Should Genetic Information About Mental Health Affect Civil Court Cases?

A rendering of DNA with a judge's gavel.
Imagine this scenario: A couple is involved in a heated custody dispute over their only child. As part of the effort to make the case of being a better guardian, one parent goes on a "genetic fishing expedition": this parent obtains a DNA sample from the other parent with the hope that such data will identify some genetic predisposition to a psychiatric condition (e.g., schizophrenia) and tilt the judge's custody decision in his or her favor.
As knowledge of psychiatric genetics is growing, it is likely to be introduced in civil cases, such as child custody disputes and education-related cases, raising a tangle of ethical and legal questions.
This is an example of how "behavioral genetic evidence" -- an umbrella term for information gathered from family history and genetic testing about pathological behaviors, including psychiatric conditions—may in the future be brought by litigants in court proceedings. Such evidence has been discussed primarily when criminal defendants sought to introduce it to make the claim that they are not responsible for their behavior or to justify their request for reduced sentencing and more lenient punishment.
However, civil cases are an emerging frontier for behavioral genetic evidence. It has already been introduced in tort litigation, such as personal injury claims, and as knowledge of psychiatric genetics is growing, it is further likely to be introduced in other civil cases, such as child custody disputes and education-related cases. But the introduction of such evidence raises a tangle of ethical and legal questions that civil courts will need to address. For example: how should such data be obtained? Who should get to present it and under what circumstances? And does the use of such evidence fit with the purposes of administering justice?
How Did We Get Here?
That behavioral genetic evidence is entering courts is unsurprising. Scientific evidence is a common feature of judicial proceedings, and genetic information may reveal relevant findings. For example, genetic evidence may elucidate whether a child's medical condition is due to genetic causes or medical malpractice, and it has been routinely used to identify alleged offenders or putative fathers. But behavioral genetic evidence is different from such other genetic data – it is shades of gray, instead of black and white.
Although efforts to understand the nature and origins of human behavior are ongoing, existing and likely future knowledge about behavioral genetics is limited. Behavioral disorders are highly complex and diverse. They commonly involve not one but multiple genes, each with a relatively small effect. They are impacted by many, yet unknown, interactions between genes, familial, and environmental factors such as poverty and childhood adversity.
And a specific gene variant may be associated with more than one behavioral disorder and be manifested with significantly different symptoms. Thus, biomarkers about "predispositions" for behavioral disorders cannot generally provide a diagnosis or an accurate estimate of whether, when, and at what severity a behavioral disorder will occur. And, unlike genetic testing that can confirm litigants' identity with 99.99% probability, behavioral genetic evidence is far more speculative.
Genetic theft raises questions about whose behavioral data are being obtained, by whom, and with what authority.
Whether judges, jurors, and other experts understand the nuances of behavioral genetics is unclear. Many people over-estimate the deterministic nature of genetics, and under-estimate the role of environments, especially with regards to mental health status. The U.S. individualistic culture of self-reliance and independence may further tilt the judicial scales because litigants in civil courts may be unjustly blamed for their "bad genes" while structural and societal determinants that lead to poor behavioral outcomes are ignored.
These concerns were recently captured in the Netflix series "13 Reasons Why," depicting a negligence lawsuit against a school brought by parents of a high-school student there (Hannah) who committed suicide. The legal tides shifted from the school's negligence in tolerating a culture of bullying to parental responsibility once cross-examination of Hannah's mother revealed a family history of anxiety, and the possibility that Hannah had a predisposition for mental illness, which (arguably) required therapy even in the absence of clear symptoms.
Where Is This Going?
The concerns are exacerbated given the ways in which behavioral genetic evidence may come to court in the future. One way is through "genetic theft," where genetic evidence is obtained from deserted property, such as soft-drink cans. This method is often used for identification purposes such as criminal and paternity proceedings, and it will likely expand to behavioral genetic data once available through "home kits" that are offered by direct-to-consumer companies.
Genetic theft raises questions about whose behavioral data are being obtained, by whom, and with what authority. In the scenario of child-custody dispute, for example, the sequencing of the other parent's DNA will necessarily intrude on the privacy of that parent, even as the scientific value of such information is limited. A parent on a "genetic fishing expedition" can also secretly sequence their child for psychiatric genetic predispositions, arguably, in order to take preventative measures to reduce the child's risk for developing a behavioral disorder. But should a parent be allowed to sequence the child without the other parent's consent, or regardless of whether the results will provide medical benefits to the child?
Similarly, although schools are required, and may be held accountable for failing to identify children with behavioral disabilities and to evaluate their educational needs, some parents may decline their child's evaluation by mental health professionals. Should schools secretly obtain a sample and sequence children for behavioral disorders, regardless of parental consent? My study of parents found that the overwhelming majority opposed imposed genetic testing by school authorities. But should parental preference or the child's best interests be the determinative factor? Alternatively, could schools use secretly obtained genetic data as a defense that they are fulfilling the child-find requirement under the law?
The stigma associated with behavioral disorders may intimidate some people enough that they back down from just claims.
In general, samples obtained through genetic theft may not meet the legal requirements for admissible evidence, and as these examples suggest, they also involve privacy infringement that may be unjustified in civil litigation. But their introduction in courts may influence judicial proceedings. It is hard to disregard such evidence even if decision-makers are told to ignore it.
The costs associated with genetic testing may further intensify power differences among litigants. Because not everyone can pay for DNA sequencing, there is a risk that those with more resources will be "better off" in court proceedings. Simultaneously, the stigma associated with behavioral disorders may intimidate some people enough that they back down from just claims. For example, a good parent may give up a custody claim to avoid disclosure of his or her genetic predispositions for psychiatric conditions. Regulating this area of law is necessary to prevent misuses of scientific technologies and to ensure that powerful actors do not have an unfair advantage over weaker litigants.
Behavioral genetic evidence may also enter the courts through subpoena of data obtained in clinical, research or other commercial genomic settings such as ancestry testing (similar to the genealogy database recently used to identify the Golden State Killer). Although court orders to testify or present evidence are common, their use for obtaining behavioral genetic evidence raises concerns.
One worry is that it may be over-intrusive. Because behavioral genetics are heritable, such data may reveal information not only about the individual litigant but also about other family members who may subsequently be stigmatized as well. And, even if we assume that many people may be willing for their data in genomic databases to be used to identify relatives who committed crimes (e.g., a rapist or a murderer), we can't assume the same for civil litigation, where the public interest in disclosure is far weaker.
Another worry is that it may deter people from participating in activities that society has an interest in advancing, including medical treatment involving genetic testing and genomic research. To address this concern, existing policy provides expanded privacy protections for NIH-funded genomic research by automatically issuing a Certificate of Confidentiality that prohibits disclosure of identifiable information in any Federal, State, or local civil, criminal, and other legal proceedings.
But this policy has limitations. It applies only to specific research settings and does not cover non-NIH funded research or clinical testing. The Certificate's protections can also be waived under certain circumstances. People who volunteer to participate in non-NIH-funded genomic research for the public good may thus find themselves worse-off if embroiled in legal proceedings.
Consider the following: if a parent in a child custody dispute had participated in a genetic study on schizophrenia years earlier, should the genetic results be subpoenaed by the court – and weaponized by the other parent? Public policy should aim to reduce the risks for such individuals. The end of obtaining behavioral genetic evidence cannot, and should not, always justify the means.
After spaceflight record, NASA looks to protect astronauts on even longer trips
NASA astronaut Frank Rubio floats by the International Space Station’s “window to the world.” Yesterday, he returned from the longest single spaceflight by a U.S. astronaut on record - over one year. Exploring deep space will require even longer missions.
At T-minus six seconds, the main engines of the Atlantis Space Shuttle ignited, rattling its capsule “like a skyscraper in an earthquake,” according to astronaut Tom Jones, describing the 1988 launch. As the rocket lifted off and accelerated to three times the force of Earth's gravity, “It felt as if two of my friends were standing on my chest and wouldn’t get off.” But when Atlantis reached orbit, the main engines cut off, and the astronauts were suddenly weightless.
Since 1961, NASA has sent hundreds of astronauts into space while working to making their voyages safer and smoother. Yet, challenges remain. Weightlessness may look amusing when watched from Earth, but it has myriad effects on cognition, movement and other functions. When missions to space stretch to six months or longer, microgravity can impact astronauts’ health and performance, making it more difficult to operate their spacecraft.
Yesterday, NASA astronaut Frank Rubio returned to Earth after over one year, the longest single spaceflight for a U.S. astronaut. But this is just the start; longer and more complex missions into deep space loom ahead, from returning to the moon in 2025 to eventually sending humans to Mars. To ensure that these missions succeed, NASA is increasing efforts to study the biological effects and prevent harm.
The dangers of microgravity are real
A NASA report published in 2016 details a long list of incidents and near-misses caused – at least partly – by space-induced changes in astronauts’ vision and coordination. These issues make it harder to move with precision and to judge distance and velocity.
According to the report, in 1997, a resupply ship collided with the Mir space station, possibly because a crew member bumped into the commander during the final docking maneuver. This mishap caused significant damage to the space station.
Returns to Earth suffered from problems, too. The same report notes that touchdown speeds during the first 100 space shuttle landings were “outside acceptable limits. The fastest landing on record – 224 knots (258 miles) per hour – was linked to the commander’s momentary spatial disorientation.” Earlier, each of the six Apollo crews that landed on the moon had difficulty recognizing moon landmarks and estimating distances. For example, Apollo 15 landed in an unplanned area, ultimately straddling the rim of a five-foot deep crater on the moon, harming one of its engines.
Spaceflight causes unique stresses on astronauts’ brains and central nervous systems. NASA is working to reduce these harmful effects.
NASA
Space messes up your brain
In space, astronauts face the challenges of microgravity, ionizing radiation, social isolation, high workloads, altered circadian rhythms, monotony, confined living quarters and a high-risk environment. Among these issues, microgravity is one of the most consequential in terms of physiological changes. It changes the brain’s structure and its functioning, which can hurt astronauts’ performance.
The brain shifts upwards within the skull, displacing the cerebrospinal fluid, which reduces the brain’s cushioning. Essentially, the brain becomes crowded inside the skull like a pair of too-tight shoes.
That’s partly because of how being in space alters blood flow. On Earth, gravity pulls our blood and other internal fluids toward our feet, but our circulatory valves ensure that the fluids are evenly distributed throughout the body. In space, there’s not enough gravity to pull the fluids down, and they shift up, says Rachael D. Seidler, a physiologist specializing in spaceflight at the University of Florida and principal investigator on many space-related studies. The head swells and legs appear thinner, causing what astronauts call “puffy face chicken legs.”
“The brain changes at the structural and functional level,” says Steven Jillings, equilibrium and aerospace researcher at the University of Antwerp in Belgium. “The brain shifts upwards within the skull,” displacing the cerebrospinal fluid, which reduces the brain’s cushioning. Essentially, the brain becomes crowded inside the skull like a pair of too-tight shoes. Some of the displaced cerebrospinal fluid goes into cavities within the brain, called ventricles, enlarging them. “The remaining fluids pool near the chest and heart,” explains Jillings. After 12 consecutive months in space, one astronaut had a ventricle that was 25 percent larger than before the mission.
Some changes reverse themselves while others persist for a while. An example of a longer-lasting problem is spaceflight-induced neuro-ocular syndrome, which results in near-sightedness and pressure inside the skull. A study of approximately 300 astronauts shows near-sightedness affects about 60 percent of astronauts after long missions on the International Space Station (ISS) and more than 25 percent after spaceflights of only a few weeks.
Another long-term change could be the decreased ability of cerebrospinal fluid to clear waste products from the brain, Seidler says. That’s because compressing the brain also compresses its waste-removing glymphatic pathways, resulting in inflammation, vulnerability to injuries and worsening its overall health.
The effects of long space missions were best demonstrated on astronaut twins Scott and Mark Kelly. This NASA Twins Study showed multiple, perhaps permanent, changes in Scott after his 340-day mission aboard the ISS, compared to Mark, who remained on Earth. The differences included declines in Scott’s speed, accuracy and cognitive abilities that persisted longer than six months after returning to Earth in March 2016.
By the end of 2020, Scott’s cognitive abilities improved, but structural and physiological changes to his eyes still remained, he said in a BBC interview.
“It seems clear that the upward shift of the brain and compression of the surrounding tissues with ventricular expansion might not be a good thing,” Seidler says. “But, at this point, the long-term consequences to brain health and human performance are not really known.”

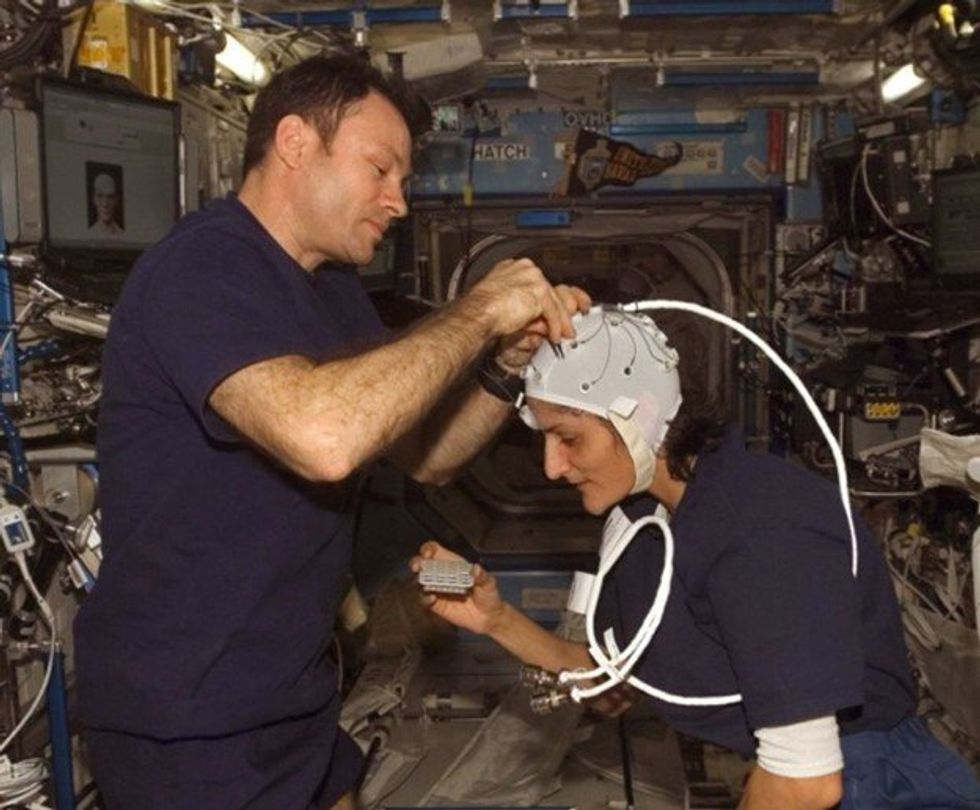
NASA astronaut Kate Rubins conducts a session for the Neuromapping investigation.
NASA
Staying sharp in space
To investigate how prolonged space travel affects the brain, NASA launched a new initiative called the Complement of Integrated Protocols for Human Exploration Research (CIPHER). “CIPHER investigates how long-duration spaceflight affects both brain structure and function,” says neurobehavioral scientist Mathias Basner at the University of Pennsylvania, a principal investigator for several NASA studies. “Through it, we can find out how the brain adapts to the spaceflight environment and how certain brain regions (behave) differently after – relative to before – the mission.”
To do this, he says, “Astronauts will perform NASA’s cognition test battery before, during and after six- to 12-month missions, and will also perform the same test battery in an MRI scanner before and after the mission. We have to make sure we better understand the functional consequences of spaceflight on the human brain before we can send humans safely to the moon and, especially, to Mars.”
As we go deeper into space, astronauts cognitive and physical functions will be even more important. “A trip to Mars will take about one year…and will introduce long communication delays,” Seidler says. “If you are on that mission and have a problem, it may take eight to 10 minutes for your message to reach mission control, and another eight to 10 minutes for the response to get back to you.” In an emergency situation, that may be too late for the response to matter.
“On a mission to Mars, astronauts will be exposed to stressors for unprecedented amounts of time,” Basner says. To counter them, NASA is considering the continuous use of artificial gravity during the journey, and Seidler is studying whether artificial gravity can reduce the harmful effects of microgravity. Some scientists are looking at precision brain stimulation as a way to improve memory and reduce anxiety due to prolonged exposure to radiation in space.
Other scientists are exploring how to protect neural stem cells (which create brain cells) from radiation damage, developing drugs to repair damaged brain cells and protect cells from radiation.
To boldly go where no astronauts have gone before, they must have optimal reflexes, vision and decision-making. In the era of deep space exploration, the brain—without a doubt—is the final frontier.
Additionally, NASA is scrutinizing each aspect of the mission, including astronaut exercise, nutrition and intellectual engagement. “We need to give astronauts meaningful work. We need to stimulate their sensory, cognitive and other systems appropriately,” Basner says, especially given their extreme confinement and isolation. The scientific experiments performed on the ISS – like studying how microgravity affects the ability of tissue to regenerate is a good example.
“We need to keep them engaged socially, too,” he continues. The ISS crew, for example, regularly broadcasts from space and answers prerecorded questions from students on Earth, and can engage with social media in real time. And, despite tight quarters, NASA is ensuring the crew capsule and living quarters on the moon or Mars include private space, which is critical for good mental health.
Exploring deep space builds on a foundation that began when astronauts first left the planet. With each mission, scientists learn more about spaceflight effects on astronauts’ bodies. NASA will be using these lessons to succeed with its plans to build science stations on the moon and, eventually, Mars.
“Through internally and externally led research, investigations implemented in space and in spaceflight simulations on Earth, we are striving to reduce the likelihood and potential impacts of neurostructural changes in future, extended spaceflight,” summarizes NASA scientist Alexandra Whitmire. To boldly go where no astronauts have gone before, they must have optimal reflexes, vision and decision-making. In the era of deep space exploration, the brain—without a doubt—is the final frontier.
A newly discovered brain cell may lead to better treatments for cognitive disorders
Swiss researchers have found a type of brain cell that appears to be a hybrid of the two other main types — and it could lead to new treatments for brain disorders.
Swiss researchers have discovered a third type of brain cell that appears to be a hybrid of the two other primary types — and it could lead to new treatments for many brain disorders.
The challenge: Most of the cells in the brain are either neurons or glial cells. While neurons use electrical and chemical signals to send messages to one another across small gaps called synapses, glial cells exist to support and protect neurons.
Astrocytes are a type of glial cell found near synapses. This close proximity to the place where brain signals are sent and received has led researchers to suspect that astrocytes might play an active role in the transmission of information inside the brain — a.k.a. “neurotransmission” — but no one has been able to prove the theory.
A new brain cell: Researchers at the Wyss Center for Bio and Neuroengineering and the University of Lausanne believe they’ve definitively proven that some astrocytes do actively participate in neurotransmission, making them a sort of hybrid of neurons and glial cells.
According to the researchers, this third type of brain cell, which they call a “glutamatergic astrocyte,” could offer a way to treat Alzheimer’s, Parkinson’s, and other disorders of the nervous system.
“Its discovery opens up immense research prospects,” said study co-director Andrea Volterra.
The study: Neurotransmission starts with a neuron releasing a chemical called a neurotransmitter, so the first thing the researchers did in their study was look at whether astrocytes can release the main neurotransmitter used by neurons: glutamate.
By analyzing astrocytes taken from the brains of mice, they discovered that certain astrocytes in the brain’s hippocampus did include the “molecular machinery” needed to excrete glutamate. They found evidence of the same machinery when they looked at datasets of human glial cells.
Finally, to demonstrate that these hybrid cells are actually playing a role in brain signaling, the researchers suppressed their ability to secrete glutamate in the brains of mice. This caused the rodents to experience memory problems.
“Our next studies will explore the potential protective role of this type of cell against memory impairment in Alzheimer’s disease, as well as its role in other regions and pathologies than those explored here,” said Andrea Volterra, University of Lausanne.
But why? The researchers aren’t sure why the brain needs glutamatergic astrocytes when it already has neurons, but Volterra suspects the hybrid brain cells may help with the distribution of signals — a single astrocyte can be in contact with thousands of synapses.
“Often, we have neuronal information that needs to spread to larger ensembles, and neurons are not very good for the coordination of this,” researcher Ludovic Telley told New Scientist.
Looking ahead: More research is needed to see how the new brain cell functions in people, but the discovery that it plays a role in memory in mice suggests it might be a worthwhile target for Alzheimer’s disease treatments.
The researchers also found evidence during their study that the cell might play a role in brain circuits linked to seizures and voluntary movements, meaning it’s also a new lead in the hunt for better epilepsy and Parkinson’s treatments.
“Our next studies will explore the potential protective role of this type of cell against memory impairment in Alzheimer’s disease, as well as its role in other regions and pathologies than those explored here,” said Volterra.