New tools could catch disease outbreaks earlier - or predict them

A team at the Catalan Institution for Research and Advanced Studies is utilizing drones and weather stations to collect data on how mosquito breeding patterns are changing in response to climate shifts.
Every year, the villages which lie in the so-called ‘Nipah belt’— which stretches along the western border between Bangladesh and India, brace themselves for the latest outbreak. For since 1998, when Nipah virus—a form of hemorrhagic fever most common in Bangladesh—first spilled over into humans, it has been a grim annual visitor to the people of this region.
With a 70 percent fatality rate, no vaccine, and no known treatments, Nipah virus has been dubbed in the Western world as ‘the worst disease no one has ever heard of.’ Currently, outbreaks tend to be relatively contained because it is not very transmissible. The virus circulates throughout Asia in fruit eating bats, and only tends to be passed on to people who consume contaminated date palm sap, a sweet drink which is harvested across Bangladesh.
But as SARS-CoV-2 has shown the world, this can quickly change.
“Nipah virus is among what virologists call ‘the Big 10,’ along with things like Lassa fever and Crimean Congo hemorrhagic fever,” says Noam Ross, a disease ecologist at New York-based non-profit EcoHealth Alliance. “These are pretty dangerous viruses from a lethality perspective, which don’t currently have the capacity to spread into broader human populations. But that can evolve, and you could very well see a variant emerge that has human-human transmission capability.”
That’s not an overstatement. Surveys suggest that mammals harbour about 40,000 viruses, with roughly a quarter capable of infecting humans. The vast majority never get a chance to do so because we don’t encounter them, but climate change can alter that. Recent studies have found that as animals relocate to new habitats due to shifting environmental conditions, the coming decades will bring around 300,000 first encounters between species which normally don’t interact, especially in tropical Africa and southeast Asia. All these interactions will make it far more likely for hitherto unknown viruses to cross paths with humans.
That’s why for the last 16 years, EcoHealth Alliance has been conducting ongoing viral surveillance projects across Bangladesh. The goal is to understand why Nipah is so much more prevalent in the western part of the country, compared to the east, and keep a watchful eye out for new Nipah strains as well as other dangerous pathogens like Ebola.
"There are a lot of different infectious agents that are sensitive to climate change that don't have these sorts of software tools being developed for them," says Cat Lippi, medical geography researcher at the University of Florida.
Until very recently this kind of work has been hampered by the limitations of viral surveillance technology. The PREDICT project, a $200 million initiative funded by the United States Agency for International Development, which conducted surveillance across the Amazon Basin, Congo Basin and extensive parts of South and Southeast Asia, relied upon so-called nucleic acid assays which enabled scientists to search for the genetic material of viruses in animal samples.
However, the project came under criticism for being highly inefficient. “That approach requires a big sampling effort, because of the rarity of individual infections,” says Ross. “Any particular animal may be infected for a couple of weeks, maybe once or twice in its lifetime. So if you sample thousands and thousands of animals, you'll eventually get one that has an Ebola virus infection right now.”
Ross explains that there is now far more interest in serological sampling—the scientific term for the process of drawing blood for antibody testing. By searching for the presence of antibodies in the blood of humans and animals, scientists have a greater chance of detecting viruses which started circulating recently.
Despite the controversy surrounding EcoHealth Alliance’s involvement in so-called gain of function research—experiments that study whether viruses might mutate into deadlier strains—the organization’s separate efforts to stay one step ahead of pathogen evolution are key to stopping the next pandemic.
“Having really cheap and fast surveillance is really important,” says Ross. “Particularly in a place where there's persistent, low level, moderate infections that potentially have the ability to develop into more epidemic or pandemic situations. It means there’s a pathway that something more dangerous can come through."
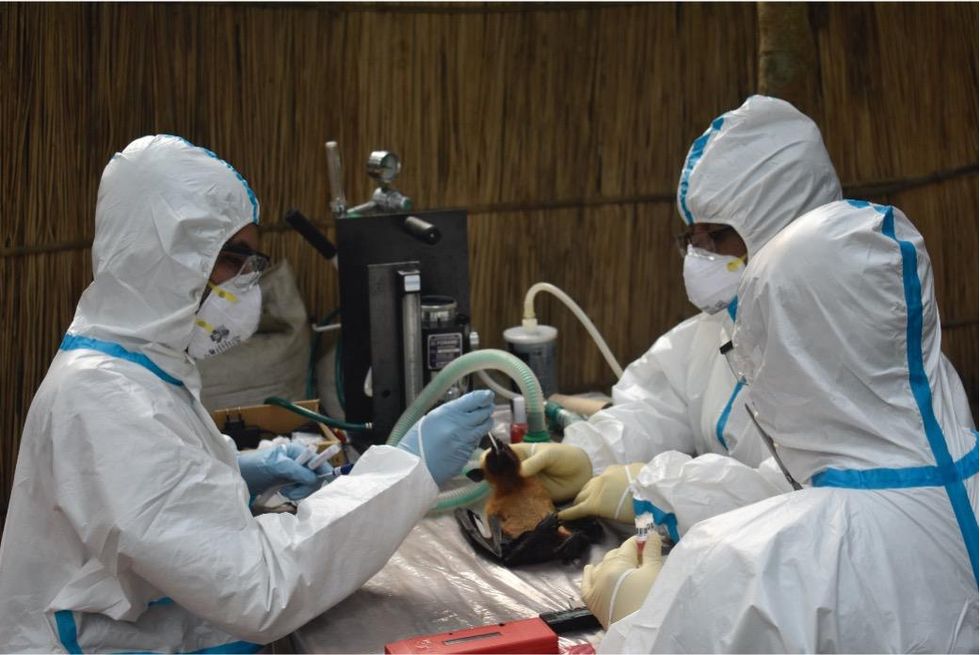
Scientists are searching for the presence of antibodies in the blood of humans and animals in hopes to detect viruses that recently started circulating.
EcoHealth Alliance
In Bangladesh, EcoHealth Alliance is attempting to do this using a newer serological technology known as a multiplex Luminex assay, which tests samples against a panel of known antibodies against many different viruses. It collects what Ross describes as a ‘footprint of information,’ which allows scientists to tell whether the sample contains the presence of a known pathogen or something completely different and needs to be investigated further.
By using this technology to sample human and animal populations across the country, they hope to gain an idea of whether there are any novel Nipah virus variants or strains from the same family, as well as other deadly viral families like Ebola.
This is just one of several novel tools being used for viral discovery in surveillance projects around the globe. Multiple research groups are taking PREDICT’s approach of looking for novel viruses in animals in various hotspots. They collect environmental DNA—mucus, faeces or shed skin left behind in soil, sediment or water—which can then be genetically sequenced.
Five years ago, this would have been a painstaking work requiring bringing collected samples back to labs. Today, thanks to the vast amounts of money spent on new technologies during COVID-19, researchers now have portable sequencing tools they can take out into the field.
Christopher Jerde, a researcher at the UC Santa Barbara Marine Science Institute, points to the Oxford Nanopore MinION sequencer as one example. “I tried one of the early versions of it four years ago, and it was miserable,” he says. “But they’ve really improved, and what we’re going to be able to do in the next five to ten years will be amazing. Instead of having to carefully transport samples back to the lab, we're going to have cigar box-shaped sequencers that we take into the field, plug into a laptop, and do the whole sequencing of an organism.”
In the past, viral surveillance has had to be very targeted and focused on known families of viruses, potentially missing new, previously unknown zoonotic pathogens. Jerde says that the rise of portable sequencers will lead to what he describes as “true surveillance.”
“Before, this was just too complex,” he says. “It had to be very focused, for example, looking for SARS-type viruses. Now we’re able to say, ‘Tell us all the viruses that are here?’ And this will give us true surveillance – we’ll be able to see the diversity of all the pathogens which are in these spots and have an understanding of which ones are coming into the population and causing damage.”
But being able to discover more viruses also comes with certain challenges. Some scientists fear that the speed of viral discovery will soon outpace the human capacity to analyze them all and assess the threat that they pose to us.
“I think we're already there,” says Jason Ladner, assistant professor at Northern Arizona University’s Pathogen and Microbiome Institute. “If you look at all the papers on the expanding RNA virus sphere, there are all of these deposited partial or complete viral sequences in groups that we just don't know anything really about yet.” Bats, for example, carry a myriad of viruses, whose ability to infect human cells we understand very poorly.
Cultivating these viruses under laboratory conditions and testing them on organoids— miniature, simplified versions of organs created from stem cells—can help with these assessments, but it is a slow and painstaking work. One hope is that in the future, machine learning could help automate this process. The new SpillOver Viral Risk Ranking platform aims to assess the risk level of a given virus based on 31 different metrics, while other computer models have tried to do the same based on the similarity of a virus’s genomic sequence to known zoonotic threats.
However, Ladner says that these types of comparisons are still overly simplistic. For one thing, scientists are still only aware of a few hundred zoonotic viruses, which is a very limited data sample for accurately assessing a novel pathogen. Instead, he says that there is a need for virologists to develop models which can determine viral compatibility with human cells, based on genomic data.
“One thing which is really useful, but can be challenging to do, is understand the cell surface receptors that a given virus might use,” he says. “Understanding whether a virus is likely to be able to use proteins on the surface of human cells to gain entry can be very informative.”
As the Earth’s climate heats up, scientists also need to better model the so-called vector borne diseases such as dengue, Zika, chikungunya and yellow fever. Transmitted by the Aedes mosquito residing in humid climates, these blights currently disproportionally affect people in low-income nations. But predictions suggest that as the planet warms and the pests find new homes, an estimated one billion people who currently don’t encounter them might be threatened by their bites by 2080. “When it comes to mosquito-borne diseases we have to worry about shifts in suitable habitat,” says Cat Lippi, a medical geography researcher at the University of Florida. “As climate patterns change on these big scales, we expect to see shifts in where people will be at risk for contracting these diseases.”
Public health practitioners and government decision-makers need tools to make climate-informed decisions about the evolving threat of different infectious diseases. Some projects are already underway. An ongoing collaboration between the Catalan Institution for Research and Advanced Studies and researchers in Brazil and Peru is utilizing drones and weather stations to collect data on how mosquitoes change their breeding patterns in response to climate shifts. This information will then be fed into computer algorithms to predict the impact of mosquito-borne illnesses on different regions.

The team at the Catalan Institution for Research and Advanced Studies is using drones and weather stations to collect data on how mosquito breeding patterns change due to climate shifts.
Gabriel Carrasco
Lippi says that similar models are urgently needed to predict how changing climate patterns affect respiratory, foodborne, waterborne and soilborne illnesses. The UK-based Wellcome Trust has allocated significant assets to fund such projects, which should allow scientists to monitor the impact of climate on a much broader range of infections. “There are a lot of different infectious agents that are sensitive to climate change that don't have these sorts of software tools being developed for them,” she says.
COVID-19’s havoc boosted funding for infectious disease research, but as its threats begin to fade from policymakers’ focus, the money may dry up. Meanwhile, scientists warn that another major infectious disease outbreak is inevitable, potentially within the next decade, so combing the planet for pathogens is vital. “Surveillance is ultimately a really boring thing that a lot of people don't want to put money into, until we have a wide scale pandemic,” Jerde says, but that vigilance is key to thwarting the next deadly horror. “It takes a lot of patience and perseverance to keep looking.”
This article originally appeared in One Health/One Planet, a single-issue magazine that explores how climate change and other environmental shifts are increasing vulnerabilities to infectious diseases by land and by sea. The magazine probes how scientists are making progress with leaders in other fields toward solutions that embrace diverse perspectives and the interconnectedness of all lifeforms and the planet.
Fungus is the ‘New Black’ in Eco-Friendly Fashion
On the left, a Hermès bag made using fine mycelium as a leather alternative, made in partnership with the biotech company MycoWorks; on right, a sheet of mycelium "leather."
A natural material that looks and feels like real leather is taking the fashion world by storm. Scientists view mycelium—the vegetative part of a mushroom-producing fungus—as a planet-friendly alternative to animal hides and plastics.
Products crafted from this vegan leather are emerging, with others poised to hit the market soon. Among them are the Hermès Victoria bag, Lululemon's yoga accessories, Adidas' Stan Smith Mylo sneaker, and a Stella McCartney apparel collection.

The Adidas' Stan Smith Mylo concept sneaker, made in partnership with Bolt Threads, uses an alternative leather grown from mycelium; a commercial version is expected in the near future.
Adidas
Hermès has held presales on the new bag, says Philip Ross, co-founder and chief technology officer of MycoWorks, a San Francisco Bay area firm whose materials constituted the design. By year-end, Ross expects several more clients to debut mycelium-based merchandise. With "comparable qualities to luxury leather," mycelium can be molded to engineer "all the different verticals within fashion," he says, particularly footwear and accessories.
More than a half-dozen trailblazers are fine-tuning mycelium to create next-generation leather materials, according to the Material Innovation Initiative, a nonprofit advocating for animal-free materials in the fashion, automotive, and home-goods industries. These high-performance products can supersede items derived from leather, silk, down, fur, wool, and exotic skins, says A. Sydney Gladman, the institute's chief scientific officer.
That's only the beginning of mycelium's untapped prowess. "We expect to see an uptick in commercial leather alternative applications for mycelium-based materials as companies refine their R&D [research and development] and scale up," Gladman says, adding that "technological innovation and untapped natural materials have the potential to transform the materials industry and solve the enormous environmental challenges it faces."
In fewer than 10 days in indoor agricultural farms, "we grow large slabs of mycelium that are many feet wide and long. We are not confined to the shape or geometry of an animal."
Reducing our carbon footprint becomes possible because mycelium can flourish in indoor farms, using agricultural waste as feedstock and emitting inherently low greenhouse gas emissions. Carbon dioxide is the primary greenhouse gas. "We often think that when plant tissues like wood rot, that they go from something to nothing," says Jonathan Schilling, professor of plant and microbial biology at the University of Minnesota and a member of MycoWorks' Scientific Advisory Board.
But that assumption doesn't hold true for all carbon in plant tissues. When the fungi dominating the decomposition of plants fulfill their function, they transform a large portion of carbon into fungal biomass, Schilling says. That, in turn, ends up in the soil, with mycelium forming a network underneath that traps the carbon.
Unlike the large amounts of fossil fuels needed to produce styrofoam, leather and plastic, less fuel-intensive processing is involved in creating similar materials with a fungal organism. While some fungi consist of a single cell, others are multicellular and develop as very fine threadlike structures. A mass of them collectively forms a "mycelium" that can be either loose and low density or tightly packed and high density. "When these fungi grow at extremely high density," Schilling explains, "they can take on the feel of a solid material such as styrofoam, leather or even plastic."
Tunable and supple in the cultivation process, mycelium is also reliably sturdy in composition. "We believe that mycelium has some unique attributes that differentiate it from plastic-based and animal-derived products," says Gavin McIntyre, who co-founded Ecovative Design, an upstate New York-based biomaterials company, in 2007 with the goal of displacing some environmentally burdensome materials and making "a meaningful impact on our planet."
After inventing a type of mushroom-based packaging for all sorts of goods, in 2013 the firm ventured into manufacturing mycelium that can be adapted for textiles, he says, because mushrooms are "nature's recycling system."
The company aims for its material—which is "so tough and tenacious" that it doesn't require any plastic add-on as reinforcement—to be generally accessible from a pricing standpoint and not confined to a luxury space. The cost, McIntyre says, would approach that of bovine leather, not the more upscale varieties of lamb and goat skins.
Already, production has taken off by leaps and bounds. In fewer than 10 days in indoor agricultural farms, "we grow large slabs of mycelium that are many feet wide and long," he says. "We are not confined to the shape or geometry of an animal," so there's a much lower scrap rate.
Decreasing the scrap rate is a major selling point. "Our customers can order the pieces to the way that they want them, and there is almost no waste in the processing," explains Ross of MycoWorks. "We can make ours thinner or thicker," depending on a client's specific needs. Growing materials locally also results in a reduction in transportation, shipping, and other supply chain costs, he says.
Yet another advantage to making things out of mycelium is its biodegradability at the end of an item's lifecycle. When a pair of old sneakers lands in a compost pile or landfill, it decomposes thanks to microbial processes that, once again, involve fungi. "It is cool to think that the same organism used to create a product can also be what recycles it, perhaps building something else useful in the same act," says biologist Schilling. That amounts to "more than a nice business model—it is a window into how sustainability works in nature."
A product can be called "sustainable" if it's biodegradable, leaves a minimal carbon footprint during production, and is also profitable, says Preeti Arya, an assistant professor at the Fashion Institute of Technology in New York City and faculty adviser to a student club of the American Association of Textile Chemists and Colorists.
On the opposite end of the spectrum, products composed of petroleum-based polymers don't biodegrade—they break down into smaller pieces or even particles. These remnants pollute landfills, oceans, and rivers, contaminating edible fish and eventually contributing to the growth of benign and cancerous tumors in humans, Arya says.
Commending the steps a few designers have taken toward bringing more environmentally conscious merchandise to consumers, she says, "I'm glad that they took the initiative because others also will try to be part of this competition toward sustainability." And consumers will take notice. "The more people become aware, the more these brands will start acting on it."
A further shift toward mycelium-based products has the capability to reap tremendous environmental dividends, says Drew Endy, associate chair of bioengineering at Stanford University and president of the BioBricks Foundation, which focuses on biotechnology in the public interest.
The continued development of "leather surrogates on a scaled and sustainable basis will provide the greatest benefit to the greatest number of people, in perpetuity," Endy says. "Transitioning the production of leather goods from a process that involves the industrial-scale slaughter of vertebrate mammals to a process that instead uses renewable fungal-based manufacturing will be more just."
Can Biotechnology Take the Allergies Out of Cats?
From a special food to a vaccine and gene editing, new technologies may offer solutions for cat lovers with allergies.
Amy Bitterman, who teaches at Rutgers Law School in Newark, gets enormous pleasure from her three mixed-breed rescue cats, Spike, Dee, and Lucy. To manage her chronically stuffy nose, three times a week she takes Allegra D, which combines the antihistamine fexofenadine with the decongestant pseudoephedrine. Amy's dog allergy is rougher--so severe that when her sister launched a business, Pet Care By Susan, from their home in Edison, New Jersey, they knew Susan would have to move elsewhere before she could board dogs. Amy has tried to visit their brother, who owns a Labrador Retriever, taking Allegra D beforehand. But she began sneezing, and then developed watery eyes and phlegm in her chest.
"It gets harder and harder to breathe," she says.
Animal lovers have long dreamed of "hypo-allergenic" cats and dogs. Although to date, there is no such thing, biotechnology is beginning to provide solutions for cat-lovers. Cats are a simpler challenge than dogs. Dog allergies involve as many as seven proteins. But up to 95 percent of people who have cat allergies--estimated at 10 to 30 percent of the population in North America and Europe--react to one protein, Fel d1. Interestingly, cats don't seem to need Fel d1. There are cats who don't produce much Fel d1 and have no known health problems.
The current technologies fight Fel d1 in ingenious ways. Nestle Purina reached the market first with a cat food, Pro Plan LiveClear, launched in the U.S. a year and a half ago. It contains Fel d1 antibodies from eggs that in effect neutralize the protein. HypoCat, a vaccine for cats, induces them to create neutralizing antibodies to their own Fel d1. It may be available in the United States by 2024, says Gary Jennings, chief executive officer of Saiba Animal Health, a University of Zurich spin-off. Another approach, using the gene-editing tool CRISPR to create a medication that would splice out Fel d1 genes in particular tissues, is the furthest from fruition.
"Our goal was to ensure that whatever we do has no negative impact on the cat."
Customer demand is high. "We already have a steady stream of allergic cat owners contacting us desperate to have access to the vaccine or participate in the testing program," Jennings said. "There is a major unmet medical need."
More than a third of Americans own a cat (while half own a dog), and pet ownership is rising. With more Americans living alone, pets may be just the right amount of company. But the number of Americans with asthma increases every year. Of that group, some 20 to 30 percent have pet allergies that could trigger a possibly deadly attack. It is not clear how many pets end up in shelters because their owners could no longer manage allergies. Instead, allergists commonly report that their patients won't give up a beloved companion.
No one can completely avoid Fel d1, which clings to clothing and lands everywhere cat-owners go, even in schools and new homes never occupied by cats. Myths among cat-lovers may lead them to underestimate their own level of risk. Short hair doesn't help: the length of cat hair doesn't affect the production of Fel d1. Bathing your cat will likely upset it and accomplish little. Washing cuts the amount on its skin and fur only for two days. In one study, researchers measured the Fel d1 in the ambient air in a small chamber occupied by a cat—and then washed the cat. Three hours later, with the cat in the chamber again, the measurable Fel d1 in the air was lower. But this benefit was gone after 24 hours.
For years, the best option has been shots for people that prompt protective antibodies. Bitterman received dog and cat allergy injections twice a week as a child. However, these treatments require up to 100 injections over three to five years, and, as in her case, the effect may be partial or wear off. Even if you do opt for shots, treating the cat also makes sense, since you could protect more than one allergic member of your household and any allergic visitors as well.
An Allergy-Neutralizing Diet
Cats produce much of their Fel d1 in their saliva, which then spreads it to their fur when they groom, observed Nestle Purina immunologist Ebenezer Satyaraj. He realized that this made saliva—and therefore a cat's mouth--an unusually effective site for change. Hens exposed to Fel d1 produce their own antibodies, which survive in their eggs. The team coated LiveClear food with a powder form of these eggs; once in a cat's mouth, the chicken antibody binds to the Fel d1 in the cat's saliva, neutralizing it.
The results are partial: In a study with 105 cats, the level of active Fel d1 in their fur had dropped on average by 47 percent after ten weeks eating LiveClear. Cats that produced more Fel d1 at baseline had a more robust response, with a drop of up to 71 percent. A safety study found no effects on cats after six months on the diet. "Our goal was to ensure that whatever we do has no negative impact on the cat," Satyaraj said. Might a dogfood that minimizes dog allergens be on the way? "There is some early work," he said.
A Vaccine
This is a year when vaccines changed the lives of billions. Saiba's vaccine, HypoCat, delivers recombinant Fel d1 and the coat from a plant virus (the Cucumber mosaic virus) without any vital genetic information. The viral coat serves as a carrier. A cat would need shots once or twice a year to produce antibodies that neutralize Fel d1.
HypoCat works much like any vaccine, with the twist that the enemy is the cat's own protein. Is that safe? Saiba's team has followed 70 cats treated with the vaccine over two years and they remain healthy. Again the active Fel d1 doesn't disappear but diminishes. The team asked 10 people with cat allergies to report on their symptoms when they pet their vaccinated cats. Eight of them could pet their cat for nearly a half hour before their symptoms began, compared with an average of 17 minutes before the vaccine.
Jennings hopes to develop a HypoDog shot with a similar approach. However, the goal would be to target four or five proteins in one vaccine, and that increases the risk of hurting the dog. In the meantime, allergic dog-lovers considering an expensive breeder dog might think again: Independent research does not support the idea that any breed of dog produces less dander in the home. In fact, one well-designed study found that Spanish water dogs, Airedales, poodles and Labradoodles--breeds touted as hypo-allergenic--had significantly more of the most common allergen on their coat than an ordinary Lab and the control group.
Gene Editing
One day you might be able to bring your cat to the vet once a year for an injection that would modify specific tissues so they wouldn't produce Fel d1.
Nicole Brackett, a postdoctoral scientist at Viriginia-based Indoor Biotechnologies, which specializes in manufacturing biologics for allergy and asthma, most recently has used CRISPR to identify Fel d1 genetic sequences in cells from 50 domestic cats and 24 exotic ones. She learned that the sequences vary substantially from one cat to the next. This discovery, she says, backs up the observations that Fel d1 doesn't have a vital purpose.
The next step will be a CRISPR knockout of the relevant genes in cells from feline salivary glands, a prime source of Fel d1. Although the company is considering using CRISPR to edit the genes in a cat embryo and possibly produce a Fel d1-free cat, designer cats won't be its ultimate product. Instead, the company aims to produce injections that could treat any cat.
Reducing pet allergens at home could have a compound benefit, Indoor Biotechnologies founder Martin Chapman, an immunologist, notes: "When you dampen down the response to one allergen, you could also dampen it down to multiple allergens." As allergies become more common around the world, that's especially good news.

