Americans Fell for a Theranos-Style Scam 100 Years Ago. Will We Ever Learn?

Medical scams like Theranos are as American as America itself.
The huckster understands what people want – an easy route to good health -- and figures out just how to provide it as long as no one asks too many questions.
"Americans are very much prone to this sort of thinking: Give me a pill or give me a magical bean that can make me lose weight!"
The keys to success: Hoopla, fancy technology, and gullibility. And oh yes, one more thing: a blood sample. Well, lots and lots of blood samples. Every testing fee counts.
Sound familiar? It could be the story of the preternaturally persuasive Elizabeth Holmes, the disgraced founder of Theranos who stands accused of perpetrating a massive blood-testing fraud. But this is a different story from a different time, one that dates back 100 years but sounds almost like it could unfold on the front page of The Wall Street Journal today.
The main difference: Back then, watchdogs thought they'd be able to vanquish fake medicine and scam science. Fat chance, it turned out. It seems like we're more likely to lose-weight-quick than make much of a dent into quackery and health fraud.
Why? Have we learned anything at all over the past century? As we sweep into a new decade, experts says we're not as advanced as we'd like to think. But the fight against fraud and fakery continues.
Quackery: As American As America Itself
In the 17th century, British healers of questionable reputation got a new name -- "quack," from the Dutch word "quacksalver," which originally referred to someone who treats others with home remedies but developed a new meaning along the lines of "charlatan." And these quacks got a new place to sell their wares: the American colonies.
By 1692, a Boston newspaper advertised a patent medicine that promised to cure "the Griping of the Guts, and the Wind Cholick" and – for good measure – "preventeth that woeful Distemper of the Dry Belly Ach." A couple centuries later, the most famous woman in the United States wasn't a first lady or feminist but a hawker of nostrums named Lydia Estes Pinkham whose "vegetable compound" promised to banish "female complaints." One advertisement suggested that the "sure cure" would have saved the life of a Connecticut clergyman whose wife killed him after suffering from feminine maladies for 16 years.
By the early 20th century, Americans were fascinated by electricity and radiation, and both healers and hucksters embraced the new high-tech era. Men with flagging libidos, for example, could irradiate their private parts with the radioactive Radiendocrinator or buy battery-powered electric belts equipped with dangling bits to supercharge their, um, dangling bits.
The Rise of the Radio Wave 'Cure'
Enter radionics, the (supposed) science of better health via radio waves. The idea was that "healthy people radiate healthy energy," and sickness could be reversed through diagnosis and re-tuning, write Dr. Lydia Kang and Nate Pedersen in their 2017 book "Quackery: A Brief History of the Worst Ways to Cure Everything."
Detecting illness and fixing it required machinery -- Dynamizers, Radioclasts and Oscillocasts – that could cost hundreds of dollars each. Thousands of physicians bought them. Fortunately, they could work remotely, for a fee. The worried-and-potentially-unwell just needed to send a blood sample and, of course, a personal check.
Sting operations revealed radionics to be bogus. A skeptic sent a blood sample to one radionics practitioner in Albuquerque who reported back with news of an infected fallopian tube. In fact, the blood sample came from a male guinea pig. As an American Medical Association leader reported, the guinea pig "had shown no female characteristics up to that time, and a postmortem examination yielded no evidence of ladylike attributes."
When Quackery Refused to Yield
The rise of bogus medical technology in the early 20th century spawned a watchdog industry as organizations like the American Medical Association swept into action, said medical historian Eric Boyle, author of 2012's "Quack Medicine: A History of Combating Health Fraud in Twentieth-Century America."
"When quackery was recognized as a major problem, the people who campaigned for its demise were confident that they could get rid of it," he said. "A lot of people believed that increased education, the truths of science, and laws designed to protect consumers would ultimately drive quackery from the marketplace. And then throughout the century, as modern medicine developed, and more effectively treated one disease after another, many observers remained confident in that prediction."
There's a bid to "flood the information highway with truth to turn the storm of fake promotional stuff into a trickle."
But fake medicine persisted as Americans continued their quest to get- healthy-quick… or get-rich-quick by promising to help others to get- healthy-quick. Even radionics refused to die. It's still around in various forms. And, as the Theranos scandal reveals, we're still hoping our blood can offer the keys to longevity and good health.
Why Do We Still Fall for Scams?
In our own era, the Theranos company rose to prominence when founder and CEO Elizabeth Holmes convinced journalists and investors that she'd found a way to cheaply test drops of blood for hundreds of conditions. Then it all fell apart, famously, when the world learned that the technology didn't work. The company has folded, and Holmes faces a federal trial on fraud charges this year.
"There were a lot of prominent, very smart people who bought into the myth of Elizabeth Holmes," a former employee told "60 Minutes," even though the blood tests never actually worked as advertised.
Shouldn't "prominent, very smart people" know better? "People are gullible," said Dr. Stephen Barrett, a psychiatrist and leading quack-buster who runs the QuackWatch website. But there's more to the story. According to him, we're uniquely vulnerable as individuals to bogus medicine.
Scam artists specifically pinpoint their target audiences, such as "smart people," desperate people and alienated people, he said.
Smart people, for example, might be overconfident about their ability to detect fraud and fall for bogus medicine. Alienated people may distrust the establishment, whether it's the medical field or government watchdogs, and be more receptive to alternative sources of information.
Dr. Barrett also points a finger at magical thinking, which comes in different forms. It could mean a New Age-style belief that our minds can control the world around us. Or, as professional quack-buster Alex Berezow said, it could refer to "our cultural obsession with quick fixes."
"Americans are very much prone to this sort of thinking: Give me a pill or give me a magical bean that can make me lose weight! But complex problems need complex solutions," said Berezow, a microbiologist who debunks junk science in his job as a spokesman for the American Council on Science & Health.
American mistrust of expertise makes matters worse, he said. "When I tell people they need to get vaccinated, I'm called a shill for the pharmaceutical industry," he said. "If I say dietary supplements generally don't work, I'm a shill for doctors who want to keep people sick."
What can ordinary citizens do to protect themselves from fake medicine? "You have to have a healthy skepticism of everything," Berezow said. "When you come across something new, is someone trying to take advantage of you? It's a horrible way to think about the world, but there's some truth to it."
"Like any chronic disease, we will have to live with it while we do our best to fight it."
The government and experts have their own roles to play via regulation and education, respectively. For all the criticism it gets, the Food & Drug Administration does serve as a bulwark against fakery in prescription medicine. And while celebrities like Gwyneth "Goop" Paltrow hawk countless questionable medical products on the Internet, scientists and physicians are fighting back by using social media as a tool to promote the truth. There's a bid to "flood the information highway with truth to turn the storm of fake promotional stuff into a trickle," said Dr. Randi Hutter Epstein, a writer in residence at Yale School of Medicine and author of 2018's "Aroused: The History of Hormones and How They Control Just About Everything."
What's next? Like death, taxes and Cher, charlatans are likely to always be with us. Boyle quoted the late William Jarvis, a pioneering quack-buster in the late 20th century who believed health fraud would never be eradicated: "Like any chronic disease, we will have to live with it while we do our best to fight it."
The Promise of Pills That Know When You Swallow Them
A woman prepares to swallow a digital pill that can track whether she has taken her medication.
Dr. Sara Browne, an associate professor of clinical medicine at the University of California, San Diego, is a specialist in infectious diseases and, less formally, "a global health person." She often travels to southern Africa to meet with colleagues working on the twin epidemics of HIV and tuberculosis.
"This technology, in my opinion, is an absolute slam dunk for tuberculosis."
Lately she has asked them to name the most pressing things she can help with as a researcher based in a wealthier country. "Over and over and over again," she says, "the only thing they wanted to know is whether their patients are taking the drugs."
Tuberculosis is one of world's deadliest diseases; every year there are 10 million new infections and more than a million deaths. When a patient with tuberculosis is prescribed medicine to combat the disease, adherence to the regimen is important not just for the individual's health, but also for the health of the community. Poor adherence can lead to lengthier and more costly treatment and, perhaps more importantly, to drug-resistant strains of the disease -- an increasing global threat.
Browne is testing a new method to help healthcare workers track their patients' adherence with greater precision—close to exact precision even. They're called digital pills, and they involve a patient swallowing medicine as they normally would, only the capsule contains a sensor that—when it contacts stomach acid—transmits a signal to a small device worn on or near the body. That device in turn sends a signal to the patient's phone or tablet and into a cloud-based database. The fact that the pill has been swallowed has therefore been recorded almost in real time, and notice is available to whoever has access to the database.
"This technology, in my opinion, is an absolute slam dunk for tuberculosis," Browne says. TB is much more prevalent in poorer regions of the world—in Sub-Saharan Africa, for example—than in richer places like the U.S., where Browne's studies thus far have taken place. But when someone is diagnosed in the U.S., because of the risk to others if it spreads, they will likely have to deal with "directly observed therapy" to ensure that they take their medicines correctly.
DOT, as it's called, requires the patient to meet with a healthcare worker several days a week, or every day, so that the medicine intake can be observed in person -- an expensive and time-consuming process. Still, the Centers for Disease Control and Prevention website says (emphasis theirs), "DOT should be used for ALL patients with TB disease, including children and adolescents. There is no way to accurately predict whether a patient will adhere to treatment without this assistance."
Digital pills can help with both the cost and time involved, and potentially improve adherence in places where DOT is impossibly expensive. With the sensors, you can monitor a patient's adherence without a healthcare worker physically being in the room. Patients can live their normal lives and if they miss a pill, they can receive a reminder by text or a phone call from the clinic or hospital. "They can get on with their lives," said Browne. "They don't need the healthcare system to interrupt them."
A 56-year-old patient who participated in one of Browne's studies when he was undergoing TB treatment says that before he started taking the digital pills, he would go to the clinic at least once every day, except weekends. Once he switched to digital pills, he could go to work and spend time with his wife and children instead of fighting traffic every day to get to the clinic. He just had to wear a small patch on his abdomen, which would send the signal to a tablet provided by Browne's team. When he returned from work, he could see the results—that he'd taken the pill—in a database accessed via the tablet. (He could also see his heart rate and respiratory rate.) "I could do my daily activities without interference," he said.
Dr. Peter Chai, a medical toxicologist and emergency medicine physician at Brigham and Women's Hospital in Boston, is studying digital pills in a slightly different context, to help fight the country's opioid overdose crisis. Doctors like Chai prescribe pain medicine, he says, but then immediately put the onus on the patient to decide when to take it. This lack of guidance can lead to abuse and addiction. Patients are often told to take the meds "as needed." Chai and his colleagues wondered, "What does that mean to patients? And are people taking more than they actually need? Because pain is such a subjective experience."
The patients "liked the fact that somebody was watching them."
They wanted to see what "take as needed" actually led to, so they designed a study with patients who had broken a bone and come to the hospital's emergency department to get it fixed. Those who were prescribed oxycodone—a pharmaceutical opioid for pain relief—got enough digital pills to last one week. They were supposed to take the pills as needed, or as many as three pills per day. When the pills were ingested, the sensor sent a signal to a card worn on a lanyard around the neck.
Chai and his colleagues were able to see exactly when the patients took the pills and how many, and to detect patterns of ingestion more precisely than ever before. They talked to the patients after the seven days were up, and Chai said most were happy to be taking digital pills. The patients saw it as a layer of protection from afar. "They liked the fact that somebody was watching them," Chai said.
Both doctors, Browne and Chai, are in early stages of studies with patients taking pre-exposure prophylaxis, medicines that can protect people with a high-risk of contracting HIV, such as injectable drug users. Without good adherence, patients leave themselves open to getting the virus. If a patient is supposed to take a pill at 2 p.m. but the digital pill sensor isn't triggered, the healthcare provider can have an automatic message sent as a reminder. Or a reminder to one of the patient's friends or loved ones.
"Like Swallowing Your Phone"?
Deven Desai, an associate professor of law and ethics at Georgia Tech, says that digital pills sound like a great idea for helping with patient adherence, a big issue that self-reporting doesn't fully solve. He likes the idea of a physician you trust having better information about whether you're taking your medication on time. "On the surface that's just cool," he says. "That's a good thing." But Desai, who formerly worked as academic research counsel at Google, said that some of the same questions that have come up in recent years with social media and the Internet in general also apply to digital pills.
"Think of it like your phone, but you swallowed it," he says. "At first it could be great, simple, very much about the user—in this case, the patient—and the data is going between you and your doctor and the medical people it ought to be going to. Wonderful. But over time, phones change. They become 'smarter.'" And when phones and other technologies become smarter, he says, the companies behind them tend to expand the type of data they collect, because they can. Desai says it will be crucial that prescribers be completely transparent about who is getting the patients' data and for what purpose.
"We're putting stuff in our body in good faith with our medical providers, and what if it turned out later that all of a sudden someone was data mining or putting in location trackers and we never knew about that?" Desai asks. "What science has to realize is if they don't start thinking about this, what could be a wonderful technology will get killed."
Leigh Turner, an associate professor at the University of Minnesota's Center for Bioethics, agrees with Desai that digital pills have great promise, and also that there are clear reasons to be concerned about their use. Turner compared the pills to credit cards and social media, in that the data from them can potentially be stolen or leaked. One question he would want answered before the pills were normalized: "What kind of protective measures are in place to make sure that personal information isn't spilling out and being acquired by others or used by others in unexpected and unwanted ways?"
If digital pills catch on, some experts worry that they may one day not be a voluntary technology.
Turner also wonders who will have access to the pills themselves. Only those who can afford both the medicine plus the smartphones that are currently required for their use? Or will people from all economic classes have access? If digital pills catch on, he also worries they may one day not be a voluntary technology.
"When it comes to digital pills, it's not something that's really being foisted on individuals. It's more something that people can be informed of and can choose to take or not to take," he says. "But down the road, I can imagine a scenario where we move away from purely voluntary agreements to it becoming more of an expectation."
He says it's easy to picture a scenario in which insurance companies demand that patient medicinal intake data be tracked and collected or else. Refuse to have your adherence tracked and you risk higher rates or even overall coverage. Maybe patients who don't take the digital pills suffer dire consequences financially or medically. "Maybe it becomes beneficial as much to health insurers and payers as it is to individual patients," Turner says.
In November 2017, the FDA approved the first-ever digital pill that includes a sensor, a drug called Abilify MyCite, made by Otsuka Pharmaceutical Company. The drug, which is yet to be released, is used to treat schizophrenia, bipolar disorder, and depression. With a built-in sensor developed by Proteus Digital Health, patients can give their doctors permission to see when exactly they are taking, or not taking, their meds. For patients with mental illness, the ability to help them stick to their prescribed regime can be life-saving.
But Turner wonders if Abilify is the best drug to be a forerunner for digital pills. Some people with schizophrenia might be suffering from paranoia, and perhaps giving them a pill developed by a large corporation that sends data from their body to be tracked by other people might not be the best idea. It could in fact exacerbate their sense of paranoia.
The Bottom Line: Protect the Data
We all have relatives who have pillboxes with separate compartments for each day of the week, or who carry pillboxes that beep when it's time to take the meds. But that's not always good enough for people with dementia, mental illness, drug addiction, or other life situations that make it difficult to remember to take their pills. Digital pills can play an important role in helping these people.
"The absolute principle here is that the data has to belong to the patient."
The one time the patient from Browne's study forgot to take his pills, he got a beeping reminder from his tablet that he'd missed a dose. "Taking a medication on a daily basis, sometimes we just forget, right?" he admits. "With our very accelerated lives nowadays, it helps us to remember that we have to take the medications. So patients are able to be on top of their own treatment."
Browne is convinced that digital pills can help people in developing countries with high rates of TB and HIV, though like Turner and Desai she cautions that patients' data must be protected. "I think it can be a tremendous technology for patient empowerment and I also think if properly used it can help the medical system to support patients that need it," she said. "But the absolute principle here is that the data has to belong to the patient."
Is Sex for Reproduction About to Become Extinct?
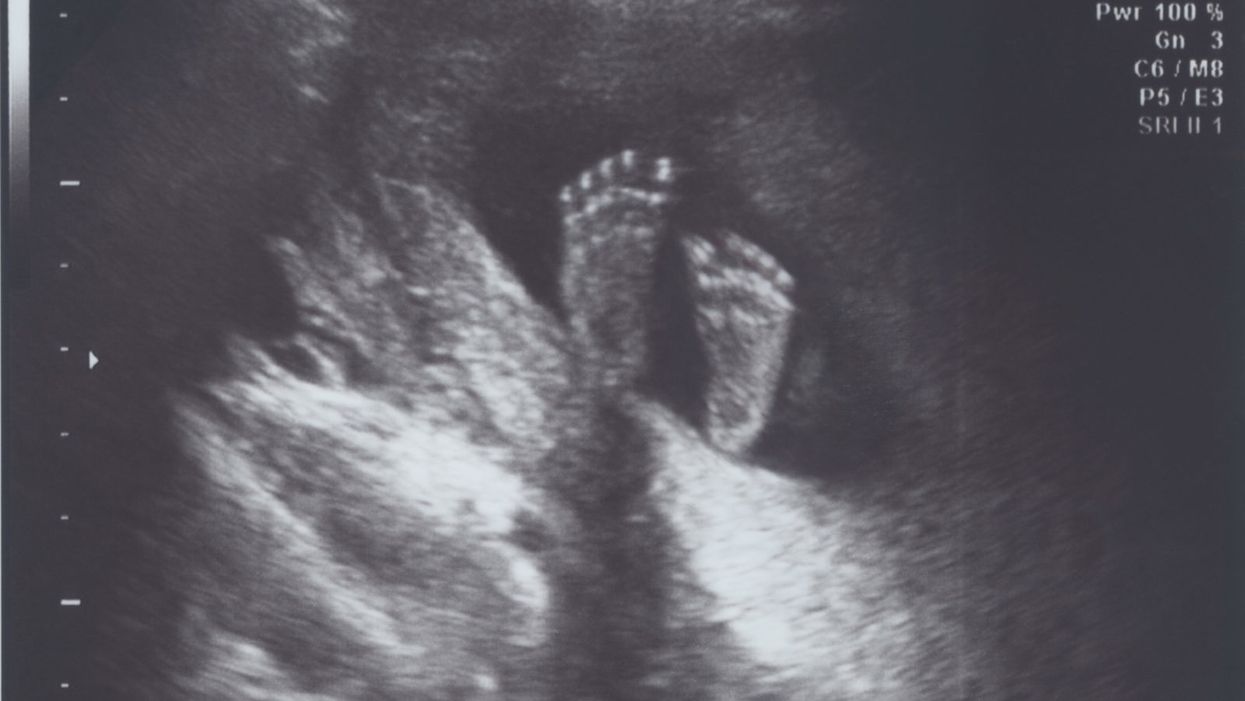
A healthy fetus in utero at 22 weeks.
There are lots of great reasons we humans have sex. We mostly do it to pair bond, realize our primal urges, and feel good. Once in a while, we also do it to make babies. As the coming genetic revolution plays out, we'll still have sex for most of the same reasons we do today. But we'll increasingly not do it to procreate.
Protecting children from harm is one of the core responsibilities of parenting.
Most parents go to great lengths to protect their children from real and imagined harms. This begins with taking prenatal vitamins during pregnancy and extends to having children immunized and protected from exposures to various diseases and dangers. Most of us look askance for good reason at mothers who abuse controlled substances during their pregnancies or parents who choose to not immunize their children. Protecting children from harm is one of the core responsibilities of parenting.
In the United States today, up to two percent of babies are estimated to be born with rare genetic diseases caused by single gene mutations. Sickle cell disease, Tay-Sachs, and Huntington's disease are among the more well-known examples of these, but the list runs to the thousands. Many babies born with these disorders suffer terribly, some die young, and nearly all spend big chunks of their lives struggling through the medical system.
Increasingly, however, many of these single-gene mutation diseases and other chromosomal disorders like Down syndrome are being identified in non-invasive prenatal tests performed on expectant mothers at the end of their first trimester of pregnancy. Knowing the hardship that children born with these types of disorders will likely face, majorities of these women in countries around the world are choosing to terminate pregnancies once these diagnoses have been made. Whatever the justification and whatever anyone's views on the morality of abortion, these decisions are inherently excruciating.
A much smaller number of prospective mothers, however, are today getting this same information about their potential future children before their pregnancies even begin. By undergoing both in vitro fertilization (IVF) and preimplantation genetic testing (PGT), these women are able to know which of the eggs that have been surgically extracted from them and fertilized with their partner or donor's sperm will carry the dangerous mutations. The in vitro embryos with these disorders are simply not implanted in the expectant mother's womb.
It would be monstrous to assert that an existing person with a deadly disease has any less right to thrive than anyone else. But it would also be hard to make a case that parents should affirmatively choose to implant embryos carrying such a disease if given the option. If prospective parents are already today choosing not to implant certain embryos based on our preliminary understanding of disease risk, what will happen when this embryo selection is based on far more information than just a few thousand single gene mutation diseases?
Our ability and willingness to make genetic alterations to our future children will grow over time along with our knowledge and technological ability.
When the first human genome was sequenced in 2003, the race to uncover the mysteries of human genetics had only just begun. Although we still know very little about our genetics relative to the complexity of the genome and even less compared to the broader ecosystem of our biology, the progress toward greater understanding is astounding. Today, the number of single gene mutation diseases and relatively simple genetic traits that can be predicted meaningfully from genetic data alone is already significant.
In the not-distant future, this list will grow to include complex diseases and disease propensities, percentage probabilities of living a long and healthy life, and increasingly the genetic component of complex human attributes like height, IQ, and personality style. This predictive power of genetic analysis will funnel straight into our fertility clinics where prospective parents choosing embryos will be making ever more consequential decisions about the genetic components of the future lives, health, and capabilities of their children.
Our understanding of what the genes extracted from early stage pre-implanted embryos are telling us will be only one of the rocket boosters driving assisted reproduction forward. Another will be the ability to induce adult cells like skin and nucleated blood cells into stem cells and then turn those stem cells into egg progenitor cells and then ultimately eggs. This will not only eliminate the need for hormone treatments and surgery to extract human eggs but also make it easy and cheap to generate an unlimited number of eggs from a given woman.
The average woman has around fifteen eggs extracted during IVF but imagine what generating a thousand eggs will do to the range of possibilities that could be realized through pre-implantation embryo selection. Each of these thousand eggs would be the natural offspring of the two parents, but the variation between them would make it possible to choose the ones with the strongest expression of the genetic component of a particular desired trait – like those with the highest possible genetic IQ potential.
Another rocket booster will be the application of gene editing technologies like CRISPR to edit the genomes of pre-implanted embryos or of the sperm and eggs used to create them. Just this week, Chinese researchers announced they had used CRISPR to edit the CCR5 gene in the pre-implanted embryos of a pair of Chinese twins to make them immune to HIV, the first ever case of gene editing humans and a harbinger of our genetically engineered future. The astounding complexity of the human genome will put limits on our ability to safely make too many simultaneous genetic changes to human embryos, but our ability and willingness to make these types of alterations to our future children will grow over time along with our knowledge and technological ability.
With so much at stake, prospective parents will increasingly have a stark choice when determining how to conceive their children. If they go the traditional route of sex, they will experience both the benign wisdom and unfathomable cruelty of nature. If they use IVF and increasingly informed embryo selection, they will eliminate most single gene mutation diseases and likely increase their children's chances of living a longer and healthier life with more opportunity than their unenhanced peers. But the optimizing parents could also set up their children for misery if these children don't particularly enjoy what they have been optimized to become or see themselves as some type of freakish consumer product with emotions.
Conceiving though sex will come to be seen more and more like not immunizing your children is today, a perfectly natural choice that comes with a significant potential risk and expense.
But although there will be pros and cons on each side, the fight between conception through good old-fashioned sex and conception in the lab will ultimately not be fair. Differences and competition within and between societies will pressure parents and societies to adopt ever more aggressive forms of reproductive technology if they believe doing so will open possibilities and create opportunities for the next generations rather than close them.
Conception through sex will remain as useful as it has always been but lab conception will only get more advantageous. Over time, only zealots will choose to roll the dice of their future children's health and well-being rather than invest, like parents always have, in protecting their children from harm and helping optimize their life potential. Conceiving though sex will come to be seen more and more like not immunizing your children is today, a perfectly natural choice that comes with a significant potential risk and expense to yourself, your children, and your community.
As this future plays out, the genetics and assisted reproduction revolutions will raise enormous, thorny, and massively consequential questions about how we value and invest in diversity, equality, and our own essential humanity – questions we aren't remotely prepared to answer. But these revolutions are coming sooner than most of us understand or are prepared for so we had better get ready.
Because where this trail is ultimately heading goes well beyond sex and toward a fundamental transformation of our evolutionary process as a species – and that should be everybody's business.