The First Cloned Monkeys Provoked More Shrugs Than Shocks

Zhong Zhong and Hua Hua, the two cloned macaques.
A few months ago, it was announced that not one, but two healthy long-tailed macaque monkeys were cloned—a first for primates of any kind. The cells were sourced from aborted monkey fetuses and the DNA transferred into eggs whose nuclei had been removed, the same method that was used in 1996 to clone "Dolly the Sheep." Two live births, females named Zhong Zhong and Hua Hua, resulted from 60 surrogate mothers. Inefficient, it's true. But over time, the methods are likely to be improved.
The scientist who supervised the project predicts that cloning, along with gene editing, will result in "ideal primate models" for studying disease mechanisms and drug screening.
Dr. Gerald Schatten, a famous would-be monkey cloner, authored a controversial paper in 2003 describing the formidable challenges to cloning monkeys and humans, speculating that the feat might never be accomplished. Now, some 15 years later, that prediction, insofar as it relates to monkeys, has blown away.
Zhong Zhong and Hua Hua were created at the Chinese Academy of Science's Institute of Neuroscience in Shanghai. The Institute founded in 1999 boasts 32 laboratories, expanding to 50 labs in 2020. It maintains two non-human primate research facilities.
The founder and director, Dr. Mu-ming Poo, supervised the project. Poo is an extremely accomplished senior researcher at the pinnacle of his field, a distinguished professor emeritus in Biology at UC Berkeley. In 2016, he was awarded the prestigious $500,000 Gruber Neuroscience Prize. At that time, Poo's experiments were described by a colleague as being "innovative and very often ingenious."
Poo maintains the reputation of studying some of the most important questions in cellular neuroscience.
But is society ready to accept cloned primates for medical research without the attendant hysteria about fears of cloned humans?
By Western standards, use of non-human primates in research focuses on the welfare of the animal subjects. As PETA reminds us, there is a dreadful and sad history of mistreatment. Dr. Poo assures us that his cloned monkeys are treated ethically and that the Institute is compliant with the highest regulatory standards, as promulgated by the U.S. National Institutes of Health.
He presents the noblest justifications for the research. He predicts that cloning, along with gene editing, will result in "ideal primate models" for studying disease mechanisms and drug screening. He declares that this will eventually help to solve Parkinson's, Huntington's and Alzheimer's disease.
But is society ready to accept cloned primates for medical research without the attendant hysteria about fears of cloned humans? It appears so.
While much of the news coverage expressed this predictable worry, my overall impression is that the societal response was muted. Where was the expected outrage? Then again, we've come a long way since Dolly the Sheep in terms of both the science and the cultural acceptance of cloning. Perhaps my unique vantage point can provide perspective on how much attitudes have evolved.
Perhaps my unique vantage point can provide perspective on how much attitudes have evolved.
I sometimes joke that I am the world's only human cloning lawyer—a great gig but there are still no clients.
I first crashed into the cloning scene in 2002 when I sued the so-called human cloning company "Clonaid" and asked in court to have a temporary guardian appointed for the alleged first human clone "Baby Eve." The claim needed to be tested, and mine was the first case ever aiming to protect the rights of a human clone. My legal basis was child welfare law, protecting minors from abuse, negligence, and exploitation.
The case had me on back-to-back global television broadcasts around the world; there was live news and "breathless" coverage at the courthouse emblazoned in headlines in every language on the planet. Cloning was, after all, perceived as a species-altering event: asexual reproduction. The controversy dominated world headlines for month until Clonaid's claim was busted as the "fakest" of fake news.
Fresh off the cloning case, the scientific community reached out to me, seeing me as the defender of legitimate science, an opponent of cloning human babies but a proponent of using cloning techniques to accelerate ethical regenerative medicine and embryonic stem cell research in general.
The years 2003 to 2006 were the era of the "stem cell wars" and a dominant issue was human cloning. Social conservative lawmakers around the world were seeking bans or criminalization not only of cloning babies but also the cloning of cells to match the donor's genetics. Scientists were being threatened with fines and imprisonment. Human cloning was being challenged in the United Nations with the United States backing a global treaty to ban and morally condemn all cloning -- including the technique that was crucial for research.
Scientists and patients were touting the cloning technique as a major biomedical breakthrough because cells could be created as direct genetic matches from a specific donor.
At the same time, scientists and patients were touting the cloning technique as a major biomedical breakthrough because cells could be created as direct genetic matches from a specific donor.
So my organization organized a conference at UN headquarters to defend research cloning and all the big names in stem cell research were there. We organized petitions to the UN and faxed 35,000 signatures to the country mission. These ongoing public policy battles were exacerbated in part because of the growing fear that cloning babies was just around the corner.
Then in 2005, the first cloned dog stunned the world, an Afghan hound named Snuppy. I met him when I visited the laboratories of Professor Woo Suk Hwang in Korea. His minders let me hold his leash -- TIME magazine's scientific breakthrough of the year. He didn't lick me or even wag his tail; I figured he must not like lawyers.
Tragically, soon thereafter, I witnessed firsthand Dr. Hwang's fall from grace when his human stem cell cloning breakthroughs proved false. The massive scientific misconduct rocked the nation of Korea, stem cell science in general, and provoked terrible news coverage.
Nevertheless, by 2007, the proposed bans lost steam, overridden by the advent of a Japanese researcher's Nobel Prize winning formula for reprogramming human cells to create genetically matched cell lines, not requiring the destruction of human embryos.
After years of panic, none of the recent cloning headlines has caused much of a stir.
Five years later, when two American scientists accomplished therapeutic human cloned stem cell lines, their news was accepted without hysteria. Perhaps enough time had passed since Hwang and the drama was drained.
In the just past 30 days we have seen more cloning headlines. Another cultural icon, Barbara Streisand, revealed she owns two cloned Coton de Tulear puppies. The other weekend, the television news show "60 Minutes" devoted close to an hour on the cloned ponies used at the top level of professional polo. And in India, scientists just cloned the first Assamese buffalo.
And you know what? After years of panic, none of this has caused much of a stir. It's as if the future described by Alvin Toffler in "Future Shock" has arrived and we are just living with it. A couple of cloned monkeys barely move the needle.
Perhaps it is the advent of the Internet and the overall dilution of wonder and outrage. Or maybe the muted response is rooted in popular culture. From Orphan Black to the plotlines of dozens of shows and books, cloning is just old news. The hand-wringing discussions about "human dignity" and "slippery slopes" have taken a backseat to the AI apocalypse and Martian missions.
We humans are enduring plagues of dementia and Alzheimer's, and we will need more monkeys. I will take mine cloned, if it will speed progress.
Personally, I still believe that cloned children should not be an option. Child welfare laws might be the best deterrent.
The same does not hold for cloning monkey research subjects. Squeamishness aside, I think Zhong Zhong and Hua Hua will soon be joined by a legion of cloned macaques and probably marmosets.
We humans are enduring plagues of dementia and Alzheimer's, and we will need more monkeys. I will take mine cloned, if it will speed the mending of these consciousness-destroying afflictions.
Scientific revolutions once took centuries, then decades, and now seem to bombard us daily. The convergence of technologies has accelerated the future. To Zhong Zhong and Hua Hua, my best wishes with the hope that their sacrifices will contribute to the health of all primates -- not just humans.
Urinary tract infections account for more than 8 million trips to the doctor each year.
Few things are more painful than a urinary tract infection (UTI). Common in men and women, these infections account for more than 8 million trips to the doctor each year and can cause an array of uncomfortable symptoms, from a burning feeling during urination to fever, vomiting, and chills. For an unlucky few, UTIs can be chronic—meaning that, despite treatment, they just keep coming back.
But new research, presented at the European Association of Urology (EAU) Congress in Paris this week, brings some hope to people who suffer from UTIs.
Clinicians from the Royal Berkshire Hospital presented the results of a long-term, nine-year clinical trial where 89 men and women who suffered from recurrent UTIs were given an oral vaccine called MV140, designed to prevent the infections. Every day for three months, the participants were given two sprays of the vaccine (flavored to taste like pineapple) and then followed over the course of nine years. Clinicians analyzed medical records and asked the study participants about symptoms to check whether any experienced UTIs or had any adverse reactions from taking the vaccine.
The results showed that across nine years, 48 of the participants (about 54%) remained completely infection-free. On average, the study participants remained infection free for 54.7 months—four and a half years.
“While we need to be pragmatic, this vaccine is a potential breakthrough in preventing UTIs and could offer a safe and effective alternative to conventional treatments,” said Gernot Bonita, Professor of Urology at the Alta Bro Medical Centre for Urology in Switzerland, who is also the EAU Chairman of Guidelines on Urological Infections.
The news comes as a relief not only for people who suffer chronic UTIs, but also to doctors who have seen an uptick in antibiotic-resistant UTIs in the past several years. Because UTIs usually require antibiotics, patients run the risk of developing a resistance to the antibiotics, making infections more difficult to treat. A preventative vaccine could mean less infections, less antibiotics, and less drug resistance overall.
“Many of our participants told us that having the vaccine restored their quality of life,” said Dr. Bob Yang, Consultant Urologist at the Royal Berkshire NHS Foundation Trust, who helped lead the research. “While we’re yet to look at the effect of this vaccine in different patient groups, this follow-up data suggests it could be a game-changer for UTI prevention if it’s offered widely, reducing the need for antibiotic treatments.”
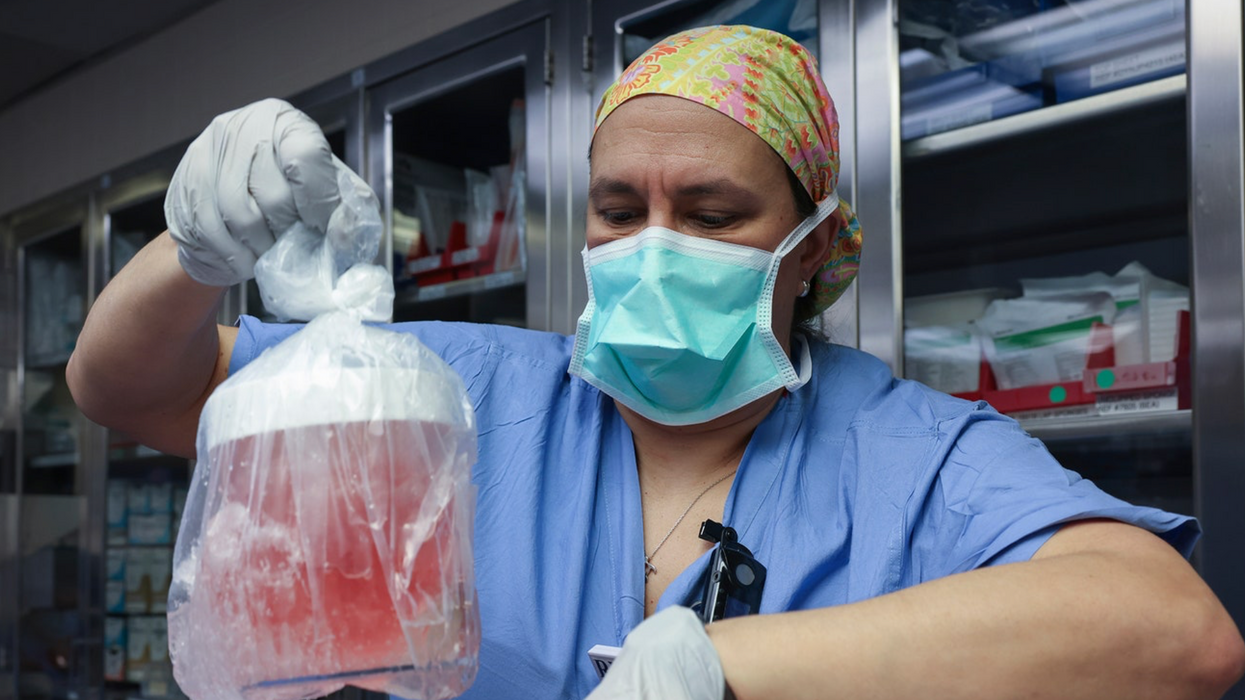
MILESTONE: Doctors have transplanted a pig organ into a human for the first time in history
A surgeon at Massachusetts General Hospital prepares a pig organ for transplant.
Surgeons at Massachusetts General Hospital made history last week when they successfully transplanted a pig kidney into a human patient for the first time ever.
The recipient was a 62-year-old man named Richard Slayman who had been living with end-stage kidney disease caused by diabetes. While Slayman had received a kidney transplant in 2018 from a human donor, his diabetes ultimately caused the kidney to fail less than five years after the transplant. Slayman had undergone dialysis ever since—a procedure that uses an artificial kidney to remove waste products from a person’s blood when the kidneys are unable to—but the dialysis frequently caused blood clots and other complications that landed him in the hospital multiple times.
As a last resort, Slayman’s kidney specialist suggested a transplant using a pig kidney provided by eGenesis, a pharmaceutical company based in Cambridge, Mass. The highly experimental surgery was made possible with the Food and Drug Administration’s “compassionate use” initiative, which allows patients with life-threatening medical conditions access to experimental treatments.
The new frontier of organ donation
Like Slayman, more than 100,000 people are currently on the national organ transplant waiting list, and roughly 17 people die every day waiting for an available organ. To make up for the shortage of human organs, scientists have been experimenting for the past several decades with using organs from animals such as pigs—a new field of medicine known as xenotransplantation. But putting an animal organ into a human body is much more complicated than it might appear, experts say.
“The human immune system reacts incredibly violently to a pig organ, much more so than a human organ,” said Dr. Joren Madsen, director of the Mass General Transplant Center. Even with immunosuppressant drugs that suppress the body’s ability to reject the transplant organ, Madsen said, a human body would reject an animal organ “within minutes.”
So scientists have had to use gene-editing technology to change the animal organs so that they would work inside a human body. The pig kidney in Slayman’s surgery, for instance, had been genetically altered using CRISPR-Cas9 technology to remove harmful pig genes and add human ones. The kidney was also edited to remove pig viruses that could potentially infect a human after transplant.
With CRISPR technology, scientists have been able to prove that interspecies organ transplants are not only possible, but may be able to successfully work long term, too. In the past several years, scientists were able to transplant a pig kidney into a monkey and have the monkey survive for more than two years. More recently, doctors have transplanted pig hearts into human beings—though each recipient of a pig heart only managed to live a couple of months after the transplant. In one of the patients, researchers noted evidence of a pig virus in the man’s heart that had not been identified before the surgery and could be a possible explanation for his heart failure.
So far, so good
Slayman and his medical team ultimately decided to pursue the surgery—and the risk paid off. When the pig organ started producing urine at the end of the four-hour surgery, the entire operating room erupted in applause.
Slayman is currently receiving an infusion of immunosuppressant drugs to prevent the kidney from being rejected, while his doctors monitor the kidney’s function with frequent ultrasounds. Slayman is reported to be “recovering well” at Massachusetts General Hospital and is expected to be discharged within the next several days.