Virtual Clinical Trials Are Letting More People of Color Participate in Research

Virtual clinical trials are helping to eradicate logistical barriers to clinical trial participation, though trust is still an issue.
Herman Taylor, director of the cardiovascular research institute at Morehouse college, got in touch with UnitedHealth Group early in the pandemic.
The very people who most require solutions to COVID are those who are least likely to be involved in the search to find them.
A colleague he worked with at Grady Hospital in Atlanta was the guy when it came to studying sickle cell disease, a recessive genetic disorder that causes red blood cells to harden into half-moon shapes, causing cardiovascular problems. Sickle cell disease is more common in African Americans than it is in Caucasians, in part because having just one gene for the disease, called sickle cell trait, is protective against malaria, which is endemic to much of Africa. Roughly one in 12 African Americans carry sickle cell trait, and Taylor's colleague wondered if this could be one factor affecting differential outcomes for COVID-19.
UnitedHealth Group granted Taylor and his colleague the money to study sickle cell trait in COVID, and then, as they continued working together, they began to ask Taylor his opinion on other topics. As an insurance company, United had realized early in the pandemic that it was sitting on a goldmine of patient data—some 120 million patients' worth—that it could sift through to look for potential COVID treatments.
Their researchers thought they had found one: In a small subset of 14,000 people who'd contracted COVID, there was a group whose bills were paid by Medicare (which the researchers took as a proxy for older age). The people in this group who were taking ACE inhibitors, blood vessel dilators often used to treat high blood pressure, were 40 percent less likely to be hospitalized than those who were not taking the drug.
The connection between ACE inhibitors and COVID hospitalizations was a correlation, a statistical association. To determine whether the drugs had any real effect on COVID outcomes, United would have to perform another, more rigorous study. They would have to assign some people to receive small doses of ACE inhibitors, and others to receive placebos, and measure the outcomes under each condition. They planned to do this virtually, allowing study participants to sign up and be screened online, and sending drugs, thermometers, and tests through the mail. There were two reasons to do it this way: First, the U.S. Food and Drug Administration had been advising medical researchers to embrace new strategies in clinical trials as a way to protect participants during the pandemic.
The second reason was why they asked Herman Taylor to co-supervise it: Clinical trials have long had a diversity problem. And going virtual is a potential solution.
Since the beginning of the pandemic, COVID-19 has infected people of color at a rate of three times that of Caucasians (killing Black people at a rate 2.5 times as high, and Hispanic and American Indian or Alaska Native people at a rate 1.3 times as high). A number of explanations have been put forth to explain this disproportionate toll. Among them: higher levels of poverty, essential jobs that increase exposure, and lower quality or inadequate access to medical care.
Unfortunately, these same factors also affect who participates in research. People of color may be less likely to have doctors recommend studies to them. They may not have the time or the resources to hang out in a waiting room for hours. They may not live near large research institutions that conduct trials. The result is that new treatments, even for diseases that affect Latin, Native American, or African American populations in greater proportions, are studied mostly in white volunteers. The very people who most require solutions to COVID are those who are least likely to be involved in the search to find them.
Virtual trials can alleviate a number of these problems. Not only can people find and request to participate in these types of trials through their phones or computers, virtual trials also cover more costs, include a larger geographical range, and have inherently flexible hours.
"[In a traditional study] you have to go to a doctor's office to enroll and drive a couple of hours and pay $20 for parking and pay $15 for a sandwich in the hospital cafeteria and arrange for daycare for your kids and take time off of work," says Dr. Jonathan Cotliar, chief medical officer of Science37, a platform that investigators can hire to host and organize their trials virtually. "That's a lot just for one visit, much less over the course of a six to 12-month study."
Cotliar's data suggests that virtual trials' enhanced access seriously affects the racial makeup of a given study's participant pool. Sixty percent of patients enrolled in Science37 trials are non-Caucasian, which is, Cotliar says, "staggering compared to what you find in traditional site-based research."
But access is not the only barrier to including more people of color in clinical trials. There is also trust. When agreeing to sign up for research, undocumented immigrants may worry about finding themselves in legal trouble or without any medical support should something go wrong. In a country with a history of experimenting on African Americans without their consent, black people may not trust institutions not to use them as guinea pigs.
"A lot of people report being somewhat disregarded or disrespected once entering the healthcare system," Taylor says. "You take it all together, then people wonder, well, okay, this is how the system tends to regard me, yet now here come these people doing research, and they're all about getting me into their studies." Not so surprising that a lot of people may respond with a resounding "No thanks."
United's ACE inhibitor trial was notable for addressing both of these challenges. In addition to covering costs and allowing study subjects to participate from their own homes, it was being co-sponsored by a professor at Morehouse, one of the country's historic black colleges and universities (often abbreviated HBCUs). United was recruiting heavily in Atlanta, whose population is 52 percent African American. The study promised a thoughtful introduction to a more egalitarian future of medical research.
There's just one problem: It isn't going to happen.
This month, in preparation for the study, United reanalyzed their ACE inhibitor data with all the new patients who'd contracted COVID in the months since their first analysis. Their original data set had been concentrated in the Northeast, mostly New York City, where the earliest outbreak took place. In the 12 weeks it had taken them to set up the virtual followup study, epicenters had shifted. United's second, more geographically comprehensive sample had ten times the number of people in it. And in that sample, the signal simply disappeared.
"I was shocked, but that's the reality," says Deneen Vojta, executive vice president of enterprise research and development for UnitedHealth Group. "You make decisions based on the data, but when you get more data, more information, you might make a different decision. The answer is the answer."
There was no point in running a virtual ACE inhibitor study if a larger, more representative sample of people indicated the drug was unlikely to help anyone. Still, the model United had established to run the trial remains viable. Even as she scrapped the ACE inhibitor study, Vojta hoped not just to continue United's relationship with Dr. Taylor and Morehouse, but to formalize it. Virtual platforms are still an important part of their forthcoming trials.
If people don't believe a vaccine has been created with them in mind, then they won't take it, and it won't matter whether it exists or not.
United is not alone in this approach. As phase three trials for vaccines against SARS CoV-2 get underway, big pharma companies have been publicly articulating their own strategies for including more people of color in clinical trials, and many of these include virtual elements. Janelle Sabo, global head of clinical innovation, systems and clinical supply chain at Eli Lilly, told me that the company is employing home health and telemedicine, direct-to-patient shipping and delivery, and recruitment using social media and geolocation to expand access to more diverse populations.
Dr. Macaya Douoguih, Head of Clinical Development and Medical Affairs for Janssen Vaccines under Johnson & Johnson, spoke to Congress about this issue during a July hearing before the House Energy and Commerce Oversight and Investigations Subcommittee. She said that the company planned to institute a "focused digital and community outreach plan to provide resources and opportunities to encourage participation in our clinical trials," and had partnered with Johns Hopkins Bloomberg School of Public Health "to understand how the COVID-19 crisis is affecting different communities in the United States."
But while some of these plans are well thought-out, others are concerningly nebulous, featuring big pronouncements but fewer tangible strategies. In that same July hearing, Massachusetts representative Joe Kennedy III (D) sounded like a frustrated teacher when admonishing four of the five leads of the present pharma companies (AstraZeneca, Johnson & Johnson, Merck, Moderna, and Pfizer) for not explaining exactly how they'd ensure diversity both in the study of their vaccines, and in their eventual distribution.
This matters: The uptake of the flu vaccine is 10 percentage points lower in both the African American and Hispanic communities than it is in Caucasians. A Pew research study conducted early in the pandemic found that just 54 percent of Black adults said they "would definitely or probably get a coronavirus vaccine," compared to 74 percent of Whites and Hispanics.
"As a good friend of mine, Dr. [James] Hildreth, president at Meharry, another HBC medical school, likes to say: 'A vaccine is great, but it is the vaccination that saves people,'" Taylor says. If people don't believe a vaccine has been created with them in mind, then they won't take it, and it won't matter whether it exists or not.
In this respect, virtual platforms remain an important first step, at least in expanding admittance. In June, United Health opened up a trial to their entire workforce for a computer game that could treat ADHD. In less than two months, 1,743 people had signed up for it, from all different socioeconomic groups, from all over the country. It was inching closer to the kind of number you need for a phase three vaccine trial, which can require tens of thousands of people. Back when they'd been planning the ACE inhibitor study, United had wanted 9,600 people to agree to participate.
Now, with the help of virtual enrollment, they hope they can pull off similarly high numbers for the COVID vaccine trial they will be running for an as-yet-unnamed pharmaceutical partner. It stands to open in September.
Scientists are making machines, wearable and implantable, to act as kidneys
Recent advancements in engineering mean that the first preclinical trials for an artificial kidney could happen soon.
Like all those whose kidneys have failed, Scott Burton’s life revolves around dialysis. For nearly two decades, Burton has been hooked up (or, since 2020, has hooked himself up at home) to a dialysis machine that performs the job his kidneys normally would. The process is arduous, time-consuming, and expensive. Except for a brief window before his body rejected a kidney transplant, Burton has depended on machines to take the place of his kidneys since he was 12-years-old. His whole life, the 39-year-old says, revolves around dialysis.
“Whenever I try to plan anything, I also have to plan my dialysis,” says Burton says, who works as a freelance videographer and editor. “It’s a full-time job in itself.”
Many of those on dialysis are in line for a kidney transplant that would allow them to trade thrice-weekly dialysis and strict dietary limits for a lifetime of immunosuppressants. Burton’s previous transplant means that his body will likely reject another donated kidney unless it matches perfectly—something he’s not counting on. It’s why he’s enthusiastic about the development of artificial kidneys, small wearable or implantable devices that would do the job of a healthy kidney while giving users like Burton more flexibility for traveling, working, and more.
Still, the devices aren’t ready for testing in humans—yet. But recent advancements in engineering mean that the first preclinical trials for an artificial kidney could happen soon, according to Jonathan Himmelfarb, a nephrologist at the University of Washington.
“It would liberate people with kidney failure,” Himmelfarb says.
An engineering marvel
Compared to the heart or the brain, the kidney doesn’t get as much respect from the medical profession, but its job is far more complex. “It does hundreds of different things,” says UCLA’s Ira Kurtz.
Kurtz would know. He’s worked as a nephrologist for 37 years, devoting his career to helping those with kidney disease. While his colleagues in cardiology and endocrinology have seen major advances in the development of artificial hearts and insulin pumps, little has changed for patients on hemodialysis. The machines remain bulky and require large volumes of a liquid called dialysate to remove toxins from a patient’s blood, along with gallons of purified water. A kidney transplant is the next best thing to someone’s own, functioning organ, but with over 600,000 Americans on dialysis and only about 100,000 kidney transplants each year, most of those in kidney failure are stuck on dialysis.
Part of the lack of progress in artificial kidney design is the sheer complexity of the kidney’s job. Each of the 45 different cell types in the kidney do something different.
Part of the lack of progress in artificial kidney design is the sheer complexity of the kidney’s job. To build an artificial heart, Kurtz says, you basically need to engineer a pump. An artificial pancreas needs to balance blood sugar levels with insulin secretion. While neither of these tasks is simple, they are fairly straightforward. The kidney, on the other hand, does more than get rid of waste products like urea and other toxins. Each of the 45 different cell types in the kidney do something different, helping to regulate electrolytes like sodium, potassium, and phosphorous; maintaining blood pressure and water balance; guiding the body’s hormonal and inflammatory responses; and aiding in the formation of red blood cells.

There's been little progress for patients during Ira Kurtz's 37 years as a nephrologist. Artificial kidneys would change that.
UCLA
Dialysis primarily filters waste, and does so well enough to keep someone alive, but it isn’t a true artificial kidney because it doesn’t perform the kidney’s other jobs, according to Kurtz, such as sensing levels of toxins, wastes, and electrolytes in the blood. Due to the size and water requirements of existing dialysis machines, the equipment isn’t portable. Physicians write a prescription for a certain duration of dialysis and assess how well it’s working with semi-regular blood tests. The process of dialysis itself, however, is conducted blind. Doctors can’t tell how much dialysis a patient needs based on kidney values at the time of treatment, says Meera Harhay, a nephrologist at Drexel University in Philadelphia.
But it’s the impact of dialysis on their day-to-day lives that creates the most problems for patients. Only one-quarter of those on dialysis are able to remain employed (compared to 85% of similar-aged adults), and many report a low quality of life. Having more flexibility in life would make a major different to her patients, Harhay says.
“Almost half their week is taken up by the burden of their treatment. It really eats away at their freedom and their ability to do things that add value to their life,” she says.
Art imitates life
The challenge for artificial kidney designers was how to compress the kidney’s natural functions into a portable, wearable, or implantable device that wouldn’t need constant access to gallons of purified and sterilized water. The other universal challenge they faced was ensuring that any part of the artificial kidney that would come in contact with blood was kept germ-free to prevent infection.
As part of the 2021 KidneyX Prize, a partnership between the U.S. Department of Health and Human Services and the American Society of Nephrology, inventors were challenged to create prototypes for artificial kidneys. Himmelfarb’s team at the University of Washington’s Center for Dialysis Innovation won the prize by focusing on miniaturizing existing technologies to create a portable dialysis machine. The backpack sized AKTIV device (Ambulatory Kidney to Increase Vitality) will recycle dialysate in a closed loop system that removes urea from blood and uses light-based chemical reactions to convert the urea to nitrogen and carbon dioxide, which allows the dialysate to be recirculated.
Himmelfarb says that the AKTIV can be used when at home, work, or traveling, which will give users more flexibility and freedom. “If you had a 30-pound device that you could put in the overhead bins when traveling, you could go visit your grandkids,” he says.
Kurtz’s team at UCLA partnered with the U.S. Kidney Research Corporation and Arkansas University to develop a dialysate-free desktop device (about the size of a small printer) as the first phase of a progression that will he hopes will lead to something small and implantable. Part of the reason for the artificial kidney’s size, Kurtz says, is the number of functions his team are cramming into it. Not only will it filter urea from blood, but it will also use electricity to help regulate electrolyte levels in a process called electrodeionization. Kurtz emphasizes that these additional functions are what makes his design a true artificial kidney instead of just a small dialysis machine.

One version of an artificial kidney.
UCLA
“It doesn't have just a static function. It has a bank of sensors that measure chemicals in the blood and feeds that information back to the device,” Kurtz says.
Other startups are getting in on the game. Nephria Bio, a spinout from the South Korean-based EOFlow, is working to develop a wearable dialysis device, akin to an insulin pump, that uses miniature cartridges with nanomaterial filters to clean blood (Harhay is a scientific advisor to Nephria). Ian Welsford, Nephria’s co-founder and CTO, says that the device’s design means that it can also be used to treat acute kidney injuries in resource-limited settings. These potentials have garnered interest and investment in artificial kidneys from the U.S. Department of Defense.
For his part, Burton is most interested in an implantable device, as that would give him the most freedom. Even having a regular outpatient procedure to change batteries or filters would be a minor inconvenience to him.
“Being plugged into a machine, that’s not mimicking life,” he says.
This article was first published by Leaps.org on May 5, 2022.
With this new technology, hospitals and pharmacies could make vaccines and medicines onsite
New research focuses on methods that could change medicine-making worldwide. The scientists propose bursting cells open, removing their DNA and using the cellular gears inside to make therapies.
Most modern biopharmaceutical medicines are produced by workhorse cells—typically bacterial but sometimes mammalian. The cells receive the synthesizing instructions on a snippet of a genetic code, which they incorporate into their DNA. The cellular machinery—ribosomes, RNAs, polymerases, and other compounds—read and use these instructions to build the medicinal molecules, which are harvested and administered to patients.
Although a staple of modern pharma, this process is complex and expensive. One must first insert the DNA instructions into the cells, which they may or may not uptake. One then must grow the cells, keeping them alive and well, so that they produce the required therapeutics, which then must be isolated and purified. To make this at scale requires massive bioreactors and big factories from where the drugs are distributed—and may take a while to arrive where they’re needed. “The pandemic showed us that this method is slow and cumbersome,” says Govind Rao, professor of biochemical engineering who directs the Center for Advanced Sensor Technology at the University of Maryland, Baltimore County (UMBC). “We need better methods that can work faster and can work locally where an outbreak is happening.”
Rao and his team of collaborators, which spans multiple research institutions, believe they have a better approach that may change medicine-making worldwide. They suggest forgoing the concept of using living cells as medicine-producers. Instead, they propose breaking the cells and using the remaining cellular gears for assembling the therapeutic compounds. Instead of inserting the DNA into living cells, the team burst them open, and removed their DNA altogether. Yet, the residual molecular machinery of ribosomes, polymerases and other cogwheels still functioned the way it would in a cell. “Now if you drop your DNA drug-making instructions into that soup, this machinery starts making what you need,” Rao explains. “And because you're no longer worrying about living cells, it becomes much simpler and more efficient.” The collaborators detail their cell-free protein synthesis or CFPS method in their recent paper published in preprint BioAxiv.
While CFPS does not use living cells, it still needs the basic building blocks to assemble proteins from—such as amino acids, nucleotides and certain types of enzymes. These are regularly added into this “soup” to keep the molecular factory chugging. “We just mix everything in as a batch and we let it integrate,” says James Robert Swartz, professor of chemical engineering and bioengineering at Stanford University and co-author of the paper. “And we make sure that we provide enough oxygen.” Rao likens the process to making milk from milk powder.
For a variety of reasons—from the field’s general inertia to regulatory approval hurdles—the method hasn’t become mainstream. The pandemic rekindled interest in medicines that can be made quickly and easily, so it drew more attention to the technology.
The idea of a cell-free protein synthesis is older than one might think. Swartz first experimented with it around 1997, when he was a chemical engineer at Genentech. While working on engineering bacteria to make pharmaceuticals, he discovered that there was a limit to what E. coli cells, the workhorse darling of pharma, could do. For example, it couldn’t grow and properly fold some complex proteins. “We tried many genetic engineering approaches, many fermentation, development, and environmental control approaches,” Swartz recalls—to no avail.
“The organism had its own agenda,” he quips. “And because everything was happening within the organism, we just couldn't really change those conditions very easily. Some of them we couldn’t change at all—we didn’t have control.”
It was out of frustration with the defiant bacteria that a new idea took hold. Could the cells be opened instead, so that the protein-forming reactions could be influenced more easily? “Obviously, we’d lose the ability for them to reproduce,” Swartz says. But that also meant that they no longer needed to keep the cells alive and could focus on making the specific reactions happen. “We could take the catalysts, the enzymes, and the more complex catalysts and activate them, make them work together, much as they would in a living cell, but the way we wanted.”
In 1998, Swartz joined Stanford, and began perfecting the biochemistry of the cell-free method, identifying the reactions he wanted to foster and stopping those he didn’t want. He managed to make the idea work, but for a variety of reasons—from the field’s general inertia to regulatory approval hurdles—the method hasn’t become mainstream. The pandemic rekindled interest in medicines that can be made quickly and easily, so it drew more attention to the technology. For their BioArxiv paper, the team tested the method by growing a specific antiviral protein called griffithsin.
First identified by Barry O’Keefe at National Cancer Institute over a decade ago, griffithsin is an antiviral known to interfere with many viruses’ ability to enter cells—including HIV, SARS, SARS-CoV-2, MERS and others. Originally isolated from the red algae Griffithsia, it works differently from antibodies and antibody cocktails.
Most antiviral medicines tend to target the specific receptors that viruses use to gain entry to the cells they infect. For example, SARS-CoV-2 uses the infamous spike protein to latch onto the ACE2 receptor of mammalian cells. The antibodies or other antiviral molecules stick to the spike protein, shutting off its ability to cling onto the ACE2 receptors. Unfortunately, the spike proteins mutate very often, so the medicines lose their potency. On the contrary, griffithsin has the ability to cling to the different parts of viral shells called capsids—namely to the molecules of mannose, a type of sugar. That extra stuff, glued all around the capsid like dead weight, makes it impossible for the virus to squeeze into the cell.
“Every time we have a vaccine or an antibody against a specific SARS-CoV-2 strain, that strain then mutates and so you lose efficacy,” Rao explains. “But griffithsin molecules glom onto the viral capsid, so the capsid essentially becomes a sticky mess and can’t enter the cell.” Mannose molecules also don’t mutate as easily as viruses’ receptors, so griffithsin-based antivirals do not have to be constantly updated. And because mannose molecules are found on many viruses’ capsids, it makes griffithsin “a universal neutralizer,” Rao explains.
“When griffithsin was discovered, we recognized that it held a lot of promise as a potential antiviral agent,” O’Keefe says. In 2010, he published a paper about griffithsin efficacy in neutralizing viruses of the corona family—after the first SARS outbreak in the early 2000s, the scientific community was interested in such antivirals. Yet, griffithsin is still not available as an off-the-shelf product. So during the Covid pandemic, the team experimented with synthesizing griffithsin using the cell-free production method. They were able to generate potent griffithsin in less than 24 hours without having to grow living cells.
The antiviral protein isn't the only type of medicine that can be made cell-free. The proteins needed for vaccine production could also be made the same way. “Such portable, on-demand drug manufacturing platforms can produce antiviral proteins within hours, making them ideal for combating future pandemics,” Rao says. “We would be able to stop the pandemic before it spreads.”
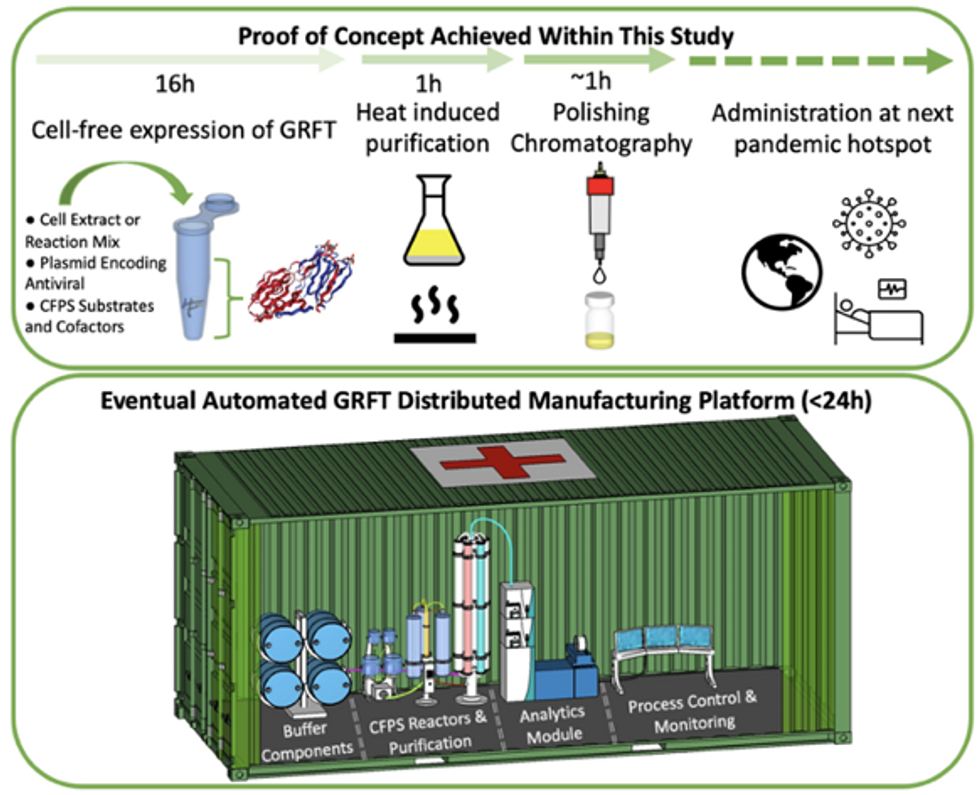
Top: Describes the process used in the study. Bottom: Describes how the new medicines and vaccines could be made at the site of a future viral outbreak.
Image courtesy of Rao and team, sourced from An approach to rapid distributed manufacturing of broad spectrumanti-viral griffithsin using cell-free systems to mitigate pandemics.
Rao’s idea is to perfect the technology to the point that any hospital or pharmacy can load up the media containing molecular factories, mix up the required amino acids, nucleotides and enzymes, and harvest the meds within hours. That will allow making medicines onsite and on demand. “That would be a self-contained production unit, so that you could just ship the production wherever the pandemic is breaking out,” says Swartz.
These units and the meds they produce, will, of course, have to undergo rigorous testing. “The biggest hurdles will be validating these against conventional technology,” Rao says. The biotech industry is risk-averse and prefers the familiar methods. But if this approach works, it may go beyond emergency situations and revolutionize the medicine-making paradigm even outside hospitals and pharmacies. Rao hopes that someday the method might become so mainstream that people may be able to buy and operate such reactors at home. “You can imagine a diabetic patient making insulin that way, or some other drugs,” Rao says. It would work not unlike making baby formula from the mere white powder. Just add water—and some oxygen, too.
Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.

