Your Community and COVID-19: How to Make Sense of the Numbers Where You Live
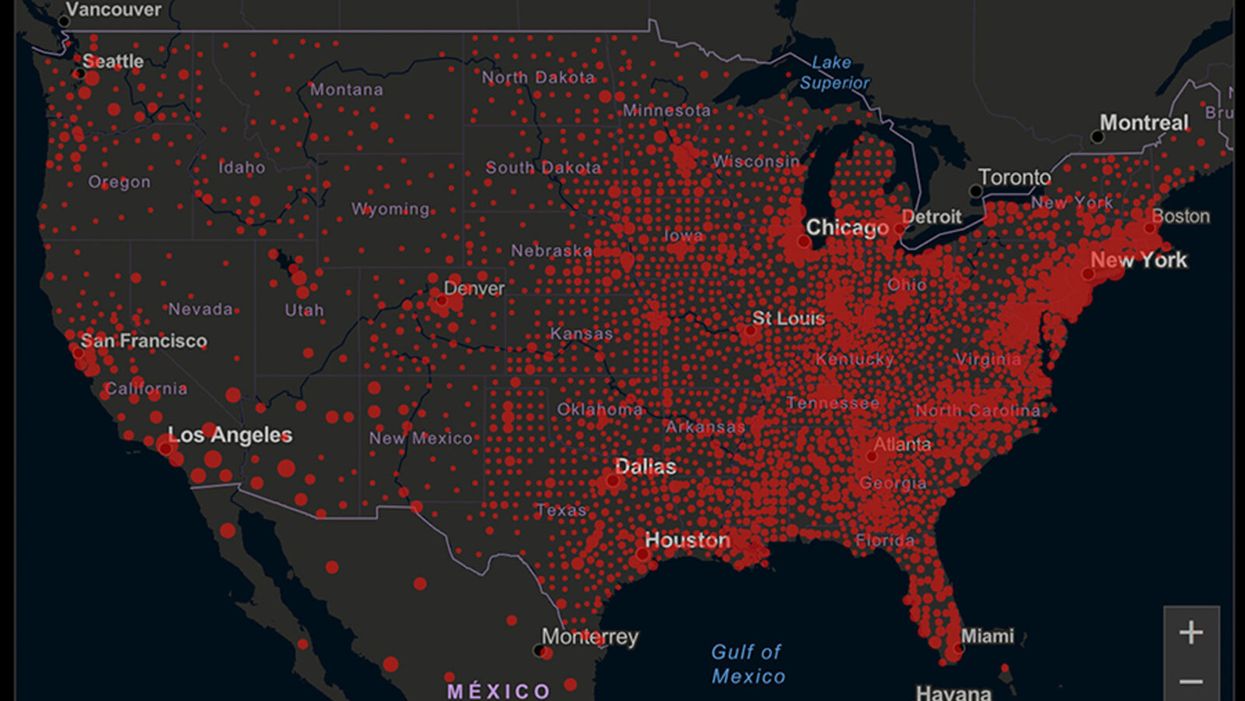
A map of cumulative known cases of COVID-19 in the U.S., as of June 12th, 2020.
Have you felt a bit like an armchair epidemiologist lately? Maybe you've been poring over coronavirus statistics on your county health department's website or on the pages of your local newspaper.
If the percentage of positive tests steadily stays under 8 percent, that's generally a good sign.
You're likely to find numbers and charts but little guidance about how to interpret them, let alone use them to make day-to-day decisions about pandemic safety precautions.
Enter the gurus. We asked several experts to provide guidance for laypeople about how to navigate the numbers. Here's a look at several common COVID-19 statistics along with tips about how to understand them.
Case Counts: Consider the Context
The number of confirmed COVID-19 cases in American counties is widely available. Local and state health departments should provide them online, or you can easily look them up at The New York Times' coronavirus database. However, you need to be cautious about interpreting them.
"Case counts are the obvious numbers to look at. But they're probably the hardest thing to sort out," said Dr. Jeff Martin, an epidemiologist at the University of California at San Francisco.
That's because case counts by themselves aren't a good window into how the coronavirus is affecting your community since they rely on testing. And testing itself varies widely from day to day and community to community.
"The more testing that's done, the more infections you'll pick up," explained Dr. F. Perry Wilson, a physician at Yale University. The numbers can also be thrown off when tests are limited to certain groups of people.
"If the tests are being mostly given to people with a high probability of having been infected -- for example, they have had symptoms or work in a high-risk setting -- then we expect lots of the tests to be positive. But that doesn't tell us what proportion of the general public is likely to have been infected," said Eleanor Murray, an epidemiologist at Boston University.
These Stats Are More Meaningful
According to Dr. Wilson, it's more useful to keep two other statistics in mind: the number of COVID tests that are being performed in your community and the percentage that turn up positive, showing that people have the disease. (These numbers may or may not be available locally. Check the websites of your community's health department and local news media outlets.)
If the number of people being tested is going up, but the percentage of positive tests is going down, Dr. Wilson said, that's a good sign. But if both numbers are going up – the number of people tested and the percentage of positive results – then "that's a sign that there are more infections burning in the community."
It's especially worrisome if the percentage of positive cases is growing compared to previous days or weeks, he said. According to him, that's a warning of a "high-risk situation."
Dr. George Rutherford, an epidemiologist at University of California at San Francisco, offered this tip: If the percentage of positive tests steadily stays under 8 percent, that's generally a good sign.
There's one more caveat about case counts. It takes an average of a week for someone to be infected with COVID-19, develop symptoms, and get tested, Dr. Rutherford said. It can take an additional several days for those test results to be reported to the county health department. This means that case numbers don't represent infections happening right now, but instead are a picture of the state of the pandemic more than a week ago.
Hospitalizations: Focus on Current Statistics
You should be able to find numbers about how many people in your community are currently hospitalized – or have been hospitalized – with diagnoses of COVID-19. But experts say these numbers aren't especially revealing unless you're able to see the number of new hospitalizations over time and track whether they're rising or falling. This number often isn't publicly available, however.
If new hospitalizations are increasing, "you may want to react by being more careful yourself."
And there's an important caveat: "The problem with hospitalizations is that they do lag," UC San Francisco's Dr. Martin said, since it takes time for someone to become ill enough to need to be hospitalized. "They tell you how much virus was being transmitted in your community 2 or 2.5 weeks ago."
Also, he said, people should be cautious about comparing new hospitalization rates between communities unless they're adjusted to account for the number of more-vulnerable older people.
Still, if new hospitalizations are increasing, he said, "you may want to react by being more careful yourself."
Deaths: They're an Even More Delayed Headline
Cable news networks obsessively track the number of coronavirus deaths nationwide, and death counts for every county in the country are available online. Local health departments and media websites may provide charts tracking the growth in deaths over time in your community.
But while death rates offer insight into the disease's horrific toll, they're not useful as an instant snapshot of the pandemic in your community because severely ill patients are typically sick for weeks. Instead, think of them as a delayed headline.
"These numbers don't tell you what's happening today. They tell you how much virus was being transmitted 3-4 weeks ago," Dr. Martin said.
'Reproduction Value': It May Be Revealing
You're not likely to find an available "reproduction value" for your community, but it is available for your state and may be useful.
A reproduction value, also known as R0 or R-naught, "tells us how many people on average we expect will be infected from a single case if we don't take any measures to intervene and if no one has been infected before," said Boston University's Murray.
As The New York Times explained, "R0 is messier than it might look. It is built on hard science, forensic investigation, complex mathematical models — and often a good deal of guesswork. It can vary radically from place to place and day to day, pushed up or down by local conditions and human behavior."
It may be impossible to find the R0 for your community. However, a website created by data specialists is providing updated estimates of a related number -- effective reproduction number, or Rt – for each state. (The R0 refers to how infectious the disease is in general and if precautions aren't taken. The Rt measures its infectiousness at a specific time – the "t" in Rt.) The site is at rt.live.
"The main thing to look at is whether the number is bigger than 1, meaning the outbreak is currently growing in your area, or smaller than 1, meaning the outbreak is currently decreasing in your area," Murray said. "It's also important to remember that this number depends on the prevention measures your community is taking. If the Rt is estimated to be 0.9 in your area and you are currently under lockdown, then to keep it below 1 you may need to remain under lockdown. Relaxing the lockdown could mean that Rt increases above 1 again."
"Whether they're on the upswing or downswing, no state is safe enough to ignore the precautions about mask wearing and social distancing."
Keep in mind that you can still become infected even if an outbreak in your community appears to be slowing. Low risk doesn't mean no risk.
Putting It All Together: Why the Numbers Matter
So you've reviewed COVID-19 statistics in your community. Now what?
Dr. Wilson suggests using the data to remind yourself that the coronavirus pandemic "is still out there. You need to take it seriously and continue precautions," he said. "Whether they're on the upswing or downswing, no state is safe enough to ignore the precautions about mask wearing and social distancing. 'My state is doing well, no one I know is sick, is it time to have a dinner party?' No."
He also recommends that laypeople avoid tracking COVID-19 statistics every day. "Check in once a week or twice a month to see how things are going," he suggested. "Don't stress too much. Just let it remind you to put that mask on before you get out of your car [and are around others]."
Staying well in the 21st century is like playing a game of chess
The control of infectious diseases was considered to be one of the “10 Great Public Health Achievements.” What we didn’t take into account was the very concept of evolution: as we built better protections, our enemies eventually boosted their attacking prowess, so soon enough we found ourselves on the defensive once again.
This article originally appeared in One Health/One Planet, a single-issue magazine that explores how climate change and other environmental shifts are increasing vulnerabilities to infectious diseases by land and by sea. The magazine probes how scientists are making progress with leaders in other fields toward solutions that embrace diverse perspectives and the interconnectedness of all lifeforms and the planet.
On July 30, 1999, the Centers for Disease Control and Prevention published a report comparing data on the control of infectious disease from the beginning of the 20th century to the end. The data showed that deaths from infectious diseases declined markedly. In the early 1900s, pneumonia, tuberculosis and diarrheal diseases were the three leading killers, accounting for one-third of total deaths in the U.S.—with 40 percent being children under five.
Mass vaccinations, the discovery of antibiotics and overall sanitation and hygiene measures eventually eradicated smallpox, beat down polio, cured cholera, nearly rid the world of tuberculosis and extended the U.S. life expectancy by 25 years. By 1997, there was a shift in population health in the U.S. such that cancer, diabetes and heart disease were now the leading causes of death.
The control of infectious diseases is considered to be one of the “10 Great Public Health Achievements.” Yet on the brink of the 21st century, new trouble was already brewing. Hospitals were seeing periodic cases of antibiotic-resistant infections. Novel viruses, or those that previously didn’t afflict humans, began to emerge, causing outbreaks of West Nile, SARS, MERS or swine flu.In the years that followed, tuberculosis made a comeback, at least in certain parts of the world. What we didn’t take into account was the very concept of evolution: as we built better protections, our enemies eventually boosted their attacking prowess, so soon enough we found ourselves on the defensive once again.
At the same time, new, previously unknown or extremely rare disorders began to rise, such as autoimmune or genetic conditions. Two decades later, scientists began thinking about health differently—not as a static achievement guaranteed to last, but as something dynamic and constantly changing—and sometimes, for the worse.
What emerged since then is a different paradigm that makes our interactions with the microbial world more like a biological chess match, says Victoria McGovern, a biochemist and program officer for the Burroughs Wellcome Fund’s Infectious Disease and Population Sciences Program. In this chess game, humans may make a clever strategic move, which could involve creating a new vaccine or a potent antibiotic, but that advantage is fleeting. At some point, the organisms we are up against could respond with a move of their own—such as developing resistance to medication or genetic mutations that attack our bodies. Simply eradicating the “opponent,” or the pathogenic microbes, as efficiently as possible isn’t enough to keep humans healthy long-term.
Instead, scientists should focus on studying the complexity of interactions between humans and their pathogens. “We need to better understand the lifestyles of things that afflict us,” McGovern says. “The solutions are going to be in understanding various parts of their biology so we can influence how they behave around our systems.”
Genetics and cell biology, combined with imaging techniques that allow one to see tissues and individual cells in actions, will enable scientists to define and quantify what it means to be healthy at the molecular level.
What is being proposed will require a pivot to basic biology and other disciplines that have suffered from lack of research funding in recent years. Yet, according to McGovern, the research teams of funded proposals are answering bigger questions. “We look for people exploring questions about hosts and pathogens, and what happens when they touch, but we’re also looking for people with big ideas,” she says. For example, if one specific infection causes a chain of pathological events in the body, can other infections cause them too? And if we find a way to break that chain for one pathogen, can we play the same trick on another? “We really want to see people thinking of not just one experiment but about big implications of their work,” McGovern says.
Jonah Cool, a cell biologist, geneticist and science officer at the Chan Zuckerberg Initiative, says that it’s necessary to define what constitutes a healthy organism and how it overcomes infections or environmental assaults, such as pollution from forest fires or toxins from industrial smokestacks. An organism that catches a disease isn’t necessarily an unhealthy one, as long as it fights it off successfully—an ability that arises from the complex interplay of its genes, the immune system, age, stress levels and other factors. Modern science allows many of these factors to be measured, recorded and compared. “We need a data-driven, deep-phenotyping approach to defining healthy biological systems and their responses to insults—which can be infectious disease or environmental exposures—and their ability to navigate their way through that space,” Cool says.
Genetics and cell biology, combined with imaging techniques that allow one to see tissues and individual cells in actions, will enable scientists to define and quantify what it means to be healthy at the molecular level. “As a geneticist and cell biologist, I believe in all these molecular underpinnings and how they arise in phenotypic differences in cells, genes, proteins—and how their combinations form complex cellular states,” Cool says.
Julie Graves, a physician, public health consultant, former adjunct professor of management, policy and community health at the University of Texas Health Science Center in Houston, stresses the necessity of nutritious diets. According to the Rockefeller Food Initiative, “poor diet is the leading risk factor for disease, disability and premature death in the majority of countries around the world.” Adequate nutrition is critical for maintaining human health and life. Yet, Western diets are often low in essential nutrients, high in calories and heavy on processed foods. Overconsumption of these foods has contributed to high rates of obesity and chronic disease in the U.S. In fact, more than half of American adults have at least one chronic disease, and 27 percent have more than one—which increases vulnerability to COVID-19 infections, according to the 2018 National Health Interview Survey.
Further, the contamination of our food supply with various agricultural and industrial toxins—petrochemicals, pesticides, PFAS and others—has implications for morbidity, mortality, and overall quality of life. “These chemicals are insidiously in everything, including our bodies,” Graves says—and they are interfering with our normal biological functions. “We need to stop how we manufacture food,” she adds, and rid our sustenance of these contaminants.
According to the Humane Society of the United States, factory farms result in nearly 40 percent of emissions of methane. Concentrated animal feeding operations or CAFOs may serve as breeding grounds for pandemics, scientists warn, so humans should research better ways to raise and treat livestock. Diego Rose, a professor of food and nutrition policy at Tulane University School of Public Health & Tropical Medicine, and his colleagues found that “20 percent of Americans’ diets account for about 45 percent of the environmental impacts [that come from food].” A subsequent study explored the impacts of specific foods and found that substituting beef for chicken lowers an individual’s carbon footprint by nearly 50 percent, with water usage decreased by 30 percent. Notably, however, eating too much red meat has been associated with a variety of illnesses.
In some communities, the option to swap food types is limited or impossible. For example, “many populations live in relative food deserts where there’s not a local grocery store that has any fresh produce,” says Louis Muglia, the president and CEO of Burroughs Wellcome. Individuals in these communities suffer from an insufficient intake of beneficial macronutrients, and they’re “probably being exposed to phenols and other toxins that are in the packaging.” An equitable, sustainable and nutritious food supply will be vital to humanity’s wellbeing in the era of climate change, unpredictable weather and spillover events.
A recent report by See Change Institute and the Climate Mental Health Network showed that people who are experiencing socioeconomic inequalities, including many people of color, contribute the least to climate change, yet they are impacted the most. For example, people in low-income communities are disproportionately exposed to vehicle emissions, Muglia says. Through its Climate Change and Human Health Seed Grants program, Burroughs Wellcome funds research that aims to understand how various factors related to climate change and environmental chemicals contribute to premature births, associated with health vulnerabilities over the course of a person’s life—and map such hot spots.
“It’s very complex, the combinations of socio-economic environment, race, ethnicity and environmental exposure, whether that’s heat or toxic chemicals,” Muglia explains. “Disentangling those things really requires a very sophisticated, multidisciplinary team. That’s what we’ve put together to describe where these hotspots are and see how they correlate with different toxin exposure levels.”
In addition to mapping the risks, researchers are developing novel therapeutics that will be crucial to our armor arsenal, but we will have to be smarter at designing and using them. We will need more potent, better-working monoclonal antibodies. Instead of directly attacking a pathogen, we may have to learn to stimulate the immune system—training it to fight the disease-causing microbes on its own. And rather than indiscriminately killing all bacteria with broad-scope drugs, we would need more targeted medications. “Instead of wiping out the entire gut flora, we will need to come up with ways that kill harmful bacteria but not healthy ones,” Graves says. Training our immune systems to recognize and react to pathogens by way of vaccination will keep us ahead of our biological opponents, too. “Continued development of vaccines against infectious diseases is critical,” says Graves.
With all of the unpredictable events that lie ahead, it is difficult to foresee what achievements in public health will be reported at the end of the 21st century. Yet, technological advances, better modeling and pursuing bigger questions in science, along with education and working closely with communities will help overcome the challenges. The Chan Zuckerberg Initiative displays an optimistic message on its website: “Is it possible to cure, prevent, or manage all diseases by the end of this century? We think so.” Cool shares the view of his employer—and believes that science can get us there. Just give it some time and a chance. “It’s a big, bold statement,” he says, “but the end of the century is a long way away.”Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.
Alzheimer’s prevention may be less about new drugs, more about income, zip code and education
(Left to right) Vickie Naylor, Bernadine Clay, and Donna Maxey read a memory prompt as they take part in the Sharing History through Active Reminiscence and Photo-Imagery (SHARP) study, September 20, 2017.
That your risk of Alzheimer’s disease depends on your salary, what you ate as a child, or the block where you live may seem implausible. But researchers are discovering that social determinants of health (SDOH) play an outsized role in Alzheimer’s disease and related dementias, possibly more than age, and new strategies are emerging for how to address these factors.
At the 2022 Alzheimer’s Association International Conference, a series of presentations offered evidence that a string of socioeconomic factors—such as employment status, social support networks, education and home ownership—significantly affected dementia risk, even when adjusting data for genetic risk. What’s more, memory declined more rapidly in people who earned lower wages and slower in people who had parents of higher socioeconomic status.
In 2020, a first-of-its kind study in JAMA linked Alzheimer’s incidence to “neighborhood disadvantage,” which is based on SDOH indicators. Through autopsies, researchers analyzed brain tissue markers related to Alzheimer’s and found an association with these indicators. In 2022, Ryan Powell, the lead author of that study, published further findings that neighborhood disadvantage was connected with having more neurofibrillary tangles and amyloid plaques, the main pathological features of Alzheimer's disease.
As of yet, little is known about the biological processes behind this, says Powell, director of data science at the Center for Health Disparities Research at the University of Wisconsin School of Medicine and Public Health. “We know the association but not the direct causal pathway.”
The corroborative findings keep coming. In a Nature study published a few months after Powell’s study, every social determinant investigated affected Alzheimer’s risk except for marital status. The links were highest for income, education, and occupational status.
Clinical trials on new Alzheimer’s medications get all the headlines but preventing dementia through policy and public health interventions should not be underestimated.
The potential for prevention is significant. One in three older adults dies with Alzheimer's or another dementia—more than breast and prostate cancers combined. Further, a 2020 report from the Lancet Commission determined that about 40 percent of dementia cases could theoretically be prevented or delayed by managing the risk factors that people can modify.
Take inactivity. Older adults who took 9,800 steps daily were half as likely to develop dementia over the next 7 years, in a 2022 JAMA study. Hearing loss, another risk factor that can be managed, accounts for about 9 percent of dementia cases.
Clinical trials on new Alzheimer’s medications get all the headlines but preventing dementia through policy and public health interventions should not be underestimated. Simply slowing the course of Alzheimer’s or delaying its onset by five years would cut the incidence in half, according to the Global Council on Brain Health.
Minorities Hit the Hardest
The World Health Organization defines SDOH as “conditions in which people are born, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life.”
Anyone who exists on processed food, smokes cigarettes, or skimps on sleep has heightened risks for dementia. But minority groups get hit harder. Older Black Americans are twice as likely to have Alzheimer’s or another form of dementia as white Americans; older Hispanics are about one and a half times more likely.
This is due in part to higher rates of diabetes, obesity, and high blood pressure within these communities. These diseases are linked to Alzheimer’s, and SDOH factors multiply the risks. Blacks and Hispanics earn less income on average than white people. This means they are more likely to live in neighborhoods with limited access to healthy food, medical care, and good schools, and suffer greater exposure to noise (which impairs hearing) and air pollution—additional risk factors for dementia.
Related Reading: The Toxic Effects of Noise and What We're Not Doing About it
Plus, when Black people are diagnosed with dementia, their cognitive impairment and neuropsychiatric symptom are more advanced than in white patients. Why? Some African-Americans delay seeing a doctor because of perceived discrimination and a sense they will not be heard, says Carl V. Hill, chief diversity, equity, and inclusion officer at the Alzheimer’s Association.
Misinformation about dementia is another issue in Black communities. The thinking is that Alzheimer’s is genetic or age-related, not realizing that diet and physical activity can improve brain health, Hill says.
African Americans are severely underrepresented in clinical trials for Alzheimer’s, too. So, researchers miss the opportunity to learn more about health disparities. “It’s a bioethical issue,” Hill says. “The people most likely to have Alzheimer’s aren’t included in the trials.”
The Cure: Systemic Change
People think of lifestyle as a choice but there are limitations, says Muniza Anum Majoka, a geriatric psychiatrist and assistant professor of psychiatry at Yale University, who published an overview of SDOH factors that impact dementia. “For a lot of people, those choices [to improve brain health] are not available,” she says. If you don’t live in a safe neighborhood, for example, walking for exercise is not an option.
Hill wants to see the focus of prevention shift from individual behavior change to ensuring everyone has access to the same resources. Advice about healthy eating only goes so far if someone lives in a food desert. Systemic change also means increasing the number of minority physicians and recruiting minorities in clinical drug trials so studies will be relevant to these communities, Hill says.
Based on SDOH impact research, raising education levels has the most potential to prevent dementia. One theory is that highly educated people have a greater brain reserve that enables them to tolerate pathological changes in the brain, thus delaying dementia, says Majoka. Being curious, learning new things and problem-solving also contribute to brain health, she adds. Plus, having more education may be associated with higher socioeconomic status, more access to accurate information and healthier lifestyle choices.
New Strategies
The chasm between what researchers know about brain health and how the knowledge is being applied is huge. “There’s an explosion of interest in this area. We’re just in the first steps,” says Powell. One day, he predicts that physicians will manage Alzheimer’s through precision medicine customized to the patient’s specific risk factors and needs.
Raina Croff, assistant professor of neurology at Oregon Health & Science University School of Medicine, created the SHARP (Sharing History through Active Reminiscence and Photo-imagery) walking program to forestall memory loss in African Americans with mild cognitive impairment or early dementia.
Participants and their caregivers walk in historically black neighborhoods three times a week over six months. A smart tablet provides information about “Memory Markers” they pass, such as the route of a civil rights march. People celebrate their community and culture while “brain health is running in the background,” Croff says.

Photos and memory prompts engage participants in the SHARP program.
OHSU/Kristyna Wentz-Graff
The project began in 2015 as a pilot study in Croff’s hometown of Portland, Ore., expanded to Seattle, and will soon start in Oakland, Calif. “Walking is good for slowing [brain] decline,” she says. A post-study assessment of 40 participants in 2017 showed that half had higher cognitive scores after the program; 78 percent had lower blood pressure; and 44 percent lost weight. Those with mild cognitive impairment showed the most gains. The walkers also reported improved mood and energy along with increased involvement in other activities.
It’s never too late to reap the benefits of working your brain and being socially engaged, Majoka says.
In Milwaukee, the Wisconsin Alzheimer’s Institute launched the The Amazing Grace Chorus® to stave off cognitive decline in seniors. People in early stages of Alzheimer’s practice and perform six concerts each year. The activity provides opportunities for social engagement, mental stimulation, and a support network. Among the benefits, 55 percent reported better communication at home and nearly half of participants said they got involved with more activities after participating in the chorus.
Private companies are offering intervention services to healthcare providers and insurers to manage SDOH, too. One such service, MyHello, makes calls to at-risk people to assess their needs—be it food, transportation or simply a friendly voice. Having a social support network is critical for seniors, says Majoka, noting there was a steep decline in cognitive function among isolated elders during Covid lockdowns.
About 1 in 9 Americans age 65 or older live with Alzheimer’s today. With a surge in people with the disease predicted, public health professionals have to think more broadly about resource targets and effective intervention points, Powell says.
Beyond breakthrough pills, that is. Like Dorothy in Kansas discovering happiness was always in her own backyard, we are beginning to learn that preventing Alzheimer’s is in our reach if only we recognized it.

