New tools could catch disease outbreaks earlier - or predict them

A team at the Catalan Institution for Research and Advanced Studies is utilizing drones and weather stations to collect data on how mosquito breeding patterns are changing in response to climate shifts.
Every year, the villages which lie in the so-called ‘Nipah belt’— which stretches along the western border between Bangladesh and India, brace themselves for the latest outbreak. For since 1998, when Nipah virus—a form of hemorrhagic fever most common in Bangladesh—first spilled over into humans, it has been a grim annual visitor to the people of this region.
With a 70 percent fatality rate, no vaccine, and no known treatments, Nipah virus has been dubbed in the Western world as ‘the worst disease no one has ever heard of.’ Currently, outbreaks tend to be relatively contained because it is not very transmissible. The virus circulates throughout Asia in fruit eating bats, and only tends to be passed on to people who consume contaminated date palm sap, a sweet drink which is harvested across Bangladesh.
But as SARS-CoV-2 has shown the world, this can quickly change.
“Nipah virus is among what virologists call ‘the Big 10,’ along with things like Lassa fever and Crimean Congo hemorrhagic fever,” says Noam Ross, a disease ecologist at New York-based non-profit EcoHealth Alliance. “These are pretty dangerous viruses from a lethality perspective, which don’t currently have the capacity to spread into broader human populations. But that can evolve, and you could very well see a variant emerge that has human-human transmission capability.”
That’s not an overstatement. Surveys suggest that mammals harbour about 40,000 viruses, with roughly a quarter capable of infecting humans. The vast majority never get a chance to do so because we don’t encounter them, but climate change can alter that. Recent studies have found that as animals relocate to new habitats due to shifting environmental conditions, the coming decades will bring around 300,000 first encounters between species which normally don’t interact, especially in tropical Africa and southeast Asia. All these interactions will make it far more likely for hitherto unknown viruses to cross paths with humans.
That’s why for the last 16 years, EcoHealth Alliance has been conducting ongoing viral surveillance projects across Bangladesh. The goal is to understand why Nipah is so much more prevalent in the western part of the country, compared to the east, and keep a watchful eye out for new Nipah strains as well as other dangerous pathogens like Ebola.
"There are a lot of different infectious agents that are sensitive to climate change that don't have these sorts of software tools being developed for them," says Cat Lippi, medical geography researcher at the University of Florida.
Until very recently this kind of work has been hampered by the limitations of viral surveillance technology. The PREDICT project, a $200 million initiative funded by the United States Agency for International Development, which conducted surveillance across the Amazon Basin, Congo Basin and extensive parts of South and Southeast Asia, relied upon so-called nucleic acid assays which enabled scientists to search for the genetic material of viruses in animal samples.
However, the project came under criticism for being highly inefficient. “That approach requires a big sampling effort, because of the rarity of individual infections,” says Ross. “Any particular animal may be infected for a couple of weeks, maybe once or twice in its lifetime. So if you sample thousands and thousands of animals, you'll eventually get one that has an Ebola virus infection right now.”
Ross explains that there is now far more interest in serological sampling—the scientific term for the process of drawing blood for antibody testing. By searching for the presence of antibodies in the blood of humans and animals, scientists have a greater chance of detecting viruses which started circulating recently.
Despite the controversy surrounding EcoHealth Alliance’s involvement in so-called gain of function research—experiments that study whether viruses might mutate into deadlier strains—the organization’s separate efforts to stay one step ahead of pathogen evolution are key to stopping the next pandemic.
“Having really cheap and fast surveillance is really important,” says Ross. “Particularly in a place where there's persistent, low level, moderate infections that potentially have the ability to develop into more epidemic or pandemic situations. It means there’s a pathway that something more dangerous can come through."
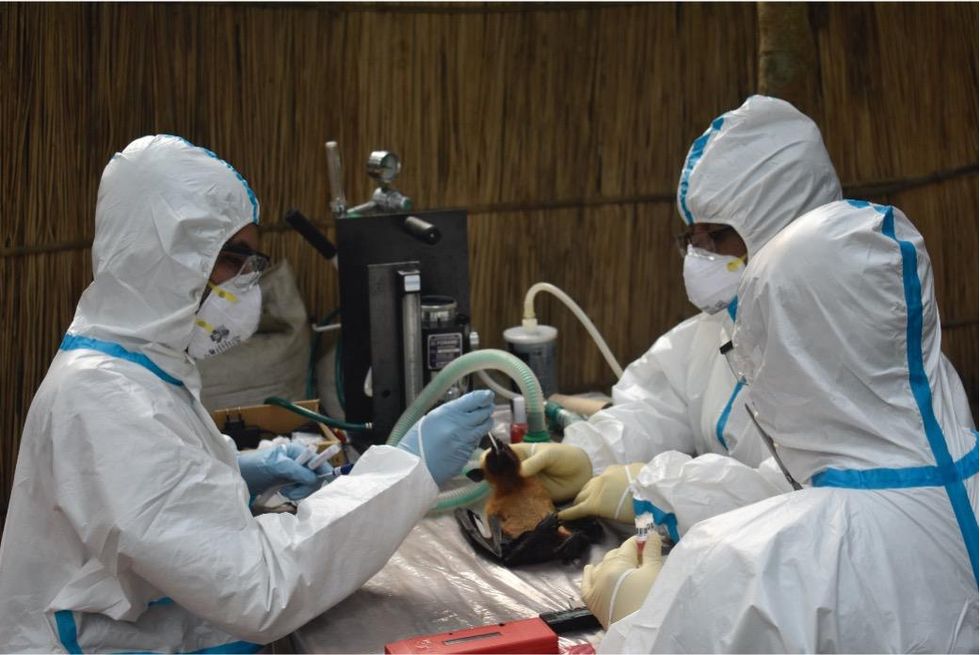
Scientists are searching for the presence of antibodies in the blood of humans and animals in hopes to detect viruses that recently started circulating.
EcoHealth Alliance
In Bangladesh, EcoHealth Alliance is attempting to do this using a newer serological technology known as a multiplex Luminex assay, which tests samples against a panel of known antibodies against many different viruses. It collects what Ross describes as a ‘footprint of information,’ which allows scientists to tell whether the sample contains the presence of a known pathogen or something completely different and needs to be investigated further.
By using this technology to sample human and animal populations across the country, they hope to gain an idea of whether there are any novel Nipah virus variants or strains from the same family, as well as other deadly viral families like Ebola.
This is just one of several novel tools being used for viral discovery in surveillance projects around the globe. Multiple research groups are taking PREDICT’s approach of looking for novel viruses in animals in various hotspots. They collect environmental DNA—mucus, faeces or shed skin left behind in soil, sediment or water—which can then be genetically sequenced.
Five years ago, this would have been a painstaking work requiring bringing collected samples back to labs. Today, thanks to the vast amounts of money spent on new technologies during COVID-19, researchers now have portable sequencing tools they can take out into the field.
Christopher Jerde, a researcher at the UC Santa Barbara Marine Science Institute, points to the Oxford Nanopore MinION sequencer as one example. “I tried one of the early versions of it four years ago, and it was miserable,” he says. “But they’ve really improved, and what we’re going to be able to do in the next five to ten years will be amazing. Instead of having to carefully transport samples back to the lab, we're going to have cigar box-shaped sequencers that we take into the field, plug into a laptop, and do the whole sequencing of an organism.”
In the past, viral surveillance has had to be very targeted and focused on known families of viruses, potentially missing new, previously unknown zoonotic pathogens. Jerde says that the rise of portable sequencers will lead to what he describes as “true surveillance.”
“Before, this was just too complex,” he says. “It had to be very focused, for example, looking for SARS-type viruses. Now we’re able to say, ‘Tell us all the viruses that are here?’ And this will give us true surveillance – we’ll be able to see the diversity of all the pathogens which are in these spots and have an understanding of which ones are coming into the population and causing damage.”
But being able to discover more viruses also comes with certain challenges. Some scientists fear that the speed of viral discovery will soon outpace the human capacity to analyze them all and assess the threat that they pose to us.
“I think we're already there,” says Jason Ladner, assistant professor at Northern Arizona University’s Pathogen and Microbiome Institute. “If you look at all the papers on the expanding RNA virus sphere, there are all of these deposited partial or complete viral sequences in groups that we just don't know anything really about yet.” Bats, for example, carry a myriad of viruses, whose ability to infect human cells we understand very poorly.
Cultivating these viruses under laboratory conditions and testing them on organoids— miniature, simplified versions of organs created from stem cells—can help with these assessments, but it is a slow and painstaking work. One hope is that in the future, machine learning could help automate this process. The new SpillOver Viral Risk Ranking platform aims to assess the risk level of a given virus based on 31 different metrics, while other computer models have tried to do the same based on the similarity of a virus’s genomic sequence to known zoonotic threats.
However, Ladner says that these types of comparisons are still overly simplistic. For one thing, scientists are still only aware of a few hundred zoonotic viruses, which is a very limited data sample for accurately assessing a novel pathogen. Instead, he says that there is a need for virologists to develop models which can determine viral compatibility with human cells, based on genomic data.
“One thing which is really useful, but can be challenging to do, is understand the cell surface receptors that a given virus might use,” he says. “Understanding whether a virus is likely to be able to use proteins on the surface of human cells to gain entry can be very informative.”
As the Earth’s climate heats up, scientists also need to better model the so-called vector borne diseases such as dengue, Zika, chikungunya and yellow fever. Transmitted by the Aedes mosquito residing in humid climates, these blights currently disproportionally affect people in low-income nations. But predictions suggest that as the planet warms and the pests find new homes, an estimated one billion people who currently don’t encounter them might be threatened by their bites by 2080. “When it comes to mosquito-borne diseases we have to worry about shifts in suitable habitat,” says Cat Lippi, a medical geography researcher at the University of Florida. “As climate patterns change on these big scales, we expect to see shifts in where people will be at risk for contracting these diseases.”
Public health practitioners and government decision-makers need tools to make climate-informed decisions about the evolving threat of different infectious diseases. Some projects are already underway. An ongoing collaboration between the Catalan Institution for Research and Advanced Studies and researchers in Brazil and Peru is utilizing drones and weather stations to collect data on how mosquitoes change their breeding patterns in response to climate shifts. This information will then be fed into computer algorithms to predict the impact of mosquito-borne illnesses on different regions.

The team at the Catalan Institution for Research and Advanced Studies is using drones and weather stations to collect data on how mosquito breeding patterns change due to climate shifts.
Gabriel Carrasco
Lippi says that similar models are urgently needed to predict how changing climate patterns affect respiratory, foodborne, waterborne and soilborne illnesses. The UK-based Wellcome Trust has allocated significant assets to fund such projects, which should allow scientists to monitor the impact of climate on a much broader range of infections. “There are a lot of different infectious agents that are sensitive to climate change that don't have these sorts of software tools being developed for them,” she says.
COVID-19’s havoc boosted funding for infectious disease research, but as its threats begin to fade from policymakers’ focus, the money may dry up. Meanwhile, scientists warn that another major infectious disease outbreak is inevitable, potentially within the next decade, so combing the planet for pathogens is vital. “Surveillance is ultimately a really boring thing that a lot of people don't want to put money into, until we have a wide scale pandemic,” Jerde says, but that vigilance is key to thwarting the next deadly horror. “It takes a lot of patience and perseverance to keep looking.”
This article originally appeared in One Health/One Planet, a single-issue magazine that explores how climate change and other environmental shifts are increasing vulnerabilities to infectious diseases by land and by sea. The magazine probes how scientists are making progress with leaders in other fields toward solutions that embrace diverse perspectives and the interconnectedness of all lifeforms and the planet.
A surprising weapon in the fight against food poisoning
Phages, which are harmless viruses that destroy specific bacteria, are becoming useful tools to protect our food supply.
Every year, one in seven people in America comes down with a foodborne illness, typically caused by a bacterial pathogen, including E.Coli, listeria, salmonella, or campylobacter. That adds up to 48 million people, of which 120,000 are hospitalized and 3000 die, according to the Centers for Disease Control. And the variety of foods that can be contaminated with bacterial pathogens is growing too. In the 20th century, E.Coli and listeria lurked primarily within meat. Now they find their way into lettuce, spinach, and other leafy greens, causing periodic consumer scares and product recalls. Onions are the most recent suspected culprit of a nationwide salmonella outbreak.
Some of these incidents are almost inevitable because of how Mother Nature works, explains Divya Jaroni, associate professor of animal and food sciences at Oklahoma State University. These common foodborne pathogens come from the cattle's intestines when the animals shed them in their manure—and then they get washed into rivers and lakes, especially in heavy rains. When this water is later used to irrigate produce farms, the bugs end up on salad greens. Plus, many small farms do both—herd cattle and grow produce.
"Unfortunately for us, these pathogens are part of the microflora of the cows' intestinal tract," Jaroni says. "Some farmers may have an acre or two of cattle pastures, and an acre of a produce farm nearby, so it's easy for this water to contaminate the crops."
Food producers and packagers fight bacteria by potent chemicals, with chlorine being the go-to disinfectant. Cattle carcasses, for example, are typically washed by chlorine solutions as the animals' intestines are removed. Leafy greens are bathed in water with added chlorine solutions. However, because the same "bath" can be used for multiple veggie batches and chlorine evaporates over time, the later rounds may not kill all of the bacteria, sparing some. The natural and organic producers avoid chlorine, substituting it with lactic acid, a more holistic sanitizer, but even with all these efforts, some pathogens survive, sickening consumers and causing food recalls. As we farm more animals and grow more produce, while also striving to use fewer chemicals and more organic growing methods, it will be harder to control bacteria's spread.
"It took us a long time to convince the FDA phages were safe and efficient alternatives. But we had worked with them to gather all the data they needed, and the FDA was very supportive in the end."
Luckily, bacteria have their own killers. Called bacteriophages, or phages for short, they are viruses that prey on bacteria only. Under the electron microscope, they look like fantasy spaceships, with oblong bodies, spider-like legs and long tails. Much smaller than a bacterium, phages pierce the microbes' cells with their tails, sneak in and begin multiplying inside, eventually bursting the microbes open—and then proceed to infect more of them.
The best part is that these phages are harmless to humans. Moreover, recent research finds that millions of phages dwell on us and in us—in our nose, throat, skin and gut, protecting us from bacterial infections as part of our healthy microbiome. A recent study suggested that we absorb about 30 billion phages into our bodies on a daily basis. Now, ingeniously, they are starting to be deployed as anti-microbial agents in the food industry.
A Maryland-based phage research company called Intralytix is doing just that. Founded by Alexander Sulakvelidze, a microbiologist and epidemiologist who came to the United States from Tbilisi, the capital of Georgia, Intralytix makes and sells five different FDA-approved phage cocktails that work against some of the most notorious food pathogens: ListShield for Listeria, SalmoFresh for Salmonella, ShigaShield for Shigella, another foodborne bug, and EcoShield for E.coli, including the infamous strain that caused the Jack in the Box outbreak in 1993 that killed four children and sickened 732 people across four states. Last year, the FDA granted its approval to yet another Intralytix phage for managing Campylobacter contamination, named CampyShield. "We call it safety by nature," Sulakvelidze says.

Intralytix grows phages inside massive 1500-liter fermenters, feeding them bacterial "fodder."
Photo credit: Living Radiant Photography
Phage preparations are relatively straightforward to make. In nature, phages thrive in any body of water where bacteria live too, including rivers, lakes and bays. "I can dip a bucket into the Chesapeake Bay, and it will be full of all kinds of phages," Sulakvelidze says. "Sewage is another great place to look for specific phages of interest, because it's teeming with all sorts of bacteria—and therefore the viruses that prey on them."
In lab settings, Intralytix grows phages inside massive 1500-liter fermenters, feeding them bacterial "fodder." Once phages multiply enough, they are harvested, dispensed into containers and shipped to food producers who have adopted this disinfecting practice into their preparation process. Typically, it's done by computer-controlled sprayer systems that disperse mist-like phage preparations onto the food.
Unlike chemicals like chlorine or antibiotics, which kill a wide spectrum of bacteria, phages are more specialized, each feeding on specific microbial species. A phage that targets salmonella will not prey on listeria and vice versa. So food producers may sometimes use a combo of different phage preparations. Intralytix is continuously researching and testing new phages. With a contract from the National Institutes of Health, Intralytix is expanding its automated high-throughput robot that tests which phages work best against which bacteria, speeding up the development of the new phage cocktails.
Phages have other "talents." In her recent study, Jaroni found that phages have the ability to destroy bacterial biofilms—colonies of microorganisms that tend to grow on surfaces of the food processing equipment, surrounding themselves with protective coating that even very harsh chemicals can't crack.
"Phages are very clever," Jaroni says. "They produce enzymes that target the biofilms, and once they break through, they can reach the bacteria."
Convincing the FDA that phages were safe to use on food products was no easy feat, Sulakvelidze says. In his home country of Georgia, phages have been used as antimicrobial remedies for over a century, but the FDA was leery of using viruses as food safety agents. "It took us a long time to convince the FDA phages were safe and efficient alternatives," Sulakvelidze says. "But we had worked with them to gather all the data they needed, and the FDA was very supportive in the end."
The agency had granted Intralytix its first approval in 2006, and over the past 10 years, the company's sales increased by over 15-fold. "We currently sell to about 40 companies and are in discussions with several other large food producers," Sulakvelidze says. One indicator that the industry now understands and appreciates the science of phages was that his company was ranked as Top Food Safety Provider in 2021 by Food and Beverage Technology Review, he adds. Notably, phage sprays are kosher, halal and organic-certified.
Intralytix's phage cocktails to safeguard food from bacteria are approved for consumers in addition to food producers, but currently the company sells to food producers only. Selling retail requires different packaging like easy-to-use spray bottles and different marketing that would inform people about phages' antimicrobial qualities. But ultimately, giving people the ability to remove pathogens from their food with probiotic phage sprays is the goal, Sulakvelidze says.
It's not the company's only goal. Now Intralytix is going a step further, investigating phages' probiotic and therapeutic abilities. Because phages are highly specialized in the bacteria they target, they can be used to treat infections caused by specific pathogens while leaving the beneficial species of our microbiome intact. In an ongoing clinical trial with Mount Sinai, Intralytix is now investigating a potential phage treatment against a certain type of E. coli for patients with Crohn's disease, and is about to start another clinical trial for treating bacterial dysentery.
"Now that we have proved that phages are safe and effective against foodborne bacteria," Sulakvelidze says, "we are going to demonstrate their potential in therapeutic applications."
This article was first published by Leaps.org on October 27, 2021.
Lina Zeldovich has written about science, medicine and technology for Popular Science, Smithsonian, National Geographic, Scientific American, Reader’s Digest, the New York Times and other major national and international publications. A Columbia J-School alumna, she has won several awards for her stories, including the ASJA Crisis Coverage Award for Covid reporting, and has been a contributing editor at Nautilus Magazine. In 2021, Zeldovich released her first book, The Other Dark Matter, published by the University of Chicago Press, about the science and business of turning waste into wealth and health. You can find her on http://linazeldovich.com/ and @linazeldovich.
Debates over transgender athletes rage on, with new state bans and rules for Olympians, NCAA sports
Some argue that transgender females should be banned from competing with women in sports, while others think such bans are unfair, as the NCAA and other organizations try to keep up with research on how testosterone affects performance.
Ashley O’Connor, who was biologically male at birth but identifies as female, decided to compete in badminton as a girl during her senior year of high school in Downers Grove, Illinois. There was no team for boys, and a female friend and badminton player “practically bullied me into joining” the girls’ team. O’Connor, who is 18 and taking hormone replacement therapy for her gender transition, recalled that “it was easily one of the best decisions I have ever made.”
She believes there are many reasons why it’s important for transgender people to have the option of playing sports on the team of their choice. “It provides a sense of community,” said O’Connor, now a first-year student concentrating in psychology at the College of DuPage in Glen Ellyn, Illinois.
“It’s a great way to get a workout, which is good for physical and mental health,” she added. She also enjoyed the opportunity to be competitive, learn about her strengths and weaknesses, and just be normal. “Trans people have friends and trans people want to play sports with their friends, especially in adolescence,” she said.
However, in 18 states, many of which are politically conservative, laws prohibit transgender students from participating in sports consistent with their gender identity, according to the Movement Advancement Project, an independent, nonprofit think tank based in Boulder, Colo., that focuses on the rights of LGBTQ people. The first ban was passed in Idaho in 2020, although federal district judges have halted this legislation and a similar law in West Virginia from taking effect.
Proponents of the bans caution that transgender females would have an unfair biological advantage in competitive school sports with other girls or women as a result of being born as stronger males, potentially usurping the athletic accomplishments of other athletes.
“The future of women’s sports is at risk, and the equal rights of female athletes is being infringed,” said Penny Nance, CEO and president of Concerned Women for America, a legislative action committee in D.C. that seeks to impact culture to promote religious values.
“As the tidal wave of gender activism consumes sports from the Olympics on down, a backlash is being felt as parents are furious about the disregard for their daughters who have worked very hard to achieve success as athletes,” Nance added. “Former athletes, whose records are being shattered, are demanding answers.”
Meanwhile, opponents of the bans contend that they bar transgender athletes from playing sports with friends and learning the value of teamwork and other life lessons. These laws target transgender girls most often in kindergarten through high school but sometimes in college as well. Many local schools and state athletic associations already have their own guidelines “to both protect transgender people and ensure a level playing field for all athletes,” according to the Movement Advancement Project’s website. But statewide bans take precedence over these policies.
"It’s easy to sympathize on some level with arguments on both sides, and it’s likely going to be impossible to make everyone happy,” said Liz Joy, a past president of the American College of Sports Medicine.
In January, the National Collegiate Athletic Association (NCAA), based in Indianapolis, tried to sort out the controversy by implementing a new policy. It requires transgender students participating in female sports to prove that they’ve been taking treatments to suppress testosterone for at least one year before competition, as well as demonstrating that their testosterone level is sufficiently low, depending on the sport, through a blood test.
Then, in August, the NCAA clarified that these athletes also must take another blood test six months after their season has started that shows their testosterone levels aren’t too high. Additional guidelines will take effect next August.
Even with these requirements, “there is no plan that is going to be considered equitable and fair to all,” said Bradley Anawalt, an endocrinologist at the University of Washington School of Medicine. Biologically, he noted, there is still some evidence that a transgender female who initiates hormone therapy with estrogen and drops her testosterone to very low levels may have some advantage over other females, based on characteristics such as hand and foot size, height and perhaps strength.
Liz Joy, a past president of the American College of Sports Medicine, agrees that allowing transgender athletes to compete on teams of their self-identifying gender poses challenges. “It’s easy to sympathize on some level with arguments on both sides, and it’s likely going to be impossible to make everyone happy,” said Joy, a physician and senior medical director of wellness and nutrition at Intermountain Healthcare in Salt Lake City, Utah. While advocating for inclusion, she added that “sport was incredibly important in my life. I just want everyone to be able to benefit from it.”
One solution may be to allow transgender youth to play sports in a way that aligns with their gender identity until a certain age and before an elite level. “There are minimal or no potential financial stakes for most youth sports before age 13 or 14, and you do not have a lot of separation in athlete performance between most boys and girls until about age 13,” said Anwalt, who was a reviewer of the Endocrine Society’s national guidelines on transgender care.
Myron Genel, a professor emeritus and former chief of pediatric endocrinology at Yale School of Medicine, said it’s difficult to argue that height gives transgender females an edge because in some sports tall women already dominate over their shorter counterparts.
He added that the decision to allow transgender females to compete with other girls or women could hinge on when athletes began taking testosterone blockers. “If the process of conversion from male to female has been undertaken in the early stages of puberty, from my perspective, they have very little unique advantage,” said Genel, who advised the International Olympic Committee (IOC), based in Switzerland, on testosterone limits for transgender athletes.
Because young athletes’ bodies are still developing, “the differences in natural abilities are so massive that they would overwhelm any advantage a transgender athlete might have,” said Thomas H. Murray, president emeritus of The Hastings Center, a pioneering bioethics research institute in Garrison, New York, and author of the book “Good Sport,” which focuses on the ethics and values in the Olympics and other competitions.
“There’s no good reason to limit the participation of transgender athletes in the sports where male athletes don’t have an advantage over women,” such as sailing, archery and shooting events, Murray said. “The burden of proof rests on those who want to restrict participation by transgender athletes. They must show that in this sport, at this level of competition, transgender athletes have a conspicuous advantage.”
Last year, the IOC issued a new framework emphasizing that the Olympic rules related to transgender participation should be specific to each sport. “This is an evolving topic and there has been—as it will continue to be—new research coming out and new developments informing our approach,” and there’s currently no consensus on how testosterone affects performance across all sports, an IOC spokesperson told Leaps.org.
Many of the new laws prohibiting transgender people from competing in sports consistent with their gender identity specifically apply to transgender females. Yet, some experts say the issue also affects transgender males, nonbinary and intersex athletes.
“There has been quite a bit of attention paid to transgender females and their participation in biological female sports and almost minimal focus on transgender male competition in male sports or in any sports,” said Katherine Drabiak, associate professor of public health law and medical ethics at University of South Florida in Tampa. In fact, “transgender men, because they were born female, would be at a disadvantage of having less lean body mass, less strength and less muscular area as a general category compared to a biological male.”
While discussing transgender students’ participation in sports, it’s important to call attention to the toll that anti-transgender legislation can take on these young people’s well-being, said Jonah DeChants, a research scientist at The Trevor Project, a suicide prevention and mental health organization for LGBTQ youth. Recent polling found that 85 percent of transgender and nonbinary youth said that debates around anti-transgender laws had a negative impact on their mental health.
“The reality is simple: Most transgender girls want to play sports for the same reasons as any student—to benefit their health, to have fun, and to build connection with friends,” DeChants said. According to a new peer-reviewed qualitative study by researchers at The Trevor Project, many trans girls who participated in sports experienced harassment and stigma based on their gender identity, which can contribute to poor mental health outcomes and suicide risk.

In addition to badminton, O'Connor played other sports such as volleyball, and she plans to become an assistant coach or manager of her old high school's badminton team.
Ashley O'Connor
However, DeChants added, research also shows that young people who reported living in an accepting community, had access to LGBTQ-affirming spaces, or had social support from family and friends reported significantly lower rates of attempting suicide in the past year. “We urge coaches, educators and school administrators to seek LGBTQ-cultural competency training, implement zero tolerance policies for anti-trans bullying, and create safe, affirming environments for all transgender students on and off the field,” DeChants said.
O’Connor said her experiences on the athletic scene have been mostly positive. The politics of her community lean somewhat liberal, and she thinks it’s probably more supportive than some other areas of the country, though she noted the local library has received threats for hosting LGBTQ events. In addition to badminton, she also played baseball, lacrosse, volleyball, basketball and hockey. In the spring, she plans to become an assistant coach or manager for the girls’ badminton team at her old high school.
“When I played badminton, I never got any direct backlash from any coaches, competitors or teammates,” she said. “I had a few other teammates that identified as trans or nonbinary, [and] nearly all of the people I ever interacted with were super pleasant and treated me like any other normal person.” She added that transgender athletes “have aspirations. We have wants and needs. We have dreams. And at the end of the day, we just want to live our lives and be happy like everyone else.”

