With Lab-Grown Chicken Nuggets, Dumplings, and Burgers, Futuristic Foods Aim to Seem Familiar

Shiok Meat's lab-grown "shrimp" dumplings, alongside a photo of the company's CTO, Ka Yi Ling, in a lab.
Sandhya Sriram is at the forefront of the expanding lab-grown meat industry in more ways than one.
"[Lab-grown meat] is kind of a brave new world for a lot of people, and food isn't something people like being brave about."
She's the CEO and co-founder of one of fewer than 30 companies that is even in this game in the first place. Her Singapore-based company, Shiok Meats, is the only one to pop up in Southeast Asia. And it's the only company in the world that's attempting to grow crustaceans in a lab, starting with shrimp. This spring, the company debuted a prototype of its shrimp, and completed a seed funding round of $4.6 million.
Yet despite all of these wins, Sriram's own mother won't try the company's shrimp. She's a staunch, lifelong vegetarian, adhering to a strict definition of what that means.
"[Lab-grown meat] is kind of a brave new world for a lot of people, and food isn't something people like being brave about. It's really a rather hard-wired thing," says Kate Krueger, the research director at New Harvest, a non-profit accelerator for cellular agriculture (the umbrella field that studies how to grow animal products in the lab, including meat, dairy, and eggs).
It's so hard-wired, in fact, that trends in food inform our species' origin story. In 2017, a group of paleoanthropologists caused an upset when they unearthed fossils in present day Morocco showing that our earliest human ancestors lived much further north and 100,000 years earlier than expected -- the remains date back 300,000 years. But the excavation not only included bones and tools, it also painted a clear picture of the prevailing menu at the time: The oldest humans were apparently chomping on tons of gazelle, as well as wildebeest and zebra when they could find them, plus the occasional seasonal ostrich egg.
These were people with a diet shaped by available resources, but also by the ability to cook in the first place. In his book Catching Fire: How Cooking Made Us Human, Harvard primatologist Richard Wrangam writes that the very thing that allowed for the evolution of Homo sapiens was the ability to transform raw ingredients into edible nutrients through cooking.
Today, our behavior and feelings around food are the product of local climate, crops, animal populations, and tools, but also religion, tradition, and superstition. So what happens when you add science to the mix? Turns out, we still trend toward the familiar. The innovations in lab-grown meat that are picking up the most steam are foods like burgers, not meat chips, and salmon, not salmon-cod-tilapia hybrids. It's not for lack of imagination, it's because the industry's practitioners know that a lifetime of food memories is a hard thing to contend with. So far, the nascent lab-grown meat industry is not so much disrupting as being shaped by the oldest culture we have.
Not a single piece of lab-grown meat is commercially available to consumers yet, and already so much ink has been spilled debating if it's really meat, if it's kosher, if it's vegetarian, if it's ethical, if it's sustainable. But whether or not the industry succeeds and sticks around is almost moot -- watching these conversations and innovations unfold serves as a mirror reflecting back who we are, what concerns us, and what we aspire to.
The More Things Change, the More They Stay the Same
The building blocks for making lab-grown meat right now are remarkably similar, no matter what type of animal protein a company is aiming to produce.
First, a small biopsy, about the size of a sesame seed, is taken from a single animal. Then, the muscle cells are isolated and added to a nutrient-dense culture in a bioreactor -- the same tool used to make beer -- where the cells can multiply, grow, and form muscle tissue. This tissue can then be mixed with additives like nutrients, seasonings, binders, and sometimes colors to form a food product. Whether a company is attempting to make chicken, fish, beef, shrimp, or any other animal protein in a lab, the basic steps remain similar. Cells from various animals do behave differently, though, and each company has its own proprietary techniques and tools. Some, for example, use fetal calf serum as their cell culture, while others, aiming for a more vegan approach, eschew it.
"New gadgets feel safest when they remind us of other objects that we already know."
According to Mark Post, who made the first lab-grown hamburger at Maastricht University in the Netherlands in 2013, the cells of just one cow can give way to 175 million four-ounce burgers. By today's available burger-making methods, you'd need to slaughter 440,000 cows for the same result. The projected difference in the purely material efficiency between the two systems is staggering. The environmental impact is hard to predict, though. Some companies claim that their lab-grown meat requires 99 percent less land and 96 percent less water than traditional farming methods -- and that rearing fewer cows, specifically, would reduce methane emissions -- but the energy cost of running a lab-grown-meat production facility at an industrial scale, especially as compared to small-scale, pasture-raised farming, could be problematic. It's difficult to truly measure any of this in a burgeoning industry.
At this point, growing something like an intact shrimp tail or a marbled steak in a lab is still a Holy Grail. It would require reproducing the complex musculo-skeletal and vascular structure of meat, not just the cellular basis, and no one's successfully done it yet. Until then, many companies working on lab-grown meat are perfecting mince. Each new company's demo of a prototype food feels distinctly regional, though: At the Disruption in Food and Sustainability Summit in March, Shiok (which is pronounced "shook," and is Singaporean slang for "very tasty and delicious") first shared a prototype of its shrimp as an ingredient in siu-mai, a dumpling of Chinese origin and a fixture at dim sum. JUST, a company based in the U.S., produced a demo chicken nugget.
As Jean Anthelme Brillat-Savarin, the 17th century founder of the gastronomic essay, famously said, "Show me what you eat, and I'll tell you who you are."
For many of these companies, the baseline animal protein they are trying to innovate also feels tied to place and culture: When meat comes from a bioreactor, not a farm, the world's largest exporter of seafood could be a landlocked region, and beef could be "reared" in a bayou, yet the handful of lab-grown fish companies, like Finless Foods and BlueNalu, hug the American coasts; VOW, based in Australia, started making lab-grown kangaroo meat in August; and of course the world's first lab-grown shrimp is in Singapore.
"In the U.S., shrimps are either seen in shrimp cocktail, shrimp sushi, and so on, but [in Singapore] we have everything from shrimp paste to shrimp oil," Sriram says. "It's used in noodles and rice, as flavoring in cup noodles, and in biscuits and crackers as well. It's seen in every form, shape, and size. It just made sense for us to go after a protein that was widely used."
It's tempting to assume that innovating on pillars of cultural significance might be easier if the focus were on a whole new kind of food to begin with, not your popular dim sum items or fast food offerings. But it's proving to be quite the opposite.
"That could have been one direction where [researchers] just said, 'Look, it's really hard to reproduce raw ground beef. Why don't we just make something completely new, like meat chips?'" says Mike Lee, co-founder and co-CEO of Alpha Food Labs, which works on food innovation more broadly. "While that strategy's interesting, I think we've got so many new things to explain to people that I don't know if you want to also explain this new format of food that you've never, ever seen before."
We've seen this same cautious approach to change before in other ways that relate to cooking. Perhaps the most obvious example is the kitchen range. As Bee Wilson writes in her book Consider the Fork: A History of How We Cook and Eat, in the 1880s, convincing ardent coal-range users to switch to newfangled gas was a hard sell. To win them over, inventor William Sugg designed a range that used gas, but aesthetically looked like the coal ones already in fashion at the time -- and which in some visual ways harkened even further back to the days of open-hearth cooking. Over time, gas range designs moved further away from those of the past, but the initial jump was only made possible through familiarity. There's a cleverness to meeting people where they are.
"New gadgets feel safest when they remind us of other objects that we already know," writes Wilson. "It is far harder to accept a technology that is entirely new."
Maybe someday we won't want anything other than meat chips, but not today.
Measuring Success
A 2018 Gallup poll shows that in the U.S., rates of true vegetarianism and veganism have been stagnant for as long as they've been measured. When the poll began in 1999, six percent of Americans were vegetarian, a number that remained steady until 2012, when the number dropped one point. As of 2018, it remained at five percent.
In 2012, when Gallup first measured the percentage of vegans, the rate was two percent. By 2018 it had gone up just one point, to three percent. Increasing awareness of animal welfare, health, and environmental concerns don't seem to be incentive enough to convince Americans, en masse, to completely slam the door on a food culture characterized in many ways by its emphasis on traditional meat consumption.
"A lot of consumers get over the ick factor when you tell them that most of the food that you're eating right now has entered the lab at some point."
Wilson writes that "experimenting with new foods has always been a dangerous business. In the wild, trying out some tempting new berries might lead to death. A lingering sense of this danger may make us risk-averse in the kitchen."
That might be one psychologically deep-seated reason that Americans are so resistant to ditch meat altogether. But a middle ground is emerging with a rise in flexitarianism, which aims to reduce reliance on traditional animal products. "Americans are eager to include alternatives to animal products in their diets, but are not willing to give up animal products completely," the same 2018 Gallup poll reported. This may represent the best opportunity for lab-grown meat to wedge itself into the culture.
Quantitatively predicting a population's willingness to try a lab-grown version of its favorite protein is proving a hard thing to measure, however, because it's still science fiction to a regular consumer. Measuring popular opinion of something that doesn't really exist yet is a dubious pastime.
In 2015, University of Wisconsin School of Public Health researchers Linnea Laestadius and Mark Caldwell conducted a study using online comments on articles about lab-grown meat to suss out public response to the food. The results showed a mostly negative attitude, but that was only two years into a field that is six years old today. Already public opinion may have shifted.
Shiok Meat's Sriram and her co-founder Ka Yi Ling have used online surveys to get a sense of the landscape, but they also take a more direct approach sometimes. Every time they give a public talk about their company and their shrimp, they poll their audience before and after the talk, using the question, "How many of you are willing to try, and pay, to eat lab-grown meat?"
They consistently find that the percentage of people willing to try goes up from 50 to 90 percent after hearing their talk, which includes information about the downsides of traditional shrimp farming (for one thing, many shrimp are raised in sewage, and peeled and deveined by slaves) and a bit of information about how lab-grown animal protein is being made now. I saw this pan out myself when Ling spoke at a New Harvest conference in Cambridge, Massachusetts in July.
"A lot of consumers get over the ick factor when you tell them that most of the food that you're eating right now has entered the lab at some point," Sriram says. "We're not going to grow our meat in the lab always. It's in the lab right now, because we're in R&D. Once we go into manufacturing ... it's going to be a food manufacturing facility, where a lot of food comes from."
The downside of the University of Wisconsin's and Shiok Meat's approach to capturing public opinion is that they each look at self-selecting groups: Online commenters are often fueled by a need to complain, and it's likely that anyone attending a talk by the co-founders of a lab-grown meat company already has some level of open-mindedness.
So Sriram says that she and Ling are also using another method to assess the landscape, and it's somewhere in the middle. They've been watching public responses to the closest available product to lab-grown meat that's on the market: Impossible Burger. As a 100 percent plant-based burger, it's not quite the same, but this bleedable, searable patty is still very much the product of science and laboratory work. Its remarkable similarity to beef is courtesy of yeast that have been genetically engineered to contain DNA from soy plant roots, which produce a protein called heme as they multiply. This heme is a plant-derived protein that can look and act like the heme found in animal muscle.
So far, the sciencey underpinnings of the burger don't seem to be turning people off. In just four years, it's already found its place within other American food icons. It's readily available everywhere from nationwide Burger Kings to Boston's Warren Tavern, which has been in operation since 1780, is one of the oldest pubs in America, and is even named after the man who sent Paul Revere on his midnight ride. Some people have already grown so attached to the Impossible Burger that they will actually walk out of a restaurant that's out of stock. Demand for the burger is outpacing production.
"Even though [Impossible] doesn't consider their product cellular agriculture, it's part of a spectrum of innovation," Krueger says. "There are novel proteins that you're not going to find in your average food, and there's some cool tech there. So to me, that does show a lot of willingness on people's part to think about trying something new."
The message for those working on animal-based lab-grown meat is clear: People will accept innovation on their favorite food if it tastes good enough and evokes the same emotional connection as the real deal.
"How people talk about lab-grown meat now, it's still a conversation about science, not about culture and emotion," Lee says. But he's confident that the conversation will start to shift in that direction if the companies doing this work can nail the flavor memory, above all.
And then proving how much power flavor lords over us, we quickly derail into a conversation about Doritos, which he calls "maniacally delicious." The chips carry no health value whatsoever and are a native product of food engineering and manufacturing — just watch how hard it is for Bon Appetit associate food editor Claire Saffitz to try and recreate them in the magazine's test kitchen — yet devotees remain unfazed and crunch on.
"It's funny because it shows you that people don't ask questions about how [some foods] are made, so why are they asking so many questions about how lab-grown meat is made?" Lee asks.
For all the hype around Impossible Burger, there are still controversies and hand-wringing around lab-grown meat. Some people are grossed out by the idea, some people are confused, and if you're the U.S. Cattlemen's Association (USCA), you're territorial. Last year, the group sent a petition to the USDA to "exclude products not derived directly from animals raised and slaughtered from the definition of 'beef' and meat.'"
"I think we are probably three or four big food safety scares away from everyone, especially younger generations, embracing lab-grown meat as like, 'Science is good; nature is dirty, and can kill you.'"
"I have this working hypothesis that if you look at the nation in 50-year spurts, we revolve back and forth between artisanal, all-natural food that's unadulterated and pure, and food that's empowered by science," Lee says. "Maybe we've only had one lap around the track on that, but I think we are probably three or four big food safety scares away from everyone, especially younger generations, embracing lab-grown meat as like, 'Science is good; nature is dirty, and can kill you.'"
Food culture goes beyond just the ingredients we know and love — it's also about how we interact with them, produce them, and expect them to taste and feel when we bite down. We accept a margin of difference among a fast food burger, a backyard burger from the grill, and a gourmet burger. Maybe someday we'll accept the difference between a burger created by killing a cow and a burger created by biopsying one.
Looking to the Future
Every time we engage with food, "we are enacting a ritual that binds us to the place we live and to those in our family, both living and dead," Wilson writes in Consider the Fork. "Such things are not easily shrugged off. Every time a new cooking technology has been introduced, however useful … it has been greeted in some quarters with hostility and protestations that the old ways were better and safer."
This is why it might be hard for a vegetarian mother to try her daughter's lab-grown shrimp, no matter how ethically it was produced or how awe-inspiring the invention is. Yet food cultures can and do change. "They're not these static things," says Benjamin Wurgaft, a historian whose book Meat Planet: Artificial Flesh and the Future of Food comes out this month. "The real tension seems to be between slow change and fast change."
In fact, the very definition of the word "meat" has never exclusively meant what the USCA wants it to mean. Before the 12th century, when it first appeared in Old English as "mete," it wasn't very specific at all and could be used to describe anything from "nourishment," to "food item," to "fodder," to "sustenance." By the 13th century it had been narrowed down to mean "flesh of warm-blooded animals killed and used as food." And yet the British mincemeat pie lives on as a sweet Christmas treat full of -- to the surprise of many non-Brits -- spiced, dried fruit. Since 1901, we've also used this word with ease as a general term for anything that's substantive -- as in, "the meat of the matter." There is room for yet more definitions to pile on.
"The conversation [about lab-ground meat] has changed remarkably in the last six years," Wurgaft says. "It has become a conversation about whether or not specific companies will bring a product to market, and that's a really different conversation than asking, 'Should we produce meat in the lab?'"
As part of the field research for his book, Wurgaft visited the Rijksmuseum Boerhaave, a Dutch museum that specializes in the history of science and medicine. It was 2015, and he was there to see an exhibit on the future of food. Just two years earlier, Mark Post had made that first lab-grown hamburger about a two-and-a-half hour drive south of the museum. When Wurgaft arrived, he found the novel invention, which Post had donated to the museum, already preserved and served up on a dinner plate, the whole outfit protected by plexiglass.
"They put this in the exhibit as if it were already part of the historical records, which to a historian looked really weird," Wurgaft says. "It looked like somebody taking the most recent supercomputer and putting it in a museum exhibit saying, 'This is the supercomputer that changed everything,' as if you were already 100 years in the future, looking back."
It seemed to symbolize an effort to codify a lab-grown hamburger as a matter of Dutch pride, perhaps someday occupying a place in people's hearts right next to the stroopwafel.
"Who's to say that we couldn't get a whole school of how to cook with lab-grown meat?"
Lee likes to imagine that part of the legacy of lab-grown meat, if it succeeds, will be to inspire entirely new fads in cooking -- a step beyond ones like the crab-filled avocado of the 1960s or the pesto of the 1980s in the U.S.
"[Lab-grown meat] is inherently going to be a different quality than anything we've done with an animal," he says. "Look at every cut [of meat] on the sphere today -- each requires a slightly different cooking method to optimize the flavor of that cut. Who's to say that we couldn't get a whole school of how to cook with lab-grown meat?"
At this point, most of us have no way of trying lab-grown meat. It remains exclusively available through sometimes gimmicky demos reserved for investors and the media. But Wurgaft says the stories we tell about this innovation, the articles we write, the films we make, and yes, even the museum exhibits we curate, all hold as much cultural significance as the product itself might someday.
Scientists are making machines, wearable and implantable, to act as kidneys
Recent advancements in engineering mean that the first preclinical trials for an artificial kidney could happen soon.
Like all those whose kidneys have failed, Scott Burton’s life revolves around dialysis. For nearly two decades, Burton has been hooked up (or, since 2020, has hooked himself up at home) to a dialysis machine that performs the job his kidneys normally would. The process is arduous, time-consuming, and expensive. Except for a brief window before his body rejected a kidney transplant, Burton has depended on machines to take the place of his kidneys since he was 12-years-old. His whole life, the 39-year-old says, revolves around dialysis.
“Whenever I try to plan anything, I also have to plan my dialysis,” says Burton says, who works as a freelance videographer and editor. “It’s a full-time job in itself.”
Many of those on dialysis are in line for a kidney transplant that would allow them to trade thrice-weekly dialysis and strict dietary limits for a lifetime of immunosuppressants. Burton’s previous transplant means that his body will likely reject another donated kidney unless it matches perfectly—something he’s not counting on. It’s why he’s enthusiastic about the development of artificial kidneys, small wearable or implantable devices that would do the job of a healthy kidney while giving users like Burton more flexibility for traveling, working, and more.
Still, the devices aren’t ready for testing in humans—yet. But recent advancements in engineering mean that the first preclinical trials for an artificial kidney could happen soon, according to Jonathan Himmelfarb, a nephrologist at the University of Washington.
“It would liberate people with kidney failure,” Himmelfarb says.
An engineering marvel
Compared to the heart or the brain, the kidney doesn’t get as much respect from the medical profession, but its job is far more complex. “It does hundreds of different things,” says UCLA’s Ira Kurtz.
Kurtz would know. He’s worked as a nephrologist for 37 years, devoting his career to helping those with kidney disease. While his colleagues in cardiology and endocrinology have seen major advances in the development of artificial hearts and insulin pumps, little has changed for patients on hemodialysis. The machines remain bulky and require large volumes of a liquid called dialysate to remove toxins from a patient’s blood, along with gallons of purified water. A kidney transplant is the next best thing to someone’s own, functioning organ, but with over 600,000 Americans on dialysis and only about 100,000 kidney transplants each year, most of those in kidney failure are stuck on dialysis.
Part of the lack of progress in artificial kidney design is the sheer complexity of the kidney’s job. Each of the 45 different cell types in the kidney do something different.
Part of the lack of progress in artificial kidney design is the sheer complexity of the kidney’s job. To build an artificial heart, Kurtz says, you basically need to engineer a pump. An artificial pancreas needs to balance blood sugar levels with insulin secretion. While neither of these tasks is simple, they are fairly straightforward. The kidney, on the other hand, does more than get rid of waste products like urea and other toxins. Each of the 45 different cell types in the kidney do something different, helping to regulate electrolytes like sodium, potassium, and phosphorous; maintaining blood pressure and water balance; guiding the body’s hormonal and inflammatory responses; and aiding in the formation of red blood cells.

There's been little progress for patients during Ira Kurtz's 37 years as a nephrologist. Artificial kidneys would change that.
UCLA
Dialysis primarily filters waste, and does so well enough to keep someone alive, but it isn’t a true artificial kidney because it doesn’t perform the kidney’s other jobs, according to Kurtz, such as sensing levels of toxins, wastes, and electrolytes in the blood. Due to the size and water requirements of existing dialysis machines, the equipment isn’t portable. Physicians write a prescription for a certain duration of dialysis and assess how well it’s working with semi-regular blood tests. The process of dialysis itself, however, is conducted blind. Doctors can’t tell how much dialysis a patient needs based on kidney values at the time of treatment, says Meera Harhay, a nephrologist at Drexel University in Philadelphia.
But it’s the impact of dialysis on their day-to-day lives that creates the most problems for patients. Only one-quarter of those on dialysis are able to remain employed (compared to 85% of similar-aged adults), and many report a low quality of life. Having more flexibility in life would make a major different to her patients, Harhay says.
“Almost half their week is taken up by the burden of their treatment. It really eats away at their freedom and their ability to do things that add value to their life,” she says.
Art imitates life
The challenge for artificial kidney designers was how to compress the kidney’s natural functions into a portable, wearable, or implantable device that wouldn’t need constant access to gallons of purified and sterilized water. The other universal challenge they faced was ensuring that any part of the artificial kidney that would come in contact with blood was kept germ-free to prevent infection.
As part of the 2021 KidneyX Prize, a partnership between the U.S. Department of Health and Human Services and the American Society of Nephrology, inventors were challenged to create prototypes for artificial kidneys. Himmelfarb’s team at the University of Washington’s Center for Dialysis Innovation won the prize by focusing on miniaturizing existing technologies to create a portable dialysis machine. The backpack sized AKTIV device (Ambulatory Kidney to Increase Vitality) will recycle dialysate in a closed loop system that removes urea from blood and uses light-based chemical reactions to convert the urea to nitrogen and carbon dioxide, which allows the dialysate to be recirculated.
Himmelfarb says that the AKTIV can be used when at home, work, or traveling, which will give users more flexibility and freedom. “If you had a 30-pound device that you could put in the overhead bins when traveling, you could go visit your grandkids,” he says.
Kurtz’s team at UCLA partnered with the U.S. Kidney Research Corporation and Arkansas University to develop a dialysate-free desktop device (about the size of a small printer) as the first phase of a progression that will he hopes will lead to something small and implantable. Part of the reason for the artificial kidney’s size, Kurtz says, is the number of functions his team are cramming into it. Not only will it filter urea from blood, but it will also use electricity to help regulate electrolyte levels in a process called electrodeionization. Kurtz emphasizes that these additional functions are what makes his design a true artificial kidney instead of just a small dialysis machine.

One version of an artificial kidney.
UCLA
“It doesn't have just a static function. It has a bank of sensors that measure chemicals in the blood and feeds that information back to the device,” Kurtz says.
Other startups are getting in on the game. Nephria Bio, a spinout from the South Korean-based EOFlow, is working to develop a wearable dialysis device, akin to an insulin pump, that uses miniature cartridges with nanomaterial filters to clean blood (Harhay is a scientific advisor to Nephria). Ian Welsford, Nephria’s co-founder and CTO, says that the device’s design means that it can also be used to treat acute kidney injuries in resource-limited settings. These potentials have garnered interest and investment in artificial kidneys from the U.S. Department of Defense.
For his part, Burton is most interested in an implantable device, as that would give him the most freedom. Even having a regular outpatient procedure to change batteries or filters would be a minor inconvenience to him.
“Being plugged into a machine, that’s not mimicking life,” he says.
This article was first published by Leaps.org on May 5, 2022.
With this new technology, hospitals and pharmacies could make vaccines and medicines onsite
New research focuses on methods that could change medicine-making worldwide. The scientists propose bursting cells open, removing their DNA and using the cellular gears inside to make therapies.
Most modern biopharmaceutical medicines are produced by workhorse cells—typically bacterial but sometimes mammalian. The cells receive the synthesizing instructions on a snippet of a genetic code, which they incorporate into their DNA. The cellular machinery—ribosomes, RNAs, polymerases, and other compounds—read and use these instructions to build the medicinal molecules, which are harvested and administered to patients.
Although a staple of modern pharma, this process is complex and expensive. One must first insert the DNA instructions into the cells, which they may or may not uptake. One then must grow the cells, keeping them alive and well, so that they produce the required therapeutics, which then must be isolated and purified. To make this at scale requires massive bioreactors and big factories from where the drugs are distributed—and may take a while to arrive where they’re needed. “The pandemic showed us that this method is slow and cumbersome,” says Govind Rao, professor of biochemical engineering who directs the Center for Advanced Sensor Technology at the University of Maryland, Baltimore County (UMBC). “We need better methods that can work faster and can work locally where an outbreak is happening.”
Rao and his team of collaborators, which spans multiple research institutions, believe they have a better approach that may change medicine-making worldwide. They suggest forgoing the concept of using living cells as medicine-producers. Instead, they propose breaking the cells and using the remaining cellular gears for assembling the therapeutic compounds. Instead of inserting the DNA into living cells, the team burst them open, and removed their DNA altogether. Yet, the residual molecular machinery of ribosomes, polymerases and other cogwheels still functioned the way it would in a cell. “Now if you drop your DNA drug-making instructions into that soup, this machinery starts making what you need,” Rao explains. “And because you're no longer worrying about living cells, it becomes much simpler and more efficient.” The collaborators detail their cell-free protein synthesis or CFPS method in their recent paper published in preprint BioAxiv.
While CFPS does not use living cells, it still needs the basic building blocks to assemble proteins from—such as amino acids, nucleotides and certain types of enzymes. These are regularly added into this “soup” to keep the molecular factory chugging. “We just mix everything in as a batch and we let it integrate,” says James Robert Swartz, professor of chemical engineering and bioengineering at Stanford University and co-author of the paper. “And we make sure that we provide enough oxygen.” Rao likens the process to making milk from milk powder.
For a variety of reasons—from the field’s general inertia to regulatory approval hurdles—the method hasn’t become mainstream. The pandemic rekindled interest in medicines that can be made quickly and easily, so it drew more attention to the technology.
The idea of a cell-free protein synthesis is older than one might think. Swartz first experimented with it around 1997, when he was a chemical engineer at Genentech. While working on engineering bacteria to make pharmaceuticals, he discovered that there was a limit to what E. coli cells, the workhorse darling of pharma, could do. For example, it couldn’t grow and properly fold some complex proteins. “We tried many genetic engineering approaches, many fermentation, development, and environmental control approaches,” Swartz recalls—to no avail.
“The organism had its own agenda,” he quips. “And because everything was happening within the organism, we just couldn't really change those conditions very easily. Some of them we couldn’t change at all—we didn’t have control.”
It was out of frustration with the defiant bacteria that a new idea took hold. Could the cells be opened instead, so that the protein-forming reactions could be influenced more easily? “Obviously, we’d lose the ability for them to reproduce,” Swartz says. But that also meant that they no longer needed to keep the cells alive and could focus on making the specific reactions happen. “We could take the catalysts, the enzymes, and the more complex catalysts and activate them, make them work together, much as they would in a living cell, but the way we wanted.”
In 1998, Swartz joined Stanford, and began perfecting the biochemistry of the cell-free method, identifying the reactions he wanted to foster and stopping those he didn’t want. He managed to make the idea work, but for a variety of reasons—from the field’s general inertia to regulatory approval hurdles—the method hasn’t become mainstream. The pandemic rekindled interest in medicines that can be made quickly and easily, so it drew more attention to the technology. For their BioArxiv paper, the team tested the method by growing a specific antiviral protein called griffithsin.
First identified by Barry O’Keefe at National Cancer Institute over a decade ago, griffithsin is an antiviral known to interfere with many viruses’ ability to enter cells—including HIV, SARS, SARS-CoV-2, MERS and others. Originally isolated from the red algae Griffithsia, it works differently from antibodies and antibody cocktails.
Most antiviral medicines tend to target the specific receptors that viruses use to gain entry to the cells they infect. For example, SARS-CoV-2 uses the infamous spike protein to latch onto the ACE2 receptor of mammalian cells. The antibodies or other antiviral molecules stick to the spike protein, shutting off its ability to cling onto the ACE2 receptors. Unfortunately, the spike proteins mutate very often, so the medicines lose their potency. On the contrary, griffithsin has the ability to cling to the different parts of viral shells called capsids—namely to the molecules of mannose, a type of sugar. That extra stuff, glued all around the capsid like dead weight, makes it impossible for the virus to squeeze into the cell.
“Every time we have a vaccine or an antibody against a specific SARS-CoV-2 strain, that strain then mutates and so you lose efficacy,” Rao explains. “But griffithsin molecules glom onto the viral capsid, so the capsid essentially becomes a sticky mess and can’t enter the cell.” Mannose molecules also don’t mutate as easily as viruses’ receptors, so griffithsin-based antivirals do not have to be constantly updated. And because mannose molecules are found on many viruses’ capsids, it makes griffithsin “a universal neutralizer,” Rao explains.
“When griffithsin was discovered, we recognized that it held a lot of promise as a potential antiviral agent,” O’Keefe says. In 2010, he published a paper about griffithsin efficacy in neutralizing viruses of the corona family—after the first SARS outbreak in the early 2000s, the scientific community was interested in such antivirals. Yet, griffithsin is still not available as an off-the-shelf product. So during the Covid pandemic, the team experimented with synthesizing griffithsin using the cell-free production method. They were able to generate potent griffithsin in less than 24 hours without having to grow living cells.
The antiviral protein isn't the only type of medicine that can be made cell-free. The proteins needed for vaccine production could also be made the same way. “Such portable, on-demand drug manufacturing platforms can produce antiviral proteins within hours, making them ideal for combating future pandemics,” Rao says. “We would be able to stop the pandemic before it spreads.”
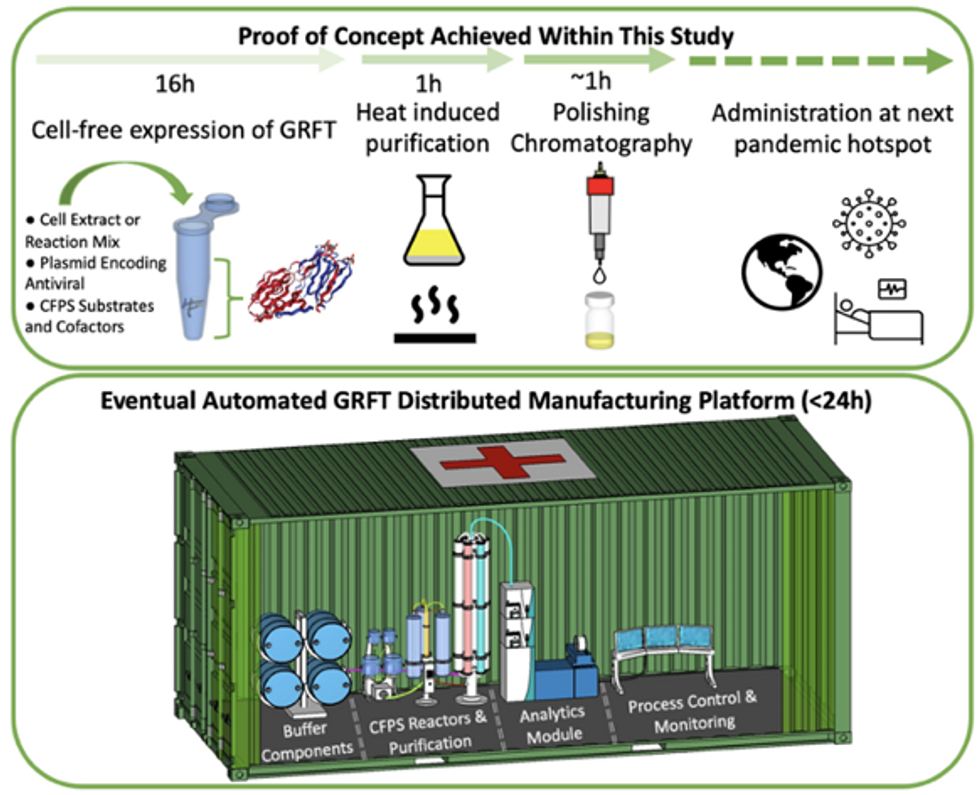
Top: Describes the process used in the study. Bottom: Describes how the new medicines and vaccines could be made at the site of a future viral outbreak.
Image courtesy of Rao and team, sourced from An approach to rapid distributed manufacturing of broad spectrumanti-viral griffithsin using cell-free systems to mitigate pandemics.
Rao’s idea is to perfect the technology to the point that any hospital or pharmacy can load up the media containing molecular factories, mix up the required amino acids, nucleotides and enzymes, and harvest the meds within hours. That will allow making medicines onsite and on demand. “That would be a self-contained production unit, so that you could just ship the production wherever the pandemic is breaking out,” says Swartz.
These units and the meds they produce, will, of course, have to undergo rigorous testing. “The biggest hurdles will be validating these against conventional technology,” Rao says. The biotech industry is risk-averse and prefers the familiar methods. But if this approach works, it may go beyond emergency situations and revolutionize the medicine-making paradigm even outside hospitals and pharmacies. Rao hopes that someday the method might become so mainstream that people may be able to buy and operate such reactors at home. “You can imagine a diabetic patient making insulin that way, or some other drugs,” Rao says. It would work not unlike making baby formula from the mere white powder. Just add water—and some oxygen, too.
Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.

