Medical Tourism Is Booming, Fueled by High Costs and Slow Access

Bridget Snell traveled to Mexico to access an unapproved stem cell therapy for MS.
When Bridget Snell found out she had multiple sclerosis, she knew she would put up a fight. The 45 year-old mother of two, who lives in Duxbury, Mass., researched options to slow the progress of the disease. The methods she had been trying were invasive, often with side effects of their own.
An estimated 2.2 million Americans will travel abroad for medical care in 2020.
Then she stumbled upon autologous hematopoietic stem cell transplantation (AHSCT), an experimental and controversial procedure that uses the patient's own stem cells to try to halt the progress of the disease. The FDA has not approved this procedure and last year issued a warning about unapproved stem cell therapies.
Despite the lack of established science, Snell weighed her options and decided she would undergo the procedure at Clinica Ruiz, a private clinic in Puebla, Mexico, which boasts of the largest volume of cases in the world using the procedure to treat MS. In April 2018, she went to Mexico for treatment, returned home in a month, and continues to do well.
But a positive outcome is far from assured, says Sheldon Krimsky, adjunct professor in the Department of Public Health and Community Medicine at the Tufts School of Medicine.
"Often you can't get a good sense of what the quality of treatment is in another country," Krimsky says, adding that many companies promise procedures whose results have not been clinically validated. "Unfortunately, people are very easily persuaded by hope."
Traveling for Medical Care
Snell is one of many Americans who have traveled abroad to access medical care. Patients Beyond Borders, a medical tourism consultancy, estimates that 2.2 million Americans will do so in 2020. A 2018 BCC report projected a five-year compounded annual industry growth rate of 13.2 percent. Adding to the demand is the aging population, which is expected to reach 95 million people by 2060 – nearly double the number in 2018.
While Snell traveled to Mexico to try a procedure that was not yet available in the United States, other patients do so for a variety of reasons, primarily cost and speed of access. For example, despite having "pretty good insurance coverage," Washington resident Soniya Gadgil needed dental procedures that would have cost thousands of dollars out-of-pocket. An India native, she decided to travel to Pune, India to visit her parents -- and while there, she got the two root canals and implant that she needed. Gadgil saved 60 percent on the final bill.
Leaving the country for medical care is not restricted to dental work or FDA-banned procedures either. Patients visit countries around the world — South America, Central America, and the Caribbean top the list — for a number of other problems, such as knee and hip replacements and bariatric operations. The most common procedures sought abroad are for dentistry, cosmetic surgery, and cardiac conditions.
Traveling abroad to access less expensive procedures is a damning indictment of healthcare delivery in the United States, says Dr. Leigh Turner, associate professor at the Center for Bioethics at the University of Minnesota. "We have people who are being forced out of the system because of high costs. Collectively it suggests a real structural problem in terms of the organization of healthcare in the United States," Turner says.
The Growth of the Online Marketplace
Nevertheless, medical tourism is booming and a number of online businesses now meet patients' demand for discovery and facilitation of medical care abroad, like PlanMyMedicalTrip.com, Doctoorum.com, and Wellness Travels.
Anurav Rane, CEO and Founder of PlanMyMedicalTrip.com, says the company presents each potential client with options, a la Expedia. A knee replacement in India costs $2,500, a significantly cheaper option even with a $1,110 round-trip airfare from the United States, Rane says. The average cost for an inpatient total knee replacement in the United States in 2019 was a little more $30,000.
Once the client chooses a specific procedure at a specific hospital, the company facilitates the necessary groundwork including the medical visa, tickets, hotel stay, booking the procedure and pre and post-op stay, and consults with the surgeons or doctors even before arrival. "The hassle of planning is on us," Rane says. Once patients are settled in the accommodations, they undergo the procedure.
Playing in the Legal Shadows
The online marketplace companies and the medical team execute an orchestrated dance – but what happens if the patient is harmed during or after the procedure?
Turner says that medical malpractice, if it occurs, can be difficult to pursue abroad. "There are countries where the courts are notoriously slow and it's very difficult to get any kind of meaningful action and settlements," he says, even if the claims have a legitimate basis.
The industry's biggest challenge is trust.
Snell signed a waiver absolving her surgeons in Mexico of any legal claims. But, she points out, that's standard process even for procedures in the United States. "I signed just as many waivers as I would going into any surgery [in the US]."
While that might well be true, Turner argues, Americans don't waive legal rights when they sign consent forms. "There are some protections for patients here in the United States."
Beyond U.S. Medical Tourism
As expected, it's not just Americans who travel abroad for medical care. Lithuania-based Wellness Travels sees a significant percentage of its clients from the EU. PlanMyMedicaltrip.com has 15,000 surgeons and doctors from 12 countries in its database. Egypt-based Doctoorum works with professionals in its own country and attracts clients from the Middle East. It is looking to expand to include doctors from Jordan and India, among other countries.
The term "tourism" is misleading here because it muddies the picture about what post-op should really look like, says Gediminas Kondrackis of Wellness Travels. "Unfortunately a lot of medical travel facilitators mislead their clients by advertising beach holiday packages and the like. Post-op is really about quiet recovery inside for a few days; being out in the sun is not advisable."
The industry's biggest challenge is trust. "The dentist I went to is actually a friend of mine who has a successful practice for several years," says Gadgil, the Washington resident who had dental work done in India. "I'd hesitate to go to someone I don't know or to a place I have no experience with." Her apprehensions are not unusual. After all, anxiety is an expected reaction to any surgery. Word-of-mouth, cost savings, and thorough research may alleviate some of these trust issues.
"I had natural apprehensions and would have had them had I gone up the road to Brigham and Women's (in Boston) just as I did over the border," Snell says, "but I had done my homework extensively. That took a lot of the fear out of it."
Medical tourism will only increase, predicts Kondrackis. "There is still a lot of room to grow. Higher numbers of medical travelers could help reduce the strain on local healthcare systems by reducing wait times and controlling costs."
While patients who have benefited from medical tourism swear by it, the best cure would be to start at home by establishing healthcare equity, Krimsky says.
On the flip side, says Turner, it is debatable whether medical tourism actually benefits host countries, where local residents might get priced out of procedures at these exclusive clinics. Even if laws in host countries such as India might mandate "charity care" for poorer local patients, that does not always happen, Turner says. The trickle-down theory that these more expensive clinics will broaden access to care is often a pipe dream, he adds.
While patients who have benefited from medical tourism swear by it, the best cure would be to start at home by establishing healthcare equity, Krimsky says. "Now if we had universal healthcare in the United States," he adds, "that would be an entirely different story."
Or maybe not. Rane, of PlanMyMedicalTrip.com, has observed an influx of patients to India from Canada, a country with universal healthcare.
The reason they say they travel for care? Long wait times for procedures.
DNA- and RNA-based electronic implants may revolutionize healthcare
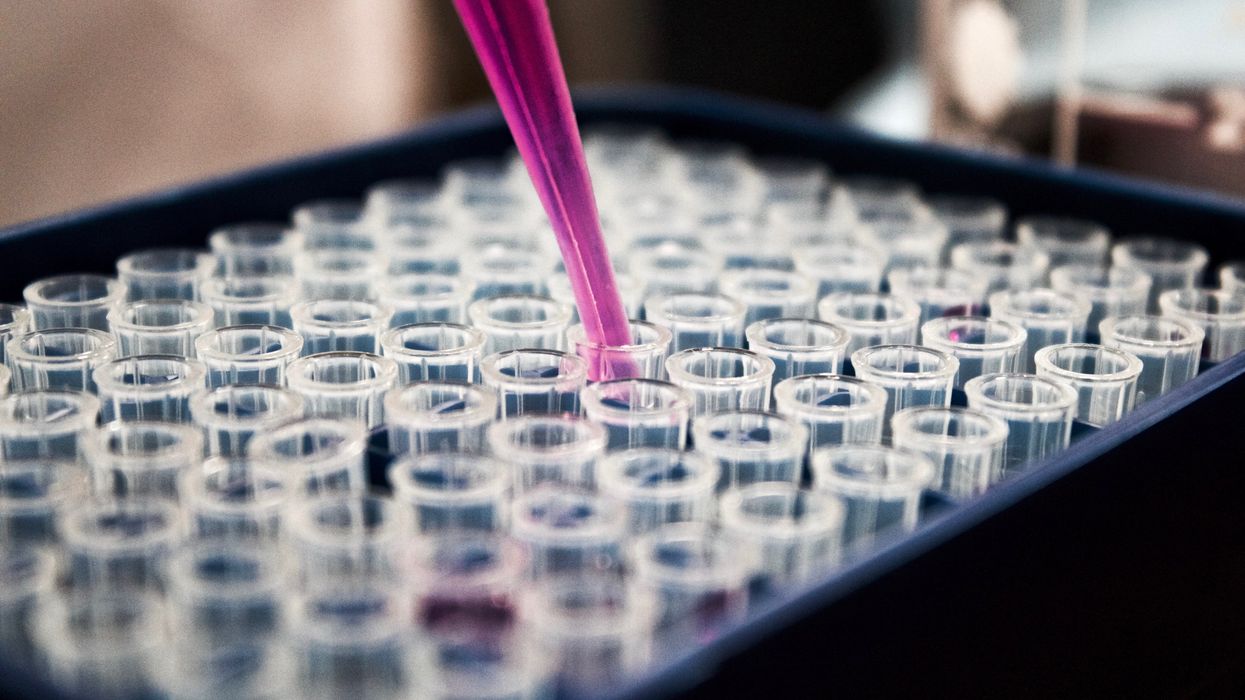
The test tubes contain tiny DNA/enzyme-based circuits, which comprise TRUMPET, a new type of electronic device, smaller than a cell.
Implantable electronic devices can significantly improve patients’ quality of life. A pacemaker can encourage the heart to beat more regularly. A neural implant, usually placed at the back of the skull, can help brain function and encourage higher neural activity. Current research on neural implants finds them helpful to patients with Parkinson’s disease, vision loss, hearing loss, and other nerve damage problems. Several of these implants, such as Elon Musk’s Neuralink, have already been approved by the FDA for human use.
Yet, pacemakers, neural implants, and other such electronic devices are not without problems. They require constant electricity, limited through batteries that need replacements. They also cause scarring. “The problem with doing this with electronics is that scar tissue forms,” explains Kate Adamala, an assistant professor of cell biology at the University of Minnesota Twin Cities. “Anytime you have something hard interacting with something soft [like muscle, skin, or tissue], the soft thing will scar. That's why there are no long-term neural implants right now.” To overcome these challenges, scientists are turning to biocomputing processes that use organic materials like DNA and RNA. Other promised benefits include “diagnostics and possibly therapeutic action, operating as nanorobots in living organisms,” writes Evgeny Katz, a professor of bioelectronics at Clarkson University, in his book DNA- And RNA-Based Computing Systems.
While a computer gives these inputs in binary code or "bits," such as a 0 or 1, biocomputing uses DNA strands as inputs, whether double or single-stranded, and often uses fluorescent RNA as an output.
Adamala’s research focuses on developing such biocomputing systems using DNA, RNA, proteins, and lipids. Using these molecules in the biocomputing systems allows the latter to be biocompatible with the human body, resulting in a natural healing process. In a recent Nature Communications study, Adamala and her team created a new biocomputing platform called TRUMPET (Transcriptional RNA Universal Multi-Purpose GatE PlaTform) which acts like a DNA-powered computer chip. “These biological systems can heal if you design them correctly,” adds Adamala. “So you can imagine a computer that will eventually heal itself.”
The basics of biocomputing
Biocomputing and regular computing have many similarities. Like regular computing, biocomputing works by running information through a series of gates, usually logic gates. A logic gate works as a fork in the road for an electronic circuit. The input will travel one way or another, giving two different outputs. An example logic gate is the AND gate, which has two inputs (A and B) and two different results. If both A and B are 1, the AND gate output will be 1. If only A is 1 and B is 0, the output will be 0 and vice versa. If both A and B are 0, the result will be 0. While a computer gives these inputs in binary code or "bits," such as a 0 or 1, biocomputing uses DNA strands as inputs, whether double or single-stranded, and often uses fluorescent RNA as an output. In this case, the DNA enters the logic gate as a single or double strand.
If the DNA is double-stranded, the system “digests” the DNA or destroys it, which results in non-fluorescence or “0” output. Conversely, if the DNA is single-stranded, it won’t be digested and instead will be copied by several enzymes in the biocomputing system, resulting in fluorescent RNA or a “1” output. And the output for this type of binary system can be expanded beyond fluorescence or not. For example, a “1” output might be the production of the enzyme insulin, while a “0” may be that no insulin is produced. “This kind of synergy between biology and computation is the essence of biocomputing,” says Stephanie Forrest, a professor and the director of the Biodesign Center for Biocomputing, Security and Society at Arizona State University.
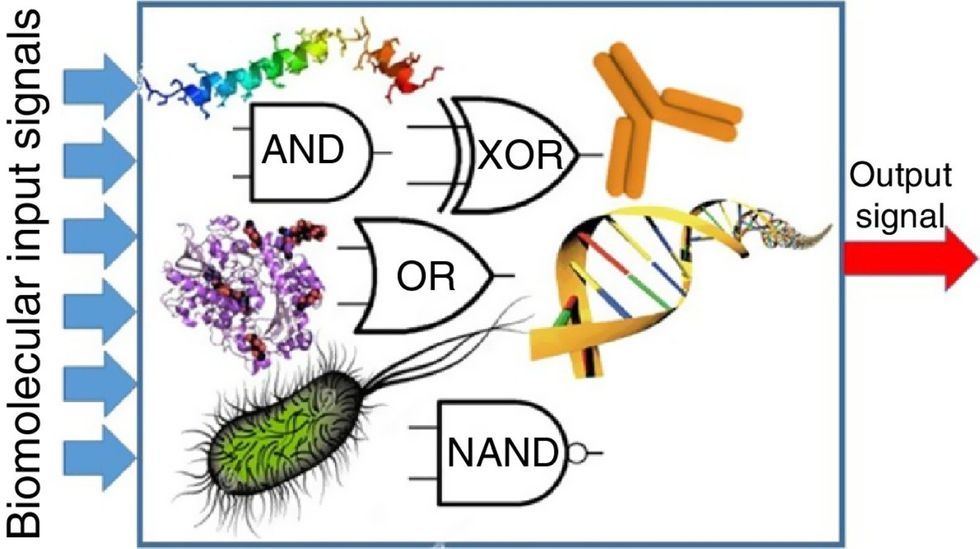
Biocomputing circles are made of DNA, RNA, proteins and even bacteria.
Evgeny Katz
The TRUMPET’s promise
Depending on whether the biocomputing system is placed directly inside a cell within the human body, or run in a test-tube, different environmental factors play a role. When an output is produced inside a cell, the cell's natural processes can amplify this output (for example, a specific protein or DNA strand), creating a solid signal. However, these cells can also be very leaky. “You want the cells to do the thing you ask them to do before they finish whatever their businesses, which is to grow, replicate, metabolize,” Adamala explains. “However, often the gate may be triggered without the right inputs, creating a false positive signal. So that's why natural logic gates are often leaky." While biocomputing outside a cell in a test tube can allow for tighter control over the logic gates, the outputs or signals cannot be amplified by a cell and are less potent.
TRUMPET, which is smaller than a cell, taps into both cellular and non-cellular biocomputing benefits. “At its core, it is a nonliving logic gate system,” Adamala states, “It's a DNA-based logic gate system. But because we use enzymes, and the readout is enzymatic [where an enzyme replicates the fluorescent RNA], we end up with signal amplification." This readout means that the output from the TRUMPET system, a fluorescent RNA strand, can be replicated by nearby enzymes in the platform, making the light signal stronger. "So it combines the best of both worlds,” Adamala adds.
These organic-based systems could detect cancer cells or low insulin levels inside a patient’s body.
The TRUMPET biocomputing process is relatively straightforward. “If the DNA [input] shows up as single-stranded, it will not be digested [by the logic gate], and you get this nice fluorescent output as the RNA is made from the single-stranded DNA, and that's a 1,” Adamala explains. "And if the DNA input is double-stranded, it gets digested by the enzymes in the logic gate, and there is no RNA created from the DNA, so there is no fluorescence, and the output is 0." On the story's leading image above, if the tube is "lit" with a purple color, that is a binary 1 signal for computing. If it's "off" it is a 0.
While still in research, TRUMPET and other biocomputing systems promise significant benefits to personalized healthcare and medicine. These organic-based systems could detect cancer cells or low insulin levels inside a patient’s body. The study’s lead author and graduate student Judee Sharon is already beginning to research TRUMPET's ability for earlier cancer diagnoses. Because the inputs for TRUMPET are single or double-stranded DNA, any mutated or cancerous DNA could theoretically be detected from the platform through the biocomputing process. Theoretically, devices like TRUMPET could be used to detect cancer and other diseases earlier.
Adamala sees TRUMPET not only as a detection system but also as a potential cancer drug delivery system. “Ideally, you would like the drug only to turn on when it senses the presence of a cancer cell. And that's how we use the logic gates, which work in response to inputs like cancerous DNA. Then the output can be the production of a small molecule or the release of a small molecule that can then go and kill what needs killing, in this case, a cancer cell. So we would like to develop applications that use this technology to control the logic gate response of a drug’s delivery to a cell.”
Although platforms like TRUMPET are making progress, a lot more work must be done before they can be used commercially. “The process of translating mechanisms and architecture from biology to computing and vice versa is still an art rather than a science,” says Forrest. “It requires deep computer science and biology knowledge,” she adds. “Some people have compared interdisciplinary science to fusion restaurants—not all combinations are successful, but when they are, the results are remarkable.”
Crickets are low on fat, high on protein, and can be farmed sustainably. They are also crunchy.
In today’s podcast episode, Leaps.org Deputy Editor Lina Zeldovich speaks about the health and ecological benefits of farming crickets for human consumption with Bicky Nguyen, who joins Lina from Vietnam. Bicky and her business partner Nam Dang operate an insect farm named CricketOne. Motivated by the idea of sustainable and healthy protein production, they started their unconventional endeavor a few years ago, despite numerous naysayers who didn’t believe that humans would ever consider munching on bugs.
Yet, making creepy crawlers part of our diet offers many health and planetary advantages. Food production needs to match the rise in global population, estimated to reach 10 billion by 2050. One challenge is that some of our current practices are inefficient, polluting and wasteful. According to nonprofit EarthSave.org, it takes 2,500 gallons of water, 12 pounds of grain, 35 pounds of topsoil and the energy equivalent of one gallon of gasoline to produce one pound of feedlot beef, although exact statistics vary between sources.
Meanwhile, insects are easy to grow, high on protein and low on fat. When roasted with salt, they make crunchy snacks. When chopped up, they transform into delicious pâtes, says Bicky, who invents her own cricket recipes and serves them at industry and public events. Maybe that’s why some research predicts that edible insects market may grow to almost $10 billion by 2030. Tune in for a delectable chat on this alternative and sustainable protein.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
Further reading:
More info on Bicky Nguyen
https://yseali.fulbright.edu.vn/en/faculty/bicky-n...
The environmental footprint of beef production
https://www.earthsave.org/environment.htm
https://www.watercalculator.org/news/articles/beef-king-big-water-footprints/
https://www.frontiersin.org/articles/10.3389/fsufs.2019.00005/full
https://ourworldindata.org/carbon-footprint-food-methane
Insect farming as a source of sustainable protein
https://www.insectgourmet.com/insect-farming-growing-bugs-for-protein/
https://www.sciencedirect.com/topics/agricultural-and-biological-sciences/insect-farming
Cricket flour is taking the world by storm
https://www.cricketflours.com/
https://talk-commerce.com/blog/what-brands-use-cricket-flour-and-why/

Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.