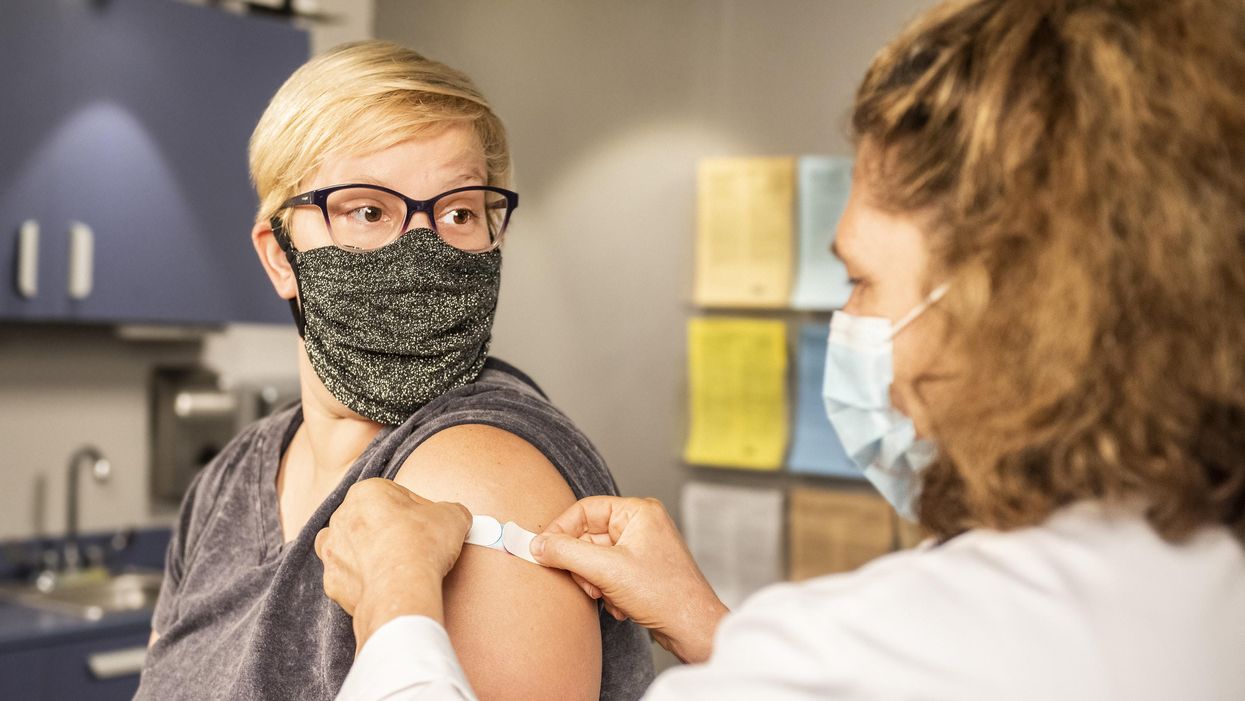
Alzheimer’s prevention may be less about new drugs, more about income, zip code and education

(Left to right) Vickie Naylor, Bernadine Clay, and Donna Maxey read a memory prompt as they take part in the Sharing History through Active Reminiscence and Photo-Imagery (SHARP) study, September 20, 2017.
That your risk of Alzheimer’s disease depends on your salary, what you ate as a child, or the block where you live may seem implausible. But researchers are discovering that social determinants of health (SDOH) play an outsized role in Alzheimer’s disease and related dementias, possibly more than age, and new strategies are emerging for how to address these factors.
At the 2022 Alzheimer’s Association International Conference, a series of presentations offered evidence that a string of socioeconomic factors—such as employment status, social support networks, education and home ownership—significantly affected dementia risk, even when adjusting data for genetic risk. What’s more, memory declined more rapidly in people who earned lower wages and slower in people who had parents of higher socioeconomic status.
In 2020, a first-of-its kind study in JAMA linked Alzheimer’s incidence to “neighborhood disadvantage,” which is based on SDOH indicators. Through autopsies, researchers analyzed brain tissue markers related to Alzheimer’s and found an association with these indicators. In 2022, Ryan Powell, the lead author of that study, published further findings that neighborhood disadvantage was connected with having more neurofibrillary tangles and amyloid plaques, the main pathological features of Alzheimer's disease.
As of yet, little is known about the biological processes behind this, says Powell, director of data science at the Center for Health Disparities Research at the University of Wisconsin School of Medicine and Public Health. “We know the association but not the direct causal pathway.”
The corroborative findings keep coming. In a Nature study published a few months after Powell’s study, every social determinant investigated affected Alzheimer’s risk except for marital status. The links were highest for income, education, and occupational status.
Clinical trials on new Alzheimer’s medications get all the headlines but preventing dementia through policy and public health interventions should not be underestimated.
The potential for prevention is significant. One in three older adults dies with Alzheimer's or another dementia—more than breast and prostate cancers combined. Further, a 2020 report from the Lancet Commission determined that about 40 percent of dementia cases could theoretically be prevented or delayed by managing the risk factors that people can modify.
Take inactivity. Older adults who took 9,800 steps daily were half as likely to develop dementia over the next 7 years, in a 2022 JAMA study. Hearing loss, another risk factor that can be managed, accounts for about 9 percent of dementia cases.
Clinical trials on new Alzheimer’s medications get all the headlines but preventing dementia through policy and public health interventions should not be underestimated. Simply slowing the course of Alzheimer’s or delaying its onset by five years would cut the incidence in half, according to the Global Council on Brain Health.
Minorities Hit the Hardest
The World Health Organization defines SDOH as “conditions in which people are born, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life.”
Anyone who exists on processed food, smokes cigarettes, or skimps on sleep has heightened risks for dementia. But minority groups get hit harder. Older Black Americans are twice as likely to have Alzheimer’s or another form of dementia as white Americans; older Hispanics are about one and a half times more likely.
This is due in part to higher rates of diabetes, obesity, and high blood pressure within these communities. These diseases are linked to Alzheimer’s, and SDOH factors multiply the risks. Blacks and Hispanics earn less income on average than white people. This means they are more likely to live in neighborhoods with limited access to healthy food, medical care, and good schools, and suffer greater exposure to noise (which impairs hearing) and air pollution—additional risk factors for dementia.
Related Reading: The Toxic Effects of Noise and What We're Not Doing About it
Plus, when Black people are diagnosed with dementia, their cognitive impairment and neuropsychiatric symptom are more advanced than in white patients. Why? Some African-Americans delay seeing a doctor because of perceived discrimination and a sense they will not be heard, says Carl V. Hill, chief diversity, equity, and inclusion officer at the Alzheimer’s Association.
Misinformation about dementia is another issue in Black communities. The thinking is that Alzheimer’s is genetic or age-related, not realizing that diet and physical activity can improve brain health, Hill says.
African Americans are severely underrepresented in clinical trials for Alzheimer’s, too. So, researchers miss the opportunity to learn more about health disparities. “It’s a bioethical issue,” Hill says. “The people most likely to have Alzheimer’s aren’t included in the trials.”
The Cure: Systemic Change
People think of lifestyle as a choice but there are limitations, says Muniza Anum Majoka, a geriatric psychiatrist and assistant professor of psychiatry at Yale University, who published an overview of SDOH factors that impact dementia. “For a lot of people, those choices [to improve brain health] are not available,” she says. If you don’t live in a safe neighborhood, for example, walking for exercise is not an option.
Hill wants to see the focus of prevention shift from individual behavior change to ensuring everyone has access to the same resources. Advice about healthy eating only goes so far if someone lives in a food desert. Systemic change also means increasing the number of minority physicians and recruiting minorities in clinical drug trials so studies will be relevant to these communities, Hill says.
Based on SDOH impact research, raising education levels has the most potential to prevent dementia. One theory is that highly educated people have a greater brain reserve that enables them to tolerate pathological changes in the brain, thus delaying dementia, says Majoka. Being curious, learning new things and problem-solving also contribute to brain health, she adds. Plus, having more education may be associated with higher socioeconomic status, more access to accurate information and healthier lifestyle choices.
New Strategies
The chasm between what researchers know about brain health and how the knowledge is being applied is huge. “There’s an explosion of interest in this area. We’re just in the first steps,” says Powell. One day, he predicts that physicians will manage Alzheimer’s through precision medicine customized to the patient’s specific risk factors and needs.
Raina Croff, assistant professor of neurology at Oregon Health & Science University School of Medicine, created the SHARP (Sharing History through Active Reminiscence and Photo-imagery) walking program to forestall memory loss in African Americans with mild cognitive impairment or early dementia.
Participants and their caregivers walk in historically black neighborhoods three times a week over six months. A smart tablet provides information about “Memory Markers” they pass, such as the route of a civil rights march. People celebrate their community and culture while “brain health is running in the background,” Croff says.

Photos and memory prompts engage participants in the SHARP program.
OHSU/Kristyna Wentz-Graff
The project began in 2015 as a pilot study in Croff’s hometown of Portland, Ore., expanded to Seattle, and will soon start in Oakland, Calif. “Walking is good for slowing [brain] decline,” she says. A post-study assessment of 40 participants in 2017 showed that half had higher cognitive scores after the program; 78 percent had lower blood pressure; and 44 percent lost weight. Those with mild cognitive impairment showed the most gains. The walkers also reported improved mood and energy along with increased involvement in other activities.
It’s never too late to reap the benefits of working your brain and being socially engaged, Majoka says.
In Milwaukee, the Wisconsin Alzheimer’s Institute launched the The Amazing Grace Chorus® to stave off cognitive decline in seniors. People in early stages of Alzheimer’s practice and perform six concerts each year. The activity provides opportunities for social engagement, mental stimulation, and a support network. Among the benefits, 55 percent reported better communication at home and nearly half of participants said they got involved with more activities after participating in the chorus.
Private companies are offering intervention services to healthcare providers and insurers to manage SDOH, too. One such service, MyHello, makes calls to at-risk people to assess their needs—be it food, transportation or simply a friendly voice. Having a social support network is critical for seniors, says Majoka, noting there was a steep decline in cognitive function among isolated elders during Covid lockdowns.
About 1 in 9 Americans age 65 or older live with Alzheimer’s today. With a surge in people with the disease predicted, public health professionals have to think more broadly about resource targets and effective intervention points, Powell says.
Beyond breakthrough pills, that is. Like Dorothy in Kansas discovering happiness was always in her own backyard, we are beginning to learn that preventing Alzheimer’s is in our reach if only we recognized it.
Is Carbon Dioxide the New Black? Yes, If These Fabric-Designing Scientists Have Their Way
The entrepreneurs Tawfiq Nasr Allah (left, standing) and Benoit Illy (right, sitting down) at Fairbrics' lab in Clichy, France.
Each year the world releases around 33 billion tons of carbon dioxide into the atmosphere. What if we could use this waste carbon dioxide to make shirts, dresses and hats? It sounds unbelievable. But two innovators are trying to tackle climate change in this truly unique way.
Chemist Tawfiq Nasr Allah set up Fairbrics with material scientist Benoît Illy in 2019. They're using waste carbon dioxide from industrial fumes as a raw material to create polyester, identical to the everyday polyester we use now. They want to take a new and very different approach to make the fashion industry more sustainable.
The Dark Side of Fast Fashion
The fashion industry is responsible for around 4% of global emissions. In a 2015 report, the MIT Materials Systems Laboratory predicted that the global impact of polyester fabric will grow from around 880 billion kg of CO2 in 2015 to 1.5 trillion kg of CO2 by 2030.
Professor Greg Peters, an expert in environmental science and sustainability, highlights the wide-ranging difficulties caused by the production of polyester. "Because it is made from petrochemical crude oil there is no real limit on how much polyester can be produced...You have to consider the ecological damage (oil spills, fracking etc.) caused by the oil and gas industry."
Many big-name brands have pledged to become carbon neutral by 2050. But nothing has really changed in the way polyester is produced.
Some companies are recycling plastic bottles into polyester. The plastic is melted into ultra-fine strands and then spun to create polyester. However, only a limited number of bottles are available. New materials must be added because of the amount of plastic degradation that takes place. Ultimately, recycling accounts for only a small percentage of the total amount of polyester produced.
Nasr Allah and Illy hope they can offer the solution the fashion industry is looking for. They are not just reducing the carbon emissions that are conventionally produced by making polyester. Their process actually goes much further. It's carbon negative and works by using up emissions from other industries.
"In a sense we imitate what nature does so well: plants capture CO2 and turn it into natural fibers using sunlight, we capture CO2 and turn it into synthetic fibers using electricity."
Experts in the field see a lot of promise. Dr Phil de Luna is an expert in carbon valorization -- the process of converting carbon dioxide into high-value chemicals. He leads a $57-million research program developing the technology to decarbonize Canada.
"I think the approach is great," he says. "Being able to take CO2 and then convert it into polymers or polyester is an excellent way to think about utilizing waste emissions and replacing fossil fuel-based materials. That is overall a net negative as compared to making polyester from fossil fuels."
From Harmful Waste to Useful Raw Material
It all started with Nasr Allah's academic research, primarily at the French Alternative Energies and Atomic Energy Commission (CEA). He spent almost 5 years investigating CO2 valorization. In essence, this involves breaking the bonds between the carbon and oxygen atoms in CO2 to create bonds with other elements.
Recycling carbon dioxide in this way requires extremely high temperatures and pressures. Catalysts are needed to break the strong bonds between the atoms. However, these are toxic, volatile and quickly lose their effectiveness over time. So, directly converting carbon dioxide into the raw material for making polyester fibers is very difficult.
Nasr Allah developed a process involving multiple simpler stages. His innovative approach involves converting carbon dioxide to intermediate chemicals. These chemicals can then be transformed into the raw material which is used in the production of polyester. After many experiments, Nasr Allah developed new processes and new catalysts that worked more effectively.
"We use a catalyst to transform CO2 into the chemicals that are used for polyester manufacturing," Illy says. "In a sense we imitate what nature does so well: plants capture CO2 and turn it into natural fibers using sunlight, we capture CO2 and turn it into synthetic fibers using electricity."
The Challenges Ahead
Nasr Allah met material scientist Illy through Entrepreneur First, a programme which pairs individuals looking to form technical start-ups. Together they set up Fairbrics and worked on converting Nasr Allah's lab findings into commercial applications and industrial success.
"The main challenge we faced was to scale up the process," Illy reveals. "[It had to be] consistent and safe to be carried out by a trained technician, not a specialist PhD as was the case in the beginning."
They recruited a team of scientists to help them develop a more effective and robust manufacturing process. Together, the team gained a more detailed theoretical understanding about what was happening at each stage of the chemical reactions. Eventually, they were able to fine tune the process and produce consistent batches of polyester.
They're making significant progress. They've produced their first samples and signed their first commercial contract to make polyester, which will then be both fabricated into clothes and sold by partner companies.
Currently, one of the largest challenges is financial. "We need to raise a fair amount to buy the equipment we need to produce at a large scale," Illy explains.
How to Power the Process?
At the moment, their main scientific focus is getting the process working reliably so they can begin commercialization. In order to remain sustainable and economically viable once they start producing polyester on a large scale, they need to consider the amount of energy they use for carbon valorization and the emissions they produce.
The more they optimize the way their catalyst works, the easier it will be to transform the CO2. The whole process can then become more cost effective and energy efficient.
De Luna explains: "My concern is...whether their process will be economical at scale. The problem is the energy cost to take carbon dioxide and transform it into these other products and that's where the science and innovation has to happen. [Whether they can scale up economically] depends on the performance of their catalyst."
They don't just need to think about the amount of energy they use to produce polyester; they also have to consider where this energy comes from.
"They need access to cheap renewable energy," De Luna says, "...so they're not using or emitting CO2 to do the conversion." If the energy they use to transform CO2 into polyester actually ends up producing more CO2, this will end up cancelling out their positive environmental impact.
Based in France, they're well located to address this issue. France has a clean electricity system, with only about 10% of their electric power coming from fossil fuels due to their reliance on nuclear energy and renewables.
Where Do They Get the Carbon Dioxide?
As they scale up, they also need to be able to access a source of CO2. They intend to obtain this from the steel industry, the cement industry, and hydrogen production.
The technology to purify and capture waste carbon dioxide from these industries is available on a large scale. However, there are only around 20 commercial operations in the world. The high cost of carbon capture means that development continues to be slow. There are a growing number of startups capturing carbon dioxide straight from the air, but this is even more costly.
One major problem is that storing captured carbon dioxide is expensive. "There are somewhat limited options for permanently storing captured CO2, so innovations like this are important,'' says T. Reed Miller, a researcher at the Yale University Center for Industrial Ecology.
Illy says: "The challenge is now to decrease the cost [of carbon capture]. By using CO2 as a raw material, we can try to increase the number of industries that capture CO2. Our goal is to turn CO2 from a waste into a valuable product."
Beyond Fashion
For Nasr Allah and Illy, fashion is just the beginning. There are many markets they can potentially break into. Next, they hope to use the polyester they've created in the packaging industry. Today, a lot of polyester is consumed to make bottles and jars. Illy believes that eventually they can produce many different chemicals from CO2. These chemicals could then be used to make paints, adhesives, and even plastics.
The Fairbrics scientists are providing a vital alternative to fossil fuels and showcasing the real potential of carbon dioxide to become a worthy resource instead of a harmful polluter.
Illy believes they can make a real difference through innovation: "We can have a significant impact in reducing climate change."
Vaccine passports, if required by businesses and universities, may give people a false sense of security, one expert cautions.
Vaccines are one of the greatest public health accomplishments of all time. For centuries, public health has relied on vaccinations to prevent and control disease outbreaks for a plethora of infectious scourges, with our crowning achievement being the successful eradication of smallpox.
The purpose of vaccine documentation is to provide proof of an individual's protection from either becoming infected or transmitting a vaccine-preventable disease. Vouching for these protections requires a firm knowledge about the epidemiology of the disease, as well as scientific knowledge concerning the efficacy of the vaccine. The vaccines we currently require be documented have met these tests; the vaccine for COVID-19 has not yet been proven to do so.
Let's acknowledge that the term "vaccine passport" is a poor choice of words. Passports are a legal travel document created by nations and governed by law for identification of the bearer to control entry and exit from nation states. They often serve as legal forms of identification and as a record of international travel. They are generally very sophisticated documents that have been created in a secure manner and may include a range of electronic and, in some cases, biometric measures such as fingerprints to ensure the holder is indeed who they say they are. Vaccine passports are medical documents used to document the vaccination status of an individual. They do not undergo the same level of administrative scrutiny and cannot be used to verify that the presenter is indeed the vaccinated individual. Some companies do have electronic methods to address concerns about verification; however, most people currently have paper records that can be easily falsified.
"Vaccine passports" as currently proposed risk giving people a false sense of security.
Successful disease control from vaccination programs relies on the ability to vaccinate at a level that prevents large-scale disease spread and the ability to rapidly identify the presence of disease outbreaks. It requires reliable, safe, and effective vaccines that are easily delivered in clinical and nonclinical settings. Keeping vaccination information as a part of the medical record, and even having a separate specialized vaccine record for personal use, is a time-honored tradition.
Keeping a vaccination record provides a method to keep track of the many shots one receives and serves as a visual reminder to help ensure the appropriate vaccine shot schedule is maintained for vaccines requiring multiple doses. The vaccine record, when combined with vaccine safety monitoring systems, serves as a mechanism to track adverse events to monitor and ensure the safety of vaccines as a consumer product. The record also serves as the official record of vaccination when required for administrative or legally prescribed purposes.
"Vaccine passports" as currently proposed risk giving people a false sense of security. In the case of the COVID-19 vaccines currently approved for use, many of the essential questions remain unanswered. While we do know the current three vaccines are highly protective against severe disease and death, and there is some evidence that these vaccinations do reduce infections and virus transmission of SARS-CoV-2, we do not yet know the full degree to which this occurs.
For example, we know there have been some cases of people that have been infected in close proximity to getting their full vaccination and rare cases of breakthrough reinfections. A breakthrough infection in a restaurant is a challenge for contact tracing, but an outbreak from a movie theater exposure or a baseball game could spark a major outbreak at our current level of vaccination. Current CDC guidance recommends continued mask wearing in order to address these concerns.
We also do not yet know how long the protections will last and if or when a booster or revaccination is required. In effect, it is too soon to know. Should an annual booster shot be required, then a vaccine passport would require annual updating, a process more frequent than renewal of a driver's license.
We also know that the current SARS-CoV-2 virus is mutating briskly. While the current approved vaccines have remained effective overall, there is evidence of some degree of degradation in vaccine effectiveness against some of the circulating strains. We also have sparse data on many of the other emerging strains of concern because we have not had the surveillance capacity in the U.S. to gain an adequate sense of how the virus is changing to fully align vaccine effectiveness with viral capabilities.
The risk of people misusing these "passports" is troubling. The potential for using these documents for hiring, firing or job limitation is a serious concern. Unvaccinated workers are at risk of this form of discrimination even from well-meaning employers or supervisors. Health insurers are prohibited by the Affordable Care Act from discriminating based on preexisting conditions, but they could probably charge a higher premium for unvaccinated individuals. There also is a risk of stigmatizing individuals who are not vaccinated or have left their vaccine documentation at home. Another concern: the opportunity to discriminate based on race, gender, sexual orientation, or religion, using one's vaccination status as an excuse.
These "passports" are being discussed as a "ticket verification" for entry to many activities, including dining at restaurants, flying domestically and/or internationally, going to movie theaters and sporting events, etc. These are all activities we already are doing at reduced levels and for which wearing a mask, hand hygiene and physical distancing are effective disease control practices. COVID-19 vaccines are indeed the measure that will make the ability to totally reopen our society complete, but we are not there yet. Documentation of one's COVID-19 vaccine status may be useful in selected situations in the future. That remains to be seen.
Finally, inadequate vaccine supply and disparities in vaccine delivery have created enormous challenges in providing equal access to vaccination. Also, the amount of misinformation, disinformation, and lingering vaccine hesitancy continue to limit the speed at which we will reach the level of vaccination of the population that would make this documentation meaningful. The requirement for "vaccine passports" is already alienating people who are opposed to vaccinations for a variety of reasons, paradoxically risking reduced vaccine uptake. This politicization of the vaccination effort is of concern. There are indeed people who, due to medical contraindications or legal exemptions, will not be vaccinated, and we do not yet have a national framework on how to address this.
Vaccine passports are not the solution for reopening our society — a robust vaccination program is. The requirement to document one's vaccination status for COVID-19 may one day have its place. For now, it is an idea whose time has not yet come.
Editor's Note: This op/ed is part of a "Big Question" series on the ethics of vaccine passports. Read the flip side argument here.