Why Haven’t Researchers Developed an HIV Vaccine or Cure Yet?
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
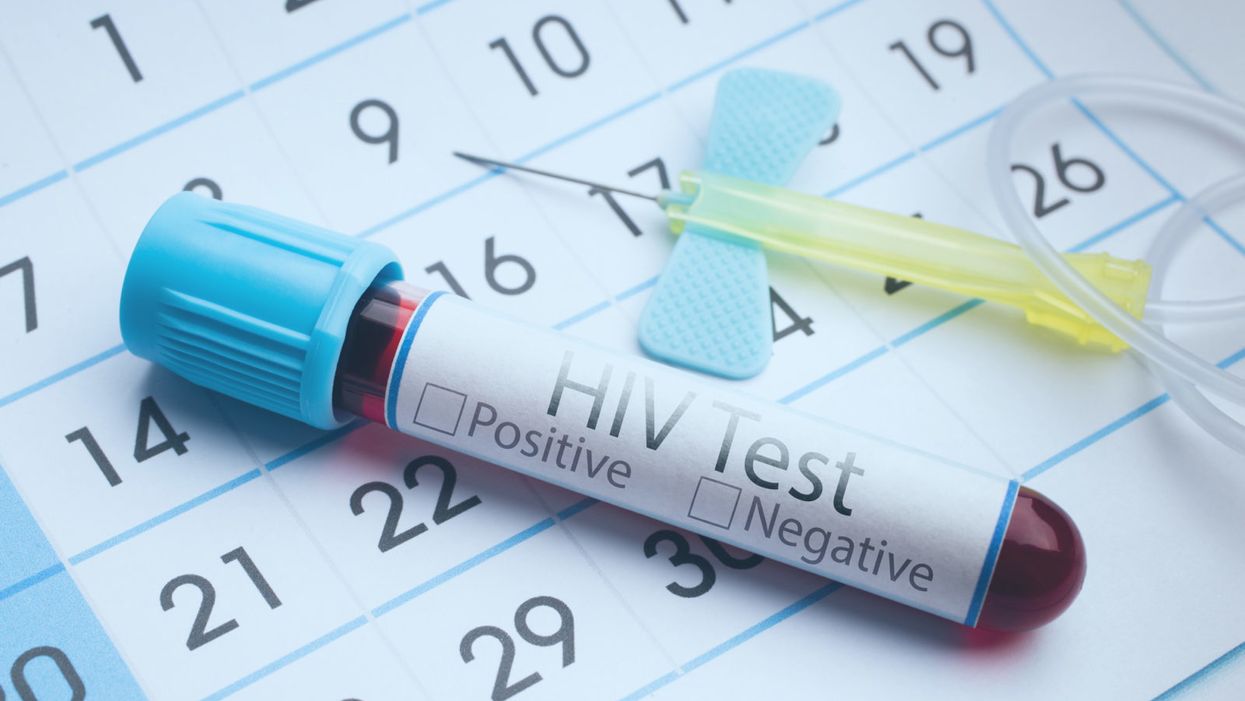
A blood test for analysis of HIV.
Last week, top experts on HIV/AIDS convened in Amsterdam for the 22nd International AIDS conference, and the mood was not great. Even though remarkable advances in treating HIV have led to effective management for many people living with the disease, and its overall incidence has declined, there are signs that the virus could make a troubling comeback.
"In a perfect world, we'd get a vaccine like the HPV vaccine that was 100% effective and I think that's ultimately what we're going to strive for."
Growing resistance to current HIV drugs, a population boom in Sub-Saharan Africa, and insufficient public health resources are all poised to contribute to a second AIDS pandemic, according to published reports.
Already, the virus is nowhere near under control. Though the infection rate has declined 47 percent since its peak in 1996, last year 1.8 million people became newly infected with HIV around the world, and 37 million people are currently living with it. About 1 million people die of AIDS every year, making it the fourth biggest killer in low-income countries.
Leapsmag Editor-in-Chief Kira Peikoff reached out to Dr. Carl Dieffenbach, Director of the Division of AIDS at the National Institute of Allergy and Infectious Diseases, to find out what the U.S. government is doing to develop an HIV vaccine and cure. This interview has been edited and condensed for clarity.
What is the general trajectory of research in HIV/AIDS today?
We can break it down to two specific domains: focus on treatment and cure, and prevention.
Let's start with people living with HIV. This is the area where we've had the most success over the past 30 plus years, because we've taken a disease that was essentially a death sentence and converted it through the development of medications to a treatable chronic disease.
The second half of this equation is, can we cure or create a functional cure for people living with HIV? And the definition of functional cure would be the absence of circulating virus in the body in the absence of therapy. Essentially the human body would control the HIV infection within the individual. That is a much more, very early research stage of discovery. There are some interesting signals but it's still in need of innovation.
I'd like to make a contrast between what we are able to do with a virus called Hepatitis C and what we can do with the virus HIV. Hep C, with 12 weeks of highly active antiviral therapy, we can cure 95 to 100% of infections. With HIV, we cannot do that. The difference is the behavior of the virus. HIV integrates into the host's genome. Hep C is an RNA virus that stays in the cytoplasm of the cell and never gets into the DNA.
On the prevention side, we have two strategies: The first is pre-exposure prophylaxis. Then of course, we have the need for a safe, effective and durable HIV vaccine, which is a very active area of discovery. We've had some spectacular success with RV144, and we're following up on that success, and other vaccines are in the pipeline. Whether they are sufficient to provide the level of durability and activity is not yet clear, but progress has been made and there's still the need for innovation.
The most important breakthrough in the past 5 to 10 years has been the discovery of broad neutralizing monoclonal antibodies. They are proteins that the body makes, and not everybody who's HIV infected makes these antibodies, but we've been able to clone out these antibodies from certain individuals that are highly potent, and when used either singly or in combination, can truly neutralize the vast majority of HIV strains. Can those be used by themselves as treatment or as prevention? That is the question.
Can you explain more about RV144 and why you consider it a success?
Prior to RV144, we had run a number of vaccine studies and nothing had ever statistically shown to be protective. RV144 showed a level of efficacy of about 31 percent, which was statistically significant. Not enough to take forward into other studies, but it allowed us to generate some ideas about why this worked, go back to the drawing board, and redesign the immunogens to optimize and test the next generation for this vaccine. We just recently opened that new study, the follow-up to RV144, called HVTN702. That's up and enrolling and moving along quite nicely.

Carl Dieffenbach, Director of the Division of AIDS at the National Institute of Allergy and Infectious Diseases
(Courtesy)
Where is that enrolling?
Primarily in Sub-Saharan Africa and South Africa.
When will you expect to see signals from that?
Between 2020 and 2021. It's complicated because the signal also takes into account the durability. After a certain time of vaccination, we're going to count up endpoints.
How would you explain the main scientific obstacle in the way of creating a very efficacious HIV vaccine?
Simply put, it's the black box of the human immune system. HIV employs a shield technology, and the virus is constantly changing its shield to protect itself, but there are some key parts of the virus that it cannot shield, so that's the trick – to be able to target that.
So, you're trying to find the Achilles' Heel of the virus?
Exactly. To make a flu vaccine or a Zika vaccine or even an Ebola vaccine, the virus is a little bit more forthcoming with the target. In HIV, the virus does everything in its power to hide the target, so we're dealing with a well-adapted [adversary] that actively avoids neutralization. That's the scientific challenge we face.
What's next?
On the vaccine side, we are currently performing, in collaboration with partners, two vaccine trials – HVTN702, which we talked about, and another one called 705. If either of those are highly successful, they would both require an additional phase 3 clinical trial before they could be licensed. This is an important but not final step. Then we would move into scale up to global vaccination. Those conversations have begun but they are not very far along and need additional attention.
What percent of people in the current trials would need to be protected to move on to phase 3?
Between 50 and 60 percent. That comes with this question of durability: how long does the vaccine last?
It also includes, can we simplify the vaccine regimen? The vaccines we're testing right now are multiple shots over a period of time. Can we get more like the polio or smallpox vaccine, a shot with a booster down the road?
We're dealing with sovereign nations. We're doing this in partnership, not as helicopter-type researchers.
If these current trials pan out, do you think kids in the developed world will end up getting an HIV vaccine one day? Or just people in-at risk areas?
That's a good question. I don't have an answer to that. In a perfect world, we'd get a vaccine like the HPV vaccine that was 100% effective and I think that's ultimately what we're going to strive for. That's where that second or third generation of vaccines that trigger broad neutralizing antibodies come in.
With any luck at all, globally, the combination of antiretroviral treatment, pre-exposure prophylaxis and other prevention and treatment strategies will lower the incidence rate where the HIV pandemic continues to wane, and we will then be able to either target the vaccine or roll it out in a way that is both cost effective and destigmatizing.
And also, what does the country want? We're dealing with sovereign nations. We're doing this in partnership, not as helicopter-type researchers.
How close do you think we are globally to eradicating HIV infections?
Eradication's a big word. It means no new infections. We are nowhere close to eradicating HIV. Whether or not we can continue to bend the curve on the epidemic and have less infections so that the total number of people continues to decline over time, I think we can achieve that if we had the political will. And that's not just the U.S. political will. That's the will of the world. We have the tools, albeit they're not perfect. But that's where a vaccine that is efficacious and simple to deliver could be the gamechanger.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.
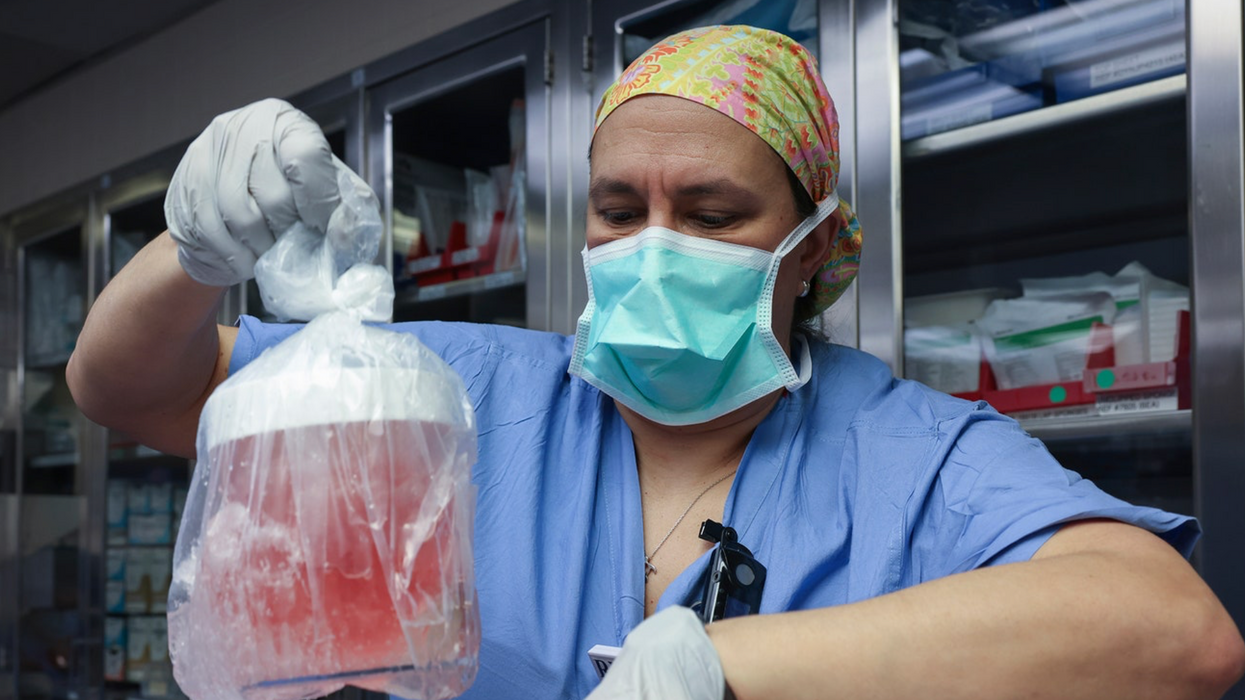
MILESTONE: Doctors have transplanted a pig organ into a human for the first time in history
A surgeon at Massachusetts General Hospital prepares a pig organ for transplant.
Surgeons at Massachusetts General Hospital made history last week when they successfully transplanted a pig kidney into a human patient for the first time ever.
The recipient was a 62-year-old man named Richard Slayman who had been living with end-stage kidney disease caused by diabetes. While Slayman had received a kidney transplant in 2018 from a human donor, his diabetes ultimately caused the kidney to fail less than five years after the transplant. Slayman had undergone dialysis ever since—a procedure that uses an artificial kidney to remove waste products from a person’s blood when the kidneys are unable to—but the dialysis frequently caused blood clots and other complications that landed him in the hospital multiple times.
As a last resort, Slayman’s kidney specialist suggested a transplant using a pig kidney provided by eGenesis, a pharmaceutical company based in Cambridge, Mass. The highly experimental surgery was made possible with the Food and Drug Administration’s “compassionate use” initiative, which allows patients with life-threatening medical conditions access to experimental treatments.
The new frontier of organ donation
Like Slayman, more than 100,000 people are currently on the national organ transplant waiting list, and roughly 17 people die every day waiting for an available organ. To make up for the shortage of human organs, scientists have been experimenting for the past several decades with using organs from animals such as pigs—a new field of medicine known as xenotransplantation. But putting an animal organ into a human body is much more complicated than it might appear, experts say.
“The human immune system reacts incredibly violently to a pig organ, much more so than a human organ,” said Dr. Joren Madsen, director of the Mass General Transplant Center. Even with immunosuppressant drugs that suppress the body’s ability to reject the transplant organ, Madsen said, a human body would reject an animal organ “within minutes.”
So scientists have had to use gene-editing technology to change the animal organs so that they would work inside a human body. The pig kidney in Slayman’s surgery, for instance, had been genetically altered using CRISPR-Cas9 technology to remove harmful pig genes and add human ones. The kidney was also edited to remove pig viruses that could potentially infect a human after transplant.
With CRISPR technology, scientists have been able to prove that interspecies organ transplants are not only possible, but may be able to successfully work long term, too. In the past several years, scientists were able to transplant a pig kidney into a monkey and have the monkey survive for more than two years. More recently, doctors have transplanted pig hearts into human beings—though each recipient of a pig heart only managed to live a couple of months after the transplant. In one of the patients, researchers noted evidence of a pig virus in the man’s heart that had not been identified before the surgery and could be a possible explanation for his heart failure.
So far, so good
Slayman and his medical team ultimately decided to pursue the surgery—and the risk paid off. When the pig organ started producing urine at the end of the four-hour surgery, the entire operating room erupted in applause.
Slayman is currently receiving an infusion of immunosuppressant drugs to prevent the kidney from being rejected, while his doctors monitor the kidney’s function with frequent ultrasounds. Slayman is reported to be “recovering well” at Massachusetts General Hospital and is expected to be discharged within the next several days.Niklas Anzinger is the founder of Infinita VC based in the charter city of Prospera in Honduras. Infinita focuses on a new trend of charter cities and other forms of alternative jurisdictions. Healso hosts a podcast about how to accelerate the future by unblocking “stranded technologies”.This spring he was a part of the network city experiment Zuzalu spearheaded by Ethereum founder Vitalik Buterin where a few hundred invited guests from the spheres of longevity, biotechnology, crypto, artificial intelligence and investment came together to form a two-monthlong community. It has been described as the world’s first pop-up city. Every morning Vitalians would descend on a long breakfast—the menu had been carefully designed by famed radical longevity self-experimenter Bryan Johnson—and there is where I first met Anzinger who told me about Prospera. Intrigued to say the least, I caught up with him later the same week and the following is a record of our conversation.
Q. We are sitting here in the so-called pop-up network state Zuzalu temporarily realized in the village of Lusticia Bay by the beautiful Mediterranean Sea. To me this is an entirely new concept: What is a network state?
A. A network state is a highly aligned online community that has a level of in-person civility; it crowd-funds territory, and it eventually seeks diplomatic recognition. In a way it's about starting a new country. The term was coined by the crypto influencer and former CTO of Coinbase Balaji Srinivasan in a book by the same title last year [2022]. What many people don't know is that it is a more recent addition or innovation in a space called competitive governance. The idea is that you have multiple jurisdictions competing to provide you services as a customer. When you have competition among governments or government service providers, these entities are forced to provide you with a better service instead of the often worse service at higher prices or higher taxes that we're currently getting. The idea went from seasteading, which was hardly feasible because of costs, to charter cities getting public/private partnerships with existing governments and a level of legal autonomy, to special economic zones, to now network states.
Q. How do network states compare to charter cities and similar jurisdictions?
A. Charter cities and special economic zones were legal forks from other existing states. Dubai, Shenzhen in China, to some degree Hong Kong, to some degree Singapore are some examples. There's a host of other charter cities, one of which I'm based in myself, which is Prospera located in Honduras on the island Roatán. Charter cities provide the full stack of governance; they provide new laws and regulations, business registration, tax codes and governance services, Estonia style: you log on to the government platform and you get services as a citizen.
When conceptualizing network states, Balagi Srinivasan turns the idea of a charter city a bit on its head: he doesn't want to start with this full stack because it's still very hard to get these kinds of partnerships with government. It's very expensive and requires lots of experience and lots of social capital. He is saying that network states could instead start as an online community. They could have a level of alignment where they trade with each other; they have their own economy; they meet in person in regular gatherings like we're doing here in Zuzulu for two months, and then they negotiate with existing governments or host cities to get a certain degree of legal autonomy that is centered around a moral innovation. So, his idea is: don't focus on building a completely new country or city; focus on a moral innovation.
Q. What would be an example of such a moral innovation?
A. An example would be longevity—life is good; death is bad—let's see what we can do to foster progress around that moral innovation and see how we can get legal forks from the existing system that allow us to accelerate progress in that area. There is an increasing realization in the science that there are hallmarks of aging and that aging is a cause of other diseases like cancer, ALS or Alzheimer's. But aging is not recognized as a disease by the FDA in the United States and in most countries around the world, so it's very hard to get scientific funding for biotechnology that would attack the hallmarks of aging and allow us potentially to reverse aging and extend life. This is a significant shortcoming of existing government systems that groups such as the ones that have come together here in Montenegro are now seeking alternatives too. Charter cities and now network states are such alternatives.
Q. Would it not be better to work within the current systems, and try to improve them, rather than abandon them for new experimental jurisdictions?
A. There are numerous failures of public policies. These failures are hard, if not impossible, to reverse, because as soon as you have these policies, you have entrenched interests who benefit from the regulations. The only way to disrupt incumbent industries is with start-ups, but the way the system is set up makes it excessively hard for such start-ups to become big companies. In fact, larger companies are weaponizing the legal system against small companies, because they can afford the lawyers and the fixed cost of compliance.
I don't believe that our institutions in many developed countries are beyond hope. I just think it's easier to change them if you could point at successful examples. ‘Hey, this country or this zone is already doing it very successfully’; if they can extend people’s lifespan by 10 years, if they can reduce maternal mortality, and if they have a massive medical tourism where people come back healthier, then that is just very embarrassing for the FDA.
Q. Perhaps a comparison here would be the relationship between Hong Kong and China?
A. Correct, so having Hong Kong right in front of your door … ‘Hey, this capitalism thing seems to work, why don't we try it here?’ It was due to the very bold leadership by Deng Xiaoping that they experimented with it in the development zone of Shenzhen. It worked really well and then they expanded with more special economic zones that also worked.

Próspera is a private city and special economic zone on the island of Roatán in the Central American state of Honduras.
Q. Tell us about Prospera, the charter city in Honduras, that you are intimately connected with.
A. Honduras is a very poor country. It has a lot of crime, never had a single VC investment, and has a GDP per capita of 2,000 per year. Honduras has suffered tremendously. The goal of these special economic zones is to bring in economic development. That's their sole purpose. It's a homegrown innovation from Honduras that started in 2009 with a very forward-thinking statesman, Octavio Sanchez, who was the chief of staff to the president of Honduras, and then president. He had his own ideas about making Honduras a more decentralized system, where more of the power lies in the municipalities.
Inspired by the ideas of Nobel laureate economist Paul Romer, who gave a famous Ted Talk in 2009 about charter cities, Sanchez initiated a process that lasted for years and eventually led to the creation of a special economic zone legal regime that’s anchored in the Hunduran constitution that provides the highest legal autonomy in the world to these zones. There are today three special economic zones approved by the Honduran government: Prospera, Ciudad Morazan and Orchidea.
Q. How did you become interested and then involved in Prospera?
A. I read about it first in an article by Scott Alexander, a famous rationalist blogger, who wrote a very long article about Prospera, and I thought, this is amazing! Then I came to Prospera and I found it to be one of the most if not the most exciting project in the world going on right now and that it also opened my heart to the country and its people. Most of my friends there are Honduran, they have been working on this for 10 or more years. They want to remake Honduras and put it on the map as the place in the world where this legal and governance innovation started.
Q. To what extent is Prospera autonomous relative to the Honduran government?
A. What's interesting about the Honduran model is that it's anchored within the Honduran constitution, and it has a very clear framework for what's possible and what's not possible, and what's possible ensures the highest degree of legal autonomy anywhere seen in the world. Prospera has really pushed the model furthest in creating a common law-based polycentric legal system. The idea is that you don't have a legislature, instead you have common law and it's based on the best practice common law principles that a legal scholar named Tom W. Bell created.
One of the core ideas is that as a business you're not obligated to follow one regulatory monopoly like the FDA. You have regulatory flexibility so you can choose what you're regulated under. So, you can say: ‘if I do a medical clinic, I do it under Norwegian law here’. And you even have the possibility to amend it a bit. You're still required to have liability insurance, and have to agree to binding arbitration in case there's a legal dispute. And your insurance has to approve you. So, under that model the insurance becomes the regulator and they regulate through prices. The limiting factor is criminal law; Honduran criminal law fully applies. So does immigration law. And we pay taxes.
Q. Is there also an idea of creating a kind of healthy living there, and encourage medical tourism?
A. Yes, we specifically look for legal advantages in autonomy around creating new drugs, doing clinical trials, doing self-medication and experimentation. There is a stem cell clinic here and they're doing clinical trials. The island of Roatán is very easily accessible for American tourists. It's a beautiful island, and it's for regulatory reasons hard to do stem cell therapies in the United States, so they're flying in patients from the United States. Most of them are very savvy and often have PhDs in biotech and are able to assess the risk for themselves of taking drugs and doing clinical trials. We're also going to get a wellness center, and there have been ideas around establishing a peptide clinic and a compound pharmacy and things like that. We are developing a healthcare ecosystem.
Q. This kind of experimental tourism raises some ethical issues. What happens if patients are harmed? And what are the moral implications for society of these new treatments?
A. As a moral principle we believe in medical freedom: people have rights over their bodies, even at the (informed) risk of harm to themselves if no unconsenting third-parties are harmed; this is a fundamental right currently not protected effectively.
What we do differently is not changing ethical norms around safety and efficacy, we’re just changing the institutional setup. Instead of one centralized bureaucracy, like the FDA, we have regulatory pluralism that allows different providers of safety and efficacy to compete under market rules. Like under any legal system, common law in Prospera punishes malpractice, fraud, murder etc. This system will still produce safe and effective drugs, and it will still work with common sense legal notions like informed consent and liability for harm. There are regulations for medical practice, there is liability insurance and things like that. It will just do so more efficiently than the current way of doing things (unless it won’t, in which case it will change and evolve – or fail).
A direct moral benefit ´to what we do is that we increase accessibility. Typical gene therapies on the market cost $1 million dollars in the US. The gene therapy developed in Prospera costs $25,000. As to concern about whether such treatments are problematic, we do not share this perspective. We are for advancing science responsibly and we believe that both individuals and society stand to gain from improving the resiliency of the human body through advanced biotechnology.
Q. How does Prospera relate to the local Honduran population?
A. I think it's very important that our projects deliver local benefits and that they're well anchored in local communities. Because when you go to a new place, you're seen as a foreigner, and you're seen as potentially a danger or a threat. The most important thing for Prospera and Ciudad Morazan is to show we're creating jobs; we're creating employment; we're improving people's lives on the ground. Prospera is directly and indirectly employing 1,100 people. More than 2/3 of the people who are working for Prospera are Honduran. It has a lot of local service workers from the island, and it has educated Hondurans from the mainland for whom it's an alternative to going to the United States.
Q. What makes a good Prosperian citizen?
A. People in Prospera are very entrepreneurial. They're opening companies on a small scale. For example, Vehinia, who is the cook in the kitchen at Prospera, she's from the neighboring village and she started an NGO that is now funding a school where children from the local village can go to instead of a school that's 45 minutes away. There's very much a spirit of ‘let's exchange and trade with each other’. Some people might see that as a bit too commercial, but that's something about the culture that people accept and that people see as a good thing.
Q. Five years from now, if everything goes well, what do we see in Prospera?
A. I think Prospera will have at least 10,000 residents and I think Honduras hopefully will have more zones. There could be zones with a thriving industrial sector and sort of a labor-intensive economy and some that are very strong in pharmaceuticals, there could also be other zones for synthetic biology, and other zones focused on agriculture. The zones of Prospera, Ciudad Morazan and Orchidea are already showing the results we want to see, the results that we will eventually be measured by, and I'm tremendously excited about Honduras.