Top Fertility Doctor: Artificially Created Sperm and Eggs "Will Become Normal" One Day
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
A rendering of in vitro fertilization.
Imagine two men making a baby. Or two women. Or an infertile couple. Or an older woman whose eggs are no longer viable. None of these people could have a baby today without the help of an egg or sperm donor.
Cells scraped from the inside of your cheek could one day be manipulated to become either eggs or sperm.
But in the future, it may be possible for them to reproduce using only their own genetic material, thanks to an emerging technology called IVG, or in vitro gametogenesis.
Researchers are learning how to reprogram adult human cells like skin cells to become lab-created egg and sperm cells, which could then be joined to form an embryo. In other words, cells scraped from the inside of your cheek could one day be manipulated to become either eggs or sperm, no matter your gender or your reproductive fitness.
In 2016, Japanese scientists proved that the concept could be successfully carried out in mice. Now some experts, like Dr. John Zhang, the founder and CEO of New Hope Fertility Center in Manhattan, say it's just "a matter of time" before the method is also made to work in humans.
Such a technological tour de force would upend our most basic assumptions about human reproduction and biology. Combined with techniques like gene editing, these tools could eventually enable prospective parents to have an unprecedented level of choice and control over their children's origins. It's a wildly controversial notion, and an especially timely one now that a Chinese scientist has announced the birth of the first allegedly CRISPR-edited babies. (The claims remain unverified.)
Zhang himself is no stranger to controversy. In 2016, he stunned the world when he announced the birth of a baby conceived using the DNA of three people, a landmark procedure intended to prevent the baby from inheriting a devastating neurological disease. (Zhang went to a clinic in Mexico to carry out the procedure because it is prohibited in the U.S.) Zhang's other achievements to date include helping a 49-year-old woman have a baby using her own eggs and restoring a young woman's fertility through an ovarian tissue transplant surgery.
Zhang recently sat down with our Editor-in-Chief in his New York office overlooking Columbus Circle to discuss the fertility world's latest provocative developments. Here are his top ten insights:
Clearly [gene-editing embryos] will be beneficial to mankind, but it's a matter of how and when the work is done.
1) On a Chinese scientist's claim of creating the first CRISPR-edited babies:
I'm glad that we made a first move toward a clinical application of this technology for mankind. Somebody has to do this. Whether this was a good case or not, there is still time to find out.
Clearly it will be beneficial to mankind, but it's a matter of how and when the work is done. Like any scientific advance, it has to be done in a very responsible way.
Today's response is identical to when the world's first IVF baby was announced in 1978. The major news media didn't take it seriously and thought it was evil, wanted to keep a distance from IVF. Many countries even abandoned IVF, but today you see it is a normal practice. And it took almost 40 years [for the researchers] to win a Nobel Prize.
I think we need more time to understand how this work was done medically, ethically, and let the scientist have the opportunity to present how it was done and let a scientific journal publish the paper. Before these become available, I don't think we should start being upset, scared, or giving harsh criticism.
2) On the international outcry in response to the news:
I feel we are in scientific shock, with many thinking it came too fast, too soon. We all embrace modern technology, but when something really comes along, we fear it. In an old Chinese saying, one of the masters always dreamed of seeing the dragon, and when the dragon really came, he got scared.

Dr. John Zhang, the founder and CEO of New Hope Fertility Center in Manhattan, pictured in his office.
3) On the Western world's perception that Chinese scientists sometimes appear to discount ethics in favor of speedy breakthroughs:
I think this perception is not fair. I don't think China is very casual. It's absolutely not what people think. I don't want people to feel that this case [of CRISPR-edited babies] will mean China has less standards over how human reproduction should be performed. Just because this happened, it doesn't mean in China you can do anything you want.
As far as the regulation of IVF clinics, China is probably the most strictly regulated of any country I know in this world.
4) On China's first public opinion poll gauging attitudes toward gene-edited babies, indicating that more than 60 percent of survey respondents supported using the technology to prevent inherited diseases, but not to enhance traits:
There is a sharp contrast between the general public and the professional world. Being a working health professional and an advocate of scientists working in this field, it is very important to be ethically responsible for what we are doing, but my own feeling is that from time to time we may not take into consideration what the patient needs.
5) On how the three-parent baby is doing today, several years after his birth:
No news is good news.
6) On the potentially game-changing research to develop artificial sperm and eggs:
First of all I think that anything that's technically possible, as long as you are not harmful to other people, to other societies, as long as you do it responsibly, and this is a legitimate desire, I think eventually it will become reality.
My research for now is really to try to overcome the very next obstacle in our field, which is how to let a lady age 44 or older have a baby with her own genetic material.
Practically 99 percent of women over age 43 will never make a baby on their own. And after age 47, we usually don't offer donor egg IVF anymore.
But with improved longevity, and quality of life, the lifespan of females continues to increase. In Japan, the average for females is about 89 years old. So for more than half of your life, you will not be able to produce a baby, which is quite significant in the animal kingdom. In most of the animal kingdom, their reproductive life is very much the same as their life, but then you can argue in the animal kingdom unlike a human being, it doesn't take such a long time for them to contribute to the society because once you know how to hunt and look for food, you're done.
"I think this will become a major ethical debate: whether we should let an older lady have a baby at a very late state of her life."
But humans are different. You need to go to college, get certain skills. It takes 20 years to really bring a human being up to become useful to society. That's why the mom and dad are not supposed to have the same reproductive life equal to their real life.
I think this will become a major ethical debate: whether we should let an older lady have a baby at a very late state of her life and leave the future generation in a very vulnerable situation in which they may lack warm caring, proper guidance, and proper education.
7) On using artificial gametes to grant more reproductive choices to gays and lesbians:
I think it is totally possible to have two sperm make a baby, and two eggs make babies.
If we have two guys, one guy to produce eggs, or two girls, one would have to become sperm. Basically you are creating artificial gametes or converting with gametes from sperm to become egg or egg to become a sperm. Which may not necessarily be very difficult. The key is to be able to do nuclear reprogramming.
So why can two sperm not make offspring now? You get exactly half of your genes from each parent. The genes have their own imprinting that say "made in mom," "made in dad." The two sperm would say "made in dad," "made in dad." If I can erase the "made in dad," and say "made in mom," then these sperm can make offspring.
8) On how close science is to creating artificial gametes for clinical use in pregnancies:
It's very hard to say until we accomplish it. It could be very quick. It could be it takes a long time. I don't want to speculate.
"I think these technologies are the solid foundation just like when we designed the computer -- we never thought a computer would become the iPhone."
9) On whether there should be ethical red lines drawn by authorities or whether the decisions should be left to patients and scientists:
I think we cannot believe a hundred percent in the scientist and the patient but it should not be 100 percent authority. It should be coming from the whole of society.
10) On his expectations for the future:
We are living in a very exciting world. I think that all these technologies can really change the way of mankind and also are not just for baby-making. The research, the experience, the mechanism we learn from these technologies, they will shine some great lights into our long-held dream of being a healthy population that is cancer-free and lives a long life, let's say 120 years.
I think these technologies are the solid foundation just like when we designed the computer -- we never thought a computer would become the iPhone. Imagine making a computer 30 years ago, that this little chip will change your life.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
Jamie Rettinger with his now fiance Amie Purnel-Davis, who helped him through the clinical trial.
Jamie Rettinger was still in his thirties when he first noticed a tiny streak of brown running through the thumbnail of his right hand. It slowly grew wider and the skin underneath began to deteriorate before he went to a local dermatologist in 2013. The doctor thought it was a wart and tried scooping it out, treating the affected area for three years before finally removing the nail bed and sending it off to a pathology lab for analysis.
"I have some bad news for you; what we removed was a five-millimeter melanoma, a cancerous tumor that often spreads," Jamie recalls being told on his return visit. "I'd never heard of cancer coming through a thumbnail," he says. None of his doctors had ever mentioned it either. "I just thought I was being treated for a wart." But nothing was healing and it continued to bleed.
A few months later a surgeon amputated the top half of his thumb. Lymph node biopsy tested negative for spread of the cancer and when the bandages finally came off, Jamie thought his medical issues were resolved.
Melanoma is the deadliest form of skin cancer. About 85,000 people are diagnosed with it each year in the U.S. and more than 8,000 die of the cancer when it spreads to other parts of the body, according to the Centers for Disease Control and Prevention (CDC).
There are two peaks in diagnosis of melanoma; one is in younger women ages 30-40 and often is tied to past use of tanning beds; the second is older men 60+ and is related to outdoor activity from farming to sports. Light-skinned people have a twenty-times greater risk of melanoma than do people with dark skin.
"When I graduated from medical school, in 2005, melanoma was a death sentence" --Diwakar Davar.
Jamie had a follow up PET scan about six months after his surgery. A suspicious spot on his lung led to a biopsy that came back positive for melanoma. The cancer had spread. Treatment with a monoclonal antibody (nivolumab/Opdivo®) didn't prove effective and he was referred to the UPMC Hillman Cancer Center in Pittsburgh, a four-hour drive from his home in western Ohio.
An alternative monoclonal antibody treatment brought on such bad side effects, diarrhea as often as 15 times a day, that it took more than a week of hospitalization to stabilize his condition. The only options left were experimental approaches in clinical trials.
Early research
"When I graduated from medical school, in 2005, melanoma was a death sentence" with a cure rate in the single digits, says Diwakar Davar, 39, an oncologist at UPMC Hillman Cancer Center who specializes in skin cancer. That began to change in 2010 with introduction of the first immunotherapies, monoclonal antibodies, to treat cancer. The antibodies attach to PD-1, a receptor on the surface of T cells of the immune system and on cancer cells. Antibody treatment boosted the melanoma cure rate to about 30 percent. The search was on to understand why some people responded to these drugs and others did not.
At the same time, there was a growing understanding of the role that bacteria in the gut, the gut microbiome, plays in helping to train and maintain the function of the body's various immune cells. Perhaps the bacteria also plays a role in shaping the immune response to cancer therapy.
One clue came from genetically identical mice. Animals ordered from different suppliers sometimes responded differently to the experiments being performed. That difference was traced to different compositions of their gut microbiome; transferring the microbiome from one animal to another in a process known as fecal transplant (FMT) could change their responses to disease or treatment.
When researchers looked at humans, they found that the patients who responded well to immunotherapies had a gut microbiome that looked like healthy normal folks, but patients who didn't respond had missing or reduced strains of bacteria.
Davar and his team knew that FMT had a very successful cure rate in treating the gut dysbiosis of Clostridioides difficile, a persistant intestinal infection, and they wondered if a fecal transplant from a patient who had responded well to cancer immunotherapy treatment might improve the cure rate of patients who did not originally respond to immunotherapies for melanoma.
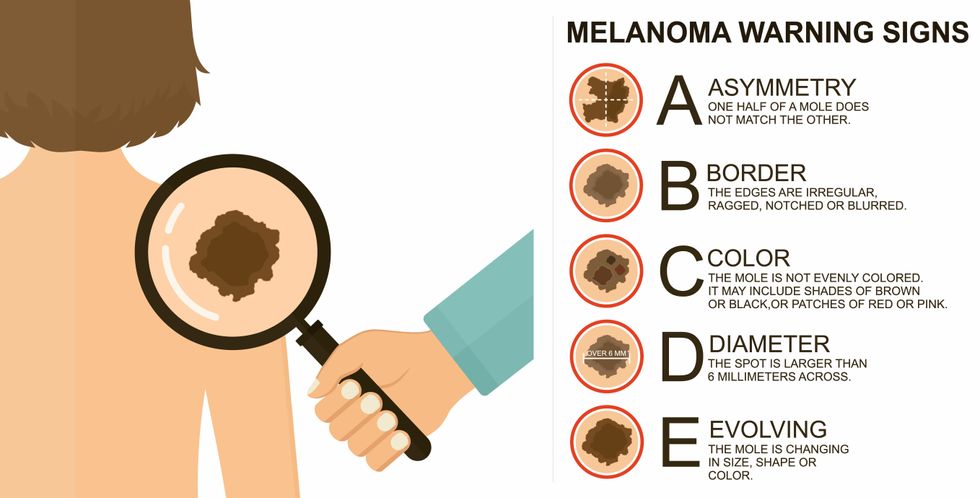
The ABCDE of melanoma detection
Adobe Stock
Clinical trial
"It was pretty weird, I was totally blasted away. Who had thought of this?" Jamie first thought when the hypothesis was explained to him. But Davar's explanation that the procedure might restore some of the beneficial bacterial his gut was lacking, convinced him to try. He quickly signed on in October 2018 to be the first person in the clinical trial.
Fecal donations go through the same safety procedures of screening for and inactivating diseases that are used in processing blood donations to make them safe for transfusion. The procedure itself uses a standard hollow colonoscope designed to screen for colon cancer and remove polyps. The transplant is inserted through the center of the flexible tube.
Most patients are sedated for procedures that use a colonoscope but Jamie doesn't respond to those drugs: "You can't knock me out. I was watching them on the TV going up my own butt. It was kind of unreal at that point," he says. "There were about twelve people in there watching because no one had seen this done before."
A test two weeks after the procedure showed that the FMT had engrafted and the once-missing bacteria were thriving in his gut. More importantly, his body was responding to another monoclonal antibody (pembrolizumab/Keytruda®) and signs of melanoma began to shrink. Every three months he made the four-hour drive from home to Pittsburgh for six rounds of treatment with the antibody drug.
"We were very, very lucky that the first patient had a great response," says Davar. "It allowed us to believe that even though we failed with the next six, we were on the right track. We just needed to tweak the [fecal] cocktail a little better" and enroll patients in the study who had less aggressive tumor growth and were likely to live long enough to complete the extensive rounds of therapy. Six of 15 patients responded positively in the pilot clinical trial that was published in the journal Science.
Davar believes they are beginning to understand the biological mechanisms of why some patients initially do not respond to immunotherapy but later can with a FMT. It is tied to the background level of inflammation produced by the interaction between the microbiome and the immune system. That paper is not yet published.
Surviving cancer
It has been almost a year since the last in his series of cancer treatments and Jamie has no measurable disease. He is cautiously optimistic that his cancer is not simply in remission but is gone for good. "I'm still scared every time I get my scans, because you don't know whether it is going to come back or not. And to realize that it is something that is totally out of my control."
"It was hard for me to regain trust" after being misdiagnosed and mistreated by several doctors he says. But his experience at Hillman helped to restore that trust "because they were interested in me, not just fixing the problem."
He is grateful for the support provided by family and friends over the last eight years. After a pause and a sigh, the ruggedly built 47-year-old says, "If everyone else was dead in my family, I probably wouldn't have been able to do it."
"I never hesitated to ask a question and I never hesitated to get a second opinion." But Jamie acknowledges the experience has made him more aware of the need for regular preventive medical care and a primary care physician. That person might have caught his melanoma at an earlier stage when it was easier to treat.
Davar continues to work on clinical studies to optimize this treatment approach. Perhaps down the road, screening the microbiome will be standard for melanoma and other cancers prior to using immunotherapies, and the FMT will be as simple as swallowing a handful of freeze-dried capsules off the shelf rather than through a colonoscopy. Earlier this year, the Food and Drug Administration approved the first oral fecal microbiota product for C. difficile, hopefully paving the way for more.
An older version of this hit article was first published on May 18, 2021
All organisms can repair damaged tissue, but none do it better than salamanders and newts. A surprising area of science could tell us how they manage this feat - and perhaps even help us develop a similar ability.
All organisms have the capacity to repair or regenerate tissue damage. None can do it better than salamanders or newts, which can regenerate an entire severed limb.
That feat has amazed and delighted man from the dawn of time and led to endless attempts to understand how it happens – and whether we can control it for our own purposes. An exciting new clue toward that understanding has come from a surprising source: research on the decline of cells, called cellular senescence.
Senescence is the last stage in the life of a cell. Whereas some cells simply break up or wither and die off, others transition into a zombie-like state where they can no longer divide. In this liminal phase, the cell still pumps out many different molecules that can affect its neighbors and cause low grade inflammation. Senescence is associated with many of the declining biological functions that characterize aging, such as inflammation and genomic instability.
Oddly enough, newts are one of the few species that do not accumulate senescent cells as they age, according to research over several years by Maximina Yun. A research group leader at the Center for Regenerative Therapies Dresden and the Max Planck Institute of Molecular and Cell Biology and Genetics, in Dresden, Germany, Yun discovered that senescent cells were induced at some stages of regeneration of the salamander limb, “and then, as the regeneration progresses, they disappeared, they were eliminated by the immune system,” she says. “They were present at particular times and then they disappeared.”
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states.
Previous research on senescence in aging had suggested, logically enough, that applying those cells to the stump of a newly severed salamander limb would slow or even stop its regeneration. But Yun stood that idea on its head. She theorized that senescent cells might also play a role in newt limb regeneration, and she tested it by both adding and removing senescent cells from her animals. It turned out she was right, as the newt limbs grew back faster than normal when more senescent cells were included.
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states, which could then be turned into progenitors, a cell type in between stem cells and specialized cells, needed to regrow the muscle tissue of the missing limb. “We think that this ability to dedifferentiate is intrinsically a big part of why salamanders can regenerate all these very complex structures, which other organisms cannot,” she explains.
Yun sees regeneration as a two part problem. First, the cells must be able to sense that their neighbors from the lost limb are not there anymore. Second, they need to be able to produce the intermediary progenitors for regeneration, , to form what is missing. “Molecularly, that must be encoded like a 3D map,” she says, otherwise the new tissue might grow back as a blob, or liver, or fin instead of a limb.
Wound healing
Another recent study, this time at the Mayo Clinic, provides evidence supporting the role of senescent cells in regeneration. Looking closely at molecules that send information between cells in the wound of a mouse, the researchers found that senescent cells appeared near the start of the healing process and then disappeared as healing progressed. In contrast, persistent senescent cells were the hallmark of a chronic wound that did not heal properly. The function and significance of senescence cells depended on both the timing and the context of their environment.
The paper suggests that senescent cells are not all the same. That has become clearer as researchers have been able to identify protein markers on the surface of some senescent cells. The patterns of these proteins differ for some senescent cells compared to others. In biology, such physical differences suggest functional differences, so it is becoming increasingly likely there are subsets of senescent cells with differing functions that have not yet been identified.
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes.
Scientists initially thought that senescent cells couldn’t play a role in regeneration because they could no longer reproduce, says Anthony Atala, a practicing surgeon and bioengineer who leads the Wake Forest Institute for Regenerative Medicine in North Carolina. But Yun’s study points in the other direction. “What this paper shows clearly is that these cells have the potential to be involved in tissue regeneration [in newts]. The question becomes, will these cells be able to do the same in humans.”
As our knowledge of senescent cells increases, Atala thinks we need to embrace a new analogy to help understand them: humans in retirement. They “have acquired a lot of wisdom throughout their whole life and they can help younger people and mentor them to grow to their full potential. We're seeing the same thing with these cells,” he says. They are no longer putting energy into their own reproduction, but the signaling molecules they secrete “can help other cells around them to regenerate.”
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes. If so, it seems that our genes are unable to express this ability, perhaps as part of a tradeoff in acquiring other traits. It is a fertile area of research.
Dedifferentiation is likely to become an important process in the field of regenerative medicine. One extreme example: a lab has been able to turn back the clock and reprogram adult male skin cells into female eggs, a potential milestone in reproductive health. It will be more difficult to control just how far back one wishes to go in the cell's dedifferentiation – part way or all the way back into a stem cell – and then direct it down a different developmental pathway. Yun is optimistic we can learn these tricks from newts.
Senolytics
A growing field of research is using drugs called senolytics to remove senescent cells and slow or even reverse disease of aging.
“Senolytics are great, but senolytics target different types of senescence,” Yun says. “If senescent cells have positive effects in the context of regeneration, of wound healing, then maybe at the beginning of the regeneration process, you may not want to take them out for a little while.”
“If you look at pretty much all biological systems, too little or too much of something can be bad, you have to be in that central zone” and at the proper time, says Atala. “That's true for proteins, sugars, and the drugs that you take. I think the same thing is true for these cells. Why would they be different?”
Our growing understanding that senescence is not a single thing but a variety of things likely means that effective senolytic drugs will not resemble a single sledge hammer but more a carefully manipulated scalpel where some types of senescent cells are removed while others are added. Combinations and timing could be crucial, meaning the difference between regenerating healthy tissue, a scar, or worse.

