New Hope for Organ Transplantation: Life Without Anti-Rejection Drugs

Kidney transplant patient Robert Waddell, center, with his wife and children after being off immunosuppresants; photo aken last summer in Perdido Key, FL. Left to right: Christian, Bailey, Rob, Karen (wife), Robby and Casey.
Rob Waddell dreaded getting a kidney transplant. He suffers from a genetic condition called polycystic kidney disease that causes the uncontrolled growth of cysts that gradually choke off kidney function. The inherited defect has haunted his family for generations, killing his great grandmother, grandmother, and numerous cousins, aunts and uncles.
But he saw how difficult it was for his mother and sister, who also suffer from this condition, to live with the side effects of the drugs they needed to take to prevent organ rejection, which can cause diabetes, high blood pressure and cancer, and even kidney failure because of their toxicity. Many of his relatives followed the same course, says Waddell: "They were all on dialysis, then a transplant and ended up usually dying from cancers caused by the medications."
When the Louisville native and father of four hit 40, his kidneys barely functioned and the only alternative was either a transplant or the slow death of dialysis. But in 2009, when Waddell heard about an experimental procedure that could eliminate the need for taking antirejection drugs, he jumped at the chance to be their first patient. Devised by scientists at the University of Louisville and Northwestern University, the innovative approach entails mixing stem cells from the live kidney donor with that of the recipient to create a hybrid immune system, known as a chimera, that would trick the immune system and prevent it from attacking the implanted kidney.
The procedure itself was done at Northwestern Memorial Hospital in Chicago, using a live kidney donated by a neighbor of Waddell's, who camped out in Chicago during his recovery. Prior to surgery, Waddell underwent a conditioning treatment that consisted of low dose radiation and chemotherapy to weaken his own immune system and make room for the infusion of stem cells.
"The low intensity chemo and radiation conditioning regimen create just enough space for the donor stem cells to gain a foothold in the bone marrow and the donor's immune system takes over," says Dr. Joseph Levanthal, the transplant surgeon who performed the operation and director of kidney and pancreas transplantation at Northwestern University Feinberg School of Medicine. "That way the recipient develops an immune system that doesn't see the donor organ as foreign."
"As a surgeon, I saw what my patients had to go through—taking 25 pills a day, dying at an early age from heart disease, or having a 35% chance of dying every year on dialysis."
A week later, Waddell had the kidney transplant. The following day, he was infused with a complex cellular cocktail that included blood-forming stem cells derived from his donor's bone marrow mixed what are called tolerance inducing facilitator cells (FCs); these cells help the foreign stem cells get established in the recipient's bone marrow.
Over the course of the following year, he was slowly weaned off of antirejection medications—a precaution in case the procedure didn't work—and remarkably, hasn't needed them since. "I felt better than I had in decades because my kidneys [had been] degrading," recalls Waddell, now 54 and a CPA for a global beverage company. And what's even better is that this new approach offers hope for one of his sons who has also inherited the disorder.
Kidney transplants are the most frequent organ transplants in the world and more than 23,000 of these procedures were done in the United States in 2019, according to the United Network for Organ Sharing. Of this, about 7,000 operations are done annually using live organ donors; the remainder use organs from people who are deceased. Right now, this revolutionary new approach—as well as a similar strategy formulated by Stanford University scientists--is in the final phase of clinical trials. Ultimately, this research may pave the way towards realizing the holy grail of organ transplantation: preventing organ rejection by creating a tolerant state in which the recipient's immune system is compatible with the donor, which would eliminate the need for a lifetime of medications.
"As a surgeon, I saw what my patients had to go through—taking 25 pills a day, dying at an early age from heart disease, or having a 35% chance of dying every year on dialysis," says Dr. Suzanne Ildstad, a transplant surgeon and director of the Institute for Cellular Therapeutics at the University of Louisville, whose discovery of facilitator cells were the basis for this therapeutic platform. Ildstad, who has spent more than two decades searching for a better way, says, "This is something I have worked for my entire life."
The Louisville group uses a combination of chemo and radiation to replace the recipient's immune and blood forming cells with that of the donor. In contrast, the Stanford protocol involves harvesting the donor's blood stem cells and T-cells, which are the foot soldiers of the immune system that fight off infections and would normally orchestrate the rejection of the transplanted organ. Their transplant recipients undergo a milder form of "conditioning" that only radiates discrete parts of the body and selectively targets the recipient's T-cells, creating room for both sets of T-cells, a strategy these researchers believe has a better safety profile and less of a chance of rejection.
"We try to achieve immune tolerance by a true chimerism," says Dr. Samuel Strober, a professor of medicine for immunology and rheumatology at Stanford University and a leader of this research team. "The recipients immune system cells are maintained but mixed in the blood with that of the donor."
Studies suggest both approaches work. In a 2018 clinical trial conducted by Talaris Therapeutics, a Louisville-based biotech founded by Ildstad, 26 of 37 (70%) of the live donor kidney transplant recipients no longer need immunosuppressants. Last fall, Talaris began the final phase of clinical tests that will eventually encompass more than 120 such patients.
The Stanford group's cell-based immunotherapy, which is called MDR-101 and is sponsored by the South San Francisco biotech, Medeor Therapeutics, has had similar results in patients who received organs from live donors who were either well matched, such as one from siblings, meaning they were immunologically identical, or partially matched; Talaris uses unrelated donors where there is only a partial match.
In their 2020 clinical trial of 51 patients, 29 were fully matched and 22 were a partial match; 22 of the fully matched recipients didn't need antirejection drugs and ten of the partial matches were able to stop taking some of these medications without rejection. "With our fully matched, roughly 80% have been completely off drugs up to 14 years later," says Strober, "and reducing the number of drugs from three to one [in the partial matches] means you have far fewer side effects. The goal is to get them off of all drugs."
But these protocols are limited to a small number of patients—living donor kidney recipients. As a consequence, both teams are experimenting with ways to broaden their approach so they can use cadaver organs from deceased donors, with human tests planned in the coming year. Here's how that would work: after the other organs are removed from a deceased donor, stem cells are harvested from the donor's vertebrae in the spinal column and then frozen for storage.
"We do the transplant and give the patient a chance to recover and maintain them on drugs," says Ildstad. "Then we do the tolerance conditioning at a later stage."
If this strategy is successful, it would be a genuine game changer, and open the door to using these protocols for transplanting other cadaver organs, including the heart, lungs and liver. While the overall procedure is complex and costly, in the long run it's less expensive than repeated transplant surgeries, the cost of medications and hospitalizations for complications caused by the drugs, or thrice weekly dialysis treatments, says Ildstad.
And she adds, you can't put a price tag on the vast improvement in quality of life.
Blood Donated from Recovered Coronavirus Patients May Soon Yield a Stopgap Treatment
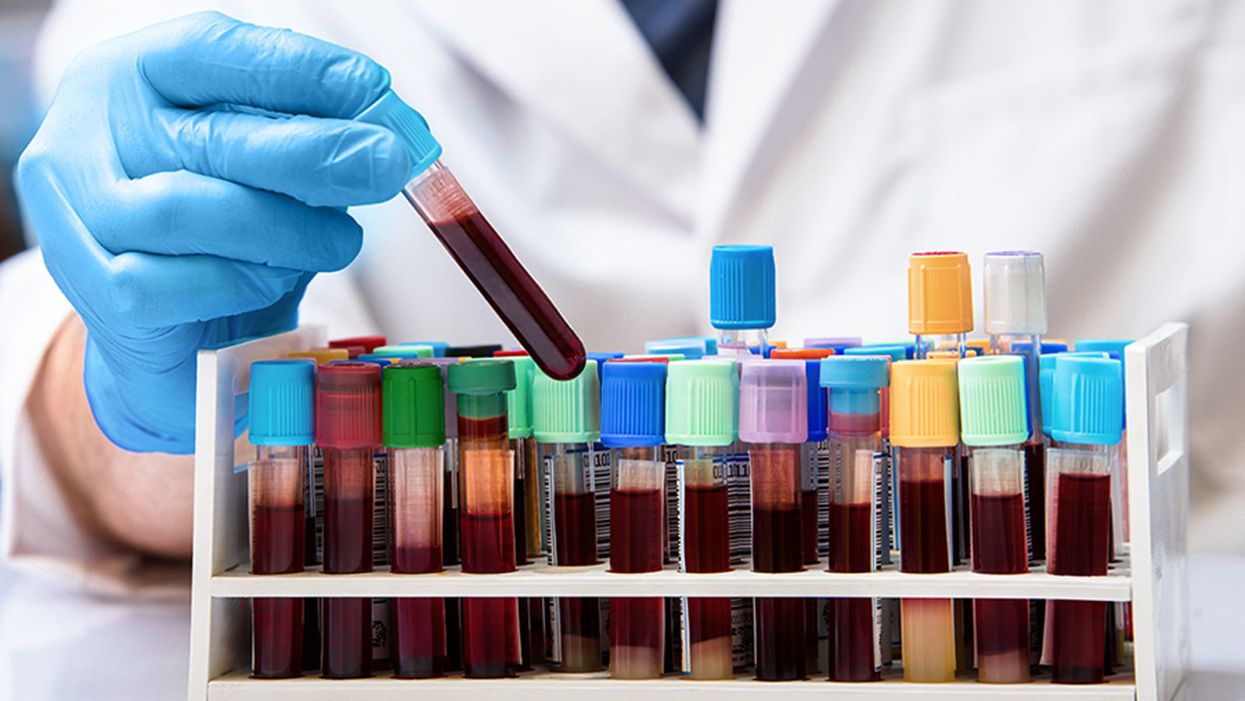
Antibodies from the blood of recovered patients is being tested as a stopgap treatment.
In October 1918, Lieutenant L.W. McGuire of the United States Navy sent a report to the American Journal of Public Health detailing a promising therapy that had already saved the lives of a number of officers suffering from pneumonia complications due to the Spanish influenza outbreak.
"These antibodies then become essentially drugs."
McGuire described how transfusions of blood from recovered patients – an idea which had first been trialed during a polio epidemic in 1916 – had led to rapid recovery in a series of severe pneumonia cases at a Naval Hospital in Massachusetts. "It is believed the serum has a decided influence in shortening the course of the disease, and lowering the mortality," he wrote.
Now more than a century on, this treatment – long forgotten in the western world - is once again coming to the fore during the current COVID-19 pandemic. With fatalities continuing to rise, and no vaccine expected for many months, experts are urging medical centers across the U.S. and Europe to initiate collaborations between critical care and transfusion services to offer this as an emergency treatment for those who need it most.
As of March 20, there are more than 90,000 individuals globally who have recovered from the disease. Some scientists believe that the blood of many of these people contains high levels of neutralizing antibodies that can kill the virus.
"These antibodies then become essentially drugs," said Arturo Casadevall, professor of Molecular Microbiology & Immunology at John Hopkins Bloomberg School of Public Health, who is currently co-ordinating a clinical trial of convalescent serum for COVID-19 involving 20 institutions across the US.
"We're talking about preparing a therapy right out of the serum of those that have recovered. It could also be used in patients who are already sick, but have not progressed to respiratory failure, to treat them before they enter intensive care units. That will provide a lot of support because there's a limited number of respirators and resources."
The first conclusive data on how the blood of recovered patients can help tackle COVID-19 is set to come out of China, where it was also used as an emergency treatment during the SARS and MERS outbreaks. On February 9, a severely ill patient in Wuhan was treated with convalescent serum and since then, hospitals across China have used the therapy on a total of 245 patients, with 91 reportedly showing an improvement in symptoms.
In China alone, more than 58,000 patients have now recovered from COVID-19. Casadevall said that last week the country shipped 90 tons of serum and plasma from these patients to Italy – the center of the pandemic in Europe – for emergency use.
Some of the first people to be treated are likely to be doctors and nurses in hospitals who are most at risk of exposure.
A current challenge, however, is that the blood donation from the recovered patients must be precisely timed in order to maximize the number of antibodies a future patient receives. Doctors in China say that obtaining the necessary blood samples at the right time is one of the major barriers to applying the treatment on a larger scale.
"It's difficult to get the donations," said Dr. Yuan Shi of Chongqing Medical University. "When patients have recovered from the disease, we would like to collect their blood two to four weeks afterwards. We try our best to call back the patients, but it's sometimes difficult to get them to come back within that time period."
Because of such hurdles, Japan's largest drugmaker, Takeda Pharmaceuticals, is now working to turn neutralizing antibodies from recovered COVID-19 patients into a standardized drug product. They hope to launch a clinical trial for this in the next few months.
In the U.S., Casadevall hopes blood transfusions from recovered patients can become clinically available as a therapy within the next four weeks, once regulatory approval has been received. Some of the first people to be treated are likely to be doctors and nurses in hospitals who are most at risk of exposure, to provide a protective boost in their immunity.
"A lot of healthcare workers in the U.S. have already been asked to quarantine, and you can imagine what effect that's going to have on the healthcare system," he said. "It can't take large numbers of people staying home; there's not the capacity."
But not all medical experts are convinced it's the way to go, especially when it comes to the most severe cases of COVID-19. "There's no knowing whether that treatment would be useful or not," warned Dr. Andrew Freedman, head of Cardiff University's School of Medicine in the U.K.
"There are going to be better things available in a few months, but we are facing, 'What do you do now?'"
However, Casadevall says that the treatment is not envisioned as a panacea to treating coronavirus, but simply a temporary measure which could give doctors some options until stronger options such as vaccines or new drugs are available.
"This is a stopgap option," he said. "There are going to be better things available in a few months, but we are facing, 'What do you do now?' The only thing we can offer severely ill people at the moment is respiratory support and oxygen, and we don't have anything to prevent those exposed from going on and getting ill."
Social distancing is a critical part of the strategy to defeat the novel coronavirus.
Kira Peikoff was the editor-in-chief of Leaps.org from 2017 to 2021. As a journalist, her work has appeared in The New York Times, Newsweek, Nautilus, Popular Mechanics, The New York Academy of Sciences, and other outlets. She is also the author of four suspense novels that explore controversial issues arising from scientific innovation: Living Proof, No Time to Die, Die Again Tomorrow, and Mother Knows Best. Peikoff holds a B.A. in Journalism from New York University and an M.S. in Bioethics from Columbia University. She lives in New Jersey with her husband and two young sons. Follow her on Twitter @KiraPeikoff.