Harvard Researchers Are Using a Breakthrough Tool to Find the Antibodies That Best Knock Out the Coronavirus
Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.
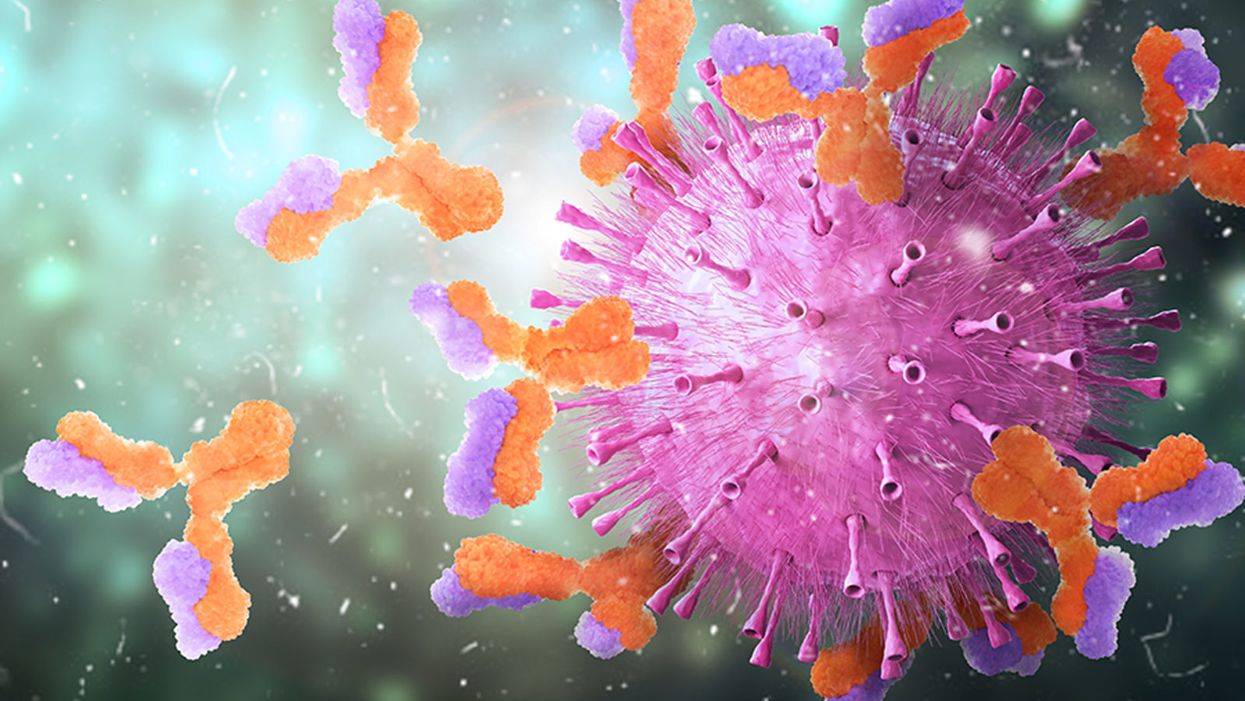
Knowing which antibodies bind best to the coronavirus can help guide new medicines and vaccine development.
To find a cure for a deadly infectious disease in the 1995 medical thriller Outbreak, scientists extract the virus's antibodies from its original host—an African monkey.
"When a person is infected, the immune system makes antibodies kind of blindly."
The antibodies prevent the monkeys from getting sick, so doctors use these antibodies to make the therapeutic serum for humans. With SARS-CoV-2, the original hosts might be bats or pangolins, but scientists don't have access to either, so they are turning to the humans who beat the virus.
Patients who recovered from COVID-19 are valuable reservoirs of viral antibodies and may help scientists develop efficient therapeutics, says Stephen J. Elledge, professor of genetics and medicine at Harvard Medical School in Boston. Studying the structure of the antibodies floating in their blood can help understand what their immune systems did right to kill the pathogen.
When viruses invade the body, the immune system builds antibodies against them. The antibodies work like Velcro strips—they use special spots on their surface called paratopes to cling to the specific spots on the viral shell called epitopes. Once the antibodies circulating in the blood find their "match," they cling on to the virus and deactivate it.
But that process is far from simple. The epitopes and paratopes are built of various peptides that have complex shapes, are folded in specific ways, and may carry an electrical charge that repels certain molecules. Only when all of these parameters match, an antibody can get close enough to a viral particle—and shut it out.
So the immune system forges many different antibodies with varied parameters in hopes that some will work. "When a person is infected, the immune system makes antibodies kind of blindly," Elledge says. "It's doing a shotgun approach. It's not sure which ones will work, but it knows once it's made a good one that works."
Elledge and his team want to take the guessing out of the process. They are using their home-built tool VirScan to comb through the blood samples of the recovered COVID-19 patients to see what parameters the efficient antibodies should have. First developed in 2015, the VirScan has a library of epitopes found on the shells of viruses known to afflict humans, akin to a database of criminals' mug shots maintained by the police.
Originally, VirScan was meant to reveal which pathogens a person overcame throughout a lifetime, and could identify over 1,000 different strains of viruses and bacteria. When the team ran blood samples against the VirScan's library, the tool would pick out all the "usual suspects." And unlike traditional blood tests called ELISA, which can only detect one pathogen at a time, VirScan can detect all of them at once. Now, the team has updated VirScan with the SARS-CoV-2 "mug shot" and is beginning to test which antibodies from the recovered patients' blood will bind to them.
Knowing which antibodies bind best can also help fine-tune vaccines.
Obtaining blood samples was a challenge that caused some delays. "So far most of the recovered patients have been in China and those samples are hard to get," Elledge says. It also takes a person five to 10 days to develop antibodies, so the blood must be drawn at the right time during the illness. If a person is asymptomatic, it's hard to pinpoint the right moment. "We just got a couple of blood samples so we are testing now," he said. The team hopes to get some results very soon.
Elucidating the structure of efficient antibodies can help create therapeutics for COVID-19. "VirScan is a powerful technology to study antibody responses," says Harvard Medical School professor Dan Barouch, who also directs the Center for Virology and Vaccine Research. "A detailed understanding of the antibody responses to COVID-19 will help guide the design of next-generation vaccines and therapeutics."
For example, scientists can synthesize antibodies to specs and give them to patients as medicine. Once vaccines are designed, medics can use VirScan to see if those vaccinated again COVID-19 generate the necessary antibodies.
Knowing which antibodies bind best can also help fine-tune vaccines. Sometimes, viruses cause the immune system to generate antibodies that don't deactivate it. "We think the virus is trying to confuse the immune system; it is its business plan," Elledge says—so those unhelpful antibodies shouldn't be included in vaccines.
More importantly, VirScan can also tell which people have developed immunity to SARS-CoV-2 and can return to their workplaces and businesses, which is crucial to restoring the economy. Knowing one's immunity status is especially important for doctors working on the frontlines, Elledge notes. "The resistant ones can intubate the sick."
Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.
How to have a good life, based on the world's longest study of happiness
In 1938, Harvard began an in-depth study of the secrets to happiness. It's still going, and in today's podcast episode, the study's director, Bob Waldinger, tells Leaps.org about the keys to a satisfying life, based on 85 years of research.
What makes for a good life? Such a simple question, yet we don't have great answers. Most of us try to figure it out as we go along, and many end up feeling like they never got to the bottom of it.
Shouldn't something so important be approached with more scientific rigor? In 1938, Harvard researchers began a study to fill this gap. Since then, they’ve followed hundreds of people over the course of their lives, hoping to identify which factors are key to long-term satisfaction.
Eighty-five years later, the Harvard Study of Adult Development is still going. And today, its directors, the psychiatrists Bob Waldinger and Marc Shulz, have published a book that pulls together the study’s most important findings. It’s called The Good Life: Lessons from the World’s Longest Scientific Study of Happiness.
In this podcast episode, I talked with Dr. Waldinger about life lessons that we can mine from the Harvard study and his new book.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
More background on the study
Back in the 1930s, the research began with 724 people. Some were first-year Harvard students paying full tuition, others were freshmen who needed financial help, and the rest were 14-year-old boys from inner city Boston – white males only. Fortunately, the study team realized the error of their ways and expanded their sample to include the wives and daughters of the first participants. And Waldinger’s book focuses on the Harvard study findings that can be corroborated by evidence from additional research on the lives of people of different races and other minorities.
The study now includes over 1,300 relatives of the original participants, spanning three generations. Every two years, the participants have sent the researchers a filled-out questionnaire, reporting how their lives are going. At five-year intervals, the research team takes a peek their health records and, every 15 years, the psychologists meet their subjects in-person to check out their appearance and behavior.
But they don’t stop there. No, the researchers factor in multiple blood samples, DNA, images from body scans, and even the donated brains of 25 participants.

Robert Waldinger, director of the Harvard Study of Adult Development.
Katherine Taylor
Dr. Waldinger is Clinical Professor of Psychiatry at Harvard Medical School, in addition to being Director of the Harvard Study of Adult Development. He got his M.D. from Harvard Medical School and has published numerous scientific papers he’s a practicing psychiatrist and psychoanalyst, he teaches Harvard medical students, and since that is clearly not enough to keep him busy, he’s also a Zen priest.
His book is a must-read if you’re looking for scientific evidence on how to design your life for more satisfaction so someday in the future you can look back on it without regret, and this episode was an amazing conversation in which Dr. Waldinger breaks down many of the cliches about the good life, making his advice real and tangible. We also get into what he calls “side-by-side” relationships, personality traits for the good life, and the downsides of being too strict about work-life balance.
Show links
- Bob Waldinger
- Waldinger's book, The Good Life: Lessons from the World's Longest Scientific Study of Happiness
- The Harvard Study of Adult Development
- Waldinger's Ted Talk
- Gallup report finding that people with good friends at work have higher engagement with their jobs
- The link between relationships and well-being
- Those with social connections live longer
The Friday Five: A new blood test to detect Alzheimer's
A new blood test has been developed to detect Alzheimer's. Other promising studies covered in this week's Friday Five include: vets with PTSD can take their psychologist anywhere with a new device, intermittent fasting could improve circadian rhythms, a new year's resolution for living longer, and a discovery in 3-D printing eye tissue.
The Friday Five covers five stories in research that you may have missed this week. There are plenty of controversies and troubling ethical issues in science – and we get into many of them in our online magazine – but this news roundup focuses on scientific creativity and progress to give you a therapeutic dose of inspiration headed into the weekend.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
Here are the promising studies covered in this week's Friday Five:
- A blood test to detect Alzheimer's
- War vets can take their psychologist wherever they go
- Does intermittent fasting affect circadian rhythms?
- A new year's resolution for living longer
- 3-D printed eyes?