Is Finding Out Your Baby’s Genetics A New Responsibility of Parenting?
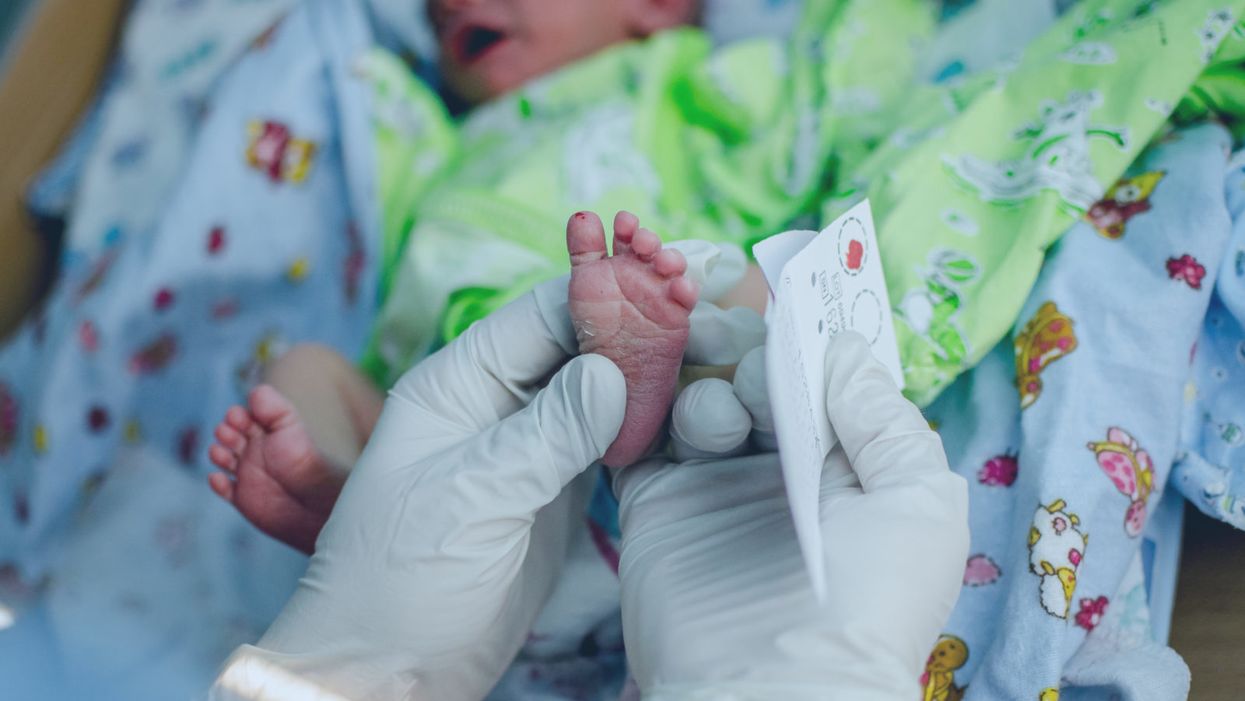
A doctor pricks the heel of a newborn for a blood test.
Hours after a baby is born, its heel is pricked with a lancet. Drops of the infant's blood are collected on a porous card, which is then mailed to a state laboratory. The dried blood spots are screened for around thirty conditions, including phenylketonuria (PKU), the metabolic disorder that kick-started this kind of newborn screening over 60 years ago. In the U.S., parents are not asked for permission to screen their child. Newborn screening programs are public health programs, and the assumption is that no good parent would refuse a screening test that could identify a serious yet treatable condition in their baby.
Learning as much as you can about your child's health might seem like a natural obligation of parenting. But it's an assumption that I think needs to be much more closely examined.
Today, with the introduction of genome sequencing into clinical medicine, some are asking whether newborn screening goes far enough. As the cost of sequencing falls, should parents take a more expansive look at their children's health, learning not just whether they have a rare but treatable childhood condition, but also whether they are at risk for untreatable conditions or for diseases that, if they occur at all, will strike only in adulthood? Should genome sequencing be a part of every newborn's care?
It's an idea that appeals to Anne Wojcicki, the founder and CEO of the direct-to-consumer genetic testing company 23andMe, who in a 2016 interview with The Guardian newspaper predicted that having newborns tested would soon be considered standard practice—"as critical as testing your cholesterol"—and a new responsibility of parenting. Wojcicki isn't the only one excited to see everyone's genes examined at birth. Francis Collins, director of the National Institutes of Health and perhaps the most prominent advocate of genomics in the United States, has written that he is "almost certain … that whole-genome sequencing will become part of new-born screening in the next few years." Whether that would happen through state-mandated screening programs, or as part of routine pediatric care—or perhaps as a direct-to-consumer service that parents purchase at birth or receive as a baby-shower gift—is not clear.
Learning as much as you can about your child's health might seem like a natural obligation of parenting. But it's an assumption that I think needs to be much more closely examined, both because the results that genome sequencing can return are more complex and more uncertain than one might expect, and because parents are not actually responsible for their child's lifelong health and well-being.
What is a parent supposed to do about such a risk except worry?
Existing newborn screening tests look for the presence of rare conditions that, if identified early in life, before the child shows any symptoms, can be effectively treated. Sequencing could identify many of these same kinds of conditions (and it might be a good tool if it could be targeted to those conditions alone), but it would also identify gene variants that confer an increased risk rather than a certainty of disease. Occasionally that increased risk will be significant. About 12 percent of women in the general population will develop breast cancer during their lives, while those who have a harmful BRCA1 or BRCA2 gene variant have around a 70 percent chance of developing the disease. But for many—perhaps most—conditions, the increased risk associated with a particular gene variant will be very small. Researchers have identified over 600 genes that appear to be associated with schizophrenia, for example, but any one of those confers only a tiny increase in risk for the disorder. What is a parent supposed to do about such a risk except worry?
Sequencing results are uncertain in other important ways as well. While we now have the ability to map the genome—to create a read-out of the pairs of genetic letters that make up a person's DNA—we are still learning what most of it means for a person's health and well-being. Researchers even have a name for gene variants they think might be associated with a disease or disorder, but for which they don't have enough evidence to be sure. They are called "variants of unknown (or uncertain) significance (VUS), and they pop up in most people's sequencing results. In cancer genetics, where much research has been done, about 1 in 5 gene variants are reclassified over time. Most are downgraded, which means that a good number of VUS are eventually designated benign.
While one parent might reasonably decide to learn about their child's risk for a condition about which nothing can be done medically, a different, yet still thoroughly reasonable, parent might prefer to remain ignorant so that they can enjoy the time before their child is afflicted.
Then there's the puzzle of what to do about results that show increased risk or even certainty for a condition that we have no idea how to prevent. Some genomics advocates argue that even if a result is not "medically actionable," it might have "personal utility" because it allows parents to plan for their child's future needs, to enroll them in research, or to connect with other families whose children carry the same genetic marker.
Finding a certain gene variant in one child might inform parents' decisions about whether to have another—and if they do, about whether to use reproductive technologies or prenatal testing to select against that variant in a future child. I have no doubt that for some parents these personal utility arguments are persuasive, but notice how far we've now strayed from the serious yet treatable conditions that motivated governments to set up newborn screening programs, and to mandate such testing for all.
Which brings me to the other problem with the call for sequencing newborn babies: the idea that even if it's not what the law requires, it's what good parents should do. That idea is very compelling when we're talking about sequencing results that show a serious threat to the child's health, especially when interventions are available to prevent or treat that condition. But as I have shown, many sequencing results are not of this type.
While one parent might reasonably decide to learn about their child's risk for a condition about which nothing can be done medically, a different, yet still thoroughly reasonable, parent might prefer to remain ignorant so that they can enjoy the time before their child is afflicted. This parent might decide that the worry—and the hypervigilence it could inspire in them—is not in their child's best interest, or indeed in their own. This parent might also think that it should be up to the child, when he or she is older, to decide whether to learn about his or her risk for adult-onset conditions, especially given that many adults at high familial risk for conditions like Alzheimer's or Huntington's disease choose never to be tested. This parent will value the child's future autonomy and right not to know more than they value the chance to prepare for a health risk that won't strike the child until 40 or 50 years in the future.
Parents are not obligated to learn about their children's risk for a condition that cannot be prevented, has a small risk of occurring, or that would appear only in adulthood.
Contemporary understandings of parenting are famously demanding. We are asked to do everything within our power to advance our children's health and well-being—to act always in our children's best interests. Against that backdrop, the need to sequence every newborn baby's genome might seem obvious. But we should be skeptical. Many sequencing results are complex and uncertain. Parents are not obligated to learn about their children's risk for a condition that cannot be prevented, has a small risk of occurring, or that would appear only in adulthood. To suggest otherwise is to stretch parental responsibilities beyond the realm of childhood and beyond factors that parents can control.
The opioid crisis depicted with a map of the USA filled with oxycodone and hydrocodone pills.
The largest ever seizure of fentanyl in the United States – 254 pounds of the white powder, enough to kill 1 in 3 Americans by overdose – was found under a shipment of cucumbers recently.
A policing approach alone is insufficient to take on the opioid crisis.
Those types of stories barely make the headlines any more, in part because illicit drugs are no longer just handsold by drug dealers; these sales have gone online. The neighborhood dealer faces the same evolving environment as other retailers and may soon go the way of Sears.
But opioids themselves are not going away. I could make an opioid purchase online in about 30 seconds and have it sent to my door, says Joe Smyser. The epidemiologist and president of The Public Good Projects isn't bragging, he's simply stating a fact about the opioid crisis that has struck the United States. The U.S Drug Enforcement Agency, social media companies, and some foreign governments have undertaken massive efforts to shut down sites selling illegal drugs, and they have gotten very good at it, shuttering most within a day of their opening.
But it's a Whac-A-Mole situation in which new ones pop up as quickly as older ones are closed; they are promoted through hashtags, social media networks, and ubiquitous email spam to lure visitors to a website or call a WhatsApp number to make a purchase. The online disruption by law enforcement has become simply another cost of doing business for drug sellers. Fentanyl, and similar analogues created to evade detection and the law, are at the center of it. Small amounts can be mixed with other "safer" opioids to get a high, and the growth of online sales have all contributed to the surge of opioid-related deaths: about 17,500 in 2006; 47,600 in 2017; and a projected 82,000 a year by 2025.
All of this has occurred even while authorities have been cracking down on the prescribing of opioids, and prescription-related deaths have declined. Clearly a policing approach alone is insufficient to take on the opioid crisis.
Building the Tools
The Public Good Projects (PGP), a nonprofit organization founded by concerned experts, was set up to better understand public health issues in this new online environment and better shape responses. The first step is to understand what people are hearing and the language they are using by monitoring social media and other forms of public communications. "We're collecting data from every publicly available media source that we can get our hands on. It's broadcast television data, it's radio, it's print newspapers and magazines. And then it's online data; it's online video, social media, blogs, websites," Smyser explains.
The purpose was to better understand the opioid crisis and find out if there were differences between affected rural and urban populations.
"Then our job is to create queries, create searches of all of that data so that we find what is the information that Americans are exposed to about a topic, and then what … Americans [are] sharing amongst themselves about that same topic."
He says it's the same thing business has been doing for years to monitor their "brand health" and be prepared for possible negative issues that might arise about their products and services. He believes PGP is the first group to use those tools for public health.
Looking At Opioids
PGP's work on opioids started with a contract from the Substance Abuse and Mental Health Administration (SAMHSA) through the National Science Foundation. The purpose was simply to better understand the opioid crisis in the United States and in particular find out if there were differences between affected rural and urban populations. A team of data scientists, public health professionals, and cultural anthropologists needed several months to sort out and organize the algorithms from the sheer volume of data.
Drug use is particularly rich in slang, where a specific drug or way of using it can be referred to in multiple ways in different towns and social groups. Traditional media often uses clinical terms, Twitter shorthand, and all of that has to be structured and integrated "so that it isn't just spitting out data that is gobbledygook and of no use to anyone," says Smyser.
The data they gather is both cumulative and in real time, tabulated and visually represented in constantly morphing hashtag and word clouds where the color and size of the word indicates the source and volume of its use.

Popular hashtags on Twitter relating to the opioid crisis.
(Credit: The Public Good Projects)
The visual presentation of data helps to understand what different groups are saying and how they are saying it. For example, compare the hashtag and word clouds. Younger people are more likely to use the hashtags of Twitter, while older people are more likely to use older forms of media, and that is reflected in their concerns and language in those clouds.

Popular words relating to the opioid crisis gathered from older forms of media.
(Credit: The Public Good Projects)
A Ping map shows the origin of messages, while a Spidey map shows the network of how messages are being forwarded and shared among people. These sets of data can be overlaid with zip code, census, and socioeconomic data to provide an even deeper sense of who is saying what. And when integrated together, they provide clues to topics and language that might best engage people in each niche.

A Ping map showing the origin of messages around the opioid crisis.
(Credit: The Public Good Projects)
Opioids Speak
One thing that quickly became apparent to PGP in monitoring the media is that "over half of the information that the American public is exposed to about opioids is a very distant policy debate," says Smyser.
It is political pronouncements in DC, the legal system going after pharmaceutical companies that promoted prescription opioids for pain relief (and more), or mandatory prison terms for offenders. Relatively little is about treatment, the impact on families and communities, and what people can do themselves. That is particularly important in light of another key finding: residents of "Trump-land," the rural areas that supported the president and are being ravaged by opioids, talk about the problem and solutions very differently from urban areas.
"In rural communities there is usually a huge emphasis on self-reliance, and we take care of each other; that's why we enjoy living here. We are a neighborhood, we come together and we fix our own problems," according to Smyser.
In contrast, urban communities tend to be more transient, less likely to live in multigenerational households and neighborhoods, and look to formal institutions rather than themselves for solutions. "The message that we're sending people is one where there is really no role whatsoever for self-efficacy...we're giving them nothing to do" to help solve the problem themselves, says Smyser. "In fact, I could argue it is reducing self-efficacy."
Residents of "Trump-land," the rural areas that supported the president and are being ravaged by opioids, talk about the problem and solutions very differently from urban areas.
The opioid crisis is complex and improving the situation will be too. Smyser believes a top-down policing approach alone will not work; it is better to provide front-line public health officers at the state and local level with more and current intelligence so they can respond in their communities.
"I think that would be enormously impactful. But right now, we just don't have that service." SAMHSA declined multiple requests to discuss this project paid for with federal money. A spokesman concluded with: "That project occurred under the previous administration, and we did not have a direct relationship with PGP. As a result, I am unable to comment on the project."
The Milken Institute Center for Public Health, a think tank that is working to find solutions to the opioid epidemic, had an upbeat response. Director Sabrina Spitaletta said, "PGP's work to provide real-time data that monitors topics of high concern in public health has been very helpful to many of the front-line organizations working to combat this crisis."
Bad Actors Getting Your Health Data Is the FBI’s Latest Worry
A hacker activating a 3D rendering of DNA data.
In February 2015, the health insurer Anthem revealed that criminal hackers had gained access to the company's servers, exposing the personal information of nearly 79 million patients. It's the largest known healthcare breach in history.
FBI agents worry that the vast amounts of healthcare data being generated for precision medicine efforts could leave the U.S. vulnerable to cyber and biological attacks.
That year, the data of millions more would be compromised in one cyberattack after another on American insurers and other healthcare organizations. In fact, for the past several years, the number of reported data breaches has increased each year, from 199 in 2010 to 344 in 2017, according to a September 2018 analysis in the Journal of the American Medical Association.
The FBI's Edward You sees this as a worrying trend. He says hackers aren't just interested in your social security or credit card number. They're increasingly interested in stealing your medical information. Hackers can currently use this information to make fake identities, file fraudulent insurance claims, and order and sell expensive drugs and medical equipment. But beyond that, a new kind of cybersecurity threat is around the corner.
Mr. You and others worry that the vast amounts of healthcare data being generated for precision medicine efforts could leave the U.S. vulnerable to cyber and biological attacks. In the wrong hands, this data could be used to exploit or extort an individual, discriminate against certain groups of people, make targeted bioweapons, or give another country an economic advantage.
Precision medicine, of course, is the idea that medical treatments can be tailored to individuals based on their genetics, environment, lifestyle or other traits. But to do that requires collecting and analyzing huge quantities of health data from diverse populations. One research effort, called All of Us, launched by the U.S. National Institutes of Health last year, aims to collect genomic and other healthcare data from one million participants with the goal of advancing personalized medical care.
Other initiatives are underway by academic institutions and healthcare organizations. Electronic medical records, genetic tests, wearable health trackers, mobile apps, and social media are all sources of valuable healthcare data that a bad actor could potentially use to learn more about an individual or group of people.
"When you aggregate all of that data together, that becomes a very powerful profile of who you are," Mr. You says.
A supervisory special agent in the biological countermeasures unit within the FBI's weapons of mass destruction directorate, it's Mr. You's job to imagine worst-case bioterror scenarios and figure out how to prevent and prepare for them.
That used to mean focusing on threats like anthrax, Ebola, and smallpox—pathogens that could be used to intentionally infect people—"basically the dangerous bugs," as he puts it. In recent years, advances in gene editing and synthetic biology have given rise to fears that rogue, or even well-intentioned, scientists could create a virulent virus that's intentionally, or unintentionally, released outside the lab.
"If a foreign source, especially a criminal one, has your biological information, then they might have some particular insights into what your future medical needs might be and exploit that."
While Mr. You is still tracking those threats, he's been traveling around the country talking to scientists, lawyers, software engineers, cyber security professionals, government officials and CEOs about new security threats—those posed by genetic and other biological data.
Emerging threats
Mr. You says one possible situation he can imagine is the potential for nefarious actors to use an individual's sensitive medical information to extort or blackmail that person.
"If a foreign source, especially a criminal one, has your biological information, then they might have some particular insights into what your future medical needs might be and exploit that," he says. For instance, "what happens if you have a singular medical condition and an outside entity says they have a treatment for your condition?" You could get talked into paying a huge sum of money for a treatment that ends up being bogus.
Or what if hackers got a hold of a politician or high-profile CEO's health records? Say that person had a disease-causing genetic mutation that could affect their ability to carry out their job in the future and hackers threatened to expose that information. These scenarios may seem far-fetched, but Mr. You thinks they're becoming increasingly plausible.
On a wider scale, Kavita Berger, a scientist at Gryphon Scientific, a Washington, D.C.-area life sciences consulting firm, worries that data from different populations could be used to discriminate against certain groups of people, like minorities and immigrants.
For instance, the advocacy group Human Rights Watch in 2017 flagged a concerning trend in China's Xinjiang territory, a region with a history of government repression. Police there had purchased 12 DNA sequencers and were collecting and cataloging DNA samples from people to build a national database.
"The concern is that this particular province has a huge population of the Muslim minority in China," Ms. Berger says. "Now they have a really huge database of genetic sequences. You have to ask, why does a police station need 12 next-generation sequencers?"
Also alarming is the potential that large amounts of data from different groups of people could lead to customized bioweapons if that data ends up in the wrong hands.
Eleonore Pauwels, a research fellow on emerging cybertechnologies at United Nations University's Centre for Policy Research, says new insights gained from genomic and other data will give scientists a better understanding of how diseases occur and why certain people are more susceptible to certain diseases.
"As you get more and more knowledge about the genomic picture and how the microbiome and the immune system of different populations function, you could get a much deeper understanding about how you could target different populations for treatment but also how you could eventually target them with different forms of bioagents," Ms. Pauwels says.
Economic competitiveness
Another reason hackers might want to gain access to large genomic and other healthcare datasets is to give their country a leg up economically. Many large cyber-attacks on U.S. healthcare organizations have been tied to Chinese hacking groups.
"This is a biological space race and we just haven't woken up to the fact that we're in this race."
"It's becoming clear that China is increasingly interested in getting access to massive data sets that come from different countries," Ms. Pauwels says.
A year after U.S. President Barack Obama conceived of the Precision Medicine Initiative in 2015—later renamed All of Us—China followed suit, announcing the launch of a 15-year, $9 billion precision health effort aimed at turning China into a global leader in genomics.
Chinese genomics companies, too, are expanding their reach outside of Asia. One company, WuXi NextCODE, which has offices in Shanghai, Reykjavik, and Cambridge, Massachusetts, has built an extensive library of genomes from the U.S., China and Iceland, and is now setting its sights on Ireland.
Another Chinese company, BGI, has partnered with Children's Hospital of Philadelphia and Sinai Health System in Toronto, and also formed a collaboration with the Smithsonian Institute to sequence all species on the planet. BGI has built its own advanced genomic sequencing machines to compete with U.S.-based Illumina.
Mr. You says having access to all this data could lead to major breakthroughs in healthcare, such as new blockbuster drugs. "Whoever has the largest, most diverse dataset is truly going to win the day and come up with something very profitable," he says.
Some direct-to-consumer genetic testing companies with offices in the U.S., like Dante Labs, also use BGI to process customers' DNA.
Experts worry that China could race ahead the U.S. in precision medicine because of Chinese laws governing data sharing. Currently, China prohibits the exportation of genetic data without explicit permission from the government. Mr. You says this creates an asymmetry in data sharing between the U.S. and China.
"This is a biological space race and we just haven't woken up to the fact that we're in this race," he said in January at an American Society for Microbiology conference in Washington, D.C. "We don't have access to their data. There is absolutely no reciprocity."
Protecting your data
While Mr. You has been stressing the importance of data security to anyone who will listen, the National Academies of Sciences, Engineering, and Medicine, which makes scientific and policy recommendations on issues of national importance, has commissioned a study on "safeguarding the bioeconomy."
In the meantime, Ms. Berger says organizations that deal with people's health data should assess their security risks and identify potential vulnerabilities in their systems.
As for what individuals can do to protect themselves, she urges people to think about the different ways they're sharing healthcare data—such as via mobile health apps and wearables.
"Ask yourself, what's the benefit of sharing this? What are the potential consequences of sharing this?" she says.
Mr. You also cautions people to think twice before taking consumer DNA tests. They may seem harmless, he says, but at the end of the day, most people don't know where their genetic information is going. "If your genetic sequence is taken, once it's gone, it's gone. There's nothing you can do about it."

