Fungus is the ‘New Black’ in Eco-Friendly Fashion

On the left, a Hermès bag made using fine mycelium as a leather alternative, made in partnership with the biotech company MycoWorks; on right, a sheet of mycelium "leather."
A natural material that looks and feels like real leather is taking the fashion world by storm. Scientists view mycelium—the vegetative part of a mushroom-producing fungus—as a planet-friendly alternative to animal hides and plastics.
Products crafted from this vegan leather are emerging, with others poised to hit the market soon. Among them are the Hermès Victoria bag, Lululemon's yoga accessories, Adidas' Stan Smith Mylo sneaker, and a Stella McCartney apparel collection.

The Adidas' Stan Smith Mylo concept sneaker, made in partnership with Bolt Threads, uses an alternative leather grown from mycelium; a commercial version is expected in the near future.
Adidas
Hermès has held presales on the new bag, says Philip Ross, co-founder and chief technology officer of MycoWorks, a San Francisco Bay area firm whose materials constituted the design. By year-end, Ross expects several more clients to debut mycelium-based merchandise. With "comparable qualities to luxury leather," mycelium can be molded to engineer "all the different verticals within fashion," he says, particularly footwear and accessories.
More than a half-dozen trailblazers are fine-tuning mycelium to create next-generation leather materials, according to the Material Innovation Initiative, a nonprofit advocating for animal-free materials in the fashion, automotive, and home-goods industries. These high-performance products can supersede items derived from leather, silk, down, fur, wool, and exotic skins, says A. Sydney Gladman, the institute's chief scientific officer.
That's only the beginning of mycelium's untapped prowess. "We expect to see an uptick in commercial leather alternative applications for mycelium-based materials as companies refine their R&D [research and development] and scale up," Gladman says, adding that "technological innovation and untapped natural materials have the potential to transform the materials industry and solve the enormous environmental challenges it faces."
In fewer than 10 days in indoor agricultural farms, "we grow large slabs of mycelium that are many feet wide and long. We are not confined to the shape or geometry of an animal."
Reducing our carbon footprint becomes possible because mycelium can flourish in indoor farms, using agricultural waste as feedstock and emitting inherently low greenhouse gas emissions. Carbon dioxide is the primary greenhouse gas. "We often think that when plant tissues like wood rot, that they go from something to nothing," says Jonathan Schilling, professor of plant and microbial biology at the University of Minnesota and a member of MycoWorks' Scientific Advisory Board.
But that assumption doesn't hold true for all carbon in plant tissues. When the fungi dominating the decomposition of plants fulfill their function, they transform a large portion of carbon into fungal biomass, Schilling says. That, in turn, ends up in the soil, with mycelium forming a network underneath that traps the carbon.
Unlike the large amounts of fossil fuels needed to produce styrofoam, leather and plastic, less fuel-intensive processing is involved in creating similar materials with a fungal organism. While some fungi consist of a single cell, others are multicellular and develop as very fine threadlike structures. A mass of them collectively forms a "mycelium" that can be either loose and low density or tightly packed and high density. "When these fungi grow at extremely high density," Schilling explains, "they can take on the feel of a solid material such as styrofoam, leather or even plastic."
Tunable and supple in the cultivation process, mycelium is also reliably sturdy in composition. "We believe that mycelium has some unique attributes that differentiate it from plastic-based and animal-derived products," says Gavin McIntyre, who co-founded Ecovative Design, an upstate New York-based biomaterials company, in 2007 with the goal of displacing some environmentally burdensome materials and making "a meaningful impact on our planet."
After inventing a type of mushroom-based packaging for all sorts of goods, in 2013 the firm ventured into manufacturing mycelium that can be adapted for textiles, he says, because mushrooms are "nature's recycling system."
The company aims for its material—which is "so tough and tenacious" that it doesn't require any plastic add-on as reinforcement—to be generally accessible from a pricing standpoint and not confined to a luxury space. The cost, McIntyre says, would approach that of bovine leather, not the more upscale varieties of lamb and goat skins.
Already, production has taken off by leaps and bounds. In fewer than 10 days in indoor agricultural farms, "we grow large slabs of mycelium that are many feet wide and long," he says. "We are not confined to the shape or geometry of an animal," so there's a much lower scrap rate.
Decreasing the scrap rate is a major selling point. "Our customers can order the pieces to the way that they want them, and there is almost no waste in the processing," explains Ross of MycoWorks. "We can make ours thinner or thicker," depending on a client's specific needs. Growing materials locally also results in a reduction in transportation, shipping, and other supply chain costs, he says.
Yet another advantage to making things out of mycelium is its biodegradability at the end of an item's lifecycle. When a pair of old sneakers lands in a compost pile or landfill, it decomposes thanks to microbial processes that, once again, involve fungi. "It is cool to think that the same organism used to create a product can also be what recycles it, perhaps building something else useful in the same act," says biologist Schilling. That amounts to "more than a nice business model—it is a window into how sustainability works in nature."
A product can be called "sustainable" if it's biodegradable, leaves a minimal carbon footprint during production, and is also profitable, says Preeti Arya, an assistant professor at the Fashion Institute of Technology in New York City and faculty adviser to a student club of the American Association of Textile Chemists and Colorists.
On the opposite end of the spectrum, products composed of petroleum-based polymers don't biodegrade—they break down into smaller pieces or even particles. These remnants pollute landfills, oceans, and rivers, contaminating edible fish and eventually contributing to the growth of benign and cancerous tumors in humans, Arya says.
Commending the steps a few designers have taken toward bringing more environmentally conscious merchandise to consumers, she says, "I'm glad that they took the initiative because others also will try to be part of this competition toward sustainability." And consumers will take notice. "The more people become aware, the more these brands will start acting on it."
A further shift toward mycelium-based products has the capability to reap tremendous environmental dividends, says Drew Endy, associate chair of bioengineering at Stanford University and president of the BioBricks Foundation, which focuses on biotechnology in the public interest.
The continued development of "leather surrogates on a scaled and sustainable basis will provide the greatest benefit to the greatest number of people, in perpetuity," Endy says. "Transitioning the production of leather goods from a process that involves the industrial-scale slaughter of vertebrate mammals to a process that instead uses renewable fungal-based manufacturing will be more just."
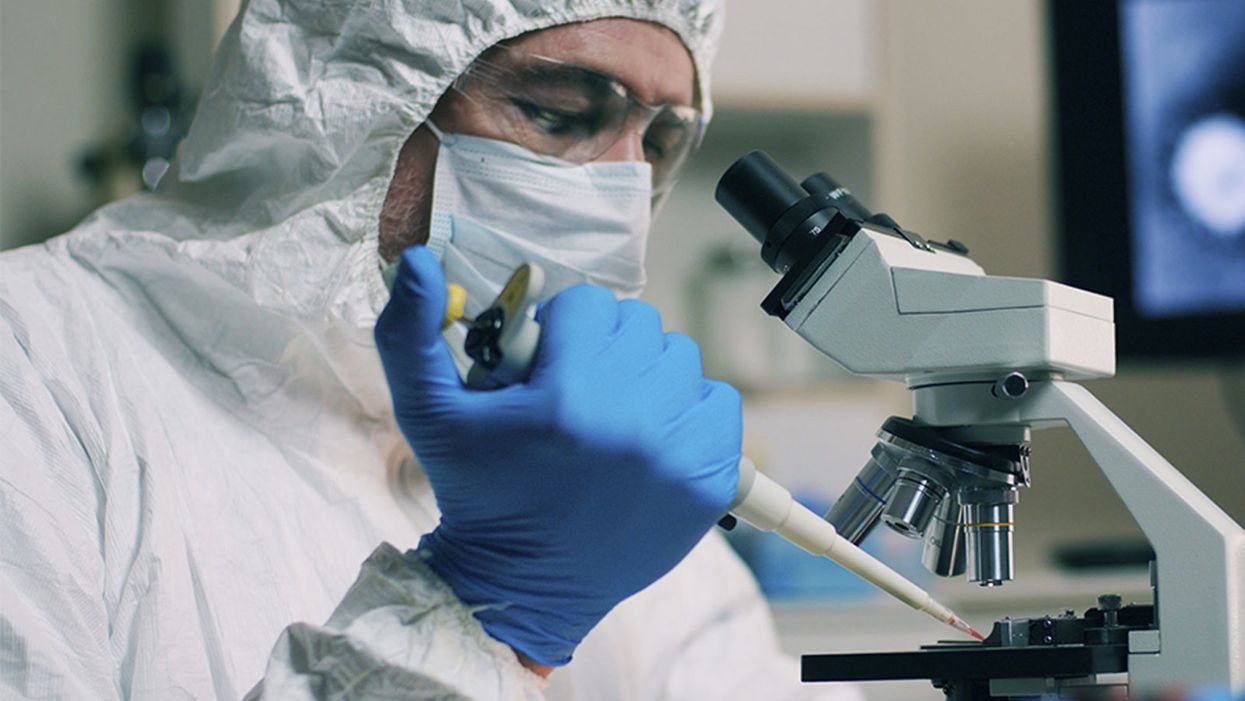
A lab tech handling a sample of the novel coronavirus.
One of the main factors that will influence the ultimate trajectory of the novel coronavirus pandemic will be the availability of a vaccine.
Vaccine development has traditionally been a process measured in years and even decades.
Vaccines are incontrovertibly the best means to control infectious diseases and there are no human vaccines against any of the (now) 7 known human coronaviruses. As soon as the gravity of this outbreak was recognized, several companies, along with governmental and non-governmental partners, have embarked on a rapid development program to develop a vaccine targeted at this virus.
Vaccine development has traditionally been a process measured in years and even decades as scientists tinker with a pathogen trying to weaken or dissemble it to render it capable of creating an effective immune response with acceptable levels of side effects. However, in 2020, powerful new vaccine technologies are available to augment traditional vaccine development and are responsible for the rapid delivery of a vaccine candidate for the start of clinical trials.
Vaccine Platforms: A Game-Changing Technology
The new technologies that are being harnessed are what are known as vaccine platform technologies. Vaccine platforms, as my colleagues and I wrote in a report assessing their promise, offer a means to use the same building blocks to make more than one vaccine. To slightly oversimply, a vaccine platform confers the ability to switch out the pathogen being targeted very rapidly, akin to changing a video game cartridge. Indeed, the recently FDA-licensed Ebola vaccine uses another virus as a platform with the requisite Ebola protein inserted.
Because of this rapid availability to utilize platforms for a variety of different targets, the initial development process can be significantly shortened. This is especially true for vaccines utilizing the genetic material of the target alone. These DNA and RNA vaccines basically can be "printed" once the genetic sequence of the target is known.
An RNA vaccine is the approach being used by the Cambridge-based biotech company Moderna – which took just 42 days to produce an experimental vaccine candidate. Clinical testing is expected to begin next month on 45 healthy volunteers.
Another biotech, the Pennsylvania-based Inovio, is using a DNA approach. In essence, such vaccines involve the genetic material being injected and translated into a viral protein by human cells, which then prompt the immune system to make antibodies.
There are other approaches as well. One company, the Maryland-based Novavax, will use nanoparticles, while another is attempting to adapt an orally administered avian coronavirus vaccine and Johnson & Johnson is using different virus platforms to deliver coronavirus proteins (similar to their experimental Ebola vaccine).
At this stage, it is important for all approaches to be on the table in the hope that at least one makes it through clinical trials. There also may be a need for different types of vaccines for different populations.
Vaccines Will Still Take Time
Despite the quick development time made possible by the use of vaccine platforms, clinical testing for safety, efficacy, and dosing schedules will still take months to complete. After this process, the vaccine will need to be mass produced in large quantities to vaccinate, basically, the world. So, for all intents and purposes, we cannot expect to see an approved vaccine for at least a year or maybe longer if everything does not go perfectly well in clinical trials.
Vaccine platform technologies offer a bright ray of hope in the bleak shadow of the pandemic.
Once a vaccine is available, it will likely appear in batches to be distributed to those at highest risk for severe disease, such as the elderly and those with underlying conditions, as well as healthcare workers, first. At this time, it appears children are less likely to experience severe illness and they may not be the first targets for the vaccine but, if this virus is with us (as is predicted), coronavirus vaccination could become part of routine childhood vaccinations.
Changing Pandemic Trajectory
Vaccination will not come fast enough to impact the initial wave of the novel virus which may continue until summer approaches in temperate climates. However, it will be a crucial tool to blunt the impact of a future appearance in the following respiratory virus season. This reappearance is all but assured as this virus has adeptly established itself in human populations and is behaving like the community-acquired coronavirus that it is.
A Glimmer of Hope
When looking at the trajectory of the virus, it can appear, thus far, that no public health effort has made a substantial impact on the spread of the virus. However, that trajectory will change with the advent of an efficacious vaccine. Such a vaccine, especially if conferring protection against other human coronaviruses, may result in coronaviruses being taken off the table of biological threats altogether in the future.
Vaccine platform technologies offer a bright ray of hope in the bleak shadow of the pandemic and, if successful, will change the way the world approaches future pandemic threats with more rapid deployment of platform-based vaccines.
Dr. Adalja is focused on emerging infectious disease, pandemic preparedness, and biosecurity. He has served on US government panels tasked with developing guidelines for the treatment of plague, botulism, and anthrax in mass casualty settings and the system of care for infectious disease emergencies, and as an external advisor to the New York City Health and Hospital Emergency Management Highly Infectious Disease training program, as well as on a FEMA working group on nuclear disaster recovery. Dr. Adalja is an Associate Editor of the journal Health Security. He was a coeditor of the volume Global Catastrophic Biological Risks, a contributing author for the Handbook of Bioterrorism and Disaster Medicine, the Emergency Medicine CorePendium, Clinical Microbiology Made Ridiculously Simple, UpToDate's section on biological terrorism, and a NATO volume on bioterrorism. He has also published in such journals as the New England Journal of Medicine, the Journal of Infectious Diseases, Clinical Infectious Diseases, Emerging Infectious Diseases, and the Annals of Emergency Medicine. He is a board-certified physician in internal medicine, emergency medicine, infectious diseases, and critical care medicine. Follow him on Twitter: @AmeshAA
Medical Tourism Is Booming, Fueled by High Costs and Slow Access
Bridget Snell traveled to Mexico to access an unapproved stem cell therapy for MS.
When Bridget Snell found out she had multiple sclerosis, she knew she would put up a fight. The 45 year-old mother of two, who lives in Duxbury, Mass., researched options to slow the progress of the disease. The methods she had been trying were invasive, often with side effects of their own.
An estimated 2.2 million Americans will travel abroad for medical care in 2020.
Then she stumbled upon autologous hematopoietic stem cell transplantation (AHSCT), an experimental and controversial procedure that uses the patient's own stem cells to try to halt the progress of the disease. The FDA has not approved this procedure and last year issued a warning about unapproved stem cell therapies.
Despite the lack of established science, Snell weighed her options and decided she would undergo the procedure at Clinica Ruiz, a private clinic in Puebla, Mexico, which boasts of the largest volume of cases in the world using the procedure to treat MS. In April 2018, she went to Mexico for treatment, returned home in a month, and continues to do well.
But a positive outcome is far from assured, says Sheldon Krimsky, adjunct professor in the Department of Public Health and Community Medicine at the Tufts School of Medicine.
"Often you can't get a good sense of what the quality of treatment is in another country," Krimsky says, adding that many companies promise procedures whose results have not been clinically validated. "Unfortunately, people are very easily persuaded by hope."
Traveling for Medical Care
Snell is one of many Americans who have traveled abroad to access medical care. Patients Beyond Borders, a medical tourism consultancy, estimates that 2.2 million Americans will do so in 2020. A 2018 BCC report projected a five-year compounded annual industry growth rate of 13.2 percent. Adding to the demand is the aging population, which is expected to reach 95 million people by 2060 – nearly double the number in 2018.
While Snell traveled to Mexico to try a procedure that was not yet available in the United States, other patients do so for a variety of reasons, primarily cost and speed of access. For example, despite having "pretty good insurance coverage," Washington resident Soniya Gadgil needed dental procedures that would have cost thousands of dollars out-of-pocket. An India native, she decided to travel to Pune, India to visit her parents -- and while there, she got the two root canals and implant that she needed. Gadgil saved 60 percent on the final bill.
Leaving the country for medical care is not restricted to dental work or FDA-banned procedures either. Patients visit countries around the world — South America, Central America, and the Caribbean top the list — for a number of other problems, such as knee and hip replacements and bariatric operations. The most common procedures sought abroad are for dentistry, cosmetic surgery, and cardiac conditions.
Traveling abroad to access less expensive procedures is a damning indictment of healthcare delivery in the United States, says Dr. Leigh Turner, associate professor at the Center for Bioethics at the University of Minnesota. "We have people who are being forced out of the system because of high costs. Collectively it suggests a real structural problem in terms of the organization of healthcare in the United States," Turner says.
The Growth of the Online Marketplace
Nevertheless, medical tourism is booming and a number of online businesses now meet patients' demand for discovery and facilitation of medical care abroad, like PlanMyMedicalTrip.com, Doctoorum.com, and Wellness Travels.
Anurav Rane, CEO and Founder of PlanMyMedicalTrip.com, says the company presents each potential client with options, a la Expedia. A knee replacement in India costs $2,500, a significantly cheaper option even with a $1,110 round-trip airfare from the United States, Rane says. The average cost for an inpatient total knee replacement in the United States in 2019 was a little more $30,000.
Once the client chooses a specific procedure at a specific hospital, the company facilitates the necessary groundwork including the medical visa, tickets, hotel stay, booking the procedure and pre and post-op stay, and consults with the surgeons or doctors even before arrival. "The hassle of planning is on us," Rane says. Once patients are settled in the accommodations, they undergo the procedure.
Playing in the Legal Shadows
The online marketplace companies and the medical team execute an orchestrated dance – but what happens if the patient is harmed during or after the procedure?
Turner says that medical malpractice, if it occurs, can be difficult to pursue abroad. "There are countries where the courts are notoriously slow and it's very difficult to get any kind of meaningful action and settlements," he says, even if the claims have a legitimate basis.
The industry's biggest challenge is trust.
Snell signed a waiver absolving her surgeons in Mexico of any legal claims. But, she points out, that's standard process even for procedures in the United States. "I signed just as many waivers as I would going into any surgery [in the US]."
While that might well be true, Turner argues, Americans don't waive legal rights when they sign consent forms. "There are some protections for patients here in the United States."
Beyond U.S. Medical Tourism
As expected, it's not just Americans who travel abroad for medical care. Lithuania-based Wellness Travels sees a significant percentage of its clients from the EU. PlanMyMedicaltrip.com has 15,000 surgeons and doctors from 12 countries in its database. Egypt-based Doctoorum works with professionals in its own country and attracts clients from the Middle East. It is looking to expand to include doctors from Jordan and India, among other countries.
The term "tourism" is misleading here because it muddies the picture about what post-op should really look like, says Gediminas Kondrackis of Wellness Travels. "Unfortunately a lot of medical travel facilitators mislead their clients by advertising beach holiday packages and the like. Post-op is really about quiet recovery inside for a few days; being out in the sun is not advisable."
The industry's biggest challenge is trust. "The dentist I went to is actually a friend of mine who has a successful practice for several years," says Gadgil, the Washington resident who had dental work done in India. "I'd hesitate to go to someone I don't know or to a place I have no experience with." Her apprehensions are not unusual. After all, anxiety is an expected reaction to any surgery. Word-of-mouth, cost savings, and thorough research may alleviate some of these trust issues.
"I had natural apprehensions and would have had them had I gone up the road to Brigham and Women's (in Boston) just as I did over the border," Snell says, "but I had done my homework extensively. That took a lot of the fear out of it."
Medical tourism will only increase, predicts Kondrackis. "There is still a lot of room to grow. Higher numbers of medical travelers could help reduce the strain on local healthcare systems by reducing wait times and controlling costs."
While patients who have benefited from medical tourism swear by it, the best cure would be to start at home by establishing healthcare equity, Krimsky says.
On the flip side, says Turner, it is debatable whether medical tourism actually benefits host countries, where local residents might get priced out of procedures at these exclusive clinics. Even if laws in host countries such as India might mandate "charity care" for poorer local patients, that does not always happen, Turner says. The trickle-down theory that these more expensive clinics will broaden access to care is often a pipe dream, he adds.
While patients who have benefited from medical tourism swear by it, the best cure would be to start at home by establishing healthcare equity, Krimsky says. "Now if we had universal healthcare in the United States," he adds, "that would be an entirely different story."
Or maybe not. Rane, of PlanMyMedicalTrip.com, has observed an influx of patients to India from Canada, a country with universal healthcare.
The reason they say they travel for care? Long wait times for procedures.