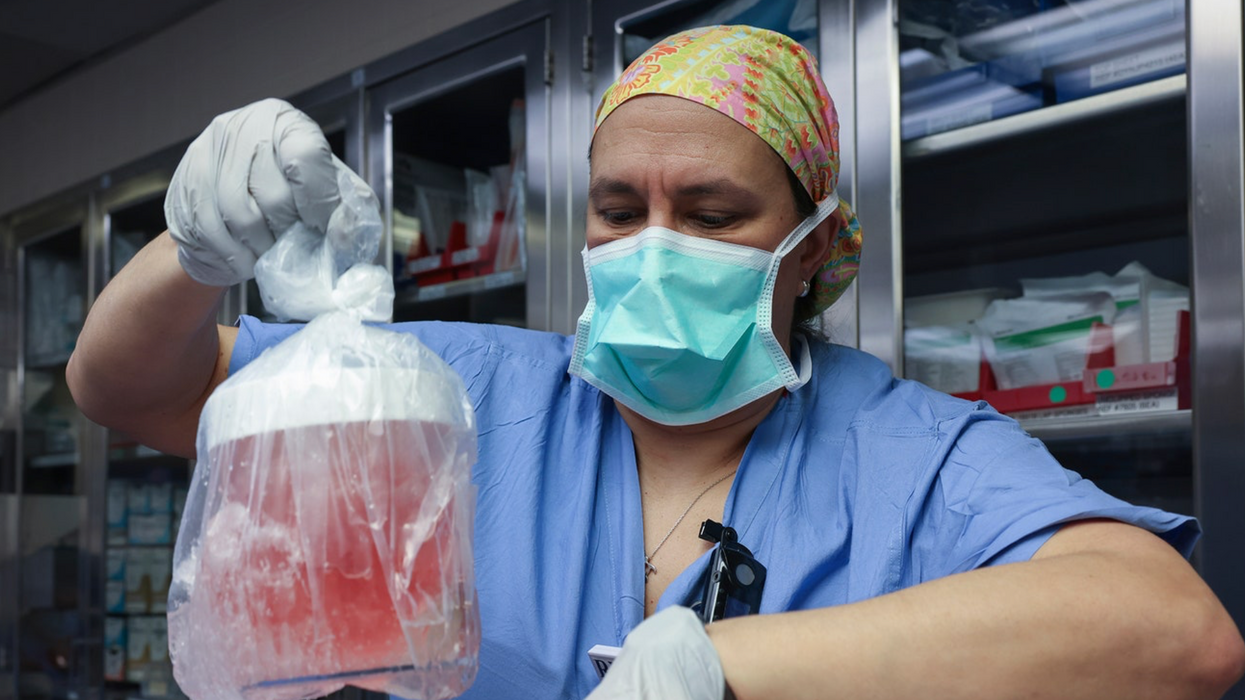
Gene Editing of Embryos Is Both Ethical and Prudent
Human cells under a microscope
BIG QUESTION OF THE MONTH: Should we use CRISPR, the new technique that enables precise DNA editing, to change the genes of human embryos to eradicate disease--or even to enhance desirable traits? LeapsMag invited three leading experts to weigh in.
Now that researchers around the world have begun to edit the genes of human embryos with CRISPR, the ethical debate has become more timely than ever: Should this kind of research be on the table or categorically ruled out?
All of us need gene editing to be pursued, and if possible, made safe enough to use in humans. Not only to pave the way for effective procedures on adults, but more importantly, to keep open the possibility of using gene editing to protect embryos from susceptibility to major diseases and to prevent other debilitating genetic conditions from being passed on through them to future generations.
Objections to gene editing in embryos rest on three fallacious arguments:
- Gene editing is wrong because it affects future generations, the argument being that the human germline is sacred and inviolable.
- It constitutes an unknown and therefore unacceptable risk to future generations.
- The inability to obtain the consent of those future generations means we must not use gene editing.
We should be clear that there is no precautionary approach; just as justice delayed is justice denied, so therapy delayed is therapy denied.
Regarding the first point, many objections to germline interventions emphasize that such interventions are objectionable in that they affect "generations down the line". But this is true, not only of all assisted reproductive technologies, but of all reproduction of any kind.
Sexual reproduction would never have been licensed by regulators
As for the second point, every year an estimated 7.9 million children - 6% of total births worldwide - are born with a serious birth defect of genetic or partially genetic origin. Had sexual reproduction been invented by scientists rather than resulting from our evolved biology, it would never have been licensed by regulators - far too inefficient and dangerous!
If the appropriate benchmark for permissible risk of harm to future generations is sexual reproduction, other germline-changing techniques would need to demonstrate severe foreseeable dangers to fail.
Raising the third point in his statement on gene-editing in human embryos, Francis S. Collins, director of the National Institutes of Health, stated: "The strong arguments against engaging in this activity remain … These include the serious and unquantifiable safety issues, ethical issues presented by altering the germline in a way that affects the next generation without their consent."
"Serious and unquantifiable" safety issues feature in all new technologies but consent is simply irrelevant for the simple and sufficient reason that there are no relevant people in existence capable of either giving or withholding consent to these sorts of changes in their own germline.
We all have to make decisions for future people without considering their inevitably absent consent. All would-be/might-be parents make numerous decisions about issues that might affect their future children. They do this all the time without thinking about consent of the children.
George Bernard Shaw and Isadora Duncan were possibly apocryphal exceptions. She, apparently, said to him something like: "Why don't we have a child? With my looks and your brains it cannot fail," and received Shaw's more rational assessment: "Yes, but what if it has my looks and your brains?"
If there is a discernible duty here, it is surely to try to create the best possible child, a child who will be the healthiest, most intelligent and most resilient to disease reasonably possible given the parents' other priorities. This is why we educate and vaccinate our children and give them a good diet if we can. That is what it is to act for the best, all things considered. This we have moral reasons to do; but they are not necessarily overriding reasons.
"There is no morally significant line between therapy and enhancement."
There is no morally significant line that can be drawn between therapy and enhancement. As I write these words in my London apartment, I am bathed in synthetic sunshine, one of the oldest and most amazing enhancement technologies. Before its invention, our ancestors had to rest or hide in the dark. With the advent of synthetic sunshine--firelight, candlelight, lamplight and electric light--we could work and play as long as we wished.Steven Hawking initially predicted that we might have about 7.6 billion years to go before the Earth gives up on us; he recently revised his position in relation to the Earth's continuing habitability as opposed to its physical survival: "We must also continue to go into space for the future of humanity," he said recently. "I don't think we will survive another thousand years without escaping beyond our fragile planet."
We will at some point have to escape both beyond our fragile planet and our fragile nature. One way to enhance our capacity to do both these things is by improving on human nature where we can do so in ways that are "safe enough." What we all have an inescapable moral duty to do is to continue with scientific investigation of gene editing techniques to the point at which we can make a rational choice. We must certainly not stop now.
At the end of a 2015 summit where I spoke about this issue, the renowned Harvard geneticist George Church noted that gene editing "opens up the possibility of not just transplantation from pigs to humans but the whole idea that a pig organ is perfectible…Gene editing could ensure the organs are very clean, available on demand and healthy, so they could be superior to human donor organs."
"We know for sure that in the future there will be no more human beings and no more planet Earth."
We know for sure that in the future there will be no more human beings and no more planet Earth. Either we will have been wiped out by our own foolishness or by brute forces of nature, or we will have further evolved by a process more rational and much quicker than Darwinian evolution--a process I described in my book Enhancing Evolution. Even more certain is that there will be no more planet Earth. Our sun will die, and with it, all possibility of life on this planet.As I say in my recent book How to Be Good:
By the time this happens, we may hope that our better evolved successors will have developed the science and the technology needed to survive and to enable us (them) to find and colonize another planet or perhaps even to build another planet; and in the meanwhile, to cope better with the problems presented by living on this planet.
Editor's Note: Check out the viewpoints expressing condemnation and mild curiosity.
Urinary tract infections account for more than 8 million trips to the doctor each year.
Few things are more painful than a urinary tract infection (UTI). Common in men and women, these infections account for more than 8 million trips to the doctor each year and can cause an array of uncomfortable symptoms, from a burning feeling during urination to fever, vomiting, and chills. For an unlucky few, UTIs can be chronic—meaning that, despite treatment, they just keep coming back.
But new research, presented at the European Association of Urology (EAU) Congress in Paris this week, brings some hope to people who suffer from UTIs.
Clinicians from the Royal Berkshire Hospital presented the results of a long-term, nine-year clinical trial where 89 men and women who suffered from recurrent UTIs were given an oral vaccine called MV140, designed to prevent the infections. Every day for three months, the participants were given two sprays of the vaccine (flavored to taste like pineapple) and then followed over the course of nine years. Clinicians analyzed medical records and asked the study participants about symptoms to check whether any experienced UTIs or had any adverse reactions from taking the vaccine.
The results showed that across nine years, 48 of the participants (about 54%) remained completely infection-free. On average, the study participants remained infection free for 54.7 months—four and a half years.
“While we need to be pragmatic, this vaccine is a potential breakthrough in preventing UTIs and could offer a safe and effective alternative to conventional treatments,” said Gernot Bonita, Professor of Urology at the Alta Bro Medical Centre for Urology in Switzerland, who is also the EAU Chairman of Guidelines on Urological Infections.
The news comes as a relief not only for people who suffer chronic UTIs, but also to doctors who have seen an uptick in antibiotic-resistant UTIs in the past several years. Because UTIs usually require antibiotics, patients run the risk of developing a resistance to the antibiotics, making infections more difficult to treat. A preventative vaccine could mean less infections, less antibiotics, and less drug resistance overall.
“Many of our participants told us that having the vaccine restored their quality of life,” said Dr. Bob Yang, Consultant Urologist at the Royal Berkshire NHS Foundation Trust, who helped lead the research. “While we’re yet to look at the effect of this vaccine in different patient groups, this follow-up data suggests it could be a game-changer for UTI prevention if it’s offered widely, reducing the need for antibiotic treatments.”
MILESTONE: Doctors have transplanted a pig organ into a human for the first time in history
A surgeon at Massachusetts General Hospital prepares a pig organ for transplant.
Surgeons at Massachusetts General Hospital made history last week when they successfully transplanted a pig kidney into a human patient for the first time ever.
The recipient was a 62-year-old man named Richard Slayman who had been living with end-stage kidney disease caused by diabetes. While Slayman had received a kidney transplant in 2018 from a human donor, his diabetes ultimately caused the kidney to fail less than five years after the transplant. Slayman had undergone dialysis ever since—a procedure that uses an artificial kidney to remove waste products from a person’s blood when the kidneys are unable to—but the dialysis frequently caused blood clots and other complications that landed him in the hospital multiple times.
As a last resort, Slayman’s kidney specialist suggested a transplant using a pig kidney provided by eGenesis, a pharmaceutical company based in Cambridge, Mass. The highly experimental surgery was made possible with the Food and Drug Administration’s “compassionate use” initiative, which allows patients with life-threatening medical conditions access to experimental treatments.
The new frontier of organ donation
Like Slayman, more than 100,000 people are currently on the national organ transplant waiting list, and roughly 17 people die every day waiting for an available organ. To make up for the shortage of human organs, scientists have been experimenting for the past several decades with using organs from animals such as pigs—a new field of medicine known as xenotransplantation. But putting an animal organ into a human body is much more complicated than it might appear, experts say.
“The human immune system reacts incredibly violently to a pig organ, much more so than a human organ,” said Dr. Joren Madsen, director of the Mass General Transplant Center. Even with immunosuppressant drugs that suppress the body’s ability to reject the transplant organ, Madsen said, a human body would reject an animal organ “within minutes.”
So scientists have had to use gene-editing technology to change the animal organs so that they would work inside a human body. The pig kidney in Slayman’s surgery, for instance, had been genetically altered using CRISPR-Cas9 technology to remove harmful pig genes and add human ones. The kidney was also edited to remove pig viruses that could potentially infect a human after transplant.
With CRISPR technology, scientists have been able to prove that interspecies organ transplants are not only possible, but may be able to successfully work long term, too. In the past several years, scientists were able to transplant a pig kidney into a monkey and have the monkey survive for more than two years. More recently, doctors have transplanted pig hearts into human beings—though each recipient of a pig heart only managed to live a couple of months after the transplant. In one of the patients, researchers noted evidence of a pig virus in the man’s heart that had not been identified before the surgery and could be a possible explanation for his heart failure.
So far, so good
Slayman and his medical team ultimately decided to pursue the surgery—and the risk paid off. When the pig organ started producing urine at the end of the four-hour surgery, the entire operating room erupted in applause.
Slayman is currently receiving an infusion of immunosuppressant drugs to prevent the kidney from being rejected, while his doctors monitor the kidney’s function with frequent ultrasounds. Slayman is reported to be “recovering well” at Massachusetts General Hospital and is expected to be discharged within the next several days.