Is Finding Out Your Baby’s Genetics A New Responsibility of Parenting?
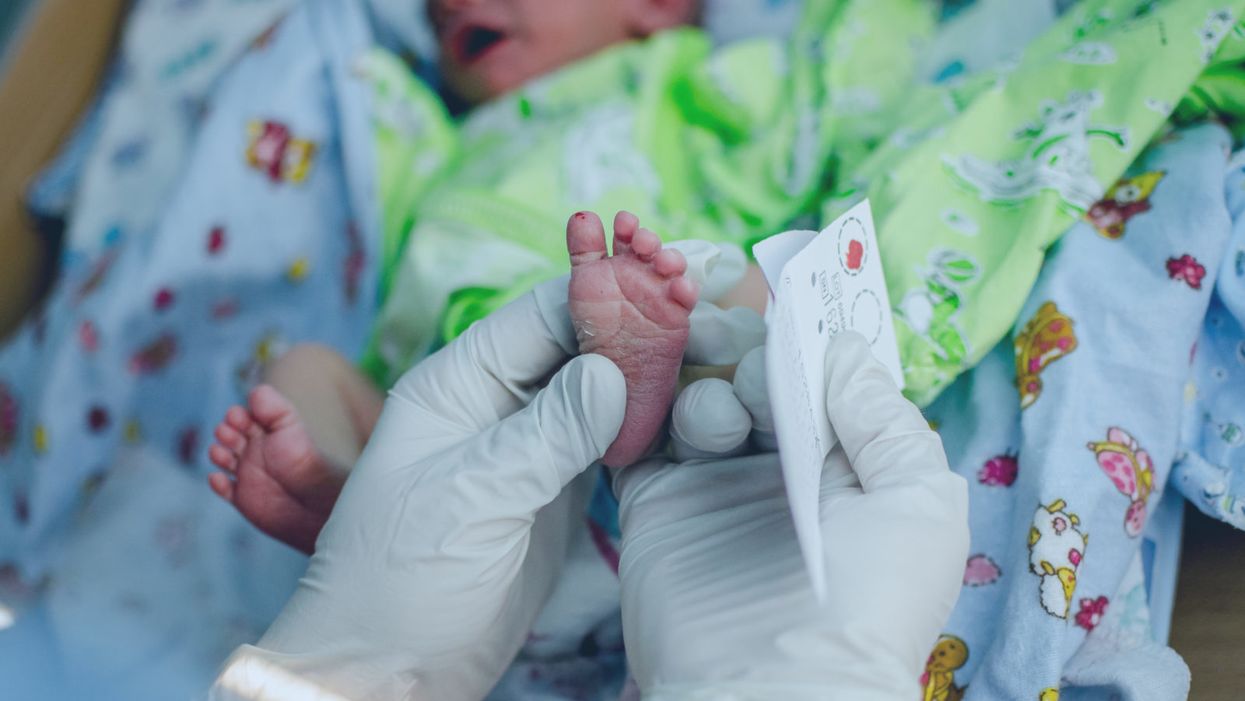
A doctor pricks the heel of a newborn for a blood test.
Hours after a baby is born, its heel is pricked with a lancet. Drops of the infant's blood are collected on a porous card, which is then mailed to a state laboratory. The dried blood spots are screened for around thirty conditions, including phenylketonuria (PKU), the metabolic disorder that kick-started this kind of newborn screening over 60 years ago. In the U.S., parents are not asked for permission to screen their child. Newborn screening programs are public health programs, and the assumption is that no good parent would refuse a screening test that could identify a serious yet treatable condition in their baby.
Learning as much as you can about your child's health might seem like a natural obligation of parenting. But it's an assumption that I think needs to be much more closely examined.
Today, with the introduction of genome sequencing into clinical medicine, some are asking whether newborn screening goes far enough. As the cost of sequencing falls, should parents take a more expansive look at their children's health, learning not just whether they have a rare but treatable childhood condition, but also whether they are at risk for untreatable conditions or for diseases that, if they occur at all, will strike only in adulthood? Should genome sequencing be a part of every newborn's care?
It's an idea that appeals to Anne Wojcicki, the founder and CEO of the direct-to-consumer genetic testing company 23andMe, who in a 2016 interview with The Guardian newspaper predicted that having newborns tested would soon be considered standard practice—"as critical as testing your cholesterol"—and a new responsibility of parenting. Wojcicki isn't the only one excited to see everyone's genes examined at birth. Francis Collins, director of the National Institutes of Health and perhaps the most prominent advocate of genomics in the United States, has written that he is "almost certain … that whole-genome sequencing will become part of new-born screening in the next few years." Whether that would happen through state-mandated screening programs, or as part of routine pediatric care—or perhaps as a direct-to-consumer service that parents purchase at birth or receive as a baby-shower gift—is not clear.
Learning as much as you can about your child's health might seem like a natural obligation of parenting. But it's an assumption that I think needs to be much more closely examined, both because the results that genome sequencing can return are more complex and more uncertain than one might expect, and because parents are not actually responsible for their child's lifelong health and well-being.
What is a parent supposed to do about such a risk except worry?
Existing newborn screening tests look for the presence of rare conditions that, if identified early in life, before the child shows any symptoms, can be effectively treated. Sequencing could identify many of these same kinds of conditions (and it might be a good tool if it could be targeted to those conditions alone), but it would also identify gene variants that confer an increased risk rather than a certainty of disease. Occasionally that increased risk will be significant. About 12 percent of women in the general population will develop breast cancer during their lives, while those who have a harmful BRCA1 or BRCA2 gene variant have around a 70 percent chance of developing the disease. But for many—perhaps most—conditions, the increased risk associated with a particular gene variant will be very small. Researchers have identified over 600 genes that appear to be associated with schizophrenia, for example, but any one of those confers only a tiny increase in risk for the disorder. What is a parent supposed to do about such a risk except worry?
Sequencing results are uncertain in other important ways as well. While we now have the ability to map the genome—to create a read-out of the pairs of genetic letters that make up a person's DNA—we are still learning what most of it means for a person's health and well-being. Researchers even have a name for gene variants they think might be associated with a disease or disorder, but for which they don't have enough evidence to be sure. They are called "variants of unknown (or uncertain) significance (VUS), and they pop up in most people's sequencing results. In cancer genetics, where much research has been done, about 1 in 5 gene variants are reclassified over time. Most are downgraded, which means that a good number of VUS are eventually designated benign.
While one parent might reasonably decide to learn about their child's risk for a condition about which nothing can be done medically, a different, yet still thoroughly reasonable, parent might prefer to remain ignorant so that they can enjoy the time before their child is afflicted.
Then there's the puzzle of what to do about results that show increased risk or even certainty for a condition that we have no idea how to prevent. Some genomics advocates argue that even if a result is not "medically actionable," it might have "personal utility" because it allows parents to plan for their child's future needs, to enroll them in research, or to connect with other families whose children carry the same genetic marker.
Finding a certain gene variant in one child might inform parents' decisions about whether to have another—and if they do, about whether to use reproductive technologies or prenatal testing to select against that variant in a future child. I have no doubt that for some parents these personal utility arguments are persuasive, but notice how far we've now strayed from the serious yet treatable conditions that motivated governments to set up newborn screening programs, and to mandate such testing for all.
Which brings me to the other problem with the call for sequencing newborn babies: the idea that even if it's not what the law requires, it's what good parents should do. That idea is very compelling when we're talking about sequencing results that show a serious threat to the child's health, especially when interventions are available to prevent or treat that condition. But as I have shown, many sequencing results are not of this type.
While one parent might reasonably decide to learn about their child's risk for a condition about which nothing can be done medically, a different, yet still thoroughly reasonable, parent might prefer to remain ignorant so that they can enjoy the time before their child is afflicted. This parent might decide that the worry—and the hypervigilence it could inspire in them—is not in their child's best interest, or indeed in their own. This parent might also think that it should be up to the child, when he or she is older, to decide whether to learn about his or her risk for adult-onset conditions, especially given that many adults at high familial risk for conditions like Alzheimer's or Huntington's disease choose never to be tested. This parent will value the child's future autonomy and right not to know more than they value the chance to prepare for a health risk that won't strike the child until 40 or 50 years in the future.
Parents are not obligated to learn about their children's risk for a condition that cannot be prevented, has a small risk of occurring, or that would appear only in adulthood.
Contemporary understandings of parenting are famously demanding. We are asked to do everything within our power to advance our children's health and well-being—to act always in our children's best interests. Against that backdrop, the need to sequence every newborn baby's genome might seem obvious. But we should be skeptical. Many sequencing results are complex and uncertain. Parents are not obligated to learn about their children's risk for a condition that cannot be prevented, has a small risk of occurring, or that would appear only in adulthood. To suggest otherwise is to stretch parental responsibilities beyond the realm of childhood and beyond factors that parents can control.
Every weekend since January, pediatrician Cora Collette Breuner has volunteered to give the COVID-19 vaccine to individuals from age 12 to 96 in an underserved community in Washington state.
Even though the COVID-19 vaccines have been shown to be incredibly safe and effective, there's still quite a bit of hesitancy among parents to vaccinate their teenage children, says Breuner, an adolescent medicine specialist at Seattle Children's Hospital and a past chair of the American Academy of Pediatrics' Committee on Adolescence. "They have questions and they have questions," she says.
Breuner patiently answers them all. Even then, parents—who have the final say in whether their child gets the vaccine—may be reluctant to sign off on it.
In 41 states, parents must consent for minors under age 18 to receive a COVID-19 vaccine. One state—Nebraska—requires parental consent for individuals under age 19, according to the Kaiser Family Foundation. Healthcare workers can't legally give teens COVID-19 vaccines otherwise. In a May report, the nonprofit healthcare organization highlights that from a legal perspective, "the landscape may be shifting slightly as more jurisdictions seek to encourage vaccination of young people."
Meanwhile, as the Delta variant creates a new surge in cases, some ethicists and pediatricians argue that state laws should be amended or loosened to allow minors to consent to COVID-19 vaccination on their own, without the need for parental permission.
"COVID-19 has killed millions of people around the world and disrupted the global economy," says pediatrician John Lantos. "It's a global catastrophe that requires special rules."
There are compelling arguments in favor of letting minors consent on their own, says Robyn Shapiro, a health care lawyer and a bioethicist in the Milwaukee area. "By that, I mean they're either old enough or they're evaluated in such a way that they have sufficient understanding of what they're agreeing to."
Shapiro and other ethicists argue that teens are perfectly capable of giving "informed consent"—a key principle in ethics that means fully understanding the benefits and risks of a medical intervention. To give informed consent, a person must be able to process that information in line with their own values. Only then can they make an autonomous choice and sign a consent form, Shapiro says.
Most states already have laws permitting minors to consent to testing and treatments related to sexually transmitted diseases, birth control, behavioral health, and substance abuse. It wouldn't be that much of a stretch to add COVID-19 vaccination to the list, Shapiro says. New Jersey and New York have introduced bills to let teens as young as 14 to consent to getting the COVID-19 vaccine and Minnesota has proposed a bill to allow children as young as 12 to give consent.
With any medical test or intervention, doctors often wrestle with how to best involve teens in conversations about their own health care, says John Lantos, a pediatrician and director of the Bioethics Center at Children's Mercy Kansas City.
"Most bioethicists would say that [teens] should be included to the degree that they have decision-making capacity," he says. "In most cases, that means including them in discussions with their parents in trying to achieve consensus about what the best choice may be."
COVID-19 vaccination also presents a unique circumstance, Lantos notes. It raises the question: Should teens have greater decisional authority because it's a public health emergency? In his opinion, the answer is yes. "COVID-19 has killed millions of people around the world and disrupted the global economy," says pediatrician Lantos. "It's a global catastrophe that requires special rules."
In North Carolina, state legislators are moving to do the opposite. State law currently allows those under 18 to make vaccination decisions on their own, but on Aug. 5, North Carolina's General Assembly approved a Republican-sponsored bill requiring parental consent for 12- to 17-year-olds to get a COVID-19 vaccine.
Kyle Brothers, a pediatrician in Louisville, Kentucky, says it's "ethically justifiable" for states to permit adolescents, especially those on the verge of adulthood, to consent to COVID-19 vaccination and other straightforward medical care.
In many cases, 16- and 17-year-old adolescents are capable of making well-informed decisions, says Brothers, a member of the American Academy of Pediatrics' Section on Bioethics. "The problem is, the law tends not to have that level of nuance," he adds. "We know in the real world that maturing and developing the ability to make decisions is a continuous process, but the law sets a bright line at age 18."
Lacking parental consent, some defiant teens are researching avenues to get vaccinated without their mom's or dad's knowledge. They may have turned to VaxTeen.org, a site operated by a Los Angeles teenager that provides information on consent laws by state.
If parents are wavering on the decision to give consent, Breuner recommends that they speak with a trusted healthcare provider about their specific concerns. These kinds of dialogues often can clarify lingering worries and may help drive up consent rates for teen vaccination.
Vaccine-hesitant parents should hear out their teens who wish to be vaccinated. Teenagers have their own opinions and belief systems, and parents should respect their child's choice to be vaccinated if they wish, considering the minimal risk of harm and the significant benefit to society as a whole.
George J. Annas, professor and director at the Center for Health Law, Ethics & Human Rights at Boston University, says parents have a legal obligation to provide their children with necessary medical treatment, or they could be found guilty of child neglect. The circumstances vary, but in the face of unrelenting COVID-19, he says parents have an ethical duty to consent to teens' vaccination because "the disease is rampant and children are dying."
The Nose Knows: Dogs Are Being Trained to Detect the Coronavirus
Security workers walk with detection dogs in an airport terminal.
Asher is eccentric and inquisitive. He loves an audience, likes keeping busy, and howls to be let through doors. He is a six-year-old working Cocker Spaniel, who, with five other furry colleagues, has now been trained to sniff body odor samples from humans to detect COVID-19 infections.
As the Delta variant and other new versions of the SARS-CoV-2 virus emerge, public health agencies are once again recommending masking while employers contemplate mandatory vaccination. While PCR tests remain the "gold standard" of COVID-19 tests, they can take hours to flag infections. To accelerate the process, scientists are turning to a new testing tool: sniffer dogs.
At the London School of Hygiene and Tropical Medicine (LSHTM), researchers deployed Asher and five other trained dogs to test sock samples from 200 asymptomatic, infected individuals and 200 healthy individuals. In May, they published the findings of the yearlong study in a preprint, concluding that dogs could identify COVID-19 infections with a high degree of accuracy – they could correctly identify a COVID-positive sample up to 94% of the time and a negative sample up to 92% of the time. The paper has yet to be peer-reviewed.
"Dogs can screen lots of people very quickly – 300 people per dog per hour. This means they could be used in places like airports or public venues like stadiums and maybe even workplaces," says James Logan, who heads the Department of Disease Control at LSHTM, adding that canines can also detect variants of SARS-CoV-2. "We included samples from two variants and the dogs could still detect them."
Detection dogs have been one of the most reliable biosensors for identifying the odor of human disease. According to Gemma Butlin, a spokesperson of Medical Detection Dogs, the UK-based charity that trained canines for the LSHTM study, the olfactory capabilities of dogs have been deployed to detect malaria, Parkinson's disease, different types of cancers, as well as pseudomonas, a type of bacteria known to cause infections in blood, lungs, eyes, and other parts of the human body.
COVID-19 has a distinctive smell — a result of chemicals known as volatile organic compounds released by infected body cells, which give off an odor "fingerprint."
"It's estimated that the percentage of a dog's brain devoted to analyzing odors is 40 times larger than that of a human," says Butlin. "Humans have around 5 million scent receptors dedicated to smell. Dogs have 350 million and can detect odors at parts per trillion. To put this into context, a dog can detect a teaspoon of sugar in a million gallons of water: two Olympic-sized pools full."
According to LSHTM scientists, COVID-19 has a distinctive smell — a result of chemicals known as volatile organic compounds released by infected body cells, which give off an odor "fingerprint." Other studies, too, have revealed that the SARS-CoV-2 virus has a distinct olfactory signature, detectable in the urine, saliva, and sweat of infected individuals. Humans can't smell the disease in these fluids, but dogs can.
"Our research shows that the smell associated with COVID-19 is at least partly due to small and volatile chemicals that are produced by the virus growing in the body or the immune response to the virus or both," said Steve Lindsay, a public health entomologist at Durham University, whose team collaborated with LSHTM for the study. He added, "There is also a further possibility that dogs can actually smell the virus, which is incredible given how small viruses are."
In April this year, researchers from the University of Pennsylvania and collaborators published a similar study in the scientific journal PLOS One, revealing that detection dogs could successfully discriminate between urine samples of infected and uninfected individuals. The accuracy rate of canines in this study was 96%. Similarly, last December, French scientists found that dogs were 76-100% effective at identifying individuals with COVID-19 when presented with sweat samples.
Grandjean Dominique, a professor at France's National Veterinary School of Alfort, who led the French study, said that the researchers used two types of dogs — search and rescue dogs, as they can sniff sweat, and explosive detection dogs, because they're often used at airports to find bomb ingredients. Dogs may very well be as good as PCR tests, said Dominique, but the goal, he added, is not to replace these tests with canines.
In France, the government gave the green light to train hundreds of disease detection dogs and deploy them in airports. "They will act as mass pre-test, and only people who are positive will undergo a PCR test to check their level of infection and the kind of variant," says Dominique. He thinks the dogs will be able to decrease the amount of PCR testing and potentially save money.
Since the accuracy rate for bio-detection dogs is fairly high, scientists think they could prove to be a quick diagnosis and mass screening tool, especially at ports, airports, train stations, stadiums, and public gatherings. Countries like Finland, Thailand, UAE, Italy, Chile, India, Australia, Pakistan, Saudi Arabia, Switzerland, and Mexico are already training and deploying canines for COVID-19 detection. The dogs are trained to sniff the area around a person, and if they find the odor of COVID-19 they will sit or stand back from an individual as a signal that they've identified an infection.
While bio-detection dogs seem promising for cheap, large-volume screening, many of the studies that have been performed to date have been small and in controlled environments. The big question is whether this approach work on people in crowded airports, not just samples of shirts and socks in a lab.
"The next step is 'real world' testing where they [canines] are placed in airports to screen people and see how they perform," says Anna Durbin, professor of international health at the John Hopkins Bloomberg School of Public Health. "Testing in real airports with lots of passengers and competing scents will need to be done."
According to Butlin of Medical Detection Dogs, scalability could be a challenge. However, scientists don't intend to have a dog in every waiting room, detecting COVID-19 or other diseases, she said.
"Dogs are the most reliable bio sensors on the planet and they have proven time and time again that they can detect diseases as accurately, if not more so, than current technological diagnostics," said Butlin. "We are learning from them all the time and what their noses know will one day enable the creation an 'E-nose' that does the same job – imagine a day when your mobile phone can tell you that you are unwell."

