Short Story Contest Winner: "The Gerry Program"

A father and son gaze at the ducks in a lake.
It's an odd sensation knowing you're going to die, but it was a feeling Gerry Ferguson had become relatively acquainted with over the past two years. What most perplexed the terminally ill, he observed, was not the concept of death so much as the continuation of all other life.
Gerry's secret project had been in the works for two years now, ever since they found the growth.
Who will mourn me when I'm gone? What trait or idiosyncrasy will people most recall? Will I still be talked of, 100 years from now?
But Gerry didn't worry about these questions. He was comfortable that his legacy would live on, in one form or another. From his cozy flat in the west end of Glasgow, Gerry had managed to put his affairs in order and still find time for small joys.
Feeding the geese in summer at the park just down from his house, reading classics from the teeming bookcase in the living room, talking with his son Michael on Skype. It was Michael who had first suggested reading some of the new works of non-fiction that now littered the large oak desk in Gerry's study.
He was just finishing 'The Master Algorithm' when his shabby grandfather clock chimed six o'clock. Time to call Michael. Crammed into his tiny study, Gerry pulled his computer's webcam close and waved at Michael's smiling face.
"Hi Dad! How're you today?"
"I'm alright, son. How're things in sunny Australia?"
"Hot as always. How's things in Scotland?"
"I'd 'ave more chance gettin' a tan from this computer screen than I do goin' out there."
Michael chuckled. He's got that hearty Ferguson laugh, Gerry thought.
"How's the project coming along?" Michael asked. "Am I going to see it one of these days?"
"Of course," grinned Gerry, "I designed it for you."
Gerry's secret project had been in the works for two years now, ever since they found the growth. He had decided it was better not to tell Michael. He would only worry.
The two men chatted for hours. They discussed Michael's love life (or lack thereof), memories of days walking in the park, and their shared passion, the unending woes of Rangers Football Club. It wasn't until Michael said his goodbyes that Gerry noticed he'd been sitting in the dark for the best part of three hours, his mesh curtains casting a dim orange glow across the room from the street light outside. Time to get back to work.
*
Every night, Gerry sat at his computer, crawling forums, nourishing his project, feeding his knowledge and debating with other programmers. Even at age 82, Gerry knew more than most about algorithms. Never wanting to feel old, and with all the kids so adept at this digital stuff, Gerry figured he should give the Internet a try too. Besides, it kept his brain active and restored some of the sociability he'd lost in the previous decades as old friends passed away and the physical scope of his world contracted.
This night, like every night, Gerry worked away into the wee hours. His back would ache come morning, but this was the only time he truly felt alive these days. From his snug red brick home in Scotland, Gerry could share thoughts and information with strangers from all over the world. It truly was a miracle of modern science!
*
The next day, Gerry woke to the warm amber sun seeping in between a crack in the curtains. Like every morning, his thoughts took a little time to come into focus. Instinctively his hand went to the other side of the bed. Nobody there. Of course; she was gone. Rita, the sweetest woman he'd ever known. Four years this spring, God rest her soul.
Puttering around the cramped kitchen, Gerry heard a knock at the door. Who could that be? He could see two women standing in the hallway, their bodies contorted in the fisheye glass of the peephole. One looked familiar, but Gerry couldn't be sure. He fiddled with the locks and pulled the door open.
"Hi Gerry. How are you today?"
"Fine, thanks," he muttered, still searching his mind for where he'd seen her face before.
Noting the confusion in his eyes, the woman proffered a hand. "Alice, Alice Corgan. I pop round every now and again to check on you."
It clicked. "Ah aye! Come in, come in. Lemme get ya a cuppa." Gerry turned and shuffled into the flat.
As Gerry set about his tiny kitchen, Alice called from the living room, "This is Mandy. She's a care worker too. She's going to pay you occasional visits if that's alright with you."
Gerry poked his head around the doorway. "I'll always welcome a beautiful young lady in ma home. Though, I've tae warn you I'm a married man, so no funny business." He winked and ducked back into the kitchen.
Alice turned to Mandy with a grin. "He's a good man, our Gerry. You'll get along just fine." She lowered her voice. "As I said, with the Alzheimer's, he has to be reminded to take his medication, but he's still mostly self-sufficient. We installed a medi-bot to remind him every day and dispense the pills. If he doesn't respond, we'll get a message to send someone over."
Mandy nodded and scribbled notes in a pad.
"When I'm gone, Michael will have somethin' to remember me by."
"Also, and this is something we've been working on for a few months now, Gerry is convinced he has something…" her voice trailed off. "He thinks he has cancer. Now, while the Alzheimer's may affect his day-to-day life, it's not at a stage where he needs to be taken into care. The last time we went for a checkup, the doctor couldn't find any sign of cancer. I think it stems from--"
Gerry shouted from the other room: "Does the young lady take sugar?"
"No, I'm fine thanks," Mandy called back.
"Of course you don't," smiled Gerry. "Young lady like yersel' is sweet enough."
*
The following week, Mandy arrived early at Gerry's. He looked unsure at first, but he invited her in.
Sitting on the sofa nurturing a cup of tea, Alice tried to keep things light. "So what do you do in your spare time, Gerry?"
"I've got nothing but spare time these days, even if it's running a little low."
"Do you have any hobbies?"
"Yes actually." Gerry smiled. "I'm makin' a computer program."
Alice was taken aback. She knew very little about computers herself. "What's the program for?" she asked.
"Well, despite ma appearance, I'm no spring chicken. I know I don't have much time left. Ma son, he lives down in Australia now, he worked on a computer program that uses AI - that's artificial intelligence - to imitate a person."
Alice still looked confused, so Gerry pressed on.
"Well, I know I've not long left, so I've been usin' this open source code to make ma own for when I'm gone. I've already written all the code. Now I just have to add the things that make it seem like me. I can upload audio, text, even videos of masel'. That way, when I'm gone, Michael will have somethin' to remember me by."
Mandy sat there, stunned. She had no idea anybody could do this, much less an octogenarian from his small, ramshackle flat in Glasgow.
"That's amazing Gerry. I'd love to see the real thing when you're done."
"O' course. I mean, it'll take time. There's so much to add, but I'll be happy to give a demonstration."
Mandy sat there and cradled her mug. Imagine, she thought, being able to preserve yourself, or at least some basic caricature of yourself, forever.
*
As the weeks went on, Gerry slowly added new shades to his coded double. Mandy would leaf through the dusty photo albums on Gerry's bookcase, pointing to photos and asking for the story behind each one. Gerry couldn't always remember but, when he could, the accompanying stories were often hilarious, incredible, and usually a little of both. As he vividly recounted tales of bombing missions over Burma, trips to the beach with a young Michael and, in one particularly interesting story, giving the finger to Margaret Thatcher, Mandy would diligently record them through a Dictaphone to be uploaded to the program.
Gerry loved the company, particularly when he could regale the young woman with tales of his son Michael. One day, as they sat on the sofa flicking through a box of trinkets from his days as a travelling salesman, Mandy asked why he didn't have a smartphone.
He shrugged. "If I'm out 'n about then I want to see the world, not some 2D version of it. Besides, there's nothin' on there for me."
Alice explained that you could get Skype on a smartphone: "You'd be able to talk with Michael and feed the geese at the park at the same time," she offered.
Gerry seemed interested but didn't mention it again.
"Only thing I'm worried about with ma computer," he remarked, "is if there's another power cut and I can't call Michael. There's been a few this year from the snow 'n I hate not bein' able to reach him."
"Well, if you ever want to use the Skype app on my phone to call him you're welcome," said Mandy. "After all, you just need to add him to my contacts."
Gerry was flattered. "That's a relief, knowing I won't miss out on calling Michael if the computer goes bust."
*
Then, in early spring, just as the first green buds burst forth from the bare branches, Gerry asked Mandy to come by. "Bring that Alice girl if ya can - I know she's excited to see this too."
The next day, Mandy and Alice dutifully filed into the cramped study and sat down on rickety wooden chairs brought from the living room for this special occasion.
An image of Gerry, somewhat younger than the man himself, flashed up on the screen.
With a dramatic throat clearing, Gerry opened the program on his computer. An image of Gerry, somewhat younger than the man himself, flashed up on the screen.
The room was silent.
"Hiya Michael!" AI Gerry blurted. The real Gerry looked flustered and clicked around the screen. "I forgot to put the facial recognition on. Michael's just the go-to name when it doesn't recognize a face." His voice lilted with anxious excitement. "This is Alice," Gerry said proudly to the camera, pointing at Alice, "and this is Mandy."
AI Gerry didn't take his eyes from real Gerry, but grinned. "Hello, Alice. Hiya Mandy." The voice was definitely his, even if the flow of speech was slightly disjointed.
"Hi," Alice and Mandy stuttered.
Gerry beamed at both of them. His eyes flitted between the girls and the screen, perhaps nervous that his digital counterpart wasn't as polished as they'd been expecting.
"You can ask him almost anything. He's not as advanced as the ones they're making in the big studios, but I think Michael will like him."
Alice and Mandy gathered closer to the monitor. A mute Gerry grinned back from the screen. Sitting in his wooden chair, the real Gerry turned to his AI twin and began chattering away: "So, what do you think o' the place? Not bad eh?"
"Oh aye, like what you've done wi' it," said AI Gerry.
"Gerry," Alice cut in. "What did you say about Michael there?"
"Ah, I made this for him. After all, it's the kind o' thing his studio was doin'. I had to clear some space to upload it 'n show you guys, so I had to remove Skype for now, but Michael won't mind. Anyway, Mandy's gonna let me Skype him from her phone."
Mandy pulled her phone out and smiled. "Aye, he'll be able to chat with two Gerry's."
Alice grabbed Mandy by the arm: "What did you tell him?" she whispered, her eyes wide.
"I told him he can use my phone if he wants to Skype Michael. Is that okay?"
Alice turned to Gerry, who was chattering away with his computerized clone. "Gerry, we'll just be one second, I need to discuss something with Mandy."
"Righto," he nodded.
Outside the room, Alice paced up and down the narrow hallway.
Mandy could see how flustered she was. "What's wrong? Don't you like the chatbot? I think it's kinda c-"
"Michael's dead," Alice spluttered.
"What do you mean? He talks to him all the time."
Alice sighed. "He doesn't talk to Michael. See, a few years back, Michael found out he had cancer. He worked for this company that did AI chatbot stuff. When he knew he was dying he--" she groped in the air for the words-- "he built this chatbot thing for Gerry, some kind of super-advanced AI. Gerry had just been diagnosed with Alzheimer's and I guess Michael was worried Gerry would forget him. He designed the chatbot to say he was in Australia to explain why he couldn't visit."
"That's awful," Mandy granted, "but I don't get what the problem is. I mean, surely he can show the AI Michael his own chatbot?"
"No, because you can't get the AI Michael on Skype. Michael just designed the program to look like Skype."
"But then--" Mandy went silent.
"Michael uploaded the entire AI to Gerry's computer before his death. Gerry didn't delete Skype. He deleted the AI Michael."
"So… that's it? He-he's gone?" Mandy's voice cracked. "He can't just be gone, surely he can't?"
The women stood staring at each other. They looked to the door of the study. They could still hear Gerry, gabbing away with his cybercopy.
"I can't go back in there," muttered Mandy. Her voice wavered as she tried to stem the misery rising in her throat.
Alice shook her head and paced the floor. She stopped and stared at Mandy with grim resignation. "We don't have a choice."
When they returned, Gerry was still happily chatting away.
"Hiya girls. Ya wanna ask my handsome twin any other questions? If not, we could get Michael on the phone?"
Neither woman spoke. Gerry clapped his hands and turned gaily to the monitor again: "I cannae wait for ya t'meet him, Gerry. He's gonna be impressed wi' you."
Alice clasped her hands to her mouth. Tears welled in the women's eyes as they watched the old man converse with his digital copy. The heat of the room seemed to swell, becoming insufferable. Mandy couldn't take it anymore. She jumped up, bolted to the door and collapsed against a wall in the hallway. Alice perched on the edge of her seat in a dumb daze, praying for the floor to open and swallow the contents of the room whole.
Oblivious, Gerry and his echo babbled away, the blue glow of the screen illuminating his euphoric face. "Just wait until y'meet him Gerry, just wait."
Everyone Should Hear My COVID Vaccine Experience
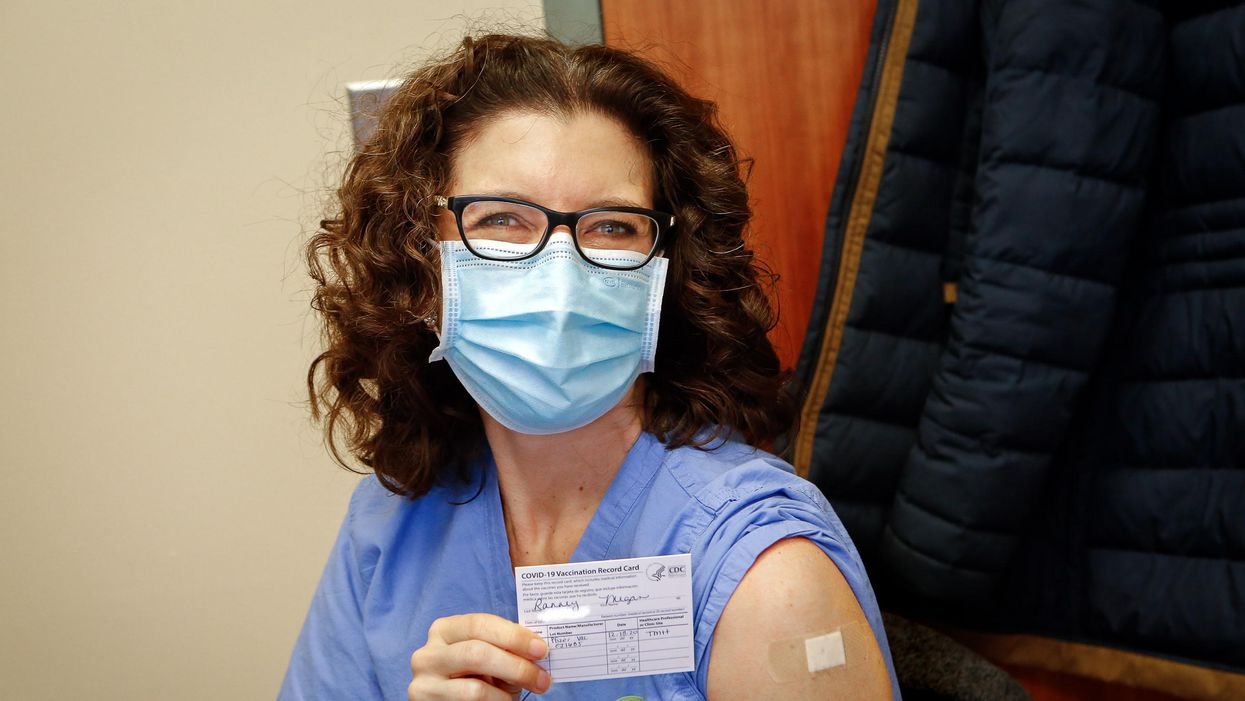
Dr. Ranney immediately after receiving her first dose of the Pfizer vaccine on December 18, 2020.
On December 18th, 2020, I received my first dose of the Pfizer mRNA vaccine against SARS-CoV-2. On January 9th, 2021, I received my second. I am now a CDC-card-carrying, fully vaccinated person.
The build-up to the first dose was momentous. I was scheduled for the first dose of the morning. Our vaccine clinic was abuzz with excitement and hope, and some media folks were there to capture the moment. A couple of fellow emergency physicians were in the same cohort of recipients as I; we exchanged virtual high-fives and took a picture of socially distanced hugs. It was, after all, the closest thing we'd had to a celebration in months.
I walked in the vaccine administration room with anticipation – it was tough to believe this moment was truly, finally here. I got a little video of my getting the shot, took my obligate vaccine selfie, waited in the observation area for 15 minutes to ensure I didn't have a reaction, and then proudly joined 1000s of fellow healthcare workers across the country in posting #ThisIsMyShot on social media. "Here we go, America!"
The first shot, though, didn't actually do all that much for me. It hurt less than a flu shot (which, by the way, doesn't hurt much). I had virtually no side effects. I also knew that it did not yet protect me. The Pfizer (and Moderna) data show very clearly that although the immune response starts to grow 10-12 days after the first shot, one doesn't reach full protection against COVID-19 until much later.
So when, two days after my first shot, I headed back to work in the emergency department, I kept wondering "Will this be the day that I get sick? Wouldn't that be ironic!" Although I never go without an N95 during patient care, it just takes one slip – scratching one's eyes, eating lunch in a break room that an infected colleague had just been in – to get ill. Ten months into this pandemic, it is so easy to get fatigued, to make a small error just one time.
Indeed, I had a few colleagues fall ill in between their first and second shots; one was hospitalized. This was not surprising, but still sad, given how close they had come to escaping infection.
Scientifically speaking, one doesn't need to feel bad to develop an immune response. Emotionally, though, I welcomed the symptoms as proof positive that I would be protected.
This time period felt a little like we had our learner's permit for driving: we were on our way to being safe, but not quite there yet.
I also watched, with dismay, our failures as a nation at timely distribution of the vaccine. On December 18th, despite the logistical snafus that many of us had started to highlight, it was still somewhat believable that we would at least distribute (if not actually administer) 20 million doses by the New Year. But by December 31, my worst fears about the feds' lack of planning had been realized. Only 14 million doses had gone to states, and fewer than 3 million had been administered. Within the public health and medical community, we began to debate how to handle the shortages and slow vaccination rates: should we change prioritization schemes? Get rid of the second dose, in contradiction to what our FDA had approved?
Let me be clear: I really, really, really wanted my second dose. It is what is supported by the data. After living this long at risk, it felt frankly unfair that I might not get fully protected. I waited with trepidation, afraid that policies would shift before I got it in my arm.
At last, my date for my second shot arrived.
This shot was a little less momentous on the outside. The vaccine clinic was much more crowded, as we were now administering first doses to more people, as well as providing the second dose to many. There were no high fives, no media, and I took no selfies. I finished my observation period without trouble (as did everyone else vaccinated the same day, as is typical for these vaccines). I walked out the door planning to spend a nice afternoon outdoors with my kids.
Within 15 minutes, though, the very common side effects – reported by 80% of people my age after the second dose – began to appear. First I got a headache (like 52% of people my age), then body aches (37%), fatigue (59%), and chills (35%). I felt "foggy", like I was fighting something. Like 45% of trial participants who had received the actual vaccine, I took acetaminophen and ibuprofen to stave off the symptoms. There is some minimal evidence from other vaccines that pre-treatment with these anti-inflammatories may reduce antibodies, but given that half of trial participants took these medications, there's no reason to make yourself suffer if you develop side effects. Forty-eight hours later, just in time for my next shift, the side effects magically cleared. Scientifically speaking, one doesn't need to feel bad to develop an immune response. Emotionally, though, I welcomed the symptoms as proof positive that I would be protected.
My reaction was truly typical. Although the media hype focuses on major negative reactions, they are – statistically speaking – tremendously rare: fewer than 11/million people who received the Pfizer vaccine, and 3/million who received the Moderna vaccine, developed anaphylaxis; of these, all were treated, and all are fine. Compare this with the fact that approximately 1200/million Americans have died of this virus. I'll choose the minor, temporary, utterly treatable side effects any day.
Now, more than 14 days after my second dose, the data says that my chance of getting really sick is, truly, infinitesimally low. I don't have to worry that each shift will put me into the hospital. I feel emotionally lighter, and a little bit like I have a secret super-power.
But I also know that we are not yet home free.
I may have my personal equivalent of Harry Potter's invisibility cloak – but we don't yet know whether it protects those around me, at all. As Dr. Fauci himself has written, while community spread is high, there is still a chance that I could be a carrier of infection to others. So I still wear my N95 at work, I still mask in public, and I still shower as soon as I get home from a shift and put my scrubs right in the washing machine to protect my husband and children. I also won't see my parents indoors until they, too, have been vaccinated.
At the end of the day, these vaccines are both amazing and life-changing, and not. My colleagues are getting sick less often, now that many of us are a week or more out from our second dose. I can do things (albeit still masked) that would simply not have been safe a month ago. These are small miracles, for which I am thankful. But like so many things in life, they would be better if shared with others. Only when my community is mostly vaccinated, will I breathe easy again.
My deepest hope is that we all have – and take - the chance to get our shots, soon. Because although the symbolism and effect of the vaccine is high, the experience itself was … not that big a deal.
New Hope for Organ Transplantation: Life Without Anti-Rejection Drugs
Kidney transplant patient Robert Waddell, center, with his wife and children after being off immunosuppresants; photo aken last summer in Perdido Key, FL. Left to right: Christian, Bailey, Rob, Karen (wife), Robby and Casey.
Rob Waddell dreaded getting a kidney transplant. He suffers from a genetic condition called polycystic kidney disease that causes the uncontrolled growth of cysts that gradually choke off kidney function. The inherited defect has haunted his family for generations, killing his great grandmother, grandmother, and numerous cousins, aunts and uncles.
But he saw how difficult it was for his mother and sister, who also suffer from this condition, to live with the side effects of the drugs they needed to take to prevent organ rejection, which can cause diabetes, high blood pressure and cancer, and even kidney failure because of their toxicity. Many of his relatives followed the same course, says Waddell: "They were all on dialysis, then a transplant and ended up usually dying from cancers caused by the medications."
When the Louisville native and father of four hit 40, his kidneys barely functioned and the only alternative was either a transplant or the slow death of dialysis. But in 2009, when Waddell heard about an experimental procedure that could eliminate the need for taking antirejection drugs, he jumped at the chance to be their first patient. Devised by scientists at the University of Louisville and Northwestern University, the innovative approach entails mixing stem cells from the live kidney donor with that of the recipient to create a hybrid immune system, known as a chimera, that would trick the immune system and prevent it from attacking the implanted kidney.
The procedure itself was done at Northwestern Memorial Hospital in Chicago, using a live kidney donated by a neighbor of Waddell's, who camped out in Chicago during his recovery. Prior to surgery, Waddell underwent a conditioning treatment that consisted of low dose radiation and chemotherapy to weaken his own immune system and make room for the infusion of stem cells.
"The low intensity chemo and radiation conditioning regimen create just enough space for the donor stem cells to gain a foothold in the bone marrow and the donor's immune system takes over," says Dr. Joseph Levanthal, the transplant surgeon who performed the operation and director of kidney and pancreas transplantation at Northwestern University Feinberg School of Medicine. "That way the recipient develops an immune system that doesn't see the donor organ as foreign."
"As a surgeon, I saw what my patients had to go through—taking 25 pills a day, dying at an early age from heart disease, or having a 35% chance of dying every year on dialysis."
A week later, Waddell had the kidney transplant. The following day, he was infused with a complex cellular cocktail that included blood-forming stem cells derived from his donor's bone marrow mixed what are called tolerance inducing facilitator cells (FCs); these cells help the foreign stem cells get established in the recipient's bone marrow.
Over the course of the following year, he was slowly weaned off of antirejection medications—a precaution in case the procedure didn't work—and remarkably, hasn't needed them since. "I felt better than I had in decades because my kidneys [had been] degrading," recalls Waddell, now 54 and a CPA for a global beverage company. And what's even better is that this new approach offers hope for one of his sons who has also inherited the disorder.
Kidney transplants are the most frequent organ transplants in the world and more than 23,000 of these procedures were done in the United States in 2019, according to the United Network for Organ Sharing. Of this, about 7,000 operations are done annually using live organ donors; the remainder use organs from people who are deceased. Right now, this revolutionary new approach—as well as a similar strategy formulated by Stanford University scientists--is in the final phase of clinical trials. Ultimately, this research may pave the way towards realizing the holy grail of organ transplantation: preventing organ rejection by creating a tolerant state in which the recipient's immune system is compatible with the donor, which would eliminate the need for a lifetime of medications.
"As a surgeon, I saw what my patients had to go through—taking 25 pills a day, dying at an early age from heart disease, or having a 35% chance of dying every year on dialysis," says Dr. Suzanne Ildstad, a transplant surgeon and director of the Institute for Cellular Therapeutics at the University of Louisville, whose discovery of facilitator cells were the basis for this therapeutic platform. Ildstad, who has spent more than two decades searching for a better way, says, "This is something I have worked for my entire life."
The Louisville group uses a combination of chemo and radiation to replace the recipient's immune and blood forming cells with that of the donor. In contrast, the Stanford protocol involves harvesting the donor's blood stem cells and T-cells, which are the foot soldiers of the immune system that fight off infections and would normally orchestrate the rejection of the transplanted organ. Their transplant recipients undergo a milder form of "conditioning" that only radiates discrete parts of the body and selectively targets the recipient's T-cells, creating room for both sets of T-cells, a strategy these researchers believe has a better safety profile and less of a chance of rejection.
"We try to achieve immune tolerance by a true chimerism," says Dr. Samuel Strober, a professor of medicine for immunology and rheumatology at Stanford University and a leader of this research team. "The recipients immune system cells are maintained but mixed in the blood with that of the donor."
Studies suggest both approaches work. In a 2018 clinical trial conducted by Talaris Therapeutics, a Louisville-based biotech founded by Ildstad, 26 of 37 (70%) of the live donor kidney transplant recipients no longer need immunosuppressants. Last fall, Talaris began the final phase of clinical tests that will eventually encompass more than 120 such patients.
The Stanford group's cell-based immunotherapy, which is called MDR-101 and is sponsored by the South San Francisco biotech, Medeor Therapeutics, has had similar results in patients who received organs from live donors who were either well matched, such as one from siblings, meaning they were immunologically identical, or partially matched; Talaris uses unrelated donors where there is only a partial match.
In their 2020 clinical trial of 51 patients, 29 were fully matched and 22 were a partial match; 22 of the fully matched recipients didn't need antirejection drugs and ten of the partial matches were able to stop taking some of these medications without rejection. "With our fully matched, roughly 80% have been completely off drugs up to 14 years later," says Strober, "and reducing the number of drugs from three to one [in the partial matches] means you have far fewer side effects. The goal is to get them off of all drugs."
But these protocols are limited to a small number of patients—living donor kidney recipients. As a consequence, both teams are experimenting with ways to broaden their approach so they can use cadaver organs from deceased donors, with human tests planned in the coming year. Here's how that would work: after the other organs are removed from a deceased donor, stem cells are harvested from the donor's vertebrae in the spinal column and then frozen for storage.
"We do the transplant and give the patient a chance to recover and maintain them on drugs," says Ildstad. "Then we do the tolerance conditioning at a later stage."
If this strategy is successful, it would be a genuine game changer, and open the door to using these protocols for transplanting other cadaver organs, including the heart, lungs and liver. While the overall procedure is complex and costly, in the long run it's less expensive than repeated transplant surgeries, the cost of medications and hospitalizations for complications caused by the drugs, or thrice weekly dialysis treatments, says Ildstad.
And she adds, you can't put a price tag on the vast improvement in quality of life.