A Stomach Implant Saved Me. When Your Organs Fail, You Could Become a Cyborg, Too

Ordinary people are living better with chronic conditions thanks to a recent explosion of developments in medical implants.
Beware, cyborgs walk among us. They’re mostly indistinguishable from regular humans and are infiltrating every nook and cranny of society. For full disclosure, I’m one myself. No, we’re not deadly intergalactic conquerors like the Borg race of Star Trek fame, just ordinary people living better with chronic conditions thanks to medical implants.
In recent years there has been an explosion of developments in implantable devices that merge multiple technologies into gadgets that work in concert with human physiology for the treatment of serious diseases. Pacemakers for the heart are the best-known implants, as well as other cardiac devices like LVADs (left-ventricular assist devices) and implanted defibrillators. Next-generation devices address an array of organ failures, and many are intended as permanent. The driving need behind this technology: a critical, persistent shortage of implantable biological organs.
The demand for transplantable organs dwarfs their availability. There are currently over 100,000 people on the transplant waiting list in the U.S., compared to 40,000 transplants completed in 2021. But even this doesn’t reflect the number of people in dire straits who don’t qualify for a transplant because of things like frailty, smoking status and their low odds of surviving the surgery.
My journey to becoming a cyborg came about because of a lifelong medical condition characterized by pathologically low motility of the digestive system, called gastroparesis. Ever since I was in my teens, I’ve had chronic problems with severe nausea. Flareups can be totally incapacitating and last anywhere from hours to months, interspersed with periods of relief. The cycle is totally unpredictable, and for decades my condition went both un- and misdiagnosed by doctors who were not even aware that the condition existed. Over the years I was labeled with whatever fashionable but totally inappropriate medical label existed at the time, and not infrequently, hypochondria.
Living with the gastric pacer is easy. In fact, most of the time, I don’t even know it’s there.
One of the biggest turning points in my life came when a surgeon at the George Washington University Hospital, Dr. Frederick Brody, ordered a gastric emptying test that revealed gastroparesis. This was in 2009, and an implantable device, called a gastric pacer, had been approved by the FDA for compassionate use, meaning that no other treatments were available. The small device is like a pacemaker that’s implanted beneath the skin of the abdomen and is attached to the stomach through electrodes that carry electrical pulses that stimulate the stomach, making it contract as it’s supposed to.
Dr. Brody implanted the electrical wires and the device, and, once my stomach started to respond to the pulses, I got the most significant nausea relief I’d had in decades of futile treatments. It sounds cliché to say that my debt to Dr. Brody is immeasurable, but the pacer has given me more years of relative normalcy than I previously could have dreamed of.
I should emphasize that the pacer is not a cure. I still take a lot of medicine and have to maintain a soft, primarily vegetarian diet, and the condition has progressed with age. I have ups and downs, and can still have periods of severe illness, but there’s no doubt I would be far worse off without the electrical stimulation provided by the pacer.
Living with the gastric pacer is easy. In fact, most of the time, I don’t even know it’s there. It entails periodic visits with a surgeon who can adjust the strength of the electrical pulses using a wireless device, so when symptoms are worse, he or she can amp up the juice. If the pulses are too strong, they can cause annoying contractions in the abdominal muscles, but this is easily fixed with a simple wireless adjustment. The battery runs down after a few years, and when this happens the whole device has to be replaced in what is considered minor surgery.
Such devices could fill gaps in treating other organ failures. By far most of the people on transplant waiting lists are waiting for kidneys. Despite the fact that live donations are possible, there’s still a dire shortage of organs. A bright spot on the horizon is The Kidney Project, a program spearheaded by bioengineer Shuvo Roy at the University of California, San Francisco, which is developing a fully implantable artificial kidney. The device combines living cells with artificial materials and relies not on a battery, but on the patient’s own blood pressure to keep it functioning.
Several years into this project, a prototype of the kidney, about the size of a smart phone, has been successfully tested in pigs. The device seems to provide many of the functions of a biological kidney (unlike dialysis, which replaces only one main function) and reliably produces urine. One of its most critical components is a special artificial membrane, called a hemofilter, that filters out toxins and waste products from the blood without leaking important molecules like albumin. Since it allows for total mobility, the artificial kidney will provide patients with a higher quality of life than those on dialysis, and is in some important ways, even better than a biological transplant.
The beauty of the device is that, even though it contains kidney cells sourced, as of now, from cadavers or pigs, the cells are treated so that they can’t be rejected and the device doesn’t require the highly problematic immunosuppressant drugs a biological organ requires. “Anti-rejection drugs,” says Roy, “make you susceptible to all kinds of infections and damage the transplanted organ, causing steady deterioration. Eventually they kill the kidney. A biological transplant has about a 10-year limit,” after which the kidney fails and the body rejects it.
Eventually, says Roy, the cells used in the artificial kidney will be sourced from the patient himself, the ultimate genetic match. The patient’s adult stem cells can be used to produce some or all of the 25 to 30 specialized cells of a biological kidney that provide all the functions of a natural organ. People formerly on dialysis could drastically improve their functionality and quality of life without being tethered to a machine for hours at a time, three days a week.
As exciting as this project is, it suffers from a common theme in early biomedical research—keeping a steady stream of funding that will move the project from the lab, into human clinical trials and eventually to the bedside. “It’s the issue,” says Roy. “Potential investors want to see more data indicating that it works, but you need funding to create data. It’s a Catch-22 that puts you in a kind of no-man’s land of funding.” The constant pursuit of funding introduces a variable that makes it hard to predict when the kidney will make it to market, despite the enormous need for such a technology.
Another critical variable is if and when insurance companies will decide to cover transplants with the artificial kidney, so that it becomes affordable for the average person. But Roy thinks that this hurdle, too, will be crossed. Insurance companies stand to save a great deal of money compared to what they ordinarily spend on transplant patients. The cost of yearly maintenance will be a fraction of that associated with the tens of thousands of dollars for immunosuppressant drugs and the attendant complications associated with a biological transplant.
One estimate that the multidisciplinary team of researchers involved with The Kidney Project are still trying to establish is how long the artificial kidney will last once transplanted into the body. Animal trials so far have been looking at how the kidney works for 30 days, and will soon extend that study to 90 days. Additional studies will extend much farther into the future, but first the kidneys have to be implanted into people who can be followed over many years to answer this question. But unlike the gastric pacer and other implants, there won’t be a need for periodic surgeries to replace a depleted battery, and the stark improvements in quality of life compared to dialysis add a special dimension to the value of whatever time the kidney lasts.
Another life-saving implant could address a major scourge of the modern world—heart disease. Despite significant advances in recent decades, including the cardiac implants mentioned above, cardiovascular disease still causes one in three deaths across the world. One of the most promising developments in recent years is the Total Artificial Heart, a pneumatically driven device that can be used in patients with biventricular heart failure, affecting both sides of the heart, when a biological organ is not available.
The TAH is implanted in the chest cavity and has two tubes that snake down the body, come out through the abdomen and attach to a 13.5-pound external driver that the patient carries around in a backpack. It was first developed as a bridge to transplant, a temporary alternative while the patient waited for a biological heart to replace it. However, SynCardia Systems, LLC, the Tucson-based company that makes it, is now investigating whether the heart can be used on a long-term basis.
There’s good reason to think that this will be the case. I spoke with Daniel Teo, one of the board members of SynCardia, who said that so far, one patient lived with the TAH for six years and nine months, before he died of other causes. Another patient, still alive, has lived with the device for over five years and another one has lived with it for over four years. About 2,000 of these transplants have been done in patients waiting for biological hearts so far, and most have lived mobile, even active lives. One TAH recipient hiked for 600 miles, and another ran the 4.2-mile Pat Tillman Run, both while on the artificial heart. This is a far cry from their activities before surgery, while living with advanced heart failure.

Randy Shepard, a recipient of the Total Artificial Heart, teaches archery to his son.
Randy Shepard
If removing and replacing one’s biological heart with a synthetic device sounds scary, it is. But then so is replacing one’s heart with biological one. “The TAH is very emotionally loaded for most people,” says Teo. “People sometimes hold back because of philosophical, existential questions and other nonmedical reasons.” He also cites cultural reasons why some people could be hesitant to accept an artificial heart, saying that some religions could frown upon it, just as they forbid other medical interventions.
The first TAHs that were approved were 70 cubic centimeters in size and fit into the chest cavities of men and larger women, but there’s now a smaller, 50 cc size meant for women and adolescents. The FDA first cleared the 70 cc heart as a bridge to transplant in 2004, and the 50 cc model received approval in 2014. SynCardia’s focus now is on seeking FDA approval to use the heart on a long-term basis. There are other improvements in the works.
One issue being refined deals with the external driver that holds the pneumatic device for moving the blood through a patient’s body. The two tubes connecting the driver to the heart entail openings in the skin that could get infected, and carrying the backpack is less than ideal. The driver also makes an audible sound that some people find disturbing. The next generation TAH will be quieter and involve wearing a smaller, lighter device on a belt rather than carrying the backpack. SynCardia is also working toward a fully implantable heart that wouldn’t require any external components and would contain an energy source that can be recharged wirelessly.
Teo says the jury is out as to whether artificial hearts will ever obviate the need for biological organs, but the world’s number one killer isn’t going away any time soon. “The heart is one of the strongest organs,” he says, “but it’s not made to last forever. If you live long enough, the heart will eventually fail, and heart failure leads to the failure of other organs like the kidney, the lungs and the liver.” As long as this remains the case and as long as the current direction of research continues, artificial organs are likely to play an ever larger part of our everyday lives.
Oh, wait. Maybe we cyborgs will take over the world after all.
Jamie Rettinger with his now fiance Amie Purnel-Davis, who helped him through the clinical trial.
Jamie Rettinger was still in his thirties when he first noticed a tiny streak of brown running through the thumbnail of his right hand. It slowly grew wider and the skin underneath began to deteriorate before he went to a local dermatologist in 2013. The doctor thought it was a wart and tried scooping it out, treating the affected area for three years before finally removing the nail bed and sending it off to a pathology lab for analysis.
"I have some bad news for you; what we removed was a five-millimeter melanoma, a cancerous tumor that often spreads," Jamie recalls being told on his return visit. "I'd never heard of cancer coming through a thumbnail," he says. None of his doctors had ever mentioned it either. "I just thought I was being treated for a wart." But nothing was healing and it continued to bleed.
A few months later a surgeon amputated the top half of his thumb. Lymph node biopsy tested negative for spread of the cancer and when the bandages finally came off, Jamie thought his medical issues were resolved.
Melanoma is the deadliest form of skin cancer. About 85,000 people are diagnosed with it each year in the U.S. and more than 8,000 die of the cancer when it spreads to other parts of the body, according to the Centers for Disease Control and Prevention (CDC).
There are two peaks in diagnosis of melanoma; one is in younger women ages 30-40 and often is tied to past use of tanning beds; the second is older men 60+ and is related to outdoor activity from farming to sports. Light-skinned people have a twenty-times greater risk of melanoma than do people with dark skin.
"When I graduated from medical school, in 2005, melanoma was a death sentence" --Diwakar Davar.
Jamie had a follow up PET scan about six months after his surgery. A suspicious spot on his lung led to a biopsy that came back positive for melanoma. The cancer had spread. Treatment with a monoclonal antibody (nivolumab/Opdivo®) didn't prove effective and he was referred to the UPMC Hillman Cancer Center in Pittsburgh, a four-hour drive from his home in western Ohio.
An alternative monoclonal antibody treatment brought on such bad side effects, diarrhea as often as 15 times a day, that it took more than a week of hospitalization to stabilize his condition. The only options left were experimental approaches in clinical trials.
Early research
"When I graduated from medical school, in 2005, melanoma was a death sentence" with a cure rate in the single digits, says Diwakar Davar, 39, an oncologist at UPMC Hillman Cancer Center who specializes in skin cancer. That began to change in 2010 with introduction of the first immunotherapies, monoclonal antibodies, to treat cancer. The antibodies attach to PD-1, a receptor on the surface of T cells of the immune system and on cancer cells. Antibody treatment boosted the melanoma cure rate to about 30 percent. The search was on to understand why some people responded to these drugs and others did not.
At the same time, there was a growing understanding of the role that bacteria in the gut, the gut microbiome, plays in helping to train and maintain the function of the body's various immune cells. Perhaps the bacteria also plays a role in shaping the immune response to cancer therapy.
One clue came from genetically identical mice. Animals ordered from different suppliers sometimes responded differently to the experiments being performed. That difference was traced to different compositions of their gut microbiome; transferring the microbiome from one animal to another in a process known as fecal transplant (FMT) could change their responses to disease or treatment.
When researchers looked at humans, they found that the patients who responded well to immunotherapies had a gut microbiome that looked like healthy normal folks, but patients who didn't respond had missing or reduced strains of bacteria.
Davar and his team knew that FMT had a very successful cure rate in treating the gut dysbiosis of Clostridioides difficile, a persistant intestinal infection, and they wondered if a fecal transplant from a patient who had responded well to cancer immunotherapy treatment might improve the cure rate of patients who did not originally respond to immunotherapies for melanoma.
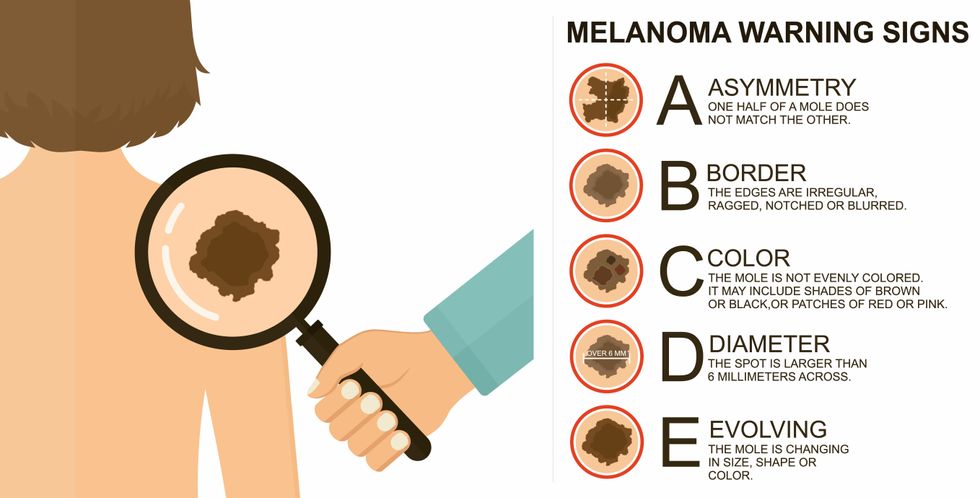
The ABCDE of melanoma detection
Adobe Stock
Clinical trial
"It was pretty weird, I was totally blasted away. Who had thought of this?" Jamie first thought when the hypothesis was explained to him. But Davar's explanation that the procedure might restore some of the beneficial bacterial his gut was lacking, convinced him to try. He quickly signed on in October 2018 to be the first person in the clinical trial.
Fecal donations go through the same safety procedures of screening for and inactivating diseases that are used in processing blood donations to make them safe for transfusion. The procedure itself uses a standard hollow colonoscope designed to screen for colon cancer and remove polyps. The transplant is inserted through the center of the flexible tube.
Most patients are sedated for procedures that use a colonoscope but Jamie doesn't respond to those drugs: "You can't knock me out. I was watching them on the TV going up my own butt. It was kind of unreal at that point," he says. "There were about twelve people in there watching because no one had seen this done before."
A test two weeks after the procedure showed that the FMT had engrafted and the once-missing bacteria were thriving in his gut. More importantly, his body was responding to another monoclonal antibody (pembrolizumab/Keytruda®) and signs of melanoma began to shrink. Every three months he made the four-hour drive from home to Pittsburgh for six rounds of treatment with the antibody drug.
"We were very, very lucky that the first patient had a great response," says Davar. "It allowed us to believe that even though we failed with the next six, we were on the right track. We just needed to tweak the [fecal] cocktail a little better" and enroll patients in the study who had less aggressive tumor growth and were likely to live long enough to complete the extensive rounds of therapy. Six of 15 patients responded positively in the pilot clinical trial that was published in the journal Science.
Davar believes they are beginning to understand the biological mechanisms of why some patients initially do not respond to immunotherapy but later can with a FMT. It is tied to the background level of inflammation produced by the interaction between the microbiome and the immune system. That paper is not yet published.
Surviving cancer
It has been almost a year since the last in his series of cancer treatments and Jamie has no measurable disease. He is cautiously optimistic that his cancer is not simply in remission but is gone for good. "I'm still scared every time I get my scans, because you don't know whether it is going to come back or not. And to realize that it is something that is totally out of my control."
"It was hard for me to regain trust" after being misdiagnosed and mistreated by several doctors he says. But his experience at Hillman helped to restore that trust "because they were interested in me, not just fixing the problem."
He is grateful for the support provided by family and friends over the last eight years. After a pause and a sigh, the ruggedly built 47-year-old says, "If everyone else was dead in my family, I probably wouldn't have been able to do it."
"I never hesitated to ask a question and I never hesitated to get a second opinion." But Jamie acknowledges the experience has made him more aware of the need for regular preventive medical care and a primary care physician. That person might have caught his melanoma at an earlier stage when it was easier to treat.
Davar continues to work on clinical studies to optimize this treatment approach. Perhaps down the road, screening the microbiome will be standard for melanoma and other cancers prior to using immunotherapies, and the FMT will be as simple as swallowing a handful of freeze-dried capsules off the shelf rather than through a colonoscopy. Earlier this year, the Food and Drug Administration approved the first oral fecal microbiota product for C. difficile, hopefully paving the way for more.
An older version of this hit article was first published on May 18, 2021
All organisms can repair damaged tissue, but none do it better than salamanders and newts. A surprising area of science could tell us how they manage this feat - and perhaps even help us develop a similar ability.
All organisms have the capacity to repair or regenerate tissue damage. None can do it better than salamanders or newts, which can regenerate an entire severed limb.
That feat has amazed and delighted man from the dawn of time and led to endless attempts to understand how it happens – and whether we can control it for our own purposes. An exciting new clue toward that understanding has come from a surprising source: research on the decline of cells, called cellular senescence.
Senescence is the last stage in the life of a cell. Whereas some cells simply break up or wither and die off, others transition into a zombie-like state where they can no longer divide. In this liminal phase, the cell still pumps out many different molecules that can affect its neighbors and cause low grade inflammation. Senescence is associated with many of the declining biological functions that characterize aging, such as inflammation and genomic instability.
Oddly enough, newts are one of the few species that do not accumulate senescent cells as they age, according to research over several years by Maximina Yun. A research group leader at the Center for Regenerative Therapies Dresden and the Max Planck Institute of Molecular and Cell Biology and Genetics, in Dresden, Germany, Yun discovered that senescent cells were induced at some stages of regeneration of the salamander limb, “and then, as the regeneration progresses, they disappeared, they were eliminated by the immune system,” she says. “They were present at particular times and then they disappeared.”
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states.
Previous research on senescence in aging had suggested, logically enough, that applying those cells to the stump of a newly severed salamander limb would slow or even stop its regeneration. But Yun stood that idea on its head. She theorized that senescent cells might also play a role in newt limb regeneration, and she tested it by both adding and removing senescent cells from her animals. It turned out she was right, as the newt limbs grew back faster than normal when more senescent cells were included.
Senescent cells added to the edges of the wound helped the healthy muscle cells to “dedifferentiate,” essentially turning back the developmental clock of those cells into more primitive states, which could then be turned into progenitors, a cell type in between stem cells and specialized cells, needed to regrow the muscle tissue of the missing limb. “We think that this ability to dedifferentiate is intrinsically a big part of why salamanders can regenerate all these very complex structures, which other organisms cannot,” she explains.
Yun sees regeneration as a two part problem. First, the cells must be able to sense that their neighbors from the lost limb are not there anymore. Second, they need to be able to produce the intermediary progenitors for regeneration, , to form what is missing. “Molecularly, that must be encoded like a 3D map,” she says, otherwise the new tissue might grow back as a blob, or liver, or fin instead of a limb.
Wound healing
Another recent study, this time at the Mayo Clinic, provides evidence supporting the role of senescent cells in regeneration. Looking closely at molecules that send information between cells in the wound of a mouse, the researchers found that senescent cells appeared near the start of the healing process and then disappeared as healing progressed. In contrast, persistent senescent cells were the hallmark of a chronic wound that did not heal properly. The function and significance of senescence cells depended on both the timing and the context of their environment.
The paper suggests that senescent cells are not all the same. That has become clearer as researchers have been able to identify protein markers on the surface of some senescent cells. The patterns of these proteins differ for some senescent cells compared to others. In biology, such physical differences suggest functional differences, so it is becoming increasingly likely there are subsets of senescent cells with differing functions that have not yet been identified.
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes.
Scientists initially thought that senescent cells couldn’t play a role in regeneration because they could no longer reproduce, says Anthony Atala, a practicing surgeon and bioengineer who leads the Wake Forest Institute for Regenerative Medicine in North Carolina. But Yun’s study points in the other direction. “What this paper shows clearly is that these cells have the potential to be involved in tissue regeneration [in newts]. The question becomes, will these cells be able to do the same in humans.”
As our knowledge of senescent cells increases, Atala thinks we need to embrace a new analogy to help understand them: humans in retirement. They “have acquired a lot of wisdom throughout their whole life and they can help younger people and mentor them to grow to their full potential. We're seeing the same thing with these cells,” he says. They are no longer putting energy into their own reproduction, but the signaling molecules they secrete “can help other cells around them to regenerate.”
There are disagreements within the research community as to whether newts have acquired their regenerative capacity through a unique evolutionary change, or if other animals, including humans, retain this capacity buried somewhere in their genes. If so, it seems that our genes are unable to express this ability, perhaps as part of a tradeoff in acquiring other traits. It is a fertile area of research.
Dedifferentiation is likely to become an important process in the field of regenerative medicine. One extreme example: a lab has been able to turn back the clock and reprogram adult male skin cells into female eggs, a potential milestone in reproductive health. It will be more difficult to control just how far back one wishes to go in the cell's dedifferentiation – part way or all the way back into a stem cell – and then direct it down a different developmental pathway. Yun is optimistic we can learn these tricks from newts.
Senolytics
A growing field of research is using drugs called senolytics to remove senescent cells and slow or even reverse disease of aging.
“Senolytics are great, but senolytics target different types of senescence,” Yun says. “If senescent cells have positive effects in the context of regeneration, of wound healing, then maybe at the beginning of the regeneration process, you may not want to take them out for a little while.”
“If you look at pretty much all biological systems, too little or too much of something can be bad, you have to be in that central zone” and at the proper time, says Atala. “That's true for proteins, sugars, and the drugs that you take. I think the same thing is true for these cells. Why would they be different?”
Our growing understanding that senescence is not a single thing but a variety of things likely means that effective senolytic drugs will not resemble a single sledge hammer but more a carefully manipulated scalpel where some types of senescent cells are removed while others are added. Combinations and timing could be crucial, meaning the difference between regenerating healthy tissue, a scar, or worse.

