How Seriously Should We Take the Promising News on Long COVID?

Jessica Lovett, who suffers from long Covid, feels a renewed sense of energy and hope since getting vaccinated.
One of the biggest challenges of the COVID-19 pandemic is the way in which it has forced us to question our hopes. In normal times, hope is a tonic we take in small doses to keep us moving forward through the slog of daily life. The pandemic, however, has made it a much scarcer commodity, spurring us not only to seek it more desperately but to scrutinize it more closely.
Every bit of reassurance seems to come with caveats: Masks can shield us from the coronavirus, but they may need to be doubled in some situations to provide adequate protection. Vaccines work, but they may not be as effective against some viral variants—and they can cause extremely rare but serious side effects. Every few weeks, another potential miracle cure makes headlines (Hydroxychloroquine! Convalescent plasma!), only to prove disappointing on closer inspection. It's hard to know which alleged breakthroughs are worth pinning our hopes on, and which are the products of wishful thinking or hucksterism.
In January 2021, a study published in the journal Gut offered evidence that bacteria in the intestines might influence a whole spectrum of symptoms in long-haul patients.
Lately, two possible sources of hope have emerged concerning so-called "long COVID"—the debilitating syndrome, estimated to affect up to one-third of patients, in which physical, neurological, and cognitive symptoms persist for months. The first encouraging item has gotten plenty of media attention: reports that some long-haulers feel better after being vaccinated. The second item, while less widely covered, has caused a stir among scientists: a study suggesting that rebalancing the gut microbiome—the community of microorganisms in our intestines—could decrease both the severity and duration of the illness.
How optimistic should we allow ourselves to be about either of these developments? Experts warn that it's too soon to tell. Yet research into how vaccines and gut bacteria affect long-haulers—and how both factors might work together—could eventually help solve key pieces of the pandemic puzzle.
Investigating the Role of the Gut Microbiome
The idea that there may be a link between COVID-19 and gut health comes as no surprise to Jessica Lovett. Her case began in June 2020 with gastrointestinal distress—a symptom that was just beginning to be recognized as commonplace in what had initially been considered a respiratory illness. "I had diarrhea three to five times a day for two months," Lovett recalls. "I lost a lot of weight." By July, she was also suffering shortness of breath, chest pain, racing heartbeat, severe fatigue, brain fog, migraines, memory lapses, and more. As with many other COVID long-haulers, these troubles waxed and waned in an endless parade.
Lovett was the marketing manager for a music school in Austin, Texas, and the mother of a two-year-old boy. Just before she got sick, she ran a 5K race for her 40th birthday. Afterward, she had to give up her job, stop driving, and delegate childcare to her husband (who fell ill shortly before she did but recovered in 12 days). Tests showed no visible damage to her lungs, heart, or other organs. But she felt intuitively that taming her GI troubles would be key to getting well. On the advice of fellow patients in a long-COVID Facebook group—and, later, with the guidance of a doctor—she tried avoiding foods thought to trigger histamine reactions or inflammation. That seemed to help some, as did nutritional supplements, antihistamines, and angina medications. Still, she relapsed frequently, and was often bedridden.
In January 2021, a study published in the journal Gut offered evidence that bacteria in the intestines might influence a whole spectrum of symptoms in patients like Lovett. Researchers at the Chinese University of Hong Kong examined blood and stool samples and medical records from 100 hospital patients with lab-confirmed COVID-19 infections, and from 78 people without the disease who were taking part in a microbiome study before the pandemic.
The team, led by professor Siew Chien Ng, found that the makeup of the gut microbiome differed sharply between the two groups. Patients with COVID had higher levels of three bacterial species than those without the infection, but lower levels of several species known to enhance immune system response. Reductions in two of those species—Faecalibacterium prausnitzii and Bifidobacterium bifidum—were associated with more severe symptoms. And the numbers of such helpful bacteria remained low in stool samples collected up to 30 days after infected patients had seemingly cleared the coronavirus from their bodies.
Analysis of blood samples, moreover, showed that these bacterial imbalances correlated with higher levels of inflammatory cytokines (immune system chemicals that are elevated in many patients with severe COVID-19) and markers of tissue damage, such as C-reactive protein.
These findings led the researchers to suggest that rebalancing the microbiome might lessen not only the intensity of COVID symptoms, but also their persistence. "Bolstering of beneficial gut species depleted in COVID-19," they wrote, "could serve as a novel avenue to mitigate severe disease, underscoring the importance of managing patients' gut biota during and after COVID-19."
Soon afterward, Ng revealed that she was working on a solution. Her team, she told Medscape, had developed "a microbiome immunity product that is targeted to what is missing in COVID-19 patients." Early research showed that hospitalized patients who received the treatment developed more antibodies, had fewer symptoms, and were discharged sooner. "So it is quite a bright and promising future," she enthused, "in alleviating some of these detrimental effects of the virus."
The Chicken-and-Egg Problem
Ng's study isn't the only one to suggest a connection between the gut and long COVID. Researchers led by gastroenterologist Saurabh Mehandru at New York's Mount Sinai Hospital recently determined that SARS-CoV-2, the virus that causes COVID-19, can linger in the intestines for months after a patient tests negative. Some studies have also found that gastrointestinal symptoms in the acute phase of the illness correlate with poorer outcomes—though that's far from settled. (In another study, Mehandru's team found lower mortality among patients presenting with GI symptoms.) But the Hong Kong group's paper was the first to posit that resident microbes may play a decisive role in the disease.
That view reflects growing evidence that these bugs can influence a range of ailments, from diabetes to schizophrenia. Over the past decade, the gut microbiome has emerged as a central regulator of the immune system. Some intestinal bacteria emit chemicals that signal immune cells to reduce production of inflammatory proteins, or help those cells effectively target invading pathogens. They also help maintain the integrity of the intestinal lining—preventing the syndrome known as "leaky gut," in which harmful microbes or toxins penetrate to the underlying tissue, potentially wreaking havoc throughout the body and brain.
Nonetheless, many experts have responded to Ng's findings with distinct caution. One problem, they point out, is the chicken-and-egg question: Do reduced levels of beneficial gut bacteria trigger the inflammation seen in COVID-19, or does inflammation triggered by COVID-19 kill off beneficial gut bacteria? "It's an issue of causality versus just association," explains Somsouk Ma, a professor of gastroenterology at the University of California, San Francisco. "I tend to think that the shift in microbes is more likely a consequence of the infection. But, of course, that's just speculation."
A related issue is whether a pill that replenishes "good" bacteria can really combat the effects of COVID-19—whether acute or chronic. Although scientists are studying fecal transplants and other probiotic therapies for many disorders, none has yet been approved by the U.S Food and Drug Administration. "The only situation where bacterial transplantation is known to work is in a form of colitis called Clostridium difficile," notes Mehandru. "I think it's a bit premature to lay too much emphasis on this in the context of COVID."
Placebo-controlled clinical trials will be needed to determine the efficacy of Ng's approach. (Consumer warning: The bacteria she's employing are not found in commercially available probiotics.) Whatever the results, such research—along with studies that track patients' gut microbiomes before, during, and after COVID-19 infection—could help scientists understand why some people have such trouble kicking the disease.
An Unexpected Benefit of Vaccines
The question of what causes long COVID is also central to understanding the effects of vaccines on the condition. In March, as inoculation campaigns took off across the nation, many long-haulers were delighted to see their symptoms disappear within days of getting the shot. "I woke up and it was like, 'Oh what a beautiful morning,'" one patient told The New York Times.
Yet the effects have been far from uniform. Although scientific surveys have not yet been conducted, an April poll by a Facebook group called Survivor Corps found numbers close to experts' estimates: 39 percent said they experienced partial to full recovery post-vaccination; 46 percent saw no difference; and 14 percent felt worse.
How could vaccines—which are designed to prevent COVID-19, not cure it—help some chronic patients get well? In a blog post, Yale immunologist Akiko Iwasaki suggested that the answer depends on what is driving a particular patient's symptoms. Iwasaki identified three possible mechanisms behind long COVID: 1) a persistent viral reservoir; 2) a "viral ghost," composed of fragments of the virus (RNA or proteins) that linger after the infection has been cleared but can still stimulate inflammation; and 3) an autoimmune response triggered by the infection, inducing a patient's immune cells to attack her own tissues.
These mechanisms "are not mutually exclusive," Iwasaki wrote, "and all three might benefit from the vaccines." If a patient has a viral reservoir, vaccine-induced immune cells and antibodies might be able to eliminate it. If the patient has a viral ghost, those vaccine-primed immune responses might knock it out as well. And if the patient is suffering from a COVID-triggered autoimmune syndrome, the vaccine might act as a decoy, shifting the immune system's attention to antigens contained in the shot (and perhaps reprogramming autoimmune cells in the process). The varying role of these underlying factors, and possibly others—such as the gut microbiome—might also help explain why vaccines don't benefit all long-haulers equally. Iwasaki and her team recently launched a clinical study to investigate this theory.
Pato Hebert, a professor of art and public policy at NYU, contracted COVID-19 in March 2020 while on sabbatical in Los Angeles. Hebert, then 50, started out with mild flu-like symptoms, but he was slammed with fatigue, headaches, and confusion a week after testing positive. In April, he landed in urgent care with severe shortness of breath. His brain fog worsened that summer, and a gentle swim brought on a dizzy spell so overwhelming that he feared it was a stroke. (Thankfully, tests showed it wasn't.) In September, he developed severe GI issues, which came and went over the following months. He found some relief through medications, dietary adjustments, acupuncture, herbal remedies, and careful conservation of his physical and mental energy—but a year after his diagnosis, he was still sick.
Hebert received his first dose of the Moderna vaccine on March 1, 2021; it made no difference in his symptoms. After his second dose, on the 29th, he suffered terrible headaches—"like early COVID days," he told me. A week later, his condition had improved slightly compared to pre-vaccination. "With a few exceptions, my fatigue and brain fog have been less challenging," he reported. "I'm cautiously optimistic." But in late April, he suffered another flareup of respiratory and GI issues.
For Jessica Lovett, the vaccine's effects were more dramatic. After her first dose of the Pfizer-BioNTech formula, on February 26, her cognitive symptoms improved enough that she was able to drive again; within a week, she was pushing her son uphill in a stroller, lifting light weights, and running for short distances. After the second dose, she says, "I had incredible energy. It was insane, like I drank three cups of coffee."
Lovett (who now runs a Facebook support group for Austin locals, ATX Covid Long Haulers) stresses that the vaccine hasn't cured her. She winds up back in bed whenever she pushes herself too hard. She still needs to take antihistamines and shun certain foodstuffs; any slip-up brings another relapse. Yet she's able to live more fully than at any time since she fell ill—and she has begun to feel a renewed sense of hope.
Recently, in fact, she and her husband decided to expand their family. "I guess that tells you something," she says with a laugh. "The doctors have given us the okay, and we're going to try."
Jamie Rettinger with his now fiance Amie Purnel-Davis, who helped him through the clinical trial.
Jamie Rettinger was still in his thirties when he first noticed a tiny streak of brown running through the thumbnail of his right hand. It slowly grew wider and the skin underneath began to deteriorate before he went to a local dermatologist in 2013. The doctor thought it was a wart and tried scooping it out, treating the affected area for three years before finally removing the nail bed and sending it off to a pathology lab for analysis.
"I have some bad news for you; what we removed was a five-millimeter melanoma, a cancerous tumor that often spreads," Jamie recalls being told on his return visit. "I'd never heard of cancer coming through a thumbnail," he says. None of his doctors had ever mentioned it either. "I just thought I was being treated for a wart." But nothing was healing and it continued to bleed.
A few months later a surgeon amputated the top half of his thumb. Lymph node biopsy tested negative for spread of the cancer and when the bandages finally came off, Jamie thought his medical issues were resolved.
Melanoma is the deadliest form of skin cancer. About 85,000 people are diagnosed with it each year in the U.S. and more than 8,000 die of the cancer when it spreads to other parts of the body, according to the Centers for Disease Control and Prevention (CDC).
There are two peaks in diagnosis of melanoma; one is in younger women ages 30-40 and often is tied to past use of tanning beds; the second is older men 60+ and is related to outdoor activity from farming to sports. Light-skinned people have a twenty-times greater risk of melanoma than do people with dark skin.
"When I graduated from medical school, in 2005, melanoma was a death sentence" --Diwakar Davar.
Jamie had a follow up PET scan about six months after his surgery. A suspicious spot on his lung led to a biopsy that came back positive for melanoma. The cancer had spread. Treatment with a monoclonal antibody (nivolumab/Opdivo®) didn't prove effective and he was referred to the UPMC Hillman Cancer Center in Pittsburgh, a four-hour drive from his home in western Ohio.
An alternative monoclonal antibody treatment brought on such bad side effects, diarrhea as often as 15 times a day, that it took more than a week of hospitalization to stabilize his condition. The only options left were experimental approaches in clinical trials.
Early research
"When I graduated from medical school, in 2005, melanoma was a death sentence" with a cure rate in the single digits, says Diwakar Davar, 39, an oncologist at UPMC Hillman Cancer Center who specializes in skin cancer. That began to change in 2010 with introduction of the first immunotherapies, monoclonal antibodies, to treat cancer. The antibodies attach to PD-1, a receptor on the surface of T cells of the immune system and on cancer cells. Antibody treatment boosted the melanoma cure rate to about 30 percent. The search was on to understand why some people responded to these drugs and others did not.
At the same time, there was a growing understanding of the role that bacteria in the gut, the gut microbiome, plays in helping to train and maintain the function of the body's various immune cells. Perhaps the bacteria also plays a role in shaping the immune response to cancer therapy.
One clue came from genetically identical mice. Animals ordered from different suppliers sometimes responded differently to the experiments being performed. That difference was traced to different compositions of their gut microbiome; transferring the microbiome from one animal to another in a process known as fecal transplant (FMT) could change their responses to disease or treatment.
When researchers looked at humans, they found that the patients who responded well to immunotherapies had a gut microbiome that looked like healthy normal folks, but patients who didn't respond had missing or reduced strains of bacteria.
Davar and his team knew that FMT had a very successful cure rate in treating the gut dysbiosis of Clostridioides difficile, a persistant intestinal infection, and they wondered if a fecal transplant from a patient who had responded well to cancer immunotherapy treatment might improve the cure rate of patients who did not originally respond to immunotherapies for melanoma.
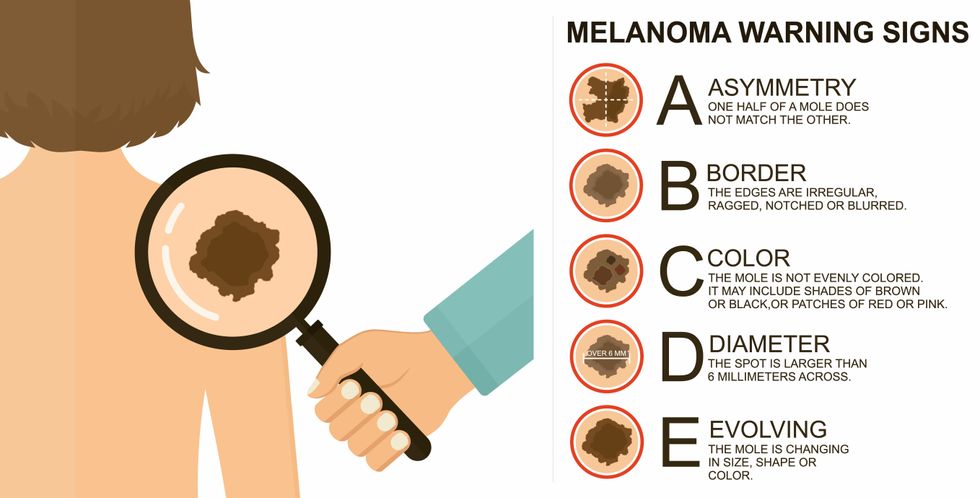
The ABCDE of melanoma detection
Adobe Stock
Clinical trial
"It was pretty weird, I was totally blasted away. Who had thought of this?" Jamie first thought when the hypothesis was explained to him. But Davar's explanation that the procedure might restore some of the beneficial bacterial his gut was lacking, convinced him to try. He quickly signed on in October 2018 to be the first person in the clinical trial.
Fecal donations go through the same safety procedures of screening for and inactivating diseases that are used in processing blood donations to make them safe for transfusion. The procedure itself uses a standard hollow colonoscope designed to screen for colon cancer and remove polyps. The transplant is inserted through the center of the flexible tube.
Most patients are sedated for procedures that use a colonoscope but Jamie doesn't respond to those drugs: "You can't knock me out. I was watching them on the TV going up my own butt. It was kind of unreal at that point," he says. "There were about twelve people in there watching because no one had seen this done before."
A test two weeks after the procedure showed that the FMT had engrafted and the once-missing bacteria were thriving in his gut. More importantly, his body was responding to another monoclonal antibody (pembrolizumab/Keytruda®) and signs of melanoma began to shrink. Every three months he made the four-hour drive from home to Pittsburgh for six rounds of treatment with the antibody drug.
"We were very, very lucky that the first patient had a great response," says Davar. "It allowed us to believe that even though we failed with the next six, we were on the right track. We just needed to tweak the [fecal] cocktail a little better" and enroll patients in the study who had less aggressive tumor growth and were likely to live long enough to complete the extensive rounds of therapy. Six of 15 patients responded positively in the pilot clinical trial that was published in the journal Science.
Davar believes they are beginning to understand the biological mechanisms of why some patients initially do not respond to immunotherapy but later can with a FMT. It is tied to the background level of inflammation produced by the interaction between the microbiome and the immune system. That paper is not yet published.
Surviving cancer
It has been almost a year since the last in his series of cancer treatments and Jamie has no measurable disease. He is cautiously optimistic that his cancer is not simply in remission but is gone for good. "I'm still scared every time I get my scans, because you don't know whether it is going to come back or not. And to realize that it is something that is totally out of my control."
"It was hard for me to regain trust" after being misdiagnosed and mistreated by several doctors he says. But his experience at Hillman helped to restore that trust "because they were interested in me, not just fixing the problem."
He is grateful for the support provided by family and friends over the last eight years. After a pause and a sigh, the ruggedly built 47-year-old says, "If everyone else was dead in my family, I probably wouldn't have been able to do it."
"I never hesitated to ask a question and I never hesitated to get a second opinion." But Jamie acknowledges the experience has made him more aware of the need for regular preventive medical care and a primary care physician. That person might have caught his melanoma at an earlier stage when it was easier to treat.
Davar continues to work on clinical studies to optimize this treatment approach. Perhaps down the road, screening the microbiome will be standard for melanoma and other cancers prior to using immunotherapies, and the FMT will be as simple as swallowing a handful of freeze-dried capsules off the shelf rather than through a colonoscopy. Earlier this year, the Food and Drug Administration approved the first oral fecal microbiota product for C. difficile, hopefully paving the way for more.
An older version of this hit article was first published on May 18, 2021
All organisms can repair damaged tissue, but none do it better than salamanders and newts. A surprising area of science could tell us how they manage this feat - and perhaps even help us develop a similar ability.
All organisms have the capacity to repair or regenerate tissue damage. None can do it better than salamanders or newts, which can regenerate an entire severed limb.
That feat has amazed and delighted man from the dawn of time and led to endless attempts to understand how it happens – and whether we can control it for our own purposes. An exciting new clue toward that understanding has come from a surprising source: research on the decline of cells, called cellular senescence.
Senescence is the last stage in the life of a cell. Whereas some cells simply break up or wither and die off, others transition into a zombie-like state where they can no longer divide. In this liminal phase, the cell still pumps out many different molecules that can affect its neighbors and cause low grade inflammation. Senescence is associated with many of the declining biological functions that characterize aging, such as inflammation and genomic instability.
Oddly enough, newts are one of the few species that do not accumulate senescent cells as they age, according to research over several years by Maximina Yun. A research group leader at the Center for Regenerative Therapies Dresden and the Max Planck Institute of Molecular and Cell Biology and Genetics, in Dresden, Germany, Yun discovered that senescent cells were induced at some stages of regeneration of the salamander limb, “and then, as the regeneration progresses, they disappeared, they were eliminated by the immune system,” she says. “They were present at particular times and then they disappeared.”
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states.
Previous research on senescence in aging had suggested, logically enough, that applying those cells to the stump of a newly severed salamander limb would slow or even stop its regeneration. But Yun stood that idea on its head. She theorized that senescent cells might also play a role in newt limb regeneration, and she tested it by both adding and removing senescent cells from her animals. It turned out she was right, as the newt limbs grew back faster than normal when more senescent cells were included.
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states, which could then be turned into progenitors, a cell type in between stem cells and specialized cells, needed to regrow the muscle tissue of the missing limb. “We think that this ability to dedifferentiate is intrinsically a big part of why salamanders can regenerate all these very complex structures, which other organisms cannot,” she explains.
Yun sees regeneration as a two part problem. First, the cells must be able to sense that their neighbors from the lost limb are not there anymore. Second, they need to be able to produce the intermediary progenitors for regeneration, , to form what is missing. “Molecularly, that must be encoded like a 3D map,” she says, otherwise the new tissue might grow back as a blob, or liver, or fin instead of a limb.
Wound healing
Another recent study, this time at the Mayo Clinic, provides evidence supporting the role of senescent cells in regeneration. Looking closely at molecules that send information between cells in the wound of a mouse, the researchers found that senescent cells appeared near the start of the healing process and then disappeared as healing progressed. In contrast, persistent senescent cells were the hallmark of a chronic wound that did not heal properly. The function and significance of senescence cells depended on both the timing and the context of their environment.
The paper suggests that senescent cells are not all the same. That has become clearer as researchers have been able to identify protein markers on the surface of some senescent cells. The patterns of these proteins differ for some senescent cells compared to others. In biology, such physical differences suggest functional differences, so it is becoming increasingly likely there are subsets of senescent cells with differing functions that have not yet been identified.
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes.
Scientists initially thought that senescent cells couldn’t play a role in regeneration because they could no longer reproduce, says Anthony Atala, a practicing surgeon and bioengineer who leads the Wake Forest Institute for Regenerative Medicine in North Carolina. But Yun’s study points in the other direction. “What this paper shows clearly is that these cells have the potential to be involved in tissue regeneration [in newts]. The question becomes, will these cells be able to do the same in humans.”
As our knowledge of senescent cells increases, Atala thinks we need to embrace a new analogy to help understand them: humans in retirement. They “have acquired a lot of wisdom throughout their whole life and they can help younger people and mentor them to grow to their full potential. We're seeing the same thing with these cells,” he says. They are no longer putting energy into their own reproduction, but the signaling molecules they secrete “can help other cells around them to regenerate.”
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes. If so, it seems that our genes are unable to express this ability, perhaps as part of a tradeoff in acquiring other traits. It is a fertile area of research.
Dedifferentiation is likely to become an important process in the field of regenerative medicine. One extreme example: a lab has been able to turn back the clock and reprogram adult male skin cells into female eggs, a potential milestone in reproductive health. It will be more difficult to control just how far back one wishes to go in the cell's dedifferentiation – part way or all the way back into a stem cell – and then direct it down a different developmental pathway. Yun is optimistic we can learn these tricks from newts.
Senolytics
A growing field of research is using drugs called senolytics to remove senescent cells and slow or even reverse disease of aging.
“Senolytics are great, but senolytics target different types of senescence,” Yun says. “If senescent cells have positive effects in the context of regeneration, of wound healing, then maybe at the beginning of the regeneration process, you may not want to take them out for a little while.”
“If you look at pretty much all biological systems, too little or too much of something can be bad, you have to be in that central zone” and at the proper time, says Atala. “That's true for proteins, sugars, and the drugs that you take. I think the same thing is true for these cells. Why would they be different?”
Our growing understanding that senescence is not a single thing but a variety of things likely means that effective senolytic drugs will not resemble a single sledge hammer but more a carefully manipulated scalpel where some types of senescent cells are removed while others are added. Combinations and timing could be crucial, meaning the difference between regenerating healthy tissue, a scar, or worse.

