How Excessive Regulation Helped Ignite COVID-19's Rampant Spread
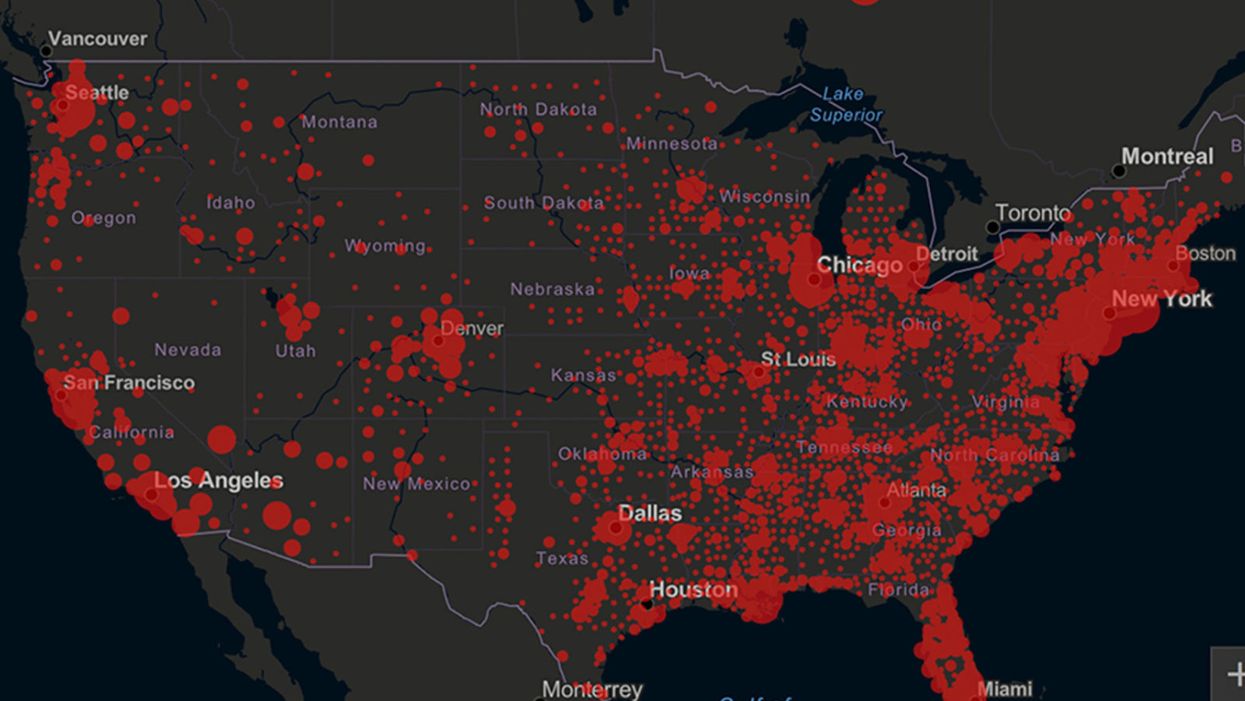
Screenshot of an interactive map of coronavirus cases across the United States, current as of 1:45 p.m. Pacific time on Tuesday, March 31st. Full map accessible at https://coronavirus.jhu.edu/map.html
When historians of the future look back at the 2020 pandemic, the heroic work of Helen Y. Chu, a flu researcher at the University of Washington, will be worthy of recognition.
Chu's team bravely defied the order and conducted the testing anyway.
In late January, Chu was testing nasal swabs for the Seattle Flu Study to monitor influenza spread when she learned of the first case of COVID-19 in Washington state. She deemed it a pressing public health matter to document if and how the illness was spreading locally, so that early containment efforts could succeed. So she sought regulatory approval to adapt the Flu Study to test for the coronavirus, but the federal government denied the request because the original project was funded to study only influenza.
Aware of the urgency, Chu's team bravely defied the order and conducted the testing anyway. Soon they identified a local case in a teenager without any travel history, followed by others. Still, the government tried to shutter their efforts until the outbreak grew dangerous enough to command attention.
Needless testing delays, prompted by excessive regulatory interference, eliminated any chances of curbing the pandemic at its initial stages. Even after Chu went out on a limb to sound alarms, a heavy-handed bureaucracy crushed the nation's ability to roll out early and widespread testing across the country. The Centers for Disease Control and Prevention infamously blundered its own test, while also impeding state and private labs from coming on board, fueling a massive shortage.
The long holdup created "a backlog of testing that needed to be done," says Amesh Adalja, an infectious disease specialist who is a senior scholar at the Johns Hopkins University Center for Health Security.
In a public health crisis, "the ideal situation" would allow the government's test to be "supplanted by private laboratories" without such "a lag in that transition," Adalja says. Only after the eventual release of CDC's test could private industry "begin in earnest" to develop its own versions under the Food and Drug Administration's emergency use authorization.
In a statement, CDC acknowledged that "this process has not gone as smoothly as we would have liked, but there is currently no backlog for testing at CDC."
Now, universities and corporations are in a race against time, playing catch up as the virus continues its relentless spread, also afflicting many health care workers on the front lines.
"Home-testing accessibility is key to preventing further spread of the COVID-19 pandemic."
Hospitals are attempting to add the novel coronavirus to the testing panel of their existent diagnostic machines, which would reduce the results processing time from 48 hours to as little as four hours. Meanwhile, at least four companies announced plans to deliver at-home collection tests to help meet the demand – before a startling injunction by the FDA halted their plans.
Everlywell, an Austin, Texas-based digital health company, had been set to launch online sales of at-home collection kits directly to consumers last week. Scaling up in a matter of days to an initial supply of 30,000 tests, Everlywell collaborated with multiple laboratories where consumers could ship their nasal swab samples overnight, projecting capacity to screen a quarter-million individuals on a weekly basis, says Frank Ong, chief medical and scientific officer.
Secure digital results would have been available online within 48 hours of a sample's arrival at the lab, as well as a telehealth consultation with an independent, board-certified doctor if someone tested positive, for an inclusive $135 cost. The test has a less than 3 percent false-negative rate, Ong says, and in the event of an inadequate self-swab, the lab would not report a conclusive finding. "Home-testing accessibility," he says, "is key to preventing further spread of the COVID-19 pandemic."
But on March 20, the FDA announced restrictions on home collection tests due to concerns about accuracy. The agency did note "the public health value in expanding the availability of COVID-19 testing through safe and accurate tests that may include home collection," while adding that "we are actively working with test developers in this space."
After the restrictions were announced, Everlywell decided to allocate its initial supply of COVID-19 collection kits to hospitals, clinics, nursing homes, and other qualifying health care companies that can commit to no-cost screening of frontline workers and high-risk symptomatic patients. For now, no consumers can order a home-collection test.
"Losing two months is close to disastrous, and that's what we did."
Currently, the U.S. has ramped up to testing an estimated 100,000 people a day, according to Stat News. But 150,000 or more Americans should be tested every day, says Ashish Jha, professor and director of the Harvard Global Health Institute. Due to the dearth of tests, many sick people who suspect they are infected still cannot get confirmation unless they need to be hospitalized.
To give a concrete sense of how far behind we are in testing, consider Palm Beach County, Fla. The state's only drive-thru test center just opened there, requiring an appointment. The center aims to test 750 people per day, but more than 330,000 people have already called to try to book a slot.
"This is such a rapidly moving infection that losing a few days is bad, and losing a couple of weeks is terrible," says Jha, a practicing general internist. "Losing two months is close to disastrous, and that's what we did."
At this point, it will take a long time to fully ramp up. "We are blindfolded," he adds, "and I'd like to take the blindfolds off so we can fight this battle with our eyes wide open."
Better late than never: Yesterday, FDA Commissioner Stephen Hahn said in a statement that the agency has worked with more than 230 test developers and has approved 20 tests since January. An especially notable one was authorized last Friday – 67 days since the country's first known case in Washington state. It's a rapid point-of-care test from medical-device firm Abbott that provides positive results in five minutes and negative results in 13 minutes. Abbott will send 50,000 tests a day to urgent care settings. The first tests are expected to ship tomorrow.
Fast for Longevity, with Less Hunger, with Dr. Valter Longo
Valter Longo, a biogerontologist at USC, and centenarian Rocco Longo (no relation) appear together in Italy in 2021. The elder Longo is from a part of Italy where people have fasted regularly and are enjoying long lifespans.
You’ve probably heard about intermittent fasting, where you don’t eat for about 16 hours each day and limit the window where you’re taking in food to the remaining eight hours.
But there’s another type of fasting, called a fasting-mimicking diet, with studies pointing to important benefits. For today’s podcast episode, I chatted with Dr. Valter Longo, a biogerontologist at the University of Southern California, about all kinds of fasting, and particularly the fasting-mimicking diet, which minimizes hunger as much as possible. Going without food for a period of time is an example of good stress: challenges that work at the cellular level to boost health and longevity.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
If you’ve ever spent more than a few minutes looking into fasting, you’ve almost certainly come upon Dr. Longo's name. He is the author of the bestselling book, The Longevity Diet, and the best known researcher of fasting-mimicking diets.
With intermittent fasting, your body might begin to switch up its fuel type. It's usually running on carbs you get from food, which gets turned into glucose, but without food, your liver starts making something called ketones, which are molecules that may benefit the body in a number of ways.
With the fasting-mimicking diet, you go for several days eating only types of food that, in a way, keep themselves secret from your body. So at the level of your cells, the body still thinks that it’s fasting. This is the best of both worlds – you’re not completely starving because you do take in some food, and you’re getting the boosts to health that come with letting a fast run longer than intermittent fasting. In this episode, Dr. Longo talks about the growing number of studies showing why this could be very advantageous for health, as long as you undertake the diet no more than a few times per year.
Dr. Longo is the director of the Longevity Institute at USC’s Leonard Davis School of Gerontology, and the director of the Longevity and Cancer program at the IFOM Institute of Molecular Oncology in Milan. In addition, he's the founder and president of the Create Cures Foundation in L.A., which focuses on nutrition for the prevention and treatment of major chronic illnesses. In 2016, he received the Glenn Award for Research on Aging for the discovery of genes and dietary interventions that regulate aging and prevent diseases. Dr. Longo received his PhD in biochemistry from UCLA and completed his postdoc in the neurobiology of aging and Alzheimer’s at USC.
Show links:
Create Cures Foundation, founded by Dr. Longo: www.createcures.org
Dr. Longo's Facebook: https://www.facebook.com/profvalterlongo/
Dr. Longo's Instagram: https://www.instagram.com/prof_valterlongo/
Dr. Longo's book: The Longevity Diet
The USC Longevity Institute: https://gero.usc.edu/longevity-institute/
Dr. Longo's research on nutrition, longevity and disease: https://pubmed.ncbi.nlm.nih.gov/35487190/
Dr. Longo's research on fasting mimicking diet and cancer: https://pubmed.ncbi.nlm.nih.gov/34707136/
Full list of Dr. Longo's studies: https://pubmed.ncbi.nlm.nih.gov/?term=Longo%2C+Valter%5BAuthor%5D&sort=date
Research on MCT oil and Alzheimer's: https://alz-journals.onlinelibrary.wiley.com/doi/f...
Keto Mojo device for measuring ketones
Silkworms with spider DNA spin silk stronger than Kevlar
Silkworm silk is fragile, which limits its uses, but a few extra genes can help.
Story by Freethink
The study and copying of nature’s models, systems, or elements to address complex human challenges is known as “biomimetics.” Five hundred years ago, an elderly Italian polymath spent months looking at the soaring flight of birds. The result was Leonardo da Vinci’s biomimetic Codex on the Flight of Birds, one of the foundational texts in the science of aerodynamics. It’s the science that elevated the Wright Brothers and has yet to peak.
Today, biomimetics is everywhere. Shark-inspired swimming trunks, gecko-inspired adhesives, and lotus-inspired water-repellents are all taken from observing the natural world. After millions of years of evolution, nature has quite a few tricks up its sleeve. They are tricks we can learn from. And now, thanks to some spider DNA and clever genetic engineering, we have another one to add to the list.
The elusive spider silk
We’ve known for a long time that spider silk is remarkable, in ways that synthetic fibers can’t emulate. Nylon is incredibly strong (it can support a lot of force), and Kevlar is incredibly tough (it can absorb a lot of force). But neither is both strong and tough. In all artificial polymeric fibers, strength and toughness are mutually exclusive, and so we pick the material best for the job and make do.
Spider silk, a natural polymeric fiber, breaks this rule. It is somehow both strong and tough. No surprise, then, that spider silk is a source of much study.The problem, though, is that spiders are incredibly hard to cultivate — let alone farm. If you put them together, they will attack and kill each other until only one or a few survive. If you put 100 spiders in an enclosed space, they will go about an aggressive, arachnocidal Hunger Games. You need to give each its own space and boundaries, and a spider hotel is hard and costly. Silkworms, on the other hand, are peaceful and productive. They’ll hang around all day to make the silk that has been used in textiles for centuries. But silkworm silk is fragile. It has very limited use.
The elusive – and lucrative – trick, then, would be to genetically engineer a silkworm to produce spider-quality silk. So far, efforts have been fruitless. That is, until now.
We can have silkworms creating silk six times as tough as Kevlar and ten times as strong as nylon.
Spider-silkworms
Junpeng Mi and his colleagues working at Donghua University, China, used CRISPR gene-editing technology to recode the silk-creating properties of a silkworm. First, they took genes from Araneus ventricosus, an East Asian orb-weaving spider known for its strong silk. Then they placed these complex genes – genes that involve more than 100 amino acids – into silkworm egg cells. (This description fails to capture how time-consuming, technical, and laborious this was; it’s a procedure that requires hundreds of thousands of microinjections.)
This had all been done before, and this had failed before. Where Mi and his team succeeded was using a concept called “localization.” Localization involves narrowing in on a very specific location in a genome. For this experiment, the team from Donghua University developed a “minimal basic structure model” of silkworm silk, which guided the genetic modifications. They wanted to make sure they had the exactly right transgenic spider silk proteins. Mi said that combining localization with this basic structure model “represents a significant departure from previous research.” And, judging only from the results, he might be right. Their “fibers exhibited impressive tensile strength (1,299 MPa) and toughness (319 MJ/m3), surpassing Kevlar’s toughness 6-fold.”
A world of super-materials
Mi’s research represents the bursting of a barrier. It opens up hugely important avenues for future biomimetic materials. As Mi puts it, “This groundbreaking achievement effectively resolves the scientific, technical, and engineering challenges that have hindered the commercialization of spider silk, positioning it as a viable alternative to commercially synthesized fibers like nylon and contributing to the advancement of ecological civilization.”
Around 60 percent of our clothing is made from synthetic fibers like nylon, polyester, and acrylic. These plastics are useful, but often bad for the environment. They shed into our waterways and sometimes damage wildlife. The production of these fibers is a source of greenhouse gas emissions. Now, we have a “sustainable, eco-friendly high-strength and ultra-tough alternative.” We can have silkworms creating silk six times as tough as Kevlar and ten times as strong as nylon.
We shouldn’t get carried away. This isn’t going to transform the textiles industry overnight. Gene-edited silkworms are still only going to produce a comparatively small amount of silk – even if farmed in the millions. But, as Mi himself concedes, this is only the beginning. If Mi’s localization and structure-model techniques are as remarkable as they seem, then this opens up the door to a great many supermaterials.
Nature continues to inspire. We had the bird, the gecko, and the shark. Now we have the spider-silkworm. What new secrets will we unravel in the future? And in what exciting ways will it change the world?
This article originally appeared on Freethink, home of the brightest minds and biggest ideas of all time.


