The New Prospective Parenthood: When Does More Info Become Too Much?
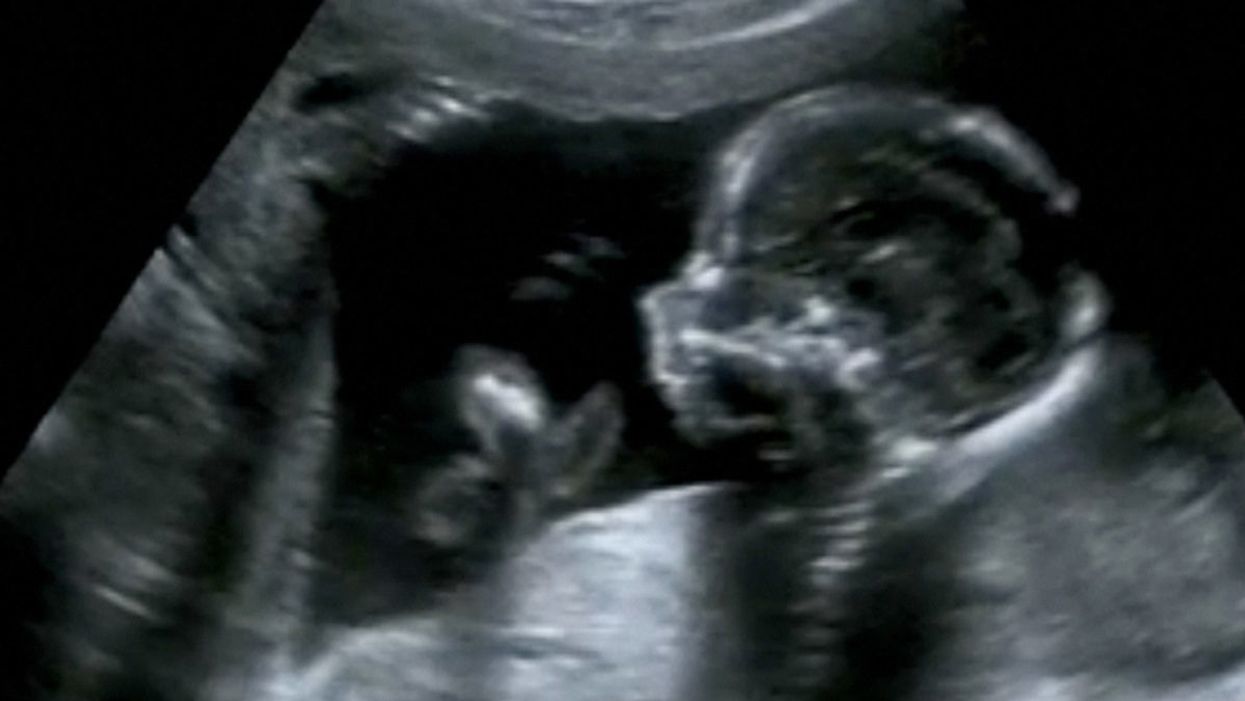
Obstetric ultrasound of a fourth-month fetus.
Peggy Clark was 12 weeks pregnant when she went in for a nuchal translucency (NT) scan to see whether her unborn son had Down syndrome. The sonographic scan measures how much fluid has accumulated at the back of the baby's neck: the more fluid, the higher the likelihood of an abnormality. The technician said the baby was in such an odd position, the test couldn't be done. Clark, whose name has been changed to protect her privacy, was told to come back in a week and a half to see if the baby had moved.
"With the growing sophistication of prenatal tests, it seems that the more questions are answered, the more new ones arise."
"It was like the baby was saying, 'I don't want you to know,'" she recently recalled.
When they went back, they found the baby had a thickened neck. It's just one factor in identifying Down's, but it's a strong indication. At that point, she was 13 weeks and four days pregnant. She went to the doctor the next day for a blood test. It took another two weeks for the results, which again came back positive, though there was still a .3% margin of error. Clark said she knew she wanted to terminate the pregnancy if the baby had Down's, but she didn't want the guilt of knowing there was a small chance the tests were wrong. At that point, she was too late to do a Chorionic villus sampling (CVS), when chorionic villi cells are removed from the placenta and sequenced. And she was too early to do an amniocentesis, which isn't done until between 14 and 20 weeks of the pregnancy. So she says she had to sit and wait, calling those few weeks "brutal."
By the time they did the amnio, she was already nearly 18 weeks pregnant and was getting really big. When that test also came back positive, she made the anguished decision to end the pregnancy.
Now, three years after Clark's painful experience, a newer form of prenatal testing routinely gives would-be parents more information much earlier on, especially for women who are over 35. As soon as nine weeks into their pregnancies, women can have a simple blood test to determine if there are abnormalities in the DNA of chromosomes 21, which indicates Down syndrome, as well as in chromosomes 13 and 18. Using next-generation sequencing technologies, the test separates out and examines circulating fetal cells in the mother's blood, which eliminates the risks of drawing fluid directly from the fetus or placenta.
"Finding out your baby has Down syndrome at 11 or 12 weeks is much easier for parents to make any decision they may want to make, as opposed to 16 or 17 weeks," said Dr. Leena Nathan, an obstetrician-gynecologist in UCLA's healthcare system. "People are much more willing or able to perhaps make a decision to terminate the pregnancy."
But with the growing sophistication of prenatal tests, it seems that the more questions are answered, the more new ones arise--questions that previous generations have never had to face. And as genomic sequencing improves in its predictive accuracy at the earliest stages of life, the challenges only stand to increase. Imagine, for example, learning your child's lifetime risk of breast cancer when you are ten weeks pregnant. Would you terminate if you knew she had a 70 percent risk? What about 40 percent? Lots of hard questions. Few easy answers. Once the cost of whole genome sequencing drops low enough, probably within the next five to ten years according to experts, such comprehensive testing may become the new standard of care. Welcome to the future of prospective parenthood.
"In one way, it's a blessing to have this information. On the other hand, it's very difficult to deal with."
How Did We Get Here?
Prenatal testing is not new. In 1979, amniocentesis was used to detect whether certain inherited diseases had been passed on to the fetus. Through the 1980s, parents could be tested to see if they carried disease like Tay-Sachs, Sickle cell anemia, Cystic fibrosis and Duchenne muscular dystrophy. By the early 1990s, doctors could test for even more genetic diseases and the CVS test was beginning to become available.
A few years later, a technique called preimplantation genetic diagnosis (PGD) emerged, in which embryos created in a lab with sperm and harvested eggs would be allowed to grow for several days and then cells would be removed and tested to see if any carried genetic diseases. Those that weren't affected could be transferred back to the mother. Once in vitro fertilization (IVF) took off, so did genetic testing. The labs test the embryonic cells and get them back to the IVF facilities within 24 hours so that embryo selection can occur. In the case of IVF, genetic tests are done so early, parents don't even have to decide whether to terminate a pregnancy. Embryos with issues often aren't even used.
"It was a very expensive endeavor but exciting to see our ability to avoid disorders, especially for families that don't want to terminate a pregnancy," said Sara Katsanis, an expert in genetic testing who teaches at Duke University. "In one way, it's a blessing to have this information (about genetic disorders). On the other hand, it's very difficult to deal with. To make that decision about whether to terminate a pregnancy is very hard."
Just Because We Can, Does It Mean We Should?
Parents in the future may not only find out whether their child has a genetic disease but will be able to potentially fix the problem through a highly controversial process called gene editing. But because we can, does it mean we should? So far, genes have been edited in other species, but to date, the procedure has not been used on an unborn child for reproductive purposes apart from research.
"There's a lot of bioethics debate and convening of groups to try to figure out where genetic manipulation is going to be useful and necessary, and where it is going to need some restrictions," said Katsanis. She notes that it's very useful in areas like cancer research, so one wouldn't want to over-regulate it.
There are already some criteria as to which genes can be manipulated and which should be left alone, said Evan Snyder, professor and director of the Center for Stem Cells and Regenerative Medicine at Sanford Children's Health Research Center in La Jolla, Calif. He noted that genes don't stand in isolation. That is, if you modify one that causes disease, will it disrupt others? There may be unintended consequences, he added.
"As the technical dilemmas get fixed, some of the ethical dilemmas get fixed. But others arise. It's kind of like ethical whack-a-mole."
But gene editing of embryos may take years to become an acceptable practice, if ever, so a more pressing issue concerns the rationale behind embryo selection during IVF. Prospective parents can end up with anywhere from zero to thirty embryos from the procedure and must choose only one (rarely two) to implant. Since embryos are routinely tested now for certain diseases, and selected or discarded based on that information, should it be ethical—and legal—to make selections based on particular traits, too? To date so far, parents can select for gender, but no other traits. Whether trait selection becomes routine is a matter of time and business opportunity, Katsanis said. So far, the old-fashioned way of making a baby combined with the luck of the draw seems to be the preferred method for the marketplace. But that could change.
"You can easily see a family deciding not to implant a lethal gene for Tay-Sachs or Duchene or Cystic fibrosis. It becomes more ethically challenging when you make a decision to implant girls and not any of the boys," said Snyder. "And then as we get better and better, we can start assigning genes to certain skills and this starts to become science fiction."
Once a pregnancy occurs, prospective parents of all stripes will face decisions about whether to keep the fetus based on the information that increasingly robust prenatal testing will provide. What influences their decision is the crux of another ethical knot, said Snyder. A clear-cut rationale would be if the baby is anencephalic, or it has no brain. A harder one might be, "It's a girl, and I wanted a boy," or "The child will only be 5' 2" tall in adulthood."
"Those are the extremes, but the ultimate question is: At what point is it a legitimate response to say, I don't want to keep this baby?'" he said. Of course, people's responses will vary, so the bigger conundrum for society is: Where should a line be drawn—if at all? Should a woman who is within the legal scope of termination (up to around 24 weeks, though it varies by state) be allowed to terminate her pregnancy for any reason whatsoever? Or must she have a so-called "legitimate" rationale?
"As the technical dilemmas get fixed, some of the ethical dilemmas get fixed. But others arise. It's kind of like ethical whack-a-mole," Snyder said.
One of the newer moles to emerge is, if one can fix a damaged gene, for how long should it be fixed? In one child? In the family's whole line, going forward? If the editing is done in the embryo right after the egg and sperm have united and before the cells begin dividing and becoming specialized, when, say, there are just two or four cells, it will likely affect that child's entire reproductive system and thus all of that child's progeny going forward.
"This notion of changing things forever is a major debate," Snyder said. "It literally gets into metaphysics. On the one hand, you could say, well, wouldn't it be great to get rid of Cystic fibrosis forever? What bad could come of getting rid of a mutant gene forever? But we're not smart enough to know what other things the gene might be doing, and how disrupting one thing could affect this network."
As with any tool, there are risks and benefits, said Michael Kalichman, Director of the Research Ethics Program at the University of California San Diego. While we can envision diverse benefits from a better understanding of human biology and medicine, it is clear that our species can also misuse those tools – from stigmatizing children with certain genetic traits as being "less than," aka dystopian sci-fi movies like Gattaca, to judging parents for making sure their child carries or doesn't carry a particular trait.
"The best chance to ensure that the benefits of this technology will outweigh the risks," Kalichman said, "is for all stakeholders to engage in thoughtful conversations, strive for understanding of diverse viewpoints, and then develop strategies and policies to protect against those uses that are considered to be problematic."
Avalanche rescue dogs train to find and dig out people buried in snow slides
Two-and-a-half year-old Huckleberry, a blue merle Australian shepherd, pulls hard at her leash; her yelps can be heard by skiers and boarders high above on the chairlift that carries them over the ski patrol hut to the top of the mountain. Huckleberry is an avalanche rescue dog — or avy dog, for short. She lives and works with her owner and handler, a ski patroller at Breckenridge Ski Resort in Colorado. As she watches the trainer play a game of hide-and-seek with six-month-old Lume, a golden retriever and avy dog-in-training, Huckleberry continues to strain on her leash; she loves the game. Hide-and-seek is one of the key training methods for teaching avy dogs the rescue skills they need to find someone caught in an avalanche — skier, snowmobiler, hiker, climber.
Lume’s owner waves a T-shirt in front of the puppy. While another patroller holds him back, Lume’s owner runs away and hides. About a minute later — after a lot of barking — Lume is released and commanded to “search.” He springs free, running around the hut to find his owner who reacts with a great amount of excitement and fanfare. Lume’s scent training will continue for the rest of the ski season (Breckenridge plans operating through May or as long as weather permits) and through the off-season. “We make this game progressively harder by not allowing the dog watch the victim run away,” explains Dave Leffler, Breckenridge's ski patroller and head of the avy dog program, who has owned, trained and raised many of them. Eventually, the trainers “dig an open hole in the snow to duck out of sight and gradually turn the hole into a cave where the dog has to dig to get the victim,” explains Leffler.
By the time he is three, Lume, like Huckleberry, will be a fully trained avy pup and will join seven other avy dogs on Breckenridge ski patrol team. Some of the team members, both human and canine, are also certified to work with Colorado Rapid Avalanche Deployment, a coordinated response team that works with the Summit County Sheriff’s office for avalanche emergencies outside of the ski slopes’ boundaries.
There have been 19 avalanche deaths in the U.S. this season, according to avalanche.org, which tracks slides; eight in Colorado. During the entirety of last season there were 17. Avalanche season runs from November through June, but avalanches can occur year-round.
High tech and high stakes
Complementing avy dogs’ ability to smell people buried in a slide, avalanche detection, rescue and recovery is becoming increasingly high tech. There are transceivers, signal locators, ground scanners and drones, which are considered “games changers” by many in avalanche rescue and recovery
For a person buried in an avalanche, the chance of survival plummets after 20 minutes, so every moment counts.
A drone can provide thermal imaging of objects caught in a slide; what looks like a rock from far away might be a human with a heat signature. Transceivers, also known as beacons, send a signal from an avalanche victim to a companion. Signal locators, like RECCO reflectors which are often sewn directly into gear, can echo back a radar signal sent by a detector; most ski resorts have RECCO detector units.
Research suggests that Ground Penetrating Radar (GPR), an electromagnetic tool used by geophysicists to pull images from inside the ground, could be used to locate an avalanche victim. A new study from the Department of Energy’s Sandia National Laboratories suggests that a computer program developed to pinpoint the source of a chemical or biological terrorist attack could also be used to find someone submerged in an avalanche. The search algorithm allows for small robots (described as cockroach-sized) to “swarm” a search area. Researchers say that this distributed optimization algorithm can help find avalanche victims four times faster than current search mechanisms. For a person buried in an avalanche, the chance of survival plummets after 20 minutes, so every moment counts.

An avy dog in training is picking up scent
Sarah McLear
While rescue gear has been evolving, predicting when a slab will fall remains an emerging science — kind of where weather forecasting science was in the 1980s. Avalanche forecasting still relies on documenting avalanches by going out and looking,” says Ethan Greene, director of the Colorado Avalanche Information Center (CAIC). “So if there's a big snowstorm, and as you might remember, most avalanches happened during snowstorms, we could have 10,000 avalanches that release and we document 50,” says Greene. “Avalanche forecasting is essentially pattern recognition,” he adds--and understanding the layering structure of snow.
However, determining where the hazards lie can be tricky. While a dense layer of snow over a softer, weaker layer may be a recipe for an avalanche, there’s so much variability in snowpack that no one formula can predict the trigger. Further, observing and measuring snow at a single point may not be representative of all nearby slopes. Finally, there’s not enough historical data to help avalanche scientists create better prediction models.
That, however, may be changing.
Last year, an international group of researchers created computer simulations of snow cover using 16 years of meteorological data to forecast avalanche hazards, publishing their research in Cold Regions Science and Technology. They believe their models, which categorize different kinds of avalanches, can support forecasting and determine whether the avalanche is natural (caused by temperature changes, wind, additional snowfall) or artificial (triggered by a human or animal).
With smell receptors ranging from 800 million for an average dog, to 4 billion for scent hounds, canines remain key to finding people caught in slides.
With data from two sites in British Columbia and one in Switzerland, researchers built computer simulations of five different avalanche types. “In terms of real time avalanche forecasting, this has potential to fill in a lot of data gaps, where we don't have field observations of what the snow looks like,” says Simon Horton, a postdoctoral fellow with the Simon Fraser University Centre for Natural Hazards Research and a forecaster with Avalanche Canada, who participated in the study. While complex models that simulate snowpack layers have been around for a few decades, they weren’t easy to apply until recently. “It's been difficult to find out how to apply that to actual decision-making and improving safety,” says Horton. If you can derive avalanche problem types from simulated snowpack properties, he says, you’ll learn “a lot about how you want to manage that risk.”
The five categories include “new snow,” which is unstable and slides down the slope, “wet snow,” when rain or heat makes it liquidly, as well as “wind-drifted snow,” “persistent weak layers” and “old snow.” “That's when there's some type of deeply buried weak layer in the snow that releases without any real change in the weather,” Horton explains. “These ones tend to cause the most accidents.” One step by a person on that structurally weak layer of snow will cause a slide. Horton is hopeful that computer simulations of avalanche types can be used by scientists in different snow climates to help predict hazard levels.
Greene is doubtful. “If you have six slopes that are lined up next to each other, and you're going to try to predict which one avalanches and the exact dimensions and what time, that's going to be really hard to do. And I think it's going to be a long time before we're able to do that,” says Greene.
What both researchers do agree on, though, is that what avalanche prediction really needs is better imagery through satellite detection. “Just being able to count the number of avalanches that are out there will have a huge impact on what we do,” Greene says. “[Satellites] will change what we do, dramatically.” In a 2022 paper, scientists at the University of Aberdeen in England used satellites to study two deadly Himalayan avalanches. The imaging helped them determine that sediment from a 2016 ice avalanche plus subsequent snow avalanches contributed to the 2021 avalanche that caused a flash flood, killing over 200 people. The researchers say that understanding the avalanches characteristics through satellite imagery can inform them how one such event increases the magnitude of another in the same area.

Avy dogs trainers hide in dug-out holes in the snow, teaching the dogs to find buried victims
Sarah McLear
Lifesaving combo: human tech and Mother Nature’s gear
Even as avalanche forecasting evolves, dogs with their built-in rescue mechanisms will remain invaluable. With smell receptors ranging from 800 million for an average dog, to 4 billion for scent hounds, canines remain key to finding people caught in slides. (Humans in comparison, have a meager 12 million.) A new study published in the Journal of Neuroscience revealed that in dogs smell and vision are connected in the brain, which has not been found in other animals. “They can detect the smell of their owner's fingerprints on a glass slide six weeks after they touched it,” says Nicholas Dodman, professor emeritus at Cummings School of Veterinary Medicine at Tufts University. “And they can track from a boat where a box filled with meat was buried in the water, 100 feet below,” says Dodman, who is also co-founder and president of the Center for Canine Behavior Studies.
Another recent study from Queens College in Belfast, United Kingdom, further confirms that dogs can smell when humans are stressed. They can also detect the smell of a person’s breath and the smell of the skin cells of a deceased person.
The emerging avalanche-predicting human-made tech and the incredible nature-made tech of dogs’ olfactory talents is the lifesaving “equipment” that Leffler believes in. Even when human-made technology develops further, it will be most efficient when used together with the millions of dogs’ smell receptors, Leffler believes. “It is a combination of technology and the avalanche dog that will always be effective in finding an avalanche victim.”
Living with someone changes your microbiome, new research shows
For the first time, research has shown that bacteria of the microbiome are transmitted between many individuals, not just infants and their mothers, in ways that can’t be explained by having the same diet or geography.
Some roommate frustration can be expected, whether it’s a sink piled high with crusty dishes or crumbs where a clean tabletop should be. Now, research suggests a less familiar issue: person-to-person transmission of shared bacterial strains in our gut and oral microbiomes. For the first time, the lab of Nicola Segata, a professor of genetics and computational biology at the University of Trento, located in Italy, has shown that bacteria of the microbiome are transmitted between many individuals, not just infants and their mothers, in ways that can’t be explained by their shared diet or geography.
It’s a finding with wide-ranging implications, yet frustratingly few predictable outcomes. Our microbiomes are an ever-growing and changing collection of helpful and harmful bacteria that we begin to accumulate the moment we’re born, but experts are still struggling to unravel why and how bacteria from one person’s gut or mouth become established in another person’s microbiome, as opposed to simply passing through.
“If we are looking at the overall species composition of the microbiome, then there is an effect of age of course, and many other factors,” Segata says. “But if we are looking at where our strains are coming from, 99 percent of them are only present in other people’s guts. They need to come from other guts.”
If we could better understand this process, we might be able to control and use it; perhaps hospital patients could avoid infections from other patients when their microbiome is depleted by antibiotics and their immune system is weakened, for example. But scientists are just beginning to link human microbiomes with various ailments. Growing evidence shows that our microbiomes steer our long-term health, impacting conditions like obesity, irritable bowel syndrome, type 2 diabetes, and cancer.
Previous work from Segata’s lab and others illuminated the ways bacteria are passed from mothers to infants during the first few months of life during vaginal birth, breastfeeding and other close contact. And scientists have long known that people in close proximity tend to share bacteria. But the factors related to that overlap, such as genetics and diet, were unclear, especially outside the mother-baby dyad.
“If we look at strain sharing between a mother and an infant at five years of age, for example, we cannot really tell which was due to transmission at birth and which is due to continued transmission because of contact,” Segata says. Experts hypothesized that they could be caused by bacterial similarities in the environment itself, genetics, or bacteria from shared foods that colonized the guts of people in close contact.
Strain sharing was highest in mother-child pairs, with 96 percent of them sharing strains, and only slightly lower in members of shared households, at 95 percent.
In Italy, researchers led by Mireia Valles-Colomer, including Segata, hoped to unravel this mystery. They compared data from 9,715 stool and saliva samples in 31 genomic datasets with existing metadata. Scientists zoomed in on variations in each bacterial strain down to the individual level. They examined not only mother-child pairs, but people living in the same household, adult twins, and people living in the same village in a level of detail that wasn’t possible before, due to its high cost and difficulties in retrieving data about interactions between individuals, Segata explained.
“This paper is, with high granularity, quantifying the percent sharing that you expect between different types of social interactions, controlling for things like genetics and diet,” Gibbons says. Strain sharing was highest in mother-child pairs, with 96 percent of them sharing strains, and only slightly lower in members of shared households, at 95 percent. And at least half of the mother-infant pairs shared 30 percent of their strains; the median was 12 percent among people in shared households. Yet, there was no sharing among eight percent of adult twins who lived separately, and 16 percent of people within villages who resided in different households. The results were published in Nature.
It’s not a regional phenomenon. Although the types of bacterial strains varied depending on whether people lived in western and eastern nations — datasets were drawn from 20 countries on five continents — the patterns of sharing were much the same. To establish these links, scientists focused on individual variations in shared bacterial strains, differences that create unique bacterial “fingerprints” in each person, while controlling for variables like diet, demonstrating that the bacteria had been transmitted between people and were not the result of environmental similarities.
The impact of this bacterial sharing isn’t clear, but shouldn’t be viewed with trepidation, according to Sean Gibbons, a microbiome scientist at the nonprofit Institute for Systems Biology.
“The vast majority of these bugs are actually either benign or beneficial to our health, and the fact that we're swapping and sharing them and that we can take someone else's strain and supplement or better diversify our own little garden is not necessarily a bad thing,” he says.
"There are hundreds of billions of dollars of investment capital moving into these microbiome therapeutic companies; bugs as drugs, so to speak,” says Sean Gibbons, a microbiome scientist at the Institute for Systems Biology.
Everyday habits like exercising and eating vegetables promote a healthy, balanced gut microbiome, which is linked to better metabolic and immune function, and fewer illnesses. While many people’s microbiomes contain bacteria like C. diff or E. coli, these bacteria don’t cause diseases in most cases because they’re present in low levels. But a microbiome that’s been wiped out by, say, antibiotics, may no longer keep these bacteria in check, allowing them to proliferate and make us sick.
“A big challenge in the microbiome field is being able to rationally predict whether, if you're exposed to a particular bug, it will stick in the context of your specific microbiome,” Gibbons says.
Gibbons predicts that explorations of microbe-based therapeutics will be “exploding” in the coming decades. “There are hundreds of billions of dollars of investment capital moving into these microbiome therapeutic companies; bugs as drugs, so to speak,” he says. Rather than taking a mass-marketed probiotic, a precise understanding of an individual’s microbiome could help target the introduction of just the right bacteria at just the right time to prevent or treat a particular illness.
Because the current study did not differentiate between different types of contact or relationships among household members sharing bacterial strains or determine the direction of transmission, Segata says his current project is examining children in daycare settings and tracking their microbiomes over time to understand the role genetics and everyday interactions play in the level of transmission that occurs.
This relatively newfound ability to trace bacterial variants to minute levels has unlocked the chance for scientists to untangle when and how bacteria leap from one microbiome to another. As researchers come to better understand the factors that permit a strain to establish itself within a microbiome, they could uncover new strategies to control these microbes, harnessing the makeup of each microbiome to help people to resist life-altering medical conditions.

