Moore's cells and made plans prior to the surgery to have the tissue saved for research rather than discarded as waste. That research began almost immediately.
"On both sides of the case, legal experts and cultural observers cautioned that ownership of a human body was the first step on the slippery slope to 'bioslavery.'"
Even after Moore moved to Seattle, Golde kept bringing him back to Los Angeles to collect additional samples of blood and tissue, saying it was part of his treatment. When Moore asked if the work could be done in Seattle, he was told no. Golde's charade even went so far as claiming to find a low-income subsidy to pay for Moore's flights and put him up in a ritzy hotel to get him to return to Los Angeles, while paying for those out of his own pocket.
Moore became suspicious when he was asked to sign new consent forms giving up all rights to his biological samples and he hired an attorney to look into the matter. It turned out that Golde had been lying to his patient all along; he had been collecting samples unnecessary to Moore's treatment and had turned them into a cell line that he and UCLA had patented and already collected millions of dollars in compensation. The market for the cell lines was estimated at $3 billion by 1990.
Moore felt he had been taken advantage of and filed suit to claim a share of the money that had been made off of his body. "On both sides of the case, legal experts and cultural observers cautioned that ownership of a human body was the first step on the slippery slope to 'bioslavery,'" wrote Priscilla Wald, a professor at Duke University whose career has focused on issues of medicine and culture. "Moore could be viewed as asking to commodify his own body part or be seen as the victim of the theft of his most private and inalienable information."
The case bounced around different levels of the court system with conflicting verdicts for nearly six years until the California Supreme Court ruled on July 9, 1990 that Moore had no legal rights to cells and tissue once they were removed from his body.
The court made a utilitarian argument that the cells had no value until scientists manipulated them in the lab. And it would be too burdensome for researchers to track individual donations and subsequent cell lines to assure that they had been ethically gathered and used. It would impinge on the free sharing of materials between scientists, slow research, and harm the public good that arose from such research.
"In effect, what Moore is asking us to do is impose a tort duty on scientists to investigate the consensual pedigree of each human cell sample used in research," the majority wrote. In other words, researchers don't need to ask any questions about the materials they are using.
One member of the court did not see it that way. In his dissent, Stanley Mosk raised the specter of slavery that "arises wherever scientists or industrialists claim, as defendants have here, the right to appropriate and exploit a patient's tissue for their sole economic benefit—the right, in other words, to freely mine or harvest valuable physical properties of the patient's body. … This is particularly true when, as here, the parties are not in equal bargaining positions."
Mosk also cited the appeals court decision that the majority overturned: "If this science has become for profit, then we fail to see any justification for excluding the patient from participation in those profits."
But the majority bought the arguments that Golde, UCLA, and the nascent biotechnology industry in California had made in amici briefs filed throughout the legal proceedings. The road was now cleared for them to develop products worth billions without having to worry about or share with the persons who provided the raw materials upon which their research was based.
Critical Views
Biomedical research requires a continuous and ever-growing supply of human materials for the foundation of its ongoing work. If an increasing number of patients come to feel as John Moore did, that the system is ripping them off, then they become much less likely to consent to use of their materials in future research.
Some legal and ethical scholars say that donors should be able to limit the types of research allowed for their tissues and researchers should be monitored to assure compliance with those agreements. For example, today it is commonplace for companies to certify that their clothing is not made by child labor, their coffee is grown under fair trade conditions, that food labeled kosher is properly handled. Should we ask any less of our pharmaceuticals than that the donors whose cells made such products possible have been treated honestly and fairly, and share in the financial bounty that comes from such drugs?
Protection of individual rights is a hallmark of the American legal system, says Lisa Ikemoto, a law professor at the University of California Davis. "Putting the needs of a generalized public over the interests of a few often rests on devaluation of the humanity of the few," she writes in a reimagined version of the Moore decision that upholds Moore's property claims to his excised cells. The commentary is in a chapter of a forthcoming book in the Feminist Judgment series, where authors may only use legal precedent in effect at the time of the original decision.
"Why is the law willing to confer property rights upon some while denying the same rights to others?" asks Radhika Rao, a professor at the University of California, Hastings College of the Law. "The researchers who invest intellectual capital and the companies and universities that invest financial capital are permitted to reap profits from human research, so why not those who provide the human capital in the form of their own bodies?" It might be seen as a kind of sweat equity where cash strapped patients make a valuable in kind contribution to the enterprise.
The Moore court also made a big deal about inhibiting the free exchange of samples between scientists. That has become much less the situation over the more than three decades since the decision was handed down. Ironically, this decision, as well as other laws and regulations, have since strengthened the power of patents in biomedicine and by doing so have increased secrecy and limited sharing.
"Although the research community theoretically endorses the sharing of research, in reality sharing is commonly compromised by the aggressive pursuit and defense of patents and by the use of licensing fees that hinder collaboration and development," Robert D. Truog, Harvard Medical School ethicist and colleagues wrote in 2012 in the journal Science. "We believe that measures are required to ensure that patients not bear all of the altruistic burden of promoting medical research."
Additionally, the increased complexity of research and the need for exacting standardization of materials has given rise to an industry that supplies certified chemical reagents, cell lines, and whole animals bred to have specific genetic traits to meet research needs. This has been more efficient for research and has helped to ensure that results from one lab can be reproduced in another.
The Court's rationale of fostering collaboration and free exchange of materials between researchers also has been undercut by the changing structure of that research. Big pharma has shrunk the size of its own research labs and over the last decade has worked out cooperative agreements with major research universities where the companies contribute to the research budget and in return have first dibs on any findings (and sometimes a share of patent rights) that come out of those university labs. It has had a chilling effect on the exchange of materials between universities.
Perhaps tracking cell line donors and use restrictions on those donations might have been burdensome to researchers when Moore was being litigated. Some labs probably still kept their cell line records on 3x5 index cards, computers were primarily expensive room-size behemoths with limited capacity, the internet barely existed, and there was no cloud storage.
But that was the dawn of a new technological age and standards have changed. Now cell lines are kept in state-of-the-art sub zero storage units, tagged with the source, type of tissue, date gathered and often other information. Adding a few more data fields and contacting the donor if and when appropriate does not seem likely to disrupt the research process, as the court asserted.
Forging the Future
"U.S. universities are awarded almost 3,000 patents each year. They earn more than $2 billion each year from patent royalties. Sharing a modest portion of these profits is a novel method for creating a greater sense of fairness in research relationships that we think is worth exploring," wrote Mark Yarborough, a bioethicist at the University of California Davis Medical School, and colleagues. That was penned nearly a decade ago and those numbers have only grown.
The Michigan BioTrust for Health might serve as a useful model in tackling some of these issues. Dried blood spots have been collected from all newborns for half a century to be tested for certain genetic diseases, but controversy arose when the huge archive of dried spots was used for other research projects. As a result, the state created a nonprofit organization to in essence become a biobank and manage access to these spots only for specific purposes, and also to share any revenue that might arise from that research.
"If there can be no property in a whole living person, does it stand to reason that there can be no property in any part of a living person? If there were, can it be said that this could equate to some sort of 'biological slavery'?" Irish ethicist Asim A. Sheikh wrote several years ago. "Any amount of effort spent pondering the issue of 'ownership' in human biological materials with existing law leaves more questions than answers."
Perhaps the biggest question will arise when -- not if but when -- it becomes possible to clone a human being. Would a human clone be a legal person or the property of those who created it? Current legal precedent points to it being the latter.
Today, October 4, is the 70th anniversary of Henrietta Lacks' death from cancer. Over those decades her immortalized cells have helped make possible miraculous advances in medicine and have had a role in generating billions of dollars in profits. Surviving family members have spoken many times about seeking a share of those profits in the name of social justice; they intend to file lawsuits today. Such cases will succeed or fail on their own merits. But regardless of their specific outcomes, one can hope that they spark a larger public discussion of the role of patients in the biomedical research enterprise and lead to establishing a legal and financial claim for their contributions toward the next generation of biomedical research.
Is a Successful HIV Vaccine Finally on the Horizon?
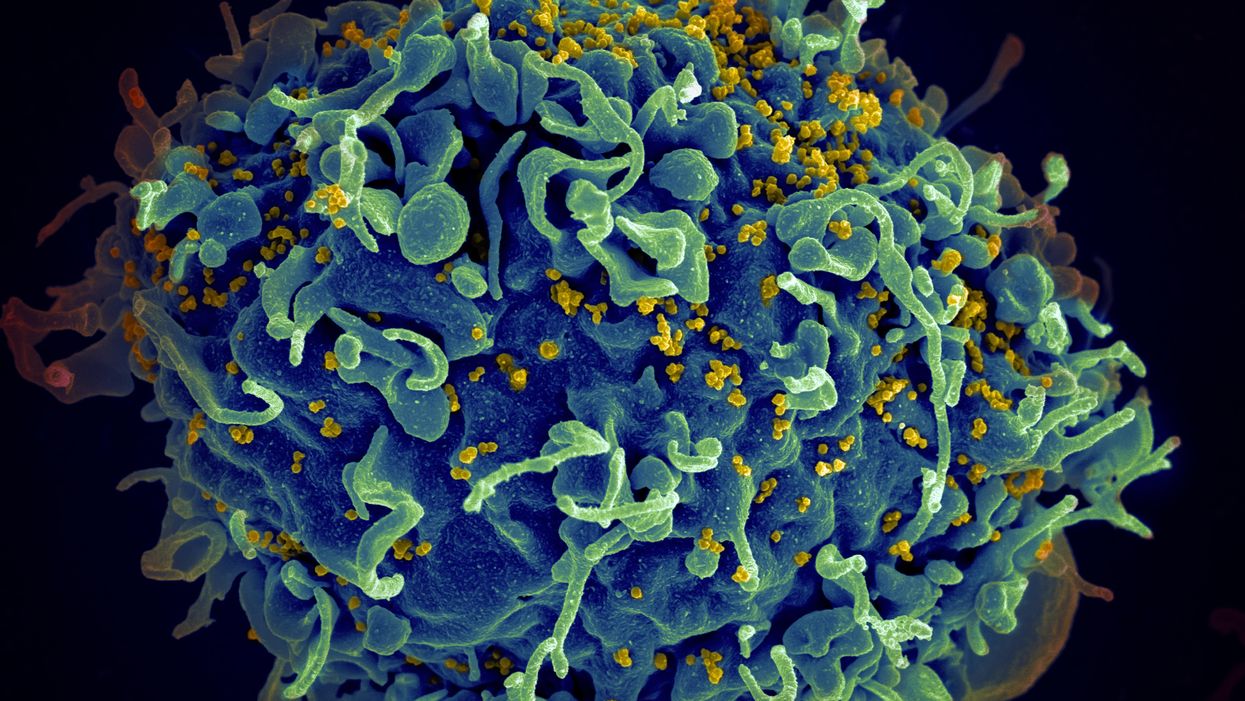
The HIV virus (yellow) infecting a human cell.
Few vaccines have been as complicated—and filled with false starts and crushed hopes—as the development of an HIV vaccine.
While antivirals help HIV-positive patients live longer and reduce viral transmission to virtually nil, these medications must be taken for life, and preventative medications like pre-exposure prophylaxis, known as PrEP, need to be taken every day to be effective. Vaccines, even if they need boosters, would make prevention much easier.
In August, Moderna began human trials for two HIV vaccine candidates based on messenger RNA.
As they have with the Covid-19 pandemic, mRNA vaccines could change the game. The technology could be applied for gene editing therapy, cancer, other infectious diseases—even a universal influenza vaccine.
In the past, three other mRNA vaccines completed phase-2 trials without success. But the easily customizable platforms mean the vaccines can be tweaked better to target HIV as researchers learn more.
Ever since HIV was discovered as the virus causing AIDS, researchers have been searching for a vaccine. But the decades-long journey has so far been fruitless; while some vaccine candidates showed promise in early trials, none of them have worked well among later-stage clinical trials.
There are two main reasons for this: HIV evolves incredibly quickly, and the structure of the virus makes it very difficult to neutralize with antibodies.
"We in HIV medicine have been desperate to find a vaccine that has effectiveness, but this goal has been elusive so far."
"You know the panic that goes on when a new coronavirus variant surfaces?" asked John Moore, professor of microbiology and immunology at Weill Cornell Medicine who has researched HIV vaccines for 25 years. "With HIV, that kind of variation [happens] pretty much every day in everybody who's infected. It's just orders of magnitude more variable a virus."
Vaccines like these usually work by imitating the outer layer of a virus to teach cells how to recognize and fight off the real thing off before it enters the cell. "If you can prevent landing, you can essentially keep the virus out of the cell," said Larry Corey, the former president and director of the Fred Hutchinson Cancer Research Center who helped run a recent trial of a Johnson & Johnson HIV vaccine candidate, which failed its first efficacy trial.
Like the coronavirus, HIV also has a spike protein with a receptor-binding domain—what Moore calls "the notorious RBD"—that could be neutralized with antibodies. But while that target sticks out like a sore thumb in a virus like SARS-CoV-2, in HIV it's buried under a dense shield. That's not the only target for neutralizing the virus, but all of the targets evolve rapidly and are difficult to reach.
"We understand these targets. We know where they are. But it's still proving incredibly difficult to raise antibodies against them by vaccination," Moore said.
In fact, mRNA vaccines for HIV have been under development for years. The Covid vaccines were built on decades of that research. But it's not as simple as building on this momentum, because of how much more complicated HIV is than SARS-CoV-2, researchers said.
"They haven't succeeded because they were not designed appropriately and haven't been able to induce what is necessary for them to induce," Moore said. "The mRNA technology will enable you to produce a lot of antibodies to the HIV envelope, but if they're the wrong antibodies that doesn't solve the problem."
Part of the problem is that the HIV vaccines have to perform better than our own immune systems. Many vaccines are created by imitating how our bodies overcome an infection, but that doesn't happen with HIV. Once you have the virus, you can't fight it off on your own.
"The human immune system actually does not know how to innately cure HIV," Corey said. "We needed to improve upon the human immune system to make it quicker… with Covid. But we have to actually be better than the human immune system" with HIV.
But in the past few years, there have been impressive leaps in understanding how an HIV vaccine might work. Scientists have known for decades that neutralizing antibodies are key for a vaccine. But in 2010 or so, they were able to mimic the HIV spike and understand how antibodies need to disable the virus. "It helps us understand the nature of the problem, but doesn't instantly solve the problem," Moore said. "Without neutralizing antibodies, you don't have a chance."
Because the vaccines need to induce broadly neutralizing antibodies, and because it's very difficult to neutralize the highly variable HIV, any vaccine will likely be a series of shots that teach the immune system to be on the lookout for a variety of potential attacks.
"Each dose is going to have to have a different purpose," Corey said. "And we hope by the end of the third or fourth dose, we will achieve the level of neutralization that we want."
That's not ideal, because each individual component has to be made and tested—and four shots make the vaccine harder to administer.
"You wouldn't even be going down that route, if there was a better alternative," Moore said. "But there isn't a better alternative."
The mRNA platform is exciting because it is easily customizable, which is especially important in fighting against a shapeshifting, complicated virus. And the mRNA platform has shown itself, in the Covid pandemic, to be safe and quick to make. Effective Covid vaccines were comparatively easy to develop, since the coronavirus is easier to battle than HIV. But companies like Moderna are capitalizing on their success to launch other mRNA therapeutics and vaccines, including the HIV trial.
"You can make the vaccine in two months, three months, in a research lab, and not a year—and the cost of that is really less," Corey said. "It gives us a chance to try many more options, if we've got a good response."
In a trial on macaque monkeys, the Moderna vaccine reduced the chances of infection by 85 percent. "The mRNA platform represents a very promising approach for the development of an HIV vaccine in the future," said Dr. Peng Zhang, who is helping lead the trial at the National Institute of Allergy and Infectious Diseases.
Moderna's trial in humans represents "a very exciting possibility for the prevention of HIV infection," Dr. Monica Gandhi, director of the UCSF-Gladstone Center for AIDS Research, said in an email. "We in HIV medicine have been desperate to find a vaccine that has effectiveness, but this goal has been elusive so far."
If a successful HIV vaccine is developed, the series of shots could include an mRNA shot that primes the immune system, followed by protein subunits that generate the necessary antibodies, Moore said.
"I think it's the only thing that's worth doing," he said. "Without something complicated like that, you have no chance of inducing broadly neutralizing antibodies."
"I can't guarantee you that's going to work," Moore added. "It may completely fail. But at least it's got some science behind it."