New Podcast: "Making Sense of Science"
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.

Making Sense of Science features interviews with leading medical and scientific experts about the latest developments and the big ethical and societal questions they raise. This monthly podcast is hosted by journalist Kira Peikoff, founding editor of the award-winning science outlet Leaps.org.
Episode 1: "COVID-19 Vaccines and Our Progress Toward Normalcy"
Bioethicist Arthur Caplan of NYU shares his thoughts on when we will build herd immunity, how enthusiastic to be about the J&J vaccine, predictions for vaccine mandates in the coming months, what should happen with kids and schools, whether you can hug your grandparents after they get vaccinated, and more.
Transcript:
KIRA: Hi, and welcome to our new podcast 'Making Sense of Science', the show that features interviews with leading experts in health and science about the latest developments and the big ethical questions. I'm your host Kira Peikoff, the editor of leaps.org. And today, we're going to talk about the Covid-19 vaccines. I'm honored that my first guest is Dr. Art Caplan of NYU, one of the world's leading bio-ethicists. Art, thanks so much for joining us today.
DR. CAPLAN: Thank you so much for having me.
KIRA: So the big topic right now is the new J&J vaccine, which is likely to be given to millions of Americans in the coming weeks. It only requires one-shot, it can be stored in refrigerators for several months. It has fewer side-effects and most importantly, it is extremely effective at the big things, preventing hospitalizations and deaths. Though not as effective as Pfizer and Moderna in preventing moderate cases, especially potentially in older adults with underlying conditions. So Art, what's your take overall, on how enthusiastic Americans should be about this vaccine?
DR. CAPLAN: I'm usually enthusiastic. The more weapons, the better. This vaccine, while maybe, slightly less efficacious than the Moderna and the Pfizer ones, is easier to make, is easier to ship. It's one-shot. You know, here there's already been problems of getting people to come back in for their second shots. I would say 5... 7% of people don't show up even though you remind them and you nag them, they don't come back. So a one-shot option is great. A one-shot option that's easy to, if you will, brew up in your rural pharmacy without having to have special instructions is great. And I think it's gonna really facilitate herd-immunity, meaning, we'll see millions and millions and millions of doses of the Janssen vaccine out there as an option, I'm gonna say, summer.
KIRA: Great. And to be fair, it's worth mentioning that the J&J vaccine was tested in clinical trials after variants began to circulate, and it's only one-shot instead of two, like the other vaccines, and it gets more effective over time. So is it really fair to directly compare its efficacy to the mRNA vaccines?
DR. CAPLAN: Well, you know, people are gonna do that. And one issue that'll come up ethically is people are gonna say, "Can I choose my vaccine? I want the most efficacious one. I want the name brand that I trust. I don't want the new platform. I like Janssen's 'cause it's an older, more established way to make vaccines or whatever." Who knows what cuckoo-cockamamie reasons they might have. To me, you take what you can get, it'll be great. It's way above what we normally would expect, those 95% success rates are off the charts. Getting something that's 70% effective, it's perfectly wonderful. I wish we had flu shots that were 70% effective.
And the other thing to keep in mind is we're gonna see more mutations, we're gonna see more strains. That's just a reality of viruses. So they'll mutate, more strains will appear, we can't just say, "Oh my goodness. There's a South-African one or the California one or the UK one. We better... I don't know, do something different." We're just gonna have to basically resign ourselves, I think, to boosters. So right now, take the vaccine. I'm almost tempted to say, "Shut up and take the vaccine. Don't worry about choosing."
Just get what you can get. If you live in a rural community and all they have is Janssen, take it. If you're in another country and all they ship to you is Janssen, take it. And then we'll worry about the next round of virus mutations, if you will, when we get to the boosters. I'm more concerned that these things aren't gonna last more than a year or two than I am that they're not gonna pick up every mutation.
KIRA: So on that note, shipping to rural places or low-income countries that lack the ultra-cold freezers that you need for the super effective mRNA vaccines, the Janssen vaccine seems like a really great option, but are we going to encounter a potential conflict of people saying, "Well, there's "poor or rich vaccines," and one is slightly less effective than the other." And so are we gonna disenfranchise people and undermine their actual willingness to take the vaccine?
DR. CAPLAN: Well, it's interesting. I think the first problem is gonna be, "I have vaccine and I don't have any vaccine," between rich and poor countries. Look, the poor countries are screaming to get vaccine supply sent to them. I think, for example, Ghana received recently 600 million doses of AstraZeneca vaccine. It was freed up by South Africa, which decided they didn't wanna use it 'cause they thought there was "a better vaccine" coming. So even among the poorer nations or the developing nations, some vaccines are getting typed as the not-as-good or the less-desirable... We've already started to see it.
But for the most part, the rich countries are gonna try and vaccinate to herd immunity, you can argue about the ethics of whether that's right, before they start sharing. And I think we'll have haves and have-nots, herd immunity produced in the rich countries, Japan, North America, Europe, by the end of the year anyway. And still some countries floundering around saying, "I didn't get anything," and what are you gonna do?
KIRA: And I know you said to people, which is a very memorable quote, "just shut up and take the vaccine, whatever you can get, whatever is available to you now, do it." But inevitably, as you mentioned, some people are going to say, "Well, I just wanna wait to get the best one possible." When will people have a choice in vaccines, do you think?
DR. CAPLAN: I don't think you'll see that till next year. I think we're gonna see distribution according to where the supply chains are that the vaccine manufacturers use. So if I use McKesson and they ship to the Northeast, and that's where my vaccine goes, that's what's available there. If I'm contracted to Walmart and they buy Janssen, that's what you're gonna see at the big box store. I don't think you're really gonna get too much in the way of choice until next year, when then they're gonna say they ship three different kinds of vaccine, and I can offer you one dose or two dose... One of them lasts a year, one of them lasts 18 months. I don't think we're gonna have the informed choice until next year.
KIRA: Okay. And right now the steep demand is outstripping the supply, and there's been a lot of pressure put on the vaccine makers to ramp up as quickly as possible. Of course, they say that they're doing that and the government is pressuring them to do that, but when do you think we'll cross over to the point where vaccine hesitancy is a bigger issue than vaccine demand?
DR. CAPLAN: Yeah. So this is a really interesting issue. I'm glad you asked me this because I think it's got good foresight. The big ethics fight now is scarcity and who goes first, and the ethicists, including me, are having a fine old time arguing about healthcare workers versus policemen versus people who work for UPS versus somebody who's working at the drug store. Who's more important? Why are they more important? Who's essential?
Actually, I think most of that is nonsense, because what we've learned is that you can't do much in the way of micro-allocation, the system strains, and it doesn't work. You've gotta use some pretty broad categories like over 65, still breathing and working, and a kid. The kid will go last, 'cause we don't have the data, everybody else should get in line and the over 65s should probably be first 'cause they're at high risk. We can't do this. We stink at the micro-management of vaccine supply, plus it encourages cheating. So everybody's out there with vaccine hunters, vaccine tourism, bribing, lying, dressing up like a grandmother to get a vaccine. My favorite one was some rich people in Vancouver flew up to the Yukon and pretended to be Inuit aboriginal people to get a vaccine. That will all pass.
We'll have enough vaccine by the summer, more or less, that the issue will then be, "How are we gonna get to herd immunity or at least maximal immunity, knowing that we don't have data on kids?" People under 18, I think are something like 20% of our population. That means the best you could do is 80%. The other population still could be passing the virus, kids here or Europe or wherever. Well, the military refusal rate that I just saw was 30% saying no. I've heard nursing home staff rates, nursing attendants, nursing aids up at 40% to 50% saying no. So these are huge refusal rates, people are nervous about how it works, the vaccine. Some of them are like, "Well Art you take it. If you're still alive in six months, then maybe I'll take it, but I wanna see that it really works and it's safe." And other people say, "We don't wanna be exploited. We don't trust the government, whatever, to offer us these vaccines."
I'm gonna answer that was a long-winded way of saying we're gonna see some mandates, we're gonna see some coercions start to show up in the vaccine supply, because I think, for example, the military. The day one of these license gets... Excuse me, one of these vaccines get licensed, right now they're on an emergency approval, collect data for three or four more months, get the FDA to formally license the thing. I'd say between five minutes and 10 minutes, the military will be mandating. They have no interest in your objection, they have no interest in your choice, they know what the mission is. It's traditionally, we're gonna get you as healthy as we can to fight a war.
The fact that you say, "Gee, I might die." They kind of say, "Yeah, we noticed that, but that's in the military culture. We fight wars and do stuff like that." So they'll be mandating, I think, very rapidly. And I think healthcare workers will. I think most hospitals are gonna say 50% refusal rate among this nursing group? Forget it. We can't risk that. Nursing homes have been devastated by COVID. They're not gonna have aids out there unvaccinated. The only thing holding up the mandates right now is that we don't have full licensure. We have emergency use approvals, and that's good.
But it's a little tough to mandate without full license. The day we get it, three months, four months, we're gonna start to see mandates. And I'll make one more prediction, as long as I'm in a crystal ball mode. It won't be the government at that point that says, you have to be vaccinated. It'll be private business, 'cause they're gonna say, "You know what? Come on my cruise ship, 'cause everybody who works here is vaccinated." "Come on into my bar, everybody who works here is vaccinated." They're gonna start to use it as an advertising marketing lure. "It's safe here. Come on in." So I think they'll say, "If you wanna work on an airline as a flight attendant, you get vaccinated. We have vaccine proof. You can show it on your iPhone, on your whatever, you have a card that you did it." And so I think we'll see many businesses moving to vaccinate so that they can bring their customers back in.
KIRA: So private businesses, that's one thing, because people do not have to patronize those places if they don't wanna get vaccinated. But of course, this is gonna open up a can of worms with schools. Public schools, if they mandate teacher vaccines and you have to send your kid to school and you have to go to work at a school. What happens then?
DR. CAPLAN: Well, schools are gonna be at the end of the line. That's where we have the least data. So I don't think we're gonna see school mandates on kids, maybe not till next year. But we already have school mandates on kids. They were the first group to feel the force of mandates, because it turns out that measles and mumps and whooping cough are easy to get at school, sneezing and coughing on one another. Some states have added flu shots. Many states, California, Maine, New York have actually eliminated exemptions. The only way out for those kids is if they have a health reason. They're not even allowing religious or so-called philosophical or personal choice exemptions. COVID vaccines will just line up right next to those things.
Teachers will demand it, the pressure will be there. We'll have a lot of information by next year on safety. I'm even gonna say people are gonna be less tolerant of non-vaccinators. Now it's sort of like, "Wow. Yeah, I guess." But this time next year, if you haven't vaccinated, people are gonna come to your house and board it up and make you stay inside.
KIRA: Well, given how much we're so dependent on these vaccines to get us back to a regular life, I can understand the sentiment. What is your take on the big controversy right now, just going back towards the present day a little bit more on having kids in schools. Is that something you support before all the teachers have been vaccinated?
DR. CAPLAN: I do, but I have a problem with the definition of a teacher and a school. So by the way, some people that I know, friends of mine have said, "Well, I'm a teacher, I'm a yoga instructor. I'm a teacher, I'm an aerobics instructor. So I should get priority access to vaccination." I don't think that's what we meant by teacher. And here's the difference in schools. I live in Ridgefield, Connecticut. Up the street for me is a very fancy private elementary school. It has endless grounds, open classrooms. If there are eight kids in a class, I'll pass out. It is great. I wish I went to college there. It's a wonderful set up. Do they need to vaccinate everybody? Probably not, they're all sitting six feet apart, everybody in there is gonna mask, they have huge auditoriums. They never have to come in contact.
I've been in some other schools in the Bronx. No ventilation, no plumbing, 35 kids in a class, the teacher's 65. And you sort of think, "Boy, I'd wanna have vaccinate everybody in sight in this place because unless we re-haul the buildings and downsize the class size, people are gonna get sick in here."
They probably were getting sick anyway before COVID, but now COVID makes it worse. They're probably getting the flu or colds at nine times the rate that they were in Ridgefield, Connecticut. So my point is this, high school kids doing certain things, they can come in on a mixed schedule three days a week, two days a week, do their thing, they know how to mask. Am I worried about vaccinating there? Not too much. Elementary school kids need psychosocial development, need to learn social skills, sometimes going to schools that aren't that wonderful. Yeah, let's vaccinate them. So even though I was complaining a bit about micro-management and trying to parse out, here I think you need to do it. I think you're probably gonna say college, I don't know that you have to vaccinate there. High schools, 50/50. Elementary school, let's do them first.
KIRA: Got it. And one more question on kids before I wanna move on, there's been talk about whether it's necessary before kids are allowed to get this vaccine to have the FDA go to full approval with the full bulk of data necessary for that versus just an emergency authorization for the general population, given that kids are at so much lower risk than adults. But then of course, it'll take a lot more time, I imagine, to get the kids the vaccines. What's your take on that?
DR. CAPLAN: We historically have demanded higher levels of evidence to do anything with a kid, and I think that's gonna hold true here too. I don't think you're gonna see emergency-use authorization for people under 18. Maybe they'd cut it and say, "We'll do it 12-18," but just looking at the history of drug development, vaccine development, people are really leery of taking risks with kids and appropriately so. Kids can't even make their own decision. I can decide if I wanna take an emergency-use vaccine, if I think it's too iffy I don't take it right now. So up to me to weigh the risk-benefit. I don't think so. I think you'll see licensing required before we really get it, at least 12 and under. Let's put it there. And I'm not worried about the safety or efficacy of these things in kids. I think there's no reason, given the biological mechanisms, to think they're gonna be any different. But it's gonna be pretty tough pre-licensure to impose anything.
KIRA: And when do you think that licensure for kids under 12 could come?
DR. CAPLAN: Well, two groups of people are now being studied, pregnant women, the studies just launched. They'll probably be done sufficiently by the end of the year. Kids for full licensure, spring next year.
KIRA: Okay. And because this is a big question for a lot of women that I know and women in general who are pregnant, what would you say to them now, where we don't have the data yet on the safety, but they have to decide and they can't wait six or nine more months?
DR. CAPLAN: Vaccinate yesterday. Literally, I think the COVID virus is too dangerous, I think it's dangerous to the mom, I think it's dangerous to the fetus. It is an unknown, but boy, I would bet on the vaccine more than I would taking my chances with the virus.
KIRA: Got it. So let's pivot a little bit and talk about some of the big open questions around the vaccines that we're starting to get some early evidence about. For one thing, do they prevent transmission and not just symptomatic disease. And I think it's worth pointing out for our audience here that there is a big difference between preventing symptoms and preventing infections, as lots of asymptomatic people know. And we have a lot of new real-world evidence from Israel, from Scotland, reporting that even asymptomatic infections are greatly reduced by the Pfizer vaccine, for example. What is your take on how this new data is going to change guidance around post-vaccination behaviors?
DR. CAPLAN: Yeah. What do we got in the podcast? Seven or eight hours to go? That's a tough one. It's complicated. But trying to over-simplify a little bit. So there is a difference, and this has gotten confusing, I fear. Some vaccines prevent you from getting infected at all. It looks like the Pfizer and the Moderna fall into that category. That's great, 'cause no matter what else, it probably means you're gonna reduce transmission, 'cause if you can't be infected, I don't know how you're gonna give it to somebody else. So I'll bet that that's a transmission reduction. Looks like Johnson & Johnson, unclear. Seems to prevent bad symptoms and death but not moderate disease, and it isn't clear that it stops you from getting infected. So that may become an issue in terms of how we strategically approach when we have enough vaccine of the different types. We may wanna say, "Look, in some environments, we've gotta control spread... Nursing home. We wanna see the Moderna there. We wanna see the Pfizer there."
In other situations, we just wanna make sure you're not dead, let's get the Janssen thing out there. And that'll be great. I'll tell you... I'll give you an example from my own current existence. So I've been pretty cautious... As I said, I live in Ridgefield, Connecticut. I have a house, pretty roomy, but I haven't left it very often. I'm willing to take the chance to go shopping. I'll confess I'm even willing to take the chance wearing a mask to go to the drug store and I've had a hair-cut or two. So I've been not hyper-cautious, but cautious. I don't invite people over that I don't know where they've been, so to speak. But now I'm vaccinated, and my wife is fully vaccinated. And the other night for the first time, we went out to an indoor restaurant. Probably haven't done that in 10 months... No, I don't know, six months. But a long time...
KIRA: I hope you really enjoyed that first meal out, 'cause that's something that I dream about. Boy, where am I gonna go and what am I gonna order?
DR. CAPLAN: Yeah. We went to the fanciest restaurant in town, as a matter of fact, and they were social distancing and everybody was masked and the wait staff. But I figure, good enough for me. If the thing isn't gonna kill me, if I was just told I was gonna have a risk of being sick for three days or something, that's good enough for me. I don't wanna infect somebody else. So I'll still mask and do that, I'm not sure. But I'm absolutely ready to say, and in fact, I've scheduled two trips. We're gonna take a trip to Florida, we're gonna take a trip to North Carolina in March and April. I'm figuring even then, things will be better. But everybody's gonna have choices like that to make. It'll be really interesting. If I'm Tony Fauci or one of our big public health guys, I don't want anybody going anywhere, I'm risk-averse, until maybe 2027. I think it'll be controlled and eliminated... We'll have lots of data and everything will be great. I'm a little bit more, shall we say, individual choice-oriented, making individual risk things, like I said. As long as I'm responsible to others.
I don't wanna make anybody else sick, but if I am ready to take the chance of just being sick for a few days, and I believe the vaccines available will keep me out of the hospital and keep me out of the Morticians building. Okay, I'm ready to do it. So each one of us is gonna have to make a value decision, this is what I find interesting, about what's normal. It isn't science. It isn't medicine. It's ethics. You're gonna have to decide how much risk do you wanna take. Do you wanna be a jerk to your neighbor, if you could still have a teeny chance of infecting them? Am I willing to live in a world where COVID is around but it's kinda rare? I know kids are still transmitting, but it's not really a huge risk. That's the kind of value choice that each of us will be faced with.
KIRA: I really appreciate your emphasis on individual choice and values here and letting... Basically allowing people to make those judgments based on their circumstances for themselves. If you're not deathly afraid of getting a mild cold-type illness, then I can understand why you wanna fly or go to a restaurant, and other people might not be comfortable with any risk at all, and they're perfectly welcome to stay home.
DR. CAPLAN: Or they may say, "I'm 80, I have nine chronic diseases. A mild illness still freaks me out." Okay, I get that. I'm perfectly respectful of that. It's interesting. I think we've been used to public health messaging, and people have this attitude that at some point, Fauci or the head of the CDC, somebody's gonna show up on TV and say, "All clear, everything's over, back to normal, we've declared victory over the enemy. It's armistice day." Whatever. It isn't gonna work like that is my prediction. It's gonna be a slow creep, different people deciding, "I'm safe enough, I'm wandering out." Other people say, "No, no, not ready." Or somebody saying, "I'm pregnant. I'm staying in. I don't care what's going on. I'm not gonna take that risk." I think people will be surprised that there isn't going to be a national day of resolution or something. [chuckle]
KIRA: Right. It's more about these individual behaviors and over time, letting people decide what to do. So for example, if you had grandkids and they were not vaccinated, but you are, would you hug them, would you get close to them, how would you behave and how do you think they should behave around you?
DR. CAPLAN: So I'd be still nervous about them transmitting, but I'm also a very strong believer in my vaccine. So yes, I would hug them, and yes, I would have them come to visit. And that's probably gonna happen actually fairly soon. But their parents aren't vaccinated yet. And so I'm still nervous that maybe better not to do a lot of social mingling right now. But yeah, people have said to me, "My grandmom is 94. I don't know how long she's gonna be here. You think if I'm vaccinated it's okay to pay a visit." I'm gonna start to say, "Yeah, I get that."
KIRA: And I think one thing that's lost in these discussions of safety is also the aspect of benefits to human life and why we even live in the first place. We don't live lives of complete safety. We drive, we fly, we do things that are risky, but we take those risks, because it's worth it. So I think that should be part of the discussion overall, not just safety, period.
DR. CAPLAN: And not just saving lives. So ski slopes, there are a lot of orthopedic clinics at the bottom of big ski slopes, and sending a message like, "You can break bones here." But people say, "I wanna do it, I enjoy it." Okay, I'm not sure all the time that we should factor all of that into our pooled insurance plan, but that's a fight for another day. Nonetheless, I would... You know something, I would pay for it 'cause I like to encourage people to enjoy themselves. So I have my bad habits, they have their bad habits. I think it's sort of a wash in a certain way. But more to your point, I think if you look out there and say, there are some areas where we don't let you choose. You must put your kid in a car seat. A kid can't make a decision, the thing is very effective, really saves their lives, they should have a life ahead of them, and we're gonna force it. And I'm all for that.
In other instances, I might go into the restaurant. I think it's part of the general, "Am I gonna drive a car, am I gonna cross a busy street... " As you said, there are many things I have to do where I have to think about the risk-benefit. I may make a lousy calculation and underestimate what it means to get in my car and drive in terms of risk relative to getting hit by lightening or some other risks, but that's a little bit more for me.
KIRA: So that's a really thought-provoking conversation, but I wanna switch for a minute to another question mark around the vaccines besides transmission, is the long-term studies of their effects on the immune system. And one thing that I've noticed some experts are concerned about is the fact that a lot of the people in the placebo groups have dropped out of the trials and gotten the vaccine because ethically you can't withhold the vaccinations from these volunteers, but at the same time, that could be hurting our ability to compare the vaccine's long-term effects against people who haven't had the vaccine for a long time. So how significant is this issue in your mind?
DR. CAPLAN: Big. Some people actually proposed that we not let them drop out, we not tell the subjects in these big trials of vaccines if they were in the placebo group. Can't do that. It's clearly unethical... Achieved consensus on that decades ago, with various studies where the researcher said, "We don't have to tell the subjects that there's a treatment." Tuskegee did that, for example, the horrible study in the early, late '60s, early '70s, where they didn't tell people there was a cure and kept the study going of venereal disease, but there have been many others since. We already know you gotta give them the option. Some people may stay in anyway, but not enough to allow the study to really have integrity. So I think current studies are likely to fall apart and we won't get answers in the way we're used to with randomized trials to the long-term effects or even to the how long does it last question.
We need to build a system that can follow people. We can't rely on them being in an observed clinical trial. We have to start to say, "You register, we're gonna check on you every year to see how you're doing." That's gotta be done. And one other provocative idea, I pushed it long ago, challenge studies. Deliberately infect a small group of people, hopefully healthy people that choose to do it with mild COVID and then see what the vaccine does in them and then get an answer faster if you study them over time, they volunteered knowingly to get exposed this way. I think you're gonna see some challenge studies done particularly to compare vaccines. There are still more vaccines coming, maybe some of them will last longer, cheaper, safer, I don't know. The only way you're gonna study the next round of vaccines is in a challenge study. You're never getting anybody to sign up to be in a placebo control randomized trial.
KIRA: So that was actually my next question, that the UK just approved the first ever challenge study to infect the volunteers on purpose with the virus. Now, the UK has often been much more progressive in doing medical research than the US. Do you think the US will ever get to that point or are we just gonna rely on other countries to do that for us?
DR. CAPLAN: I think we won't get there. We're so conservative, so litigation conscious. People are freaked out that if somebody got sick and died in a challenge study, it would bankrupt the sponsor. I think the UK is on the right path, but I don't really think we're gonna follow.
KIRA: Okay, well, I hope that they can do the work that we really need. And I'm grateful that there are other countries that are more permissive of risk-taking and doing the controversial studies that are required.
DR. CAPLAN: Ironically, if you don't do the challenge studies, the only other way you're gonna get to do big-scale randomized placebo trials is in the poorest countries that can't get anything. And that makes it an awful lot like exploitation, taking advantage, as opposed to choice. But that's where you'd go, you'd say, "Oh, I got this new vaccine, I'll test it out in Sierra Leone and they don't have anything anyway. So better that half of them get the vaccine than not." And I still think the challenge study makes more ethic sense.
KIRA: Yeah, absolutely. That would really be a shame to be put in that position instead of just allowing people to decide. We let people sign up for the army where they might die. What's the ethical difference with signing up for a potentially dangerous study, but if you're young and healthy, the risk is low?
DR. CAPLAN: By the way, the risk from COVID to say, 18 to 35-year-olds, who's who you'd be looking at, is about the same as donating a kidney, which we also allow all the time.
KIRA: Right, right. Great point. Before we finish up here, I just wanna quickly touch on, of course, the big elephant in the room, which we all have to deal with, unfortunately, which is the variants. So I wanna talk about where we stand. I've heard some vaccine experts recently say, like Paul Offit, for example, has said he doesn't expect a fourth surge due to this, but others are more cautious and take the flip side saying, "This is the calm before the storm. We're about to see another huge explosion." California has recently reported a new strain as accounts for maybe potentially 50% of cases now, and it could be 90% by the end of March. But we're seeing such big declines in the numbers in hospitalizations, in cases. So what should people make of these conflicting messages?
DR. CAPLAN: There's an attitude in medicine that many doctors take toward things like incipient or new prostate cancer, sometimes toward breast cancer, or at least lumps. It's called watchful waiting. You pay attention. You watch what's going on. But you don't do anything right away. I would still get vaccinated, I would still take what I could get. I still believe that it's likely that these vaccines are gonna provide some protection, if not against infection, then at least against the worst symptoms and the worst chances of dying because they're really gonna boost up the basic immune system, which should be able to start to fight against viruses.
That said, could we wind up with some virulent new strain that evades the current vaccine platforms? Yes. Is it likely? I don't think so. But what it does mean is get ready to get boosters because the response to new strains that have been a result of viral mutations is you gotta adjust your vaccine. That's what we'll do. I hope it doesn't send us back into quarantine and isolation and distancing and all the rest of it as our only control. I'm hoping that the manufacturers can roll out boosters more quickly than the first round of vaccines.
KIRA: And the FDA has just said that the vaccine developers will not need to start over with new clinical trials to these boosters. So that will greatly expedite the process. And do you think that's the right call?
DR. CAPLAN: Yes, absolutely. You're not changing the fundamental nature of the vaccine platform, you're just tweaking, if you will, which chemistry responds to the virus. So yeah, I do.
KIRA: And one question then that necessarily everyone is gonna wonder is, "Well, if I got the J&J vaccine, can I get an mRNA booster?" Can you mix and match? Is that gonna work for your immune system?
DR. CAPLAN: Yeah. We don't have any idea. And I wouldn't do that right away. I know some countries are thinking about that to get more, if you will, use out of a limited supply. I'd say wait three months and do it the right way, where the data is in evidence. I'm not worried about people getting a second shot of something different and dropping dead. I'm just worried that it won't work. [chuckle] So I'm not a fan of mix and match. You can do it in some studies, by the way. You could do it in some challenge studies and get a faster answer than you would having to try and do this in 30,000 people over a year. But no, I don't think that's a good way to go. And I'm not a big fan of one-shot strategies either. I think, what we know is that the second shot really kicks your immune system into high gear and that's what you want for real protection. So I know why people say it but I wouldn't advocate for it.
KIRA: Right. And for my last question. One of our big themes this year that we'll be following all throughout the year at leaps.org is our progress towards an eventual return to life and return to normalcy. So I have to ask that question to you. Given everything that you know and that we've discussed today, when do you think our lives and society will start to look normal again, with schools, and restaurants, and businesses open, people are flying and gathering without fear, traveling, etcetera?
DR. CAPLAN: I think you're gonna see a lot of that this summer. There's gonna be enough vaccine out there, even if the epidemiologists aren't 100% happy. As I said, I think a lot of people are gonna say, "I'm happy enough, good enough for me. I'm going to sports and I'm flying, and I'm taking a vacation." And we'll be outside again. Remember we had the ability to eat outdoors and congregate less when the weather's better around the whole country, and I think that will open up Europe and the US in addition. What I'm worried about is if we had to go back in the fall to a more controlled environment, either 'cause a new strain appeared, or just because things weren't as efficacious as we hoped they'd be. But I think summer is gonna be good this year.
KIRA: Well, I hope you're right. I hope your crystal ball is working today. [chuckle]
DR. CAPLAN: [chuckle] And if it's not working right, email Kira. Don't talk to me.
KIRA: Yeah, I cannot be held liable for this. Thank you Art for a fascinating discussion. And thanks to everyone for listening. If you like this show, follow Making Sense of Science to hear new episodes coming once a month. And if you wanna give us feedback, we'd love to hear from you. Get in touch on our website, leaps.org. And until next time, thanks everyone.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
New tech for prison reform spreads to 11 states
The U.S. has the highest incarceration rate in the world, costing $182 billion per year, partly because its antiquated data systems often fail to identify people who should be released. A tech nonprofit is trying to change that.
A new non-profit called Recidiviz is using data technology to reduce the size of the U.S. criminal justice system. The bi-coastal company (SF and NYC) is currently working with 11 states to improve their systems and, so far, has helped remove nearly 69,000 people — ones left floundering in jail or on parole when they should have been released.
“The root cause is fragmentation,” says Clementine Jacoby, 31, a software engineer who worked at Google before co-founding Recidiviz in 2019. In the 1970s and 80s, the U.S. built a series of disconnected data systems, and this patchwork is still being used by criminal justice authorities today. It requires parole officers to manually calculate release dates, leading to errors in many cases. “[They] have done everything they need to do to earn their release, but they're still stuck in the system,” Jacoby says.
Recidiviz has built a platform that connects the different databases, with the goal of identifying people who are already qualified for release but remain behind bars or on supervision. “Think of Recidiviz like Google Maps,” says Jacoby, who worked on Maps when she was at the tech giant. Google Maps takes in data from different sources – satellite images, street maps, local business data — and organizes it into one easy view. “Recidiviz does something similar with criminal justice data,” Jacoby explains, “making it easy to identify people eligible to come home or to move to less intensive levels of supervision.”
People like Jacoby’s uncle. His experience with incarceration is what inspired her passion for criminal justice reform in the first place.
The problems are vast
The U.S. has the highest incarceration rate in the world — 2 million people according to the watchdog group, Prison Policy Initiative — at a cost of $182 billion a year. The numbers could be a lot lower if not for an array of problems including inaccurate sentencing calculations, flawed algorithms and parole violations laws.
Sentencing miscalculations
To determine eligibility for release, the current system requires corrections officers to check 21 different requirements spread across five different databases for each of the 90 to 100 people under their supervision. These manual calculations are time prohibitive, says Jacoby, and fall victim to human error.
In addition, Recidiviz found that policies aimed at helping to reduce the prison population don’t always work correctly. A key example is time off for good behavior laws that allow inmates to earn one day off for every 30 days of good behavior. Some states' data systems are built to calculate time off as one day per month of good behavior, rather than per day. Over the course of a decade-long sentence, Jacoby says these miscalculations can lead to a huge discrepancy in the calculated release data and the actual release date.
Algorithms
Commercial algorithm-based software systems for risk assessment continue to be widely used in the criminal justice system, even though a 2018 study published in Science Advances exposed their limitations. After the study went viral, it took three years for the Justice Department to issue a report on their own flawed algorithms used to reduce the federal prison population as part of the 2018 First Step Act. The program, it was determined, overestimated the risk of putting inmates of color into early-release programs.
Despite its name, Recidiviz does not build these types of algorithms for predicting recidivism, or whether someone will commit another crime after being released from prison. Rather, Jacoby says the company’s "descriptive analytics” approach is specifically intended to weed out incarceration inequalities and avoid algorithmic pitfalls.
Parole violation laws
Research shows that 350,000 people a year — about a quarter of the total prison population — are sent back not because they’ve committed another crime, but because they’ve broken a specific rule of their probation. “Things that wouldn't send you or I to prison, but would send someone on parole,” such as crossing county lines or being in the presence of alcohol when they shouldn’t be, are inflating the prison population, says Jacoby.
It’s personal for the co-founder and CEO
“I grew up with an uncle who went into the prison system,” Jacoby says. At 19, he was sentenced to ten years in prison for a non-violent crime. A few months after being released from jail, he was sent back for a non-violent parole violation.
“For my family, the fact that one in four prison admissions are driven not by a crime but by someone who's broken a rule on probation and parole was really profound because that happened to my uncle,” Jacoby says. The experience led her to begin studying criminal justice in high school, then college. She continued her dive into how the criminal justice system works as part of her Passion Project while at Google, a program that allows employees to spend 20 percent of their time on pro-bono work. Two colleagues whose family members had also been stuck in the system joined her.
As part of the project, Jacoby interviewed hundreds of people involved in the criminal justice system. “Those on the right, those on the left, agreed that bad data was slowing down reform,” she says. Their research brought them to North Dakota where they began to understand the root of the problem. The corrections department is making “huge, consequential decisions every day [without] … the data,” Jacoby says. In a new video by Recidiviz not yet released, Jacoby recounts her exchange with the state’s director of corrections who told her, “‘It’s not that we have the data and we just don’t know how to make it public; we don’t have the information you think we have.'"
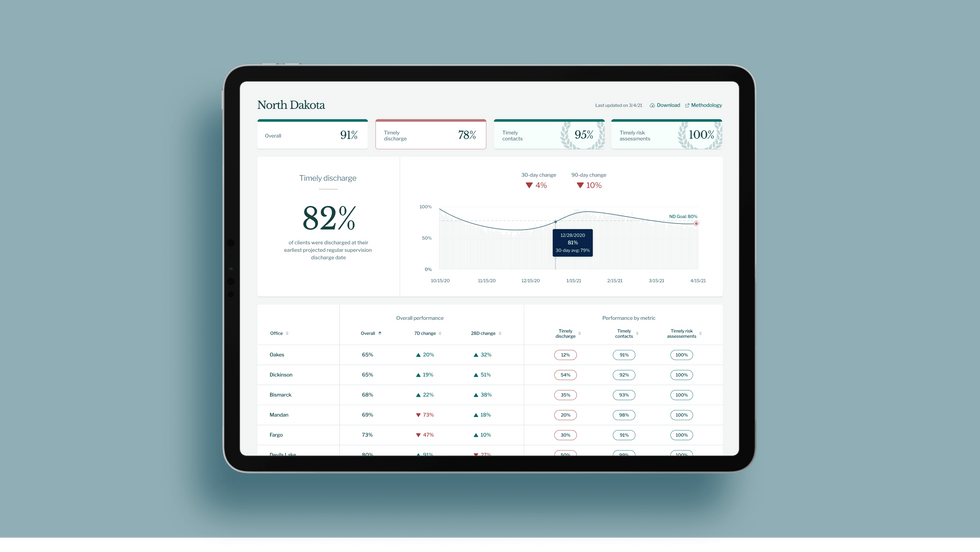
A mock-up (with fake data) of the types of dashboards and insights that Recidiviz provides to state governments.
Recidiviz
As a software engineer, Jacoby says the comment made no sense to her — until she witnessed it first-hand. “We spent a lot of time driving around in cars with corrections directors and parole officers watching them use these incredibly taxing, frankly terrible, old data systems,” Jacoby says.
As they weeded through thousands of files — some computerized, some on paper — they unearthed the consequences of bad data: Hundreds of people in prison well past their release date and thousands more whose release from parole was delayed because of minor paperwork issues. They found individuals stuck in parole because they hadn’t checked one last item off their eligibility list — like simply failing to provide their parole officer with a paystub. And, even when parolees advocated for themselves, the archaic system made it difficult for their parole officers to confirm their eligibility, so they remained in the system. Jacoby and her team also unpacked specific policies that drive racial disparities — such as fines and fees.
The Solution
It’s more than a trivial technical challenge to bring the incomplete, fragmented data onto a 21st century data platform. It takes months for Recidiviz to sift through a state’s information systems to connect databases “with the goal of tracking a person all the way through their journey and find out what’s working for 18- to 25-year-old men, what’s working for new mothers,” explains Jacoby in the video.
TED Talk: How bad data traps people in the U.S. justice system

TED Fellow Clementine Jacoby's TED Talk went live on Jan. 13. It describes how we can fix bad data in the criminal justice system, "bringing thousands of people home, reducing costs and improving public safety along the way."
Clementine Jacoby • TED2022
Ojmarrh Mitchell, an associate professor in the School of Criminology and Criminal Justice at Arizona State University, who is not involved with the company, says what Recidiviz is doing is “remarkable.” His perspective goes beyond academic analysis. In his pre-academic years, Mitchell was a probation officer, working within the framework of the “well known, but invisible” information sharing issues that plague criminal justice departments. The flexibility of Recidiviz’s approach is what makes it especially innovative, he says. “They identify the specific gaps in each jurisdiction and tailor a solution for that jurisdiction.”
On the downside, the process used by Recidiviz is “a bit opaque,” Mitchell says, with few details available on how Recidiviz designs its tools and tracks outcomes. By sharing more information about how its actions lead to progress in a given jurisdiction, Recidiviz could help reformers in other places figure out which programs have the best potential to work well.
The eleven states in which Recidiviz is working include California, Colorado, Maine, Michigan, Missouri, Pennsylvania and Tennessee. And a pilot program launched last year in Idaho, if scaled nationally, with could reduce the number of people in the criminal justice system by a quarter of a million people, Jacoby says. As part of the pilot, rather than relying on manual calculations, Recidiviz is equipping leaders and the probation officers with actionable information with a few clicks of an app that Recidiviz built.
Mitchell is disappointed that there’s even the need for Recidiviz. “This is a problem that government agencies have a responsibility to address,” he says. “But they haven’t.” For one company to come along and fill such a large gap is “remarkable.”
How Leqembi became the biggest news in Alzheimer’s disease in 40 years, and what comes next
Betsy Groves, 73, with her granddaughter. Groves learned in 2021 that she has Alzheimer's disease. She hopes to take Leqembi, a drug approved by the FDA last week.
A few months ago, Betsy Groves traveled less than a mile from her home in Cambridge, Mass. to give a talk to a bunch of scientists. The scientists, who worked for the pharmaceutical companies Biogen and Eisai, wanted to know how she lived her life, how she thought about her future, and what it was like when a doctor’s appointment in 2021 gave her the worst possible news. Groves, 73, has Alzheimer’s disease. She caught it early, through a lumbar puncture that showed evidence of amyloid, an Alzheimer’s hallmark, in her cerebrospinal fluid. As a way of dealing with her diagnosis, she joined the Alzheimer’s Association’s National Early-Stage Advisory Board, which helped her shift into seeing her diagnosis as something she could use to help others.
After her talk, Groves stayed for lunch with the scientists, who were eager to put a face to their work. Biogen and Eisai were about to release the first drug to successfully combat Alzheimer’s in 40 years of experimental disaster. Their drug, which is known by the scientific name lecanemab and the marketing name Leqembi, was granted accelerated approval by the U.S. Food and Drug Administration last Friday, Jan. 6, after a study in 1,800 people showed that it reduced cognitive decline by 27 percent over 18 months.
It is no exaggeration to say that this result is a huge deal. The field of Alzheimer’s drug development has been absolutely littered with failures. Almost everything researchers have tried has tanked in clinical trials. “Most of the things that we've done have proven not to be effective, and it's not because we haven’t been taking a ton of shots at goal,” says Anton Porsteinsson, director of the University of Rochester Alzheimer's Disease Care, Research, and Education Program, who worked on the lecanemab trial. “I think it's fair to say you don't survive in this field unless you're an eternal optimist.”
As far back as 1984, a cure looked like it was within reach: Scientists discovered that the sticky plaques that develop in the brains of those who have Alzheimer’s are made up of a protein fragment called beta-amyloid. Buildup of beta-amyloid seemed to be sufficient to disrupt communication between, and eventually kill, memory cells. If that was true, then the cure should be straightforward: Stop the buildup of beta-amyloid; stop the Alzheimer’s disease.
It wasn’t so simple. Over the next 38 years, hundreds of drugs designed either to interfere with the production of abnormal amyloid or to clear it from the brain flamed out in trials. It got so bad that neuroscience drug divisions at major pharmaceutical companies (AstraZeneca, Pfizer, Bristol-Myers, GSK, Amgen) closed one by one, leaving the field to smaller, scrappier companies, like Cambridge-based Biogen and Tokyo-based Eisai. Some scientists began to dismiss the amyloid hypothesis altogether: If this protein fragment was so important to the disease, why didn’t ridding the brain of it do anything for patients? There was another abnormal protein that showed up in the brains of Alzheimer’s patients, called tau. Some researchers defected to the tau camp, or came to believe the proteins caused damage in combination.
The situation came to a head in 2021, when the FDA granted provisional approval to a drug called aducanumab, marketed as Aduhelm, against the advice of its own advisory council. The approval was based on proof that Aduhelm reduced beta-amyloid in the brain, even though one research trial showed it had no effect on people’s symptoms or daily life. Aduhelm could also cause serious side effects, like brain swelling and amyloid related imaging abnormalities (known as ARIA, these are basically micro-bleeds that appear on MRI scans). Without a clear benefit to memory loss that would make these risks worth it, Medicare refused to pay for Aduhelm among the general population. Two congressional committees launched an investigation into the drug’s approval, citing corporate greed, lapses in protocol, and an unjustifiably high price. (Aduhelm was also produced by the pharmaceutical company Biogen.)
To be clear, Leqembi is not the cure Alzheimer’s researchers hope for. While the drug is the first to show clear signs of a clinical benefit, the scientific establishment is split on how much of a difference Leqembi will make in the real world.
So far, Leqembi is like Aduhelm in that it has been given accelerated approval only for its ability to remove amyloid from the brain. Both are monoclonal antibodies that direct the immune system to attack and clear dysfunctional beta-amyloid. The difference is that, while that’s all Aduhelm was ever shown to do, Leqembi’s makers have already asked the FDA to give it full approval – a decision that would increase the likelihood that Medicare will cover it – based on data that show it also improves Alzheimer’s sufferer’s lives. Leqembi targets a different type of amyloid, a soluble version called “protofibrils,” and that appears to change the effect. “It can give individuals and their families three, six months longer to be participating in daily life and living independently,” says Claire Sexton, PhD, senior director of scientific programs & outreach for the Alzheimer's Association. “These types of changes matter for individuals and for their families.”
To be clear, Leqembi is not the cure Alzheimer’s researchers hope for. It does not halt or reverse the disease, and people do not get better. While the drug is the first to show clear signs of a clinical benefit, the scientific establishment is split on how much of a difference Leqembi will make in the real world. It has “a rather small effect,” wrote NIH Alzheimer’s researcher Madhav Thambisetty, MD, PhD, in an email to Leaps.org. “It is unclear how meaningful this difference will be to patients, and it is unlikely that this level of difference will be obvious to a patient (or their caregivers).” Another issue is cost: Leqembi will become available to patients later this month, but Eisai is setting the price at $26,500 per year, meaning that very few patients will be able to afford it unless Medicare chooses to reimburse them for it.
The same side effects that plagued Aduhelm are common in Leqembi treatment as well. In many patients, amyloid doesn’t just accumulate around neurons, it also forms deposits in the walls of blood vessels. Blood vessels that are shot through with amyloid are more brittle. If you infuse a drug that targets amyloid, brittle blood vessels in the brain can develop leakage that results in swelling or bleeds. Most of these come with no symptoms, and are only seen during testing, which is why they are called “imaging abnormalities.” But in situations where patients have multiple diseases or are prescribed incompatible drugs, they can be serious enough to cause death. The three deaths reported from Leqembi treatment (so far) are enough to make Thambisetty wonder “how well the drug may be tolerated in real world clinical practice where patients are likely to be sicker and have multiple other medical conditions in contrast to carefully selected patients in clinical trials.”
Porsteinsson believes that earlier detection of Alzheimer’s disease will be the next great advance in treatment, a more important step forward than Leqembi’s approval.
Still, there are reasons to be excited. A successful Alzheimer’s drug can pave the way for combination studies, in which patients try a known effective drug alongside newer, more experimental ones; or preventative studies, which take place years before symptoms occur. It also represents enormous strides in researchers’ understanding of the disease. For example, drug dosages have increased massively—in some cases quadrupling—from the early days of Alzheimer’s research. And patient selection for studies has changed drastically as well. Doctors now know that you’ve got to catch the disease early, through PET-scans or CSF tests for amyloid, if you want any chance of changing its course.
Porsteinsson believes that earlier detection of Alzheimer’s disease will be the next great advance in treatment, a more important step forward than Leqembi’s approval. His lab already uses blood tests for different types of amyloid, for different types of tau, and for measures of neuroinflammation, neural damage, and synaptic health, but commercially available versions from companies like C2N, Quest, and Fuji Rebio are likely to hit the market in the next couple of years. “[They are] going to transform the diagnosis of Alzheimer's disease,” Porsteinsson says. “If someone is experiencing memory problems, their physicians will be able to order a blood test that will tell us if this is the result of changes in your brain due to Alzheimer's disease. It will ultimately make it much easier to identify people at a very early stage of the disease, where they are most likely to benefit from treatment.”
Learn more about new blood tests to detect Alzheimer's
Early detection can help patients for more philosophical reasons as well. Betsy Groves credits finding her Alzheimer’s early with giving her the space to understand and process the changes that were happening to her before they got so bad that she couldn’t. She has been able to update her legal documents and, through her role on the Advisory Group, help the Alzheimer’s Association with developing its programs and support services for people in the early stages of the disease. She still drives, and because she and her husband love to travel, they are hoping to get out of grey, rainy Cambridge and off to Texas or Arizona this spring.
Because her Alzheimer’s disease involves amyloid deposits (a “substantial portion” do not, says Claire Sexton, which is an additional complication for research), and has not yet reached an advanced stage, Groves may be a good candidate to try Leqembi. She says she’d welcome the opportunity to take it. If she can get access, Groves hopes the drug will give her more days to be fully functioning with her husband, daughters, and three grandchildren. Mostly, she avoids thinking about what the latter stages of Alzheimer’s might be like, but she knows the time will come when it will be her reality. “So whatever lecanemab can do to extend my more productive ways of engaging with relationships in the world,” she says. “I'll take that in a minute.”

