SCOOP: Largest Cryobank in the U.S. to Offer Ancestry Testing

Vanessa Colimorio (left) and Sharon Kochlany (right) at a farm with their four-year-old twin daughters and one-year-old son. The kids share the same sperm donor.
Sharon Kochlany and Vanessa Colimorio's four-year-old twin girls had a classic school assignment recently: make a family tree. They drew themselves and their one-year-old brother branching off from their moms, with aunts, uncles, and grandparents forking off to the sides.
The recently-gained sovereignty of queer families stands to be lost if a consumer DNA test brings a stranger's identity out of the woodwork.
What you don't see in the invisible space between Kochlany and Colimorio, however, is the sperm donor they used to conceive all three children.
To look at a family tree like this is to see in its purest form that kinship can supersede biology—the boundaries of where this family starts and stops are clear to everyone in it, in spite of a third party's genetic involvement. This kind of self-definition has always been synonymous with LGBTQ families, especially those that rely on donor gametes (sperm or eggs) to exist.
But the world around them has changed quite suddenly: The recent consumer DNA testing boom has made it more complicated than ever for families built through reproductive technology—openly, not secretively—to maintain the strong sense of autonomy and privacy that can be crucial for their emotional security. Prospective parents and cryobanks are now mulling how best to bring a new generation of donor-conceived people into this world in a way that leaves open the choice to know more about their ancestry without obliterating an equally important choice: the right not to know about biological relatives.
For queer parents who have long fought for social acceptance, having a biological relationship to their children has been revolutionary, and using an unknown donor as a means to this end especially so. Getting help from a friend often comes with the expectation that the friend will also have social involvement in the family, which some people are comfortable with, but being able to access sperm from an unknown donor—which queer parents have only been able to openly do since the early 1980s—grants them the reproductive autonomy to create families seemingly on their own. That recently-gained sovereignty stands to be lost if a consumer DNA test brings a stranger's identity out of the woodwork.
At the same time, it's natural for donor-conceived people to want to know more about where they come from ethnically, even if they don't want to know the identity of their donor. As a donor-conceived person myself, I know my donor's self-reported ethnicity, but have often wondered how accurate it is.
Opening the Pandora's box of a consumer DNA test as a way to find out has always felt profoundly unappealing to me, however. Many people have accidentally learned they're donor-conceived by unwittingly using these tools, but I already know that about myself going in, and subsequently know I'll be connected to a large web of people whose existence I'm not interested in learning about. In addition to possibly identifying my anonymous donor, his family could also show up, along with any donor-siblings—other people with whom I share a donor. My single lesbian mom is enough for me, and the trade off to learn more about my ethnic ancestry has never seemed worth it.
In 1992, when I was born, no one was planning for how consumer DNA tests might upend or illuminate one's sense of self. But the donor community has always had to stay nimble with balancing privacy concerns and psychological well-being, so it should come as no surprise that figuring out how to do so in 2020 includes finding a way to offer ancestry insight while circumventing consumer DNA tests.
A New Paradigm
This is the rationale behind unprecedented industry news that LeapsMag can exclusively break: Within the next few weeks, California Cryobank, the largest cryobank in the country, will begin offering genetically-verified ancestry information on the free public part of every donor's anonymous profile in its database, something no other cryobanks yet offer (an exact launch date was not available at the time of publication). Currently, California Cryobank's donor profiles include a short self-reported list that might merely say, "Ancestry: German, Lebanese, Scottish."
The new information will be a report in pie chart form that details exactly what percentages of a donor's DNA come from up to 26 ethnicities—it's analogous to, but on a smaller scale than, the format offered by consumer DNA testing companies, and uses the same base technology that looks for single nucleotide polymorphisms in DNA that are associated with specific ethnicities. But crucially, because the donor takes the DNA test through California Cryobank, not a consumer-facing service, the information is not connected in a network to anyone else's DNA test. It's also taken before any offspring exist so there's no chance of revealing a donor-conceived person's identity this way.
Later, when a donor-conceived person is born, grows up, and wants information about their ethnicity from the donor side, all they need is their donor's anonymous ID number to look it up. The donor-conceived person never takes a genetic test, and therefore also can't accidentally find donor siblings this way. People who want to be connected to donor siblings can use a sibling registry where other people who want to be found share donor ID numbers and look for matches (this is something that's been available for decades, and remains so).
"With genetic testing, you have no control over who reaches out to you, and at what point in your life."
California Cryobank will require all new donors to consent to this extra level of genetic testing, setting a new standard for what information prospective parents and donor-conceived people can expect to have. In the immediate, this information will be most useful for prospective parents looking for donors with specific backgrounds, possibly ones similar to their own.
It's a solution that was actually hiding in plain sight. Two years ago, California Cryobank's partner Sema4, the company handling the genetic carrier testing that's used to screen for heritable diseases, started analyzing ethnic data in its samples. That extra information was being collected because it can help calculate a more accurate assessment of genetic risks that run in certain populations—like Ashkenazi Jews and Tay Sachs disease—than relying on oral family histories. Shortly after a plan to start collecting these extra data, Jamie Shamonki, chief medical officer of California Cryobank, realized the companies would be sitting on a goldmine for a different reason.
"I didn't want to use one of these genetic testing companies like Ancestry to accomplish this," says Shamonki. "The whole thing we're trying to accomplish is also privacy."
Consumer-facing DNA testing companies are not HIPAA compliant (whereas Sema4, which isn't direct-to-consumer, is HIPAA compliant), which means there are no legal privacy protections covering people who add their DNA to these databases. Although some companies, like 23andMe, allow users to opt-out of being connected with genetic relatives, the language can be confusing to navigate, requires a high level of knowledge and self-advocacy on the user's part, and, as an opt-out system, is not set up to protect the user from unwanted information by default; many unwittingly walk right into such information as a result.
Additionally, because consumer-facing DNA testing companies operate outside the legal purview that applies to other health care entities, like hospitals, even a person who does opt-out of being linked to genetic relatives is not protected in perpetuity from being re-identified in the future by a change in company policy. The safest option for people with privacy concerns is to stay out of these databases altogether.
For California Cryobank, the new information about donor heritage won't retroactively be added to older profiles in the system, so donor-conceived people who already exist won't benefit from the ancestry tool, but it'll be the new standard going forward. The company has about 500 available donors right now, many of which have been in their registry for a while; about 100 of those donors, all new, will have this ancestry data on their profiles.
Shamonki says it has taken about two years to get to the point of publicly including ancestry information on a donor's profile because it takes about nine months of medical and psychological screening for a donor to go from walking through the door to being added to their registry. The company wanted to wait to launch until it could offer this information for a significant number of donors. As more new donors come online under the new protocol, the number with ancestry information on their profiles will go up.
For Parents: An Unexpected Complication
While this change will no doubt be welcome progress for LGBTQ families contemplating parenthood, it'll never be possible to put this entire new order back in the box. What are such families who already have donor-conceived children losing in today's world of widespread consumer genetic testing?
Kochlany and Colimorio's twins aren't themselves much older than the moment at-home DNA testing really started to take off. They were born in 2015, and two years later the industry saw its most significant spike. By now, more than 26 million people's DNA is in databases like 23andMe and Ancestry; as a result, it's estimated that within a year, 90 percent of Americans of European descent will be identifiable through these consumer databases, by way of genetic third cousins, even if they didn't want to be found and never took the test themselves. This was the principle behind solving the Golden State Killer cold case.
The waning of privacy through consumer DNA testing fundamentally clashes with the priorities of the cyrobank industry, which has long sought to protect the privacy of donor-conceived people, even as open identification became standard. Since the 1980s, donors have been able to allow their identity to be released to any offspring who is at least 18 and wants the information. Lesbian moms pushed for this option early on so their children—who would obviously know they couldn't possibly be the biological product of both parents—would never feel cut off from the chance to know more about themselves. But importantly, the openness is not a two-way street: the donors can't ever ask for the identities of their offspring. It's the latter that consumer DNA testing really puts at stake.
"23andMe basically created the possibility that there will be donors who will have contact with their donor-conceived children, and that's not something that I think the donor community is comfortable with," says I. Glenn Cohen, director of Harvard Law School's Center for Health Law Policy, Biotechnology & Bioethics. "That's about the donor's autonomy, not the rearing parents' autonomy, or the donor-conceived child's autonomy."
Kochlany and Colimorio have an open identification donor and fully support their children reaching out to California Cryobank to get more information about him if they want to when they're 18, but having a singular name revealed isn't the same thing as having contact, nor is it the same thing as revealing a web of dozens of extended genetic relations. Their concern now is that if their kids participate in genetic testing, a stranger—someone they're careful to refer to as only "the donor" and never "dad"—will reach out to the children to begin some kind of relationship. They know other people who are contemplating giving their children DNA tests, and feel staunchly that it wouldn't be right for their family.
"With genetic testing, you have no control over who reaches out to you, and at what point in your life," Kochlany says. "[People] reaching out and trying to say, 'Hey I know who your dad is' throws a curveball. It's like, 'Wait, I never thought I had a dad.' It might put insecurities in their minds."
"We want them to have the opportunity to choose whether or not they want to reach out," Colimorio adds.
Kochlany says that when their twins are old enough to start asking questions, she and Colimorio plan to frame it like this: "The donor was kind of like a technology that helped us make you a person, and make sure that you exist," she says, role playing a conversation with their kids. "But it's not necessarily that you're looking to this person [for] support or love, or because you're missing a piece."
It's a line in the sand that's present even for couples still far off from conceiving. When Mallory Schwartz, a film and TV producer in Los Angeles, and Lauren Pietra, a marriage and family therapy associate (and Shamonki's step-daughter), talk about getting married someday, it's a package deal with talking about how they'll approach having kids. They feel there are too many variables and choices to make around family planning as a same-sex couple these days to not have those conversations simultaneously. Consumer DNA databases are already on their minds.
"It frustrates me that the DNA databases are just totally unregulated," says Schwartz. "I hope they are by the time we do this. I think everyone deserves a right to privacy when making your family [using a sperm donor]."
"I wouldn't want to create a world where people who are donor-conceived feel like they can't participate in this technology because they're trying to shut out [other] information."
On the prospect of having a donor relation pop up non-consensually for a future child, Pietra says, "I don't like it. It would be really disappointing if the child didn't want [contact], and unfortunately they're on the receiving end."
You can see how important preserving the right to keep this door closed is when you look at what's going on at The Sperm Bank of California. This pioneering cryobank was the first in the world to openly serve LGBTQ people and single women, and also the first to offer the open identification option when it opened in 1982, but not as many people are asking for their donor's identity as expected.
"We're finding a third of young people are coming forward for their donor's identity," says Alice Ruby, executive director. "We thought it would be a higher number." Viewed the other way, two-thirds of the donor-conceived people who could ethically get their donor's identity through The Sperm Bank of California are not asking the cryobank for it.
Ruby says that part of what historically made an open identification program appealing, rather than invasive or nerve-wracking, is how rigidly it's always been formatted around mutual consent, and protects against surprises for all parties. Those [donor-conceived people] who wanted more information were never barred from it, while those who wanted to remain in the dark could. No one group's wish eclipsed the other's. The potential breakdown of a system built around consent, expectations, and respect for privacy is why unregulated consumer DNA testing is most concerning to her as a path for connecting with genetic relatives.
For the last few decades in cryobanks around the world, the largest cohort of people seeking out donor sperm has been lesbian couples, followed by single women. For infertile heterosexual couples, the smallest client demographic, Ruby says donor sperm offers a solution to a medical problem, but in contrast, it historically "provided the ability for [lesbian] couples and single moms to have some reproductive autonomy." Yes, it was still a solution to a biological problem, but it was also a solution to a social one.
The Sperm Bank of California updated its registration forms to include language urging parents, donor-conceived people, and donors not to use consumer DNA tests, and to go through the cryobank if they, understandably, want to learn more about who they're connected to. But truthfully, there's not much else cryobanks can do to protect clients on any side of the donor transaction from surprise contact right now—especially not from relatives of the donor who may not even know someone in their family has donated sperm.
A Tricky Position
Personally, I've known I was donor-conceived from day one. It has never been a source of confusion, angst, or curiosity, and in fact has never loomed particularly large for me in any way. I see it merely as a type of reproductive technology—on par with in vitro fertilization—that enabled me to exist, and, now that I do exist, is irrelevant. Being confronted with my donor's identity or any donor siblings would make this fact of my conception bigger than I need it to be, as an adult with a full-blown identity derived from all of my other life experiences. But I still wonder about the minutiae of my ethnicity in much the same way as anyone else who wonders, and feel there's no safe way for me to find out without relinquishing some of my existential independence.
"People obviously want to participate in 23andMe and Ancestry because they're interested in knowing more about themselves," says Shamonki. "I wouldn't want to create a world where people who are donor-conceived feel like they can't participate in this technology because they're trying to shut out [other] information."
After all, it was the allure of that exact conceit—knowing more about oneself—that seemed to magnetically draw in millions of people to these tools in the first place. It's an experience that clearly taps into a population-wide psychic need, even—perhaps especially—if one's origins are a mystery.
Is Sex for Reproduction About to Become Extinct?
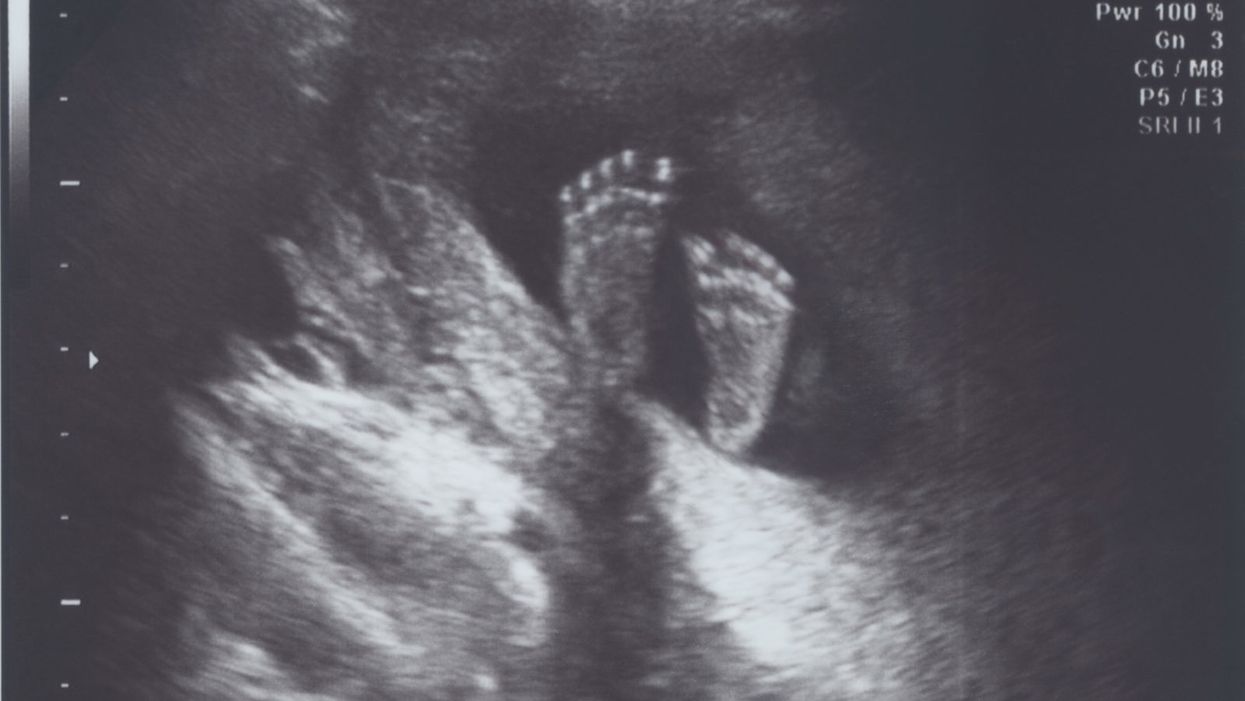
A healthy fetus in utero at 22 weeks.
There are lots of great reasons we humans have sex. We mostly do it to pair bond, realize our primal urges, and feel good. Once in a while, we also do it to make babies. As the coming genetic revolution plays out, we'll still have sex for most of the same reasons we do today. But we'll increasingly not do it to procreate.
Protecting children from harm is one of the core responsibilities of parenting.
Most parents go to great lengths to protect their children from real and imagined harms. This begins with taking prenatal vitamins during pregnancy and extends to having children immunized and protected from exposures to various diseases and dangers. Most of us look askance for good reason at mothers who abuse controlled substances during their pregnancies or parents who choose to not immunize their children. Protecting children from harm is one of the core responsibilities of parenting.
In the United States today, up to two percent of babies are estimated to be born with rare genetic diseases caused by single gene mutations. Sickle cell disease, Tay-Sachs, and Huntington's disease are among the more well-known examples of these, but the list runs to the thousands. Many babies born with these disorders suffer terribly, some die young, and nearly all spend big chunks of their lives struggling through the medical system.
Increasingly, however, many of these single-gene mutation diseases and other chromosomal disorders like Down syndrome are being identified in non-invasive prenatal tests performed on expectant mothers at the end of their first trimester of pregnancy. Knowing the hardship that children born with these types of disorders will likely face, majorities of these women in countries around the world are choosing to terminate pregnancies once these diagnoses have been made. Whatever the justification and whatever anyone's views on the morality of abortion, these decisions are inherently excruciating.
A much smaller number of prospective mothers, however, are today getting this same information about their potential future children before their pregnancies even begin. By undergoing both in vitro fertilization (IVF) and preimplantation genetic testing (PGT), these women are able to know which of the eggs that have been surgically extracted from them and fertilized with their partner or donor's sperm will carry the dangerous mutations. The in vitro embryos with these disorders are simply not implanted in the expectant mother's womb.
It would be monstrous to assert that an existing person with a deadly disease has any less right to thrive than anyone else. But it would also be hard to make a case that parents should affirmatively choose to implant embryos carrying such a disease if given the option. If prospective parents are already today choosing not to implant certain embryos based on our preliminary understanding of disease risk, what will happen when this embryo selection is based on far more information than just a few thousand single gene mutation diseases?
Our ability and willingness to make genetic alterations to our future children will grow over time along with our knowledge and technological ability.
When the first human genome was sequenced in 2003, the race to uncover the mysteries of human genetics had only just begun. Although we still know very little about our genetics relative to the complexity of the genome and even less compared to the broader ecosystem of our biology, the progress toward greater understanding is astounding. Today, the number of single gene mutation diseases and relatively simple genetic traits that can be predicted meaningfully from genetic data alone is already significant.
In the not-distant future, this list will grow to include complex diseases and disease propensities, percentage probabilities of living a long and healthy life, and increasingly the genetic component of complex human attributes like height, IQ, and personality style. This predictive power of genetic analysis will funnel straight into our fertility clinics where prospective parents choosing embryos will be making ever more consequential decisions about the genetic components of the future lives, health, and capabilities of their children.
Our understanding of what the genes extracted from early stage pre-implanted embryos are telling us will be only one of the rocket boosters driving assisted reproduction forward. Another will be the ability to induce adult cells like skin and nucleated blood cells into stem cells and then turn those stem cells into egg progenitor cells and then ultimately eggs. This will not only eliminate the need for hormone treatments and surgery to extract human eggs but also make it easy and cheap to generate an unlimited number of eggs from a given woman.
The average woman has around fifteen eggs extracted during IVF but imagine what generating a thousand eggs will do to the range of possibilities that could be realized through pre-implantation embryo selection. Each of these thousand eggs would be the natural offspring of the two parents, but the variation between them would make it possible to choose the ones with the strongest expression of the genetic component of a particular desired trait – like those with the highest possible genetic IQ potential.
Another rocket booster will be the application of gene editing technologies like CRISPR to edit the genomes of pre-implanted embryos or of the sperm and eggs used to create them. Just this week, Chinese researchers announced they had used CRISPR to edit the CCR5 gene in the pre-implanted embryos of a pair of Chinese twins to make them immune to HIV, the first ever case of gene editing humans and a harbinger of our genetically engineered future. The astounding complexity of the human genome will put limits on our ability to safely make too many simultaneous genetic changes to human embryos, but our ability and willingness to make these types of alterations to our future children will grow over time along with our knowledge and technological ability.
With so much at stake, prospective parents will increasingly have a stark choice when determining how to conceive their children. If they go the traditional route of sex, they will experience both the benign wisdom and unfathomable cruelty of nature. If they use IVF and increasingly informed embryo selection, they will eliminate most single gene mutation diseases and likely increase their children's chances of living a longer and healthier life with more opportunity than their unenhanced peers. But the optimizing parents could also set up their children for misery if these children don't particularly enjoy what they have been optimized to become or see themselves as some type of freakish consumer product with emotions.
Conceiving though sex will come to be seen more and more like not immunizing your children is today, a perfectly natural choice that comes with a significant potential risk and expense.
But although there will be pros and cons on each side, the fight between conception through good old-fashioned sex and conception in the lab will ultimately not be fair. Differences and competition within and between societies will pressure parents and societies to adopt ever more aggressive forms of reproductive technology if they believe doing so will open possibilities and create opportunities for the next generations rather than close them.
Conception through sex will remain as useful as it has always been but lab conception will only get more advantageous. Over time, only zealots will choose to roll the dice of their future children's health and well-being rather than invest, like parents always have, in protecting their children from harm and helping optimize their life potential. Conceiving though sex will come to be seen more and more like not immunizing your children is today, a perfectly natural choice that comes with a significant potential risk and expense to yourself, your children, and your community.
As this future plays out, the genetics and assisted reproduction revolutions will raise enormous, thorny, and massively consequential questions about how we value and invest in diversity, equality, and our own essential humanity – questions we aren't remotely prepared to answer. But these revolutions are coming sooner than most of us understand or are prepared for so we had better get ready.
Because where this trail is ultimately heading goes well beyond sex and toward a fundamental transformation of our evolutionary process as a species – and that should be everybody's business.
Top Fertility Doctor: Artificially Created Sperm and Eggs "Will Become Normal" One Day
A rendering of in vitro fertilization.
Imagine two men making a baby. Or two women. Or an infertile couple. Or an older woman whose eggs are no longer viable. None of these people could have a baby today without the help of an egg or sperm donor.
Cells scraped from the inside of your cheek could one day be manipulated to become either eggs or sperm.
But in the future, it may be possible for them to reproduce using only their own genetic material, thanks to an emerging technology called IVG, or in vitro gametogenesis.
Researchers are learning how to reprogram adult human cells like skin cells to become lab-created egg and sperm cells, which could then be joined to form an embryo. In other words, cells scraped from the inside of your cheek could one day be manipulated to become either eggs or sperm, no matter your gender or your reproductive fitness.
In 2016, Japanese scientists proved that the concept could be successfully carried out in mice. Now some experts, like Dr. John Zhang, the founder and CEO of New Hope Fertility Center in Manhattan, say it's just "a matter of time" before the method is also made to work in humans.
Such a technological tour de force would upend our most basic assumptions about human reproduction and biology. Combined with techniques like gene editing, these tools could eventually enable prospective parents to have an unprecedented level of choice and control over their children's origins. It's a wildly controversial notion, and an especially timely one now that a Chinese scientist has announced the birth of the first allegedly CRISPR-edited babies. (The claims remain unverified.)
Zhang himself is no stranger to controversy. In 2016, he stunned the world when he announced the birth of a baby conceived using the DNA of three people, a landmark procedure intended to prevent the baby from inheriting a devastating neurological disease. (Zhang went to a clinic in Mexico to carry out the procedure because it is prohibited in the U.S.) Zhang's other achievements to date include helping a 49-year-old woman have a baby using her own eggs and restoring a young woman's fertility through an ovarian tissue transplant surgery.
Zhang recently sat down with our Editor-in-Chief in his New York office overlooking Columbus Circle to discuss the fertility world's latest provocative developments. Here are his top ten insights:
Clearly [gene-editing embryos] will be beneficial to mankind, but it's a matter of how and when the work is done.
1) On a Chinese scientist's claim of creating the first CRISPR-edited babies:
I'm glad that we made a first move toward a clinical application of this technology for mankind. Somebody has to do this. Whether this was a good case or not, there is still time to find out.
Clearly it will be beneficial to mankind, but it's a matter of how and when the work is done. Like any scientific advance, it has to be done in a very responsible way.
Today's response is identical to when the world's first IVF baby was announced in 1978. The major news media didn't take it seriously and thought it was evil, wanted to keep a distance from IVF. Many countries even abandoned IVF, but today you see it is a normal practice. And it took almost 40 years [for the researchers] to win a Nobel Prize.
I think we need more time to understand how this work was done medically, ethically, and let the scientist have the opportunity to present how it was done and let a scientific journal publish the paper. Before these become available, I don't think we should start being upset, scared, or giving harsh criticism.
2) On the international outcry in response to the news:
I feel we are in scientific shock, with many thinking it came too fast, too soon. We all embrace modern technology, but when something really comes along, we fear it. In an old Chinese saying, one of the masters always dreamed of seeing the dragon, and when the dragon really came, he got scared.

Dr. John Zhang, the founder and CEO of New Hope Fertility Center in Manhattan, pictured in his office.
3) On the Western world's perception that Chinese scientists sometimes appear to discount ethics in favor of speedy breakthroughs:
I think this perception is not fair. I don't think China is very casual. It's absolutely not what people think. I don't want people to feel that this case [of CRISPR-edited babies] will mean China has less standards over how human reproduction should be performed. Just because this happened, it doesn't mean in China you can do anything you want.
As far as the regulation of IVF clinics, China is probably the most strictly regulated of any country I know in this world.
4) On China's first public opinion poll gauging attitudes toward gene-edited babies, indicating that more than 60 percent of survey respondents supported using the technology to prevent inherited diseases, but not to enhance traits:
There is a sharp contrast between the general public and the professional world. Being a working health professional and an advocate of scientists working in this field, it is very important to be ethically responsible for what we are doing, but my own feeling is that from time to time we may not take into consideration what the patient needs.
5) On how the three-parent baby is doing today, several years after his birth:
No news is good news.
6) On the potentially game-changing research to develop artificial sperm and eggs:
First of all I think that anything that's technically possible, as long as you are not harmful to other people, to other societies, as long as you do it responsibly, and this is a legitimate desire, I think eventually it will become reality.
My research for now is really to try to overcome the very next obstacle in our field, which is how to let a lady age 44 or older have a baby with her own genetic material.
Practically 99 percent of women over age 43 will never make a baby on their own. And after age 47, we usually don't offer donor egg IVF anymore.
But with improved longevity, and quality of life, the lifespan of females continues to increase. In Japan, the average for females is about 89 years old. So for more than half of your life, you will not be able to produce a baby, which is quite significant in the animal kingdom. In most of the animal kingdom, their reproductive life is very much the same as their life, but then you can argue in the animal kingdom unlike a human being, it doesn't take such a long time for them to contribute to the society because once you know how to hunt and look for food, you're done.
"I think this will become a major ethical debate: whether we should let an older lady have a baby at a very late state of her life."
But humans are different. You need to go to college, get certain skills. It takes 20 years to really bring a human being up to become useful to society. That's why the mom and dad are not supposed to have the same reproductive life equal to their real life.
I think this will become a major ethical debate: whether we should let an older lady have a baby at a very late state of her life and leave the future generation in a very vulnerable situation in which they may lack warm caring, proper guidance, and proper education.
7) On using artificial gametes to grant more reproductive choices to gays and lesbians:
I think it is totally possible to have two sperm make a baby, and two eggs make babies.
If we have two guys, one guy to produce eggs, or two girls, one would have to become sperm. Basically you are creating artificial gametes or converting with gametes from sperm to become egg or egg to become a sperm. Which may not necessarily be very difficult. The key is to be able to do nuclear reprogramming.
So why can two sperm not make offspring now? You get exactly half of your genes from each parent. The genes have their own imprinting that say "made in mom," "made in dad." The two sperm would say "made in dad," "made in dad." If I can erase the "made in dad," and say "made in mom," then these sperm can make offspring.
8) On how close science is to creating artificial gametes for clinical use in pregnancies:
It's very hard to say until we accomplish it. It could be very quick. It could be it takes a long time. I don't want to speculate.
"I think these technologies are the solid foundation just like when we designed the computer -- we never thought a computer would become the iPhone."
9) On whether there should be ethical red lines drawn by authorities or whether the decisions should be left to patients and scientists:
I think we cannot believe a hundred percent in the scientist and the patient but it should not be 100 percent authority. It should be coming from the whole of society.
10) On his expectations for the future:
We are living in a very exciting world. I think that all these technologies can really change the way of mankind and also are not just for baby-making. The research, the experience, the mechanism we learn from these technologies, they will shine some great lights into our long-held dream of being a healthy population that is cancer-free and lives a long life, let's say 120 years.
I think these technologies are the solid foundation just like when we designed the computer -- we never thought a computer would become the iPhone. Imagine making a computer 30 years ago, that this little chip will change your life.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.