Is Sex for Reproduction About to Become Extinct?
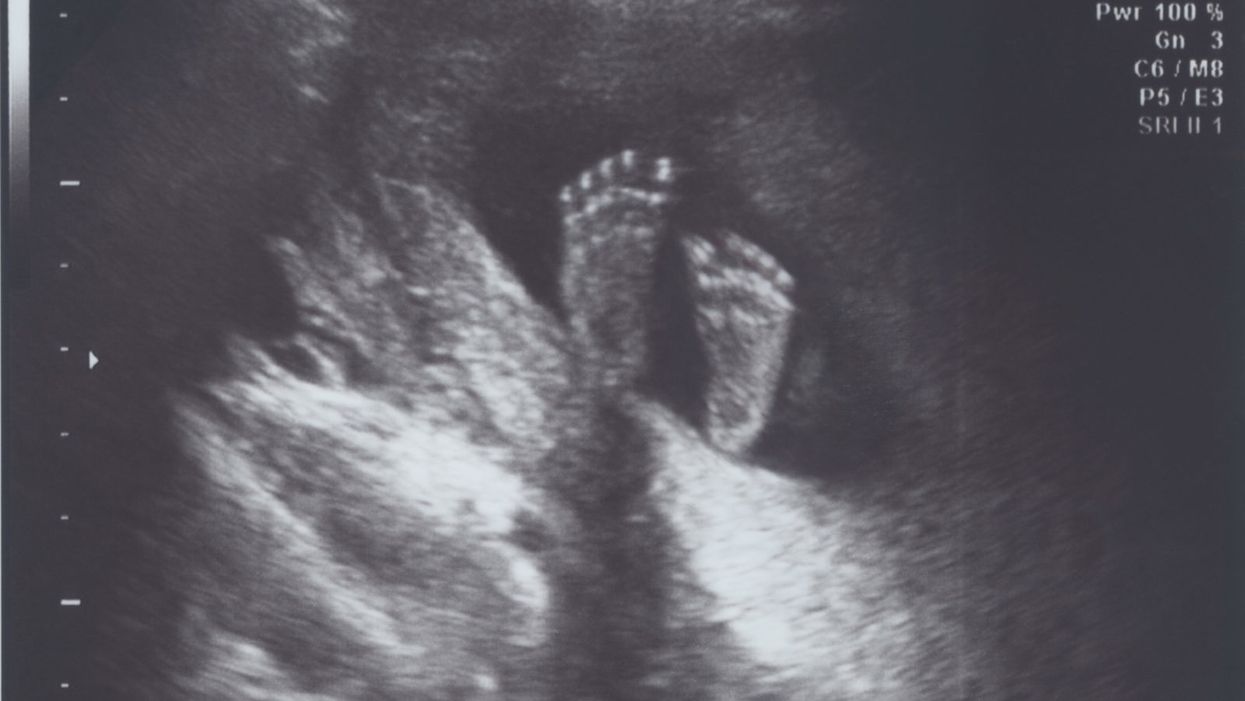
A healthy fetus in utero at 22 weeks.
There are lots of great reasons we humans have sex. We mostly do it to pair bond, realize our primal urges, and feel good. Once in a while, we also do it to make babies. As the coming genetic revolution plays out, we'll still have sex for most of the same reasons we do today. But we'll increasingly not do it to procreate.
Protecting children from harm is one of the core responsibilities of parenting.
Most parents go to great lengths to protect their children from real and imagined harms. This begins with taking prenatal vitamins during pregnancy and extends to having children immunized and protected from exposures to various diseases and dangers. Most of us look askance for good reason at mothers who abuse controlled substances during their pregnancies or parents who choose to not immunize their children. Protecting children from harm is one of the core responsibilities of parenting.
In the United States today, up to two percent of babies are estimated to be born with rare genetic diseases caused by single gene mutations. Sickle cell disease, Tay-Sachs, and Huntington's disease are among the more well-known examples of these, but the list runs to the thousands. Many babies born with these disorders suffer terribly, some die young, and nearly all spend big chunks of their lives struggling through the medical system.
Increasingly, however, many of these single-gene mutation diseases and other chromosomal disorders like Down syndrome are being identified in non-invasive prenatal tests performed on expectant mothers at the end of their first trimester of pregnancy. Knowing the hardship that children born with these types of disorders will likely face, majorities of these women in countries around the world are choosing to terminate pregnancies once these diagnoses have been made. Whatever the justification and whatever anyone's views on the morality of abortion, these decisions are inherently excruciating.
A much smaller number of prospective mothers, however, are today getting this same information about their potential future children before their pregnancies even begin. By undergoing both in vitro fertilization (IVF) and preimplantation genetic testing (PGT), these women are able to know which of the eggs that have been surgically extracted from them and fertilized with their partner or donor's sperm will carry the dangerous mutations. The in vitro embryos with these disorders are simply not implanted in the expectant mother's womb.
It would be monstrous to assert that an existing person with a deadly disease has any less right to thrive than anyone else. But it would also be hard to make a case that parents should affirmatively choose to implant embryos carrying such a disease if given the option. If prospective parents are already today choosing not to implant certain embryos based on our preliminary understanding of disease risk, what will happen when this embryo selection is based on far more information than just a few thousand single gene mutation diseases?
Our ability and willingness to make genetic alterations to our future children will grow over time along with our knowledge and technological ability.
When the first human genome was sequenced in 2003, the race to uncover the mysteries of human genetics had only just begun. Although we still know very little about our genetics relative to the complexity of the genome and even less compared to the broader ecosystem of our biology, the progress toward greater understanding is astounding. Today, the number of single gene mutation diseases and relatively simple genetic traits that can be predicted meaningfully from genetic data alone is already significant.
In the not-distant future, this list will grow to include complex diseases and disease propensities, percentage probabilities of living a long and healthy life, and increasingly the genetic component of complex human attributes like height, IQ, and personality style. This predictive power of genetic analysis will funnel straight into our fertility clinics where prospective parents choosing embryos will be making ever more consequential decisions about the genetic components of the future lives, health, and capabilities of their children.
Our understanding of what the genes extracted from early stage pre-implanted embryos are telling us will be only one of the rocket boosters driving assisted reproduction forward. Another will be the ability to induce adult cells like skin and nucleated blood cells into stem cells and then turn those stem cells into egg progenitor cells and then ultimately eggs. This will not only eliminate the need for hormone treatments and surgery to extract human eggs but also make it easy and cheap to generate an unlimited number of eggs from a given woman.
The average woman has around fifteen eggs extracted during IVF but imagine what generating a thousand eggs will do to the range of possibilities that could be realized through pre-implantation embryo selection. Each of these thousand eggs would be the natural offspring of the two parents, but the variation between them would make it possible to choose the ones with the strongest expression of the genetic component of a particular desired trait – like those with the highest possible genetic IQ potential.
Another rocket booster will be the application of gene editing technologies like CRISPR to edit the genomes of pre-implanted embryos or of the sperm and eggs used to create them. Just this week, Chinese researchers announced they had used CRISPR to edit the CCR5 gene in the pre-implanted embryos of a pair of Chinese twins to make them immune to HIV, the first ever case of gene editing humans and a harbinger of our genetically engineered future. The astounding complexity of the human genome will put limits on our ability to safely make too many simultaneous genetic changes to human embryos, but our ability and willingness to make these types of alterations to our future children will grow over time along with our knowledge and technological ability.
With so much at stake, prospective parents will increasingly have a stark choice when determining how to conceive their children. If they go the traditional route of sex, they will experience both the benign wisdom and unfathomable cruelty of nature. If they use IVF and increasingly informed embryo selection, they will eliminate most single gene mutation diseases and likely increase their children's chances of living a longer and healthier life with more opportunity than their unenhanced peers. But the optimizing parents could also set up their children for misery if these children don't particularly enjoy what they have been optimized to become or see themselves as some type of freakish consumer product with emotions.
Conceiving though sex will come to be seen more and more like not immunizing your children is today, a perfectly natural choice that comes with a significant potential risk and expense.
But although there will be pros and cons on each side, the fight between conception through good old-fashioned sex and conception in the lab will ultimately not be fair. Differences and competition within and between societies will pressure parents and societies to adopt ever more aggressive forms of reproductive technology if they believe doing so will open possibilities and create opportunities for the next generations rather than close them.
Conception through sex will remain as useful as it has always been but lab conception will only get more advantageous. Over time, only zealots will choose to roll the dice of their future children's health and well-being rather than invest, like parents always have, in protecting their children from harm and helping optimize their life potential. Conceiving though sex will come to be seen more and more like not immunizing your children is today, a perfectly natural choice that comes with a significant potential risk and expense to yourself, your children, and your community.
As this future plays out, the genetics and assisted reproduction revolutions will raise enormous, thorny, and massively consequential questions about how we value and invest in diversity, equality, and our own essential humanity – questions we aren't remotely prepared to answer. But these revolutions are coming sooner than most of us understand or are prepared for so we had better get ready.
Because where this trail is ultimately heading goes well beyond sex and toward a fundamental transformation of our evolutionary process as a species – and that should be everybody's business.
Have You Heard of the Best Sport for Brain Health?
In this week's Friday Five, research points to this brain healthiest of sports. Plus, the natural way to reprogram cells to a younger state, the network that could underlie many different mental illnesses, and a new test could diagnose autism in newborns. Plus, scientists 3D print an ear and attach it to woman
The Friday Five covers five stories in research that you may have missed this week. There are plenty of controversies and troubling ethical issues in science – and we get into many of them in our online magazine – but this news roundup focuses on scientific creativity and progress to give you a therapeutic dose of inspiration headed into the weekend.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
Here are the promising studies covered in this week's Friday Five:
- Reprogram cells to a younger state
- Pick up this sport for brain health
- Do all mental illnesses have the same underlying cause?
- New test could diagnose autism in newborns
- Scientists 3D print an ear and attach it to woman
Can blockchain help solve the Henrietta Lacks problem?
Marielle Gross, a professor at the University of Pittsburgh, shows patients a new app that tracks how their samples are used during biomedical research.
Science has come a long way since Henrietta Lacks, a Black woman from Baltimore, succumbed to cervical cancer at age 31 in 1951 -- only eight months after her diagnosis. Since then, research involving her cancer cells has advanced scientific understanding of the human papilloma virus, polio vaccines, medications for HIV/AIDS and in vitro fertilization.
Today, the World Health Organization reports that those cells are essential in mounting a COVID-19 response. But they were commercialized without the awareness or permission of Lacks or her family, who have filed a lawsuit against a biotech company for profiting from these “HeLa” cells.
While obtaining an individual's informed consent has become standard procedure before the use of tissues in medical research, many patients still don’t know what happens to their samples. Now, a new phone-based app is aiming to change that.
Tissue donors can track what scientists do with their samples while safeguarding privacy, through a pilot program initiated in October by researchers at the Johns Hopkins Berman Institute of Bioethics and the University of Pittsburgh’s Institute for Precision Medicine. The program uses blockchain technology to offer patients this opportunity through the University of Pittsburgh's Breast Disease Research Repository, while assuring that their identities remain anonymous to investigators.
A blockchain is a digital, tamper-proof ledger of transactions duplicated and distributed across a computer system network. Whenever a transaction occurs with a patient’s sample, multiple stakeholders can track it while the owner’s identity remains encrypted. Special certificates called “nonfungible tokens,” or NFTs, represent patients’ unique samples on a trusted and widely used blockchain that reinforces transparency.
Blockchain could be used to notify people if cancer researchers discover that they have certain risk factors.
“Healthcare is very data rich, but control of that data often does not lie with the patient,” said Julius Bogdan, vice president of analytics for North America at the Healthcare Information and Management Systems Society (HIMSS), a Chicago-based global technology nonprofit. “NFTs allow for the encapsulation of a patient’s data in a digital asset controlled by the patient.” He added that this technology enables a more secure and informed method of participating in clinical and research trials.
Without this technology, de-identification of patients’ samples during biomedical research had the unintended consequence of preventing them from discovering what researchers find -- even if that data could benefit their health. A solution was urgently needed, said Marielle Gross, assistant professor of obstetrics, gynecology and reproductive science and bioethics at the University of Pittsburgh School of Medicine.
“A researcher can learn something from your bio samples or medical records that could be life-saving information for you, and they have no way to let you or your doctor know,” said Gross, who is also an affiliate assistant professor at the Berman Institute. “There’s no good reason for that to stay the way that it is.”
For instance, blockchain could be used to notify people if cancer researchers discover that they have certain risk factors. Gross estimated that less than half of breast cancer patients are tested for mutations in BRCA1 and BRCA2 — tumor suppressor genes that are important in combating cancer. With normal function, these genes help prevent breast, ovarian and other cells from proliferating in an uncontrolled manner. If researchers find mutations, it’s relevant for a patient’s and family’s follow-up care — and that’s a prime example of how this newly designed app could play a life-saving role, she said.
Liz Burton was one of the first patients at the University of Pittsburgh to opt for the app -- called de-bi, which is short for decentralized biobank -- before undergoing a mastectomy for early-stage breast cancer in November, after it was diagnosed on a routine mammogram. She often takes part in medical research and looks forward to tracking her tissues.
“Anytime there’s a scientific experiment or study, I’m quick to participate -- to advance my own wellness as well as knowledge in general,” said Burton, 49, a life insurance service representative who lives in Carnegie, Pa. “It’s my way of contributing.”

Liz Burton was one of the first patients at the University of Pittsburgh to opt for the app before undergoing a mastectomy for early-stage breast cancer.
Liz Burton
The pilot program raises the issue of what investigators may owe study participants, especially since certain populations, such as Black and indigenous peoples, historically were not treated in an ethical manner for scientific purposes. “It’s a truly laudable effort,” Tamar Schiff, a postdoctoral fellow in medical ethics at New York University’s Grossman School of Medicine, said of the endeavor. “Research participants are beautifully altruistic.”
Lauren Sankary, a bioethicist and associate director of the neuroethics program at Cleveland Clinic, agrees that the pilot program provides increased transparency for study participants regarding how scientists use their tissues while acknowledging individuals’ contributions to research.
However, she added, “it may require researchers to develop a process for ongoing communication to be responsive to additional input from research participants.”
Peter H. Schwartz, professor of medicine and director of Indiana University’s Center for Bioethics in Indianapolis, said the program is promising, but he wonders what will happen if a patient has concerns about a particular research project involving their tissues.
“I can imagine a situation where a patient objects to their sample being used for some disease they’ve never heard about, or which carries some kind of stigma like a mental illness,” Schwartz said, noting that researchers would have to evaluate how to react. “There’s no simple answer to those questions, but the technology has to be assessed with an eye to the problems it could raise.”
To truly make a difference, blockchain must enable broad consent from patients, not just de-identification.
As a result, researchers may need to factor in how much information to share with patients and how to explain it, Schiff said. There are also concerns that in tracking their samples, patients could tell others what they learned before researchers are ready to publicly release this information. However, Bogdan, the vice president of the HIMSS nonprofit, believes only a minimal study identifier would be stored in an NFT, not patient data, research results or any type of proprietary trial information.
Some patients may be confused by blockchain and reluctant to embrace it. “The complexity of NFTs may prevent the average citizen from capitalizing on their potential or vendors willing to participate in the blockchain network,” Bogdan said. “Blockchain technology is also quite costly in terms of computational power and energy consumption, contributing to greenhouse gas emissions and climate change.”
In addition, this nascent, groundbreaking technology is immature and vulnerable to data security flaws, disputes over intellectual property rights and privacy issues, though it does offer baseline protections to maintain confidentiality. To truly make a difference, blockchain must enable broad consent from patients, not just de-identification, said Robyn Shapiro, a bioethicist and founding attorney at Health Sciences Law Group near Milwaukee.
The Henrietta Lacks story is a prime example, Shapiro noted. During her treatment for cervical cancer at Johns Hopkins, Lacks’s tissue was de-identified (albeit not entirely, because her cell line, HeLa, bore her initials). After her death, those cells were replicated and distributed for important and lucrative research and product development purposes without her knowledge or consent.
Nonetheless, Shapiro thinks that the initiative by the University of Pittsburgh and Johns Hopkins has potential to solve some ethical challenges involved in research use of biospecimens. “Compared to the system that allowed Lacks’s cells to be used without her permission, Shapiro said, “blockchain technology using nonfungible tokens that allow patients to follow their samples may enhance transparency, accountability and respect for persons who contribute their tissue and clinical data for research.”
Read more about laws that have prevented people from the rights to their own cells.

