I'm a Transplant Surgeon Who Designed the Breakthrough That Saved My Own Life
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
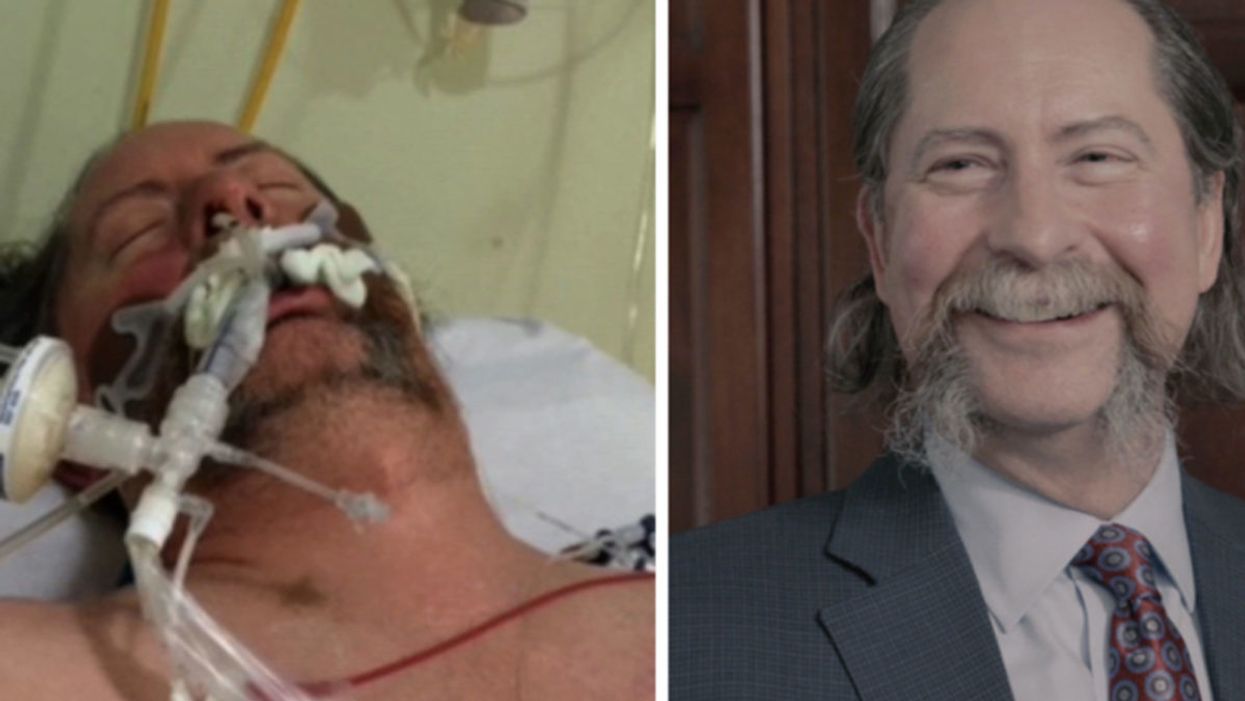
Dr. Robert Montgomery, the director of NYU Langone's Transplant Institute, is ironically the recipient of a heart transplant.
[Ed. Note: This is the fourth episode in our Moonshot series, which explores four cutting-edge scientific developments that stand to fundamentally transform our world.]
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
Abortions Before Fetal Viability Are Legal: Might Science and the Change on the Supreme Court Undermine That?
The United States Supreme Court Building in Washington, D.C.
This article is part of the magazine, "The Future of Science In America: The Election Issue," co-published by LeapsMag, the Aspen Institute Science & Society Program, and GOOD.
Viability—the potential for a fetus to survive outside the womb—is a core dividing line in American law. For almost 50 years, the Supreme Court of the United States has struck down laws that ban all or most abortions, ruling that women's constitutional rights include choosing to end pregnancies before the point of viability. Once viability is reached, however, states have a "compelling interest" in protecting fetal life. At that point, states can choose to ban or significantly restrict later-term abortions provided states allow an exception to preserve the life or health of the mother.
This distinction between a fetus that could survive outside its mother's body, albeit with significant medical intervention, and one that could not, is at the heart of the court's landmark 1973 decision in Roe v. Wade. The framework of viability remains central to the country's abortion law today, even as some states have passed laws in the name of protecting women's health that significantly undermine Roe. Over the last 30 years, the Supreme Court has upheld these laws, which have the effect of restricting pre-viability abortion access, imposing mandatory waiting periods, requiring parental consent for minors, and placing restrictions on abortion providers.
Viability has always been a slippery notion on which to pin legal rights.
Today, the Guttmacher Institute reports that more than half of American women live in states whose laws are considered hostile to abortion, largely as a result of these intrusions on pre-viability abortion access. Nevertheless, the viability framework stands: while states can pass pre-viability abortion restrictions that (ostensibly) protect the health of the woman or that strike some kind a balance between women's rights and fetal life, it is only after viability that they can completely favor fetal life over the rights of the woman (with limited exceptions when the woman's life is threatened). As a result, judges have struck down certain states' so-called heartbeat laws, which tried to prohibit abortions after detection of a fetal heartbeat (as early as six weeks of pregnancy). Bans on abortion after 12 or 15 weeks' gestation have also been reversed.
Now, with a new Supreme Court Justice expected to be hostile to abortion rights, advances in the care of preterm babies and ongoing research on artificial wombs suggest that the point of viability is already sooner than many assume and could soon be moved radically earlier in gestation, potentially providing a legal basis for earlier and earlier abortion bans.
Viability has always been a slippery notion on which to pin legal rights. It represents an inherently variable and medically shifting moment in the pregnancy timeline that the Roe majority opinion declined to firmly define, noting instead that "[v]iability is usually placed at about seven months (28 weeks) but may occur earlier, even at 24 weeks." Even in 1977, this definition was an optimistic generalization. Every baby is different, and while some 28-week infants born the year Roe was decided did indeed live into adulthood, most died at or shortly after birth. The prognosis for infants born at 24 weeks was much worse.
Today, a baby born at 28 weeks' gestation can be expected to do much better, largely due to the development of surfactant treatment in the early 1990s to help ease the air into babies' lungs. Now, the majority of 24-week-old babies can survive, and several very premature babies, born just shy of 22 weeks' gestation, have lived into childhood. All this variability raises the question: Should the law take a very optimistic, if largely unrealistic, approach to defining viability and place it at 22 weeks, even though the overall survival rate for those preemies remains less than 10% today? Or should the law recognize that keeping a premature infant alive requires specialist care, meaning that actual viability differs not just pregnancy-to-pregnancy but also by healthcare facility and from country to country? A 24-week premature infant born in a rural area or in a developing nation may not be viable as a practical matter, while one born in a major U.S. city with access to state-of-the-art care has a greater than 70% chance of survival. Just as some extremely premature newborns survive, some full-term babies die before, during, or soon after birth, regardless of whether they have access to advanced medical care.
To be accurate, viability should be understood as pregnancy-specific and should take into account the healthcare resources available to that woman. But state laws can't capture this degree of variability by including gestation limits in their abortion laws. Instead, many draw a somewhat arbitrary line at 22, 24, or 28 weeks' gestation, regardless of the particulars of the pregnancy or the medical resources available in that state.
As variable and resource-dependent as viability is today, science may soon move that point even earlier. Ectogenesis is a term coined in 1923 for the growth of an organism outside the body. Long considered science fiction, this technology has made several key advances in the past few years, with scientists announcing in 2017 that they had successfully gestated premature lamb fetuses in an artificial womb for four weeks. Currently in development for use in human fetuses between 22 and 23 weeks' gestation, this technology will almost certainly seek to push viability earlier in pregnancy.
Ectogenesis and other improvements in managing preterm birth deserve to be celebrated, offering new hope to the parents of very premature infants. But in the U.S., and in other nations whose abortion laws are fixed to viability, these same advances also pose a threat to abortion access. Abortion opponents have long sought to move the cutoff for legal abortions, and it is not hard to imagine a state prohibiting all abortions after 18 or 20 weeks by arguing that medical advances render this stage "the new viability," regardless of whether that level of advanced care is available to women in that state. If ectogenesis advances further, the limit could be moved to keep pace.
The Centers for Disease Control and Prevention reports that over 90% of abortions in America are performed at or before 13 weeks, meaning that in the short term, only a small number women would be affected by shifting viability standards. Yet these women are in difficult situations and deserve care and consideration. Research has shown that women seeking later terminations often did not recognize that they were pregnant or had their dates quite wrong, while others report that they had trouble accessing a termination earlier in pregnancy, were afraid to tell their partner or parents, or only recently received a diagnosis of health problems with the fetus.
Shifts in viability over the past few decades have already affected these women, many of whom report struggling to find a provider willing to perform a termination at 18 or 20 weeks out of concern that the woman may have her dates wrong. Ever-earlier gestational limits would continue this chilling effect, making doctors leery of terminating a pregnancy that might be within 2–4 weeks of each new ban. Some states' existing gestational limits on abortion are also inconsistent with prenatal care, which includes genetic testing between 12 and 20 weeks' gestation, as well as an anatomy scan to check the fetus's organ development performed at approximately 20 weeks. If viability moves earlier, prenatal care will be further undermined.
Perhaps most importantly, earlier and earlier abortion bans are inconsistent with the rights and freedoms on which abortion access is based, including recognition of each woman's individual right to bodily integrity and decision-making authority over her own medical care. Those rights and freedoms become meaningless if abortion bans encroach into the weeks that women need to recognize they are pregnant, assess their options, seek medical advice, and access appropriate care. Fetal viability, with its shifting goalposts, isn't the best framework for abortion protection in light of advancing medical science.
Ideally, whether to have an abortion would be a decision that women make in consultation with their doctors, free of state interference. The vast majority of women already make this decision early in pregnancy; the few who come to the decision later do so because something has gone seriously wrong in their lives or with their pregnancies. If states insist on drawing lines based on historical measures of viability, at 24 or 26 or 28 weeks, they should stick with those gestational limits and admit that they no longer represent actual viability but correspond instead to some form of common morality about when the fetus has a protected, if not absolute, right to life. Women need a reasonable amount of time to make careful and informed decisions about whether to continue their pregnancies precisely because these decisions have a lasting impact on their bodies and their lives. To preserve that time, legislators and the courts should decouple abortion rights from ectogenesis and other advances in the care of extremely premature infants that move the point of viability ever earlier.
[Editor's Note: This article was updated after publication to reflect Amy Coney Barrett's confirmation. To read other articles in this special magazine issue, visit the e-reader version.]
Democratize the White Coat by Honoring Black, Indigenous, and People of Color in Science
Celebrating BIPOC's achievements in science are a strong first step to make science a guiding force for all.
This article is part of the magazine, "The Future of Science In America: The Election Issue," co-published by LeapsMag, the Aspen Institute Science & Society Program, and GOOD.
Journalists, educators, and curators have responded to Black Lives Matter by highlighting the history and achievements of Black Americans in a variety of fields, including science. The movement has also sparked important demands to address longstanding scientific inequities such as lack of access to quality healthcare and the disproportionate impact of climate change and environmental pollution on neighborhoods of Black, Indigenous, and people of color (BIPOC). Making such improvements requires bringing BIPOC into science and into positions of leadership in laboratories, graduate schools, medical practices, and clinical trials. The moment is right to challenge scientific gatekeepers to respond to Black Lives Matter by widening the pathways that determine who becomes a scientist, a researcher, or a clinician.
The scientific workforce has long lacked diversity, which in turn discourages Black people from pursuing such careers. Causes include a dearth of mentors and role models, preconceived notions that science is exclusive to white males, and subpar STEM education. Across race, gender, class, ability, and all other dimensions that inform how an individual navigates the world, from the familial to the global level, seeing role models who resemble you impacts what you strive for and believe possible. As Marian Wright Edelman stated, "You can't be what you can't see"—a truth with ever-increasing resonance since the U.S. is projected to be minority-white by 2045.
Black Americans have paved the way for the nation to lead in science and technology, despite marginalization and exclusion from textbooks. Physicist Dr. Shirley Ann Jackson invented the technology behind Caller I.D. and Call Waiting. Otis Boykin's patents made televisions and radios what they are today. Thanks to the 2017 movie Hidden Figures, millions of Americans know about Katherine Johnson, the NASA mathematician whose calculations were essential to the successful trajectory of the Apollo 11 mission.
However, highlighting past role models who were Black achievers is not enough and paints too static a picture—especially when examples of transformative work by contemporary BIPOC scientists serving BIPOC communities abound. Cognitive neuroscientist Dr. Jonathan Jackson founded the Community Access, Recruitment, & Engagement (CARE) Research Center with the goal to break down barriers so that people of color participate in clinical trials. Geneticist Dr. Nanibaa' Garrison's research creates ethical frameworks to overcome genomic injustices so Indigenous populations can benefit from genetic research. Computer scientists Joy Buolamwini and Dr. Timnit Gebru's research drew attention to reinforced racial bias in artificial intelligence, leading Microsoft, Amazon, and IBM this summer to halt use of their facial recognition software.
"Integration does not mean equality if the space being integrated isn't exuberantly down for the cause."
In order to honor concretely the ubiquitous public statements and commitments to justice and equity that flooded everyone's inboxes in early June, we must include traditionally underrepresented voices in all phases of science and its applications. For guidance, we would benefit from listening to activists leading, for example, climate marches and protests over toxic water. Indeed, science is at the core of the issues for which young BIPOC are mobilizing. We need to sit down with these individuals to gain their input on how the narratives, practices, and opportunities in science should change. As Zeena Abdulkarim, a youth climate change organizer working with Zero Hour, explains: "Minority communities are exposed to what the privileged and people in power are not; therefore these communities know the right steps to take in the change we need for the kickstart of true social and environmental justice."
Two other Black youth, for example, used the platform of the laboratory while in high school to mobilize for change. Elle Lanair Lett, now specializing in epidemiology as an M.D.-Ph.D. student in Philadelphia, was prompted by family prevalence of diabetes to research the genetics of pancreatic cells. Dr. Otana Jakpor, now an ophthalmology resident in Michigan, was motivated by the pollution in her hometown of Riverside, California, to research the pulmonary effects of indoor air purifiers, with findings that influenced California ozone regulations. Both became finalists in a national science fair, propelling them on paths toward science careers. These young scientists demonstrate how people's communities and lived experiences can shape trajectories of science research, which, in turn, determines which visions for society are materialized and popularized.
We can also gain insight from another childhood science fair veteran, self-proclaimed "Black STEMinist" Augusta Uwamanzu-Nna, who graduated from college in May and works as a bioengineer. In her view, "we need to shift the burden away from Black people and onto individuals who have contributed to our current reality—fundamentally requiring understanding, open-mindedness, a lack of bias, cultural competency, anti-racism, anti-homophobia, and many, many other things."
Celebrating BIPOC's accomplishments in science and cultivating new leadership today are strong first steps to make science a guiding force for all. Ms. Uwamanzu-Nna keenly reminds us, "Integration does not mean equality if the space being integrated isn't exuberantly down for the cause." Indeed, educational institutions, scientific companies, and medical centers must acknowledge and embrace their role in democratizing science in order for society to realize racial and scientific justice.
[Editor's Note: To read other articles in this special magazine issue, visit the beautifully designed e-reader version.]

