I'm a Healthy Young Woman: Here's Why I Would Get Tested for Alzheimer's Now

The author as a child with her father in 1981, before he was diagnosed with Alzheimer's.
Editor's Note: A team of researchers in Italy recently used artificial intelligence and machine learning to diagnose Alzheimer's disease on a brain scan an entire decade before symptoms show up in the patient. While some people argue that early detection is critical, others believe the knowledge would do more harm than good. LeapsMag invited contributors with opposite opinions to share their perspectives.
Alzheimer's doesn't run in my family. When my father was diagnosed at the age of 58, we looked at his familial history. Both his parents lived into their late 80's. All of their surviving siblings were similarly long-lived and none had had Alzheimer's or any related dementias. My dad had spent 20 years working for the United Nations in the 60's and 70's in Africa. He was convinced that the Alzheimer's had come from his time spent in dodgy mines where he was exposed without the proper protections to all kinds of chemical processes.
Maybe that was true. Maybe it wasn't. The theory that metals, particularly aluminum, is an environmental factor leading to Alzheimer's has been around for a while. It's mostly been debunked, but clearly something is causing this epidemic as the vast majority of the cases in the world today are age-related. But no one knows what the trigger is, nor are we close to knowing.
If my father had had the Alzheimer's gene, I would go get myself checked for it. If some new MRI were commercially available to scan my brain and let me know if I was developing Alzheimer's, I would also take that test. There are four reasons why.
First, studies have shown that lifestyle has a major impact on the disease. I already run three miles a day. I eat relatively healthily. But like anyone, I don't live strictly on boiled chicken and broccoli. And I definitely enjoy a glass of wine or two. If I knew I had a propensity for the disease, or was developing it, I would be more diligent. I would eat my broccoli and cut out my wine. Life would be less fun, but I'd get more life and that's what's important.

The last picture taken of the author with her father before his death, in 2015.
Secondly, I would also have time to create an end-of-life plan the way my father did not. He told me repeatedly early on in his diagnosis that he did not want to live when he no longer knew me, when he became a burden, when he couldn't feed or bathe himself. I did my best in his final years to help him die quicker: I know that was what he wanted. But, given U.S. laws, all that meant was taking him off his heart and stroke medications and letting him eat anything he wanted, no matter how unhealthy. Knowing what's to come, having seen him go through it, I might consider moving to Belgium, which has begun to allow assisted suicide of those living with Alzheimer's and dementia if they can clearly state their intentions early on in the disease when they still have clarity of mind.
Next, I could help. Right now, there are dozens of Alzheimer's and dementia studies in the works. They are short thousands of willing test subjects. One of the top barriers to learning what's triggering the disease, and finding a cure, is populating these studies. So, knowing would make me a stronger candidate and would potentially help others down the road.
Finally, it would change my priorities. My father died the longest death possible: he succumbed last year more than 15 years after his diagnosis. My mother died the quickest possible way: she had a stress-related brain aneurysm 10 years after my father's diagnosis. Caring for him was too much for her and aneurysms ran in her family; her mother died of one as well. I already get a scan once every five years to see if I'm developing a brain aneurysm. If I am, odds are only 66% that they can operate on it—some aneurysms develop much too deep in the brain to operate, like my mother's.
Would she have wanted to know? Even though the aneurysm in her case was inoperable? I'm not sure. But I imagine if she had known, she would've lived her final years differently. She might have taken that trip to Alaska that she debated but thought was too expensive. She might have gotten organized earlier to make out a will so I wasn't left with chaos in the wake of her death; we'd planned for my father's death, knowing he was ill, but not my mother's. And she might have finally gotten around to dictating her story to me, as she'd always promised me she would when she found the time.
Telling my father's story at the end of his life helped his care.
With my startup MemoryWell, I spend my life now collecting senior stories before they are lost, in part because telling my father's story at the end of his life helped his care. But it's also in part for the story I lost with my mother.
If I knew that my time was limited, I'd not worry so much about saving for retirement. I'd make progress on my bucket list: hike Machu Picchu, scuba dive the Maldives, or raft the Grand Canyon. I'd tell my loved ones as much as I can in my time remaining how much they mean to me. And I would spend more time writing my own story to pass it down—finally finishing the book I've been working on. Maybe it's the writer in me, or maybe it's that I don't have kids of my own yet to carry on a legacy, but I'd want my story to be known, to have others learn from my experiences. And that's the biggest gift knowing would give me.
Editor's Note: Consider the other side of the argument here.
A robot server, controlled remotely by a disabled worker, delivers drinks to patrons at the DAWN cafe in Tokyo.
A sleek, four-foot tall white robot glides across a cafe storefront in Tokyo’s Nihonbashi district, holding a two-tiered serving tray full of tea sandwiches and pastries. The cafe’s patrons smile and say thanks as they take the tray—but it’s not the robot they’re thanking. Instead, the patrons are talking to the person controlling the robot—a restaurant employee who operates the avatar from the comfort of their home.
It’s a typical scene at DAWN, short for Diverse Avatar Working Network—a cafe that launched in Tokyo six years ago as an experimental pop-up and quickly became an overnight success. Today, the cafe is a permanent fixture in Nihonbashi, staffing roughly 60 remote workers who control the robots remotely and communicate to customers via a built-in microphone.
More than just a creative idea, however, DAWN is being hailed as a life-changing opportunity. The workers who control the robots remotely (known as “pilots”) all have disabilities that limit their ability to move around freely and travel outside their homes. Worldwide, an estimated 16 percent of the global population lives with a significant disability—and according to the World Health Organization, these disabilities give rise to other problems, such as exclusion from education, unemployment, and poverty.
These are all problems that Kentaro Yoshifuji, founder and CEO of Ory Laboratory, which supplies the robot servers at DAWN, is looking to correct. Yoshifuji, who was bedridden for several years in high school due to an undisclosed health problem, launched the company to help enable people who are house-bound or bedridden to more fully participate in society, as well as end the loneliness, isolation, and feelings of worthlessness that can sometimes go hand-in-hand with being disabled.
“It’s heartbreaking to think that [people with disabilities] feel they are a burden to society, or that they fear their families suffer by caring for them,” said Yoshifuji in an interview in 2020. “We are dedicating ourselves to providing workable, technology-based solutions. That is our purpose.”
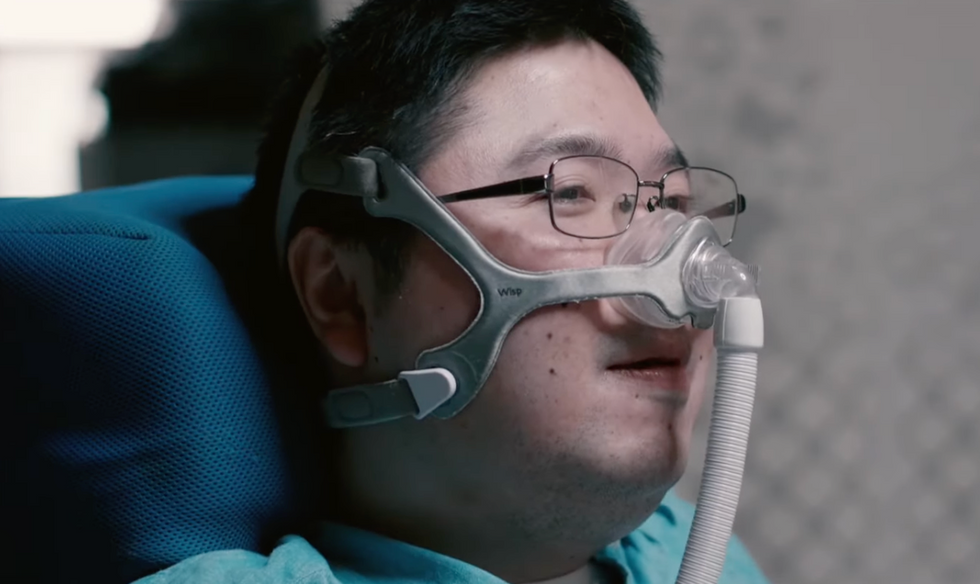
Shota, Kuwahara, a DAWN employee with muscular dystrophy, agrees. "There are many difficulties in my daily life, but I believe my life has a purpose and is not being wasted," he says. "Being useful, able to help other people, even feeling needed by others, is so motivational."
A woman receives a mammogram, which can detect the presence of tumors in a patient's breast.
When a patient is diagnosed with early-stage breast cancer, having surgery to remove the tumor is considered the standard of care. But what happens when a patient can’t have surgery?
Whether it’s due to high blood pressure, advanced age, heart issues, or other reasons, some breast cancer patients don’t qualify for a lumpectomy—one of the most common treatment options for early-stage breast cancer. A lumpectomy surgically removes the tumor while keeping the patient’s breast intact, while a mastectomy removes the entire breast and nearby lymph nodes.
Fortunately, a new technique called cryoablation is now available for breast cancer patients who either aren’t candidates for surgery or don’t feel comfortable undergoing a surgical procedure. With cryoablation, doctors use an ultrasound or CT scan to locate any tumors inside the patient’s breast. They then insert small, needle-like probes into the patient's breast which create an “ice ball” that surrounds the tumor and kills the cancer cells.
Cryoablation has been used for decades to treat cancers of the kidneys and liver—but only in the past few years have doctors been able to use the procedure to treat breast cancer patients. And while clinical trials have shown that cryoablation works for tumors smaller than 1.5 centimeters, a recent clinical trial at Memorial Sloan Kettering Cancer Center in New York has shown that it can work for larger tumors, too.
In this study, doctors performed cryoablation on patients whose tumors were, on average, 2.5 centimeters. The cryoablation procedure lasted for about 30 minutes, and patients were able to go home on the same day following treatment. Doctors then followed up with the patients after 16 months. In the follow-up, doctors found the recurrence rate for tumors after using cryoablation was only 10 percent.
For patients who don’t qualify for surgery, radiation and hormonal therapy is typically used to treat tumors. However, said Yolanda Brice, M.D., an interventional radiologist at Memorial Sloan Kettering Cancer Center, “when treated with only radiation and hormonal therapy, the tumors will eventually return.” Cryotherapy, Brice said, could be a more effective way to treat cancer for patients who can’t have surgery.
“The fact that we only saw a 10 percent recurrence rate in our study is incredibly promising,” she said.


