The Sickest Babies Are Covered in Wires. New Tech Is Changing That.
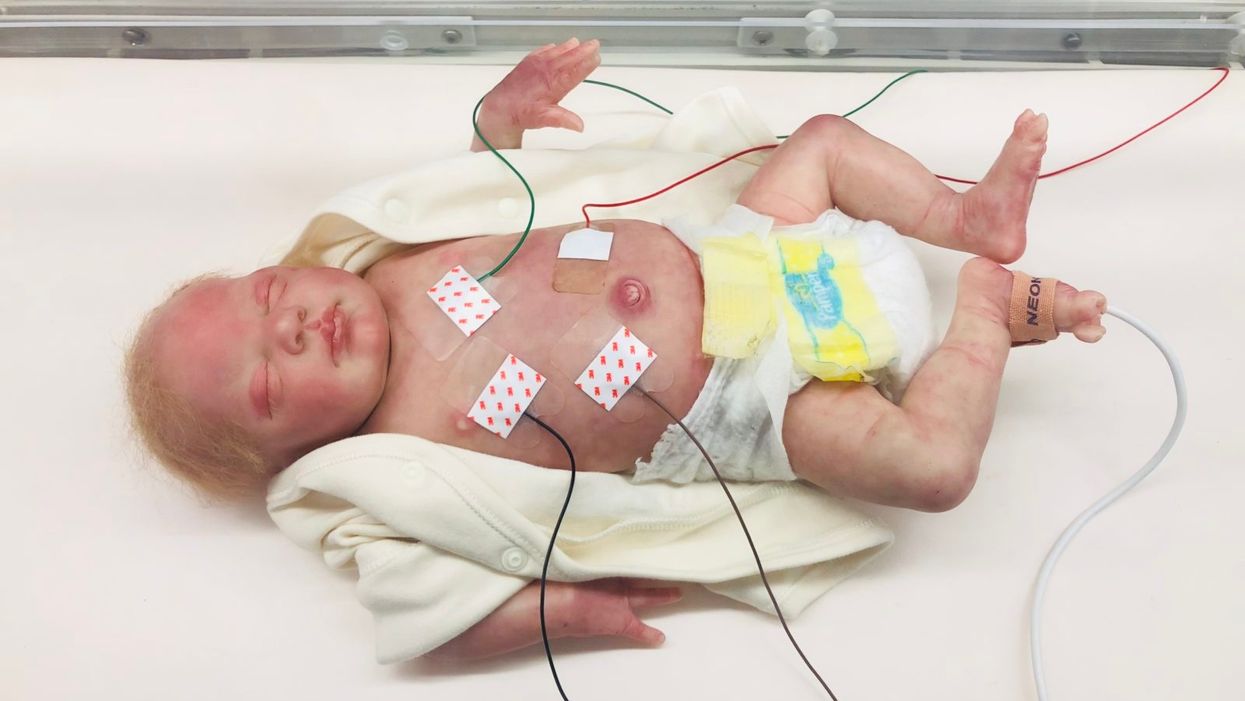
A wired baby in a neonatal intensive care unit.
I'll never forget the experience of having a child in the neonatal intensive care unit (NICU).
Now more than ever, we're working to remove the barriers between new parents and their infants.
It was another layer of uncertainty that filtered into my experience of being a first-time parent. There was so much I didn't know, and the wires attached to my son's small body for the first week of his life were a reminder of that.
I wanted to be the best mother possible. I deeply desired to bring my son home to start our lives. More than anything, I longed for a wireless baby whom I could hold and love freely without limitations.
The wires suggested my baby was fragile and it left me feeling severely unprepared, anxious, and depressed.
In recent years, research has documented the ways that NICU experiences take a toll on parents' mental health. But thankfully, medical technology is rapidly being developed to help reduce the emotional fallout of the NICU. Now more than ever, we're working to remove the barriers between new parents and their infants. The latest example is the first ever wireless monitoring system that was recently developed by a team at Northwestern University.
After listening to the needs of parents and medical staff, Debra Weese-Mayer, M.D., a professor of pediatric autonomic medicine at Feinberg School of Medicine, along with a team of materials scientists, engineers, dermatologists and pediatricians, set out to develop this potentially life-changing technology. Weese-Mayer believes wireless monitoring will have a significant impact for people on all sides of the NICU experience.
"With elimination of the cumbersome wires," she says, "the parents will find their infant more approachable/less intimidating and have improved access to their long-awaited but delivered-too-early infant, allowing them to begin skin-to-skin contact and holding with reduced concern for dislodging wires."
So how does the new system work?
Very thin "skin like" patches made of silicon rubber are placed on the surface of the skin to monitor vitals like heart rate, respiration rate, and body temperature. One patch is placed on the chest or back and the other is placed on the foot.
These patches are safer on the skin than previously used adhesives, reducing the cuts and infections associated with past methods. Finally, an antenna continuously delivers power, often from under the mattress.
The data collected from the patches stream from the body to a tablet or computer.

New wireless sensor technology is being studied to replace wired monitoring in NICUs in the coming years.
(Northwestern University)
Weese-Mayer hopes that wireless systems will be standard soon, but first they must undergo more thorough testing. "I would hope that in the next five years, wireless monitoring will be the standard in NICUs, but there are many essential validation steps before this technology will be embraced nationally," she says.
Until the new systems are ready, parents will be left struggling with the obstacles that wired monitoring presents.
Physical intimacy, for example, appears to have pain-reducing qualities -- something that is particularly important for babies who are battling serious illness. But wires make those cuddles more challenging.
There's also been minimal discussion about how wired monitoring can be particularly limiting for parents with disabilities and mobility aids, or even C-sections.
"When he was first born and I was recovering from my c-section, I couldn't deal with keeping the wires untangled while trying to sit down without hurting myself," says Rhiannon Giles, a writer from North Carolina, who delivered her son at just over 31 weeks after suffering from severe preeclampsia.
"The wires were awful," she remembers. "They fell off constantly when I shifted positions or he kicked a leg, which meant the monitors would alarm. It felt like an intrusion into the quiet little world I was trying to mentally create for us."
Over the last few years, researchers have begun to dive deeper into the literal and metaphorical challenges of wired monitoring.
For many parents, the wires prompt anxiety that worsens an already tense and vulnerable time.
I'll never forget the first time I got to hold my son without wires. It was the first time that motherhood felt manageable.
"Seeing my five-pound-babies covered in wires from head to toe rendered me completely overwhelmed," recalls Caila Smith, a mom of five from Indiana, whose NICU experience began when her twins were born pre-term. "The nurses seemed to handle them perfectly, but I was scared to touch them while they appeared so medically frail."
During the nine days it took for both twins to come home, the limited access she had to her babies started to impact her mental health. "If we would've had wireless sensors and monitors, it would've given us a much greater sense of freedom and confidence when snuggling our newborns," Smith says.
Besides enabling more natural interactions, wireless monitoring would make basic caregiving tasks much easier, like putting on a onesie.
"One thing I noticed is that many preemie outfits are made with zippers," points out Giles, "which just don't work well when your baby has wires coming off of them, head to toe."
Wired systems can pose issues for medical staff as well as parents.
"The main concern regarding wired systems is that they restrict access to the baby and often get tangled with other equipment, like IV lines," says Lamia Soghier, Medical Director of the Neonatal Intensive Care Unit at Children's National in Washington, D.C , who was also a NICU parent herself. "The nurses have to untangle the wires, which takes time, before handing the baby to the family."
I'll never forget the first time I got to hold my son without wires. It was the first time that motherhood felt manageable, and I couldn't stop myself from crying. Suddenly, anything felt possible and all the limitations from that first week of life seemed to fade away. The rise of wired-free monitoring will make some of the stressors that accompany NICU stays a thing of the past.
Waste smothering our oceans is worth billions – here’s what we can do with all that sh$t
In 2015, human poop was valued at $9.5 billion per year, which today would be $11.5 billion. The Ocean Sewage Alliance is uniting experts from key sectors to change how we handle our sewage and, in the process, create all sorts of economic benefits.
There’s hardly a person out there who hasn’t heard of the Great Pacific Garbage Patch. That type of pollution is impossible to miss. It stares you in the face from pictures and videos of sea turtles with drinking straws up their noses and acres of plastic swirling in the sea.
It demands you to solve the problem—and it works. The campaign to raise awareness about plastic pollution in the oceans has resulted in new policies, including bans on microplastics in personal care products, technology to clean up the plastic, and even new plastic-like materials that are better for the environment.
But there’s a different type of pollution smothering the ocean as you read this. Unfortunately, this one is almost invisible, but no less damaging. In fact, it’s even more serious than plastic and most people have no idea it even exists. It is literally under our noses, destroying our oceans, lakes, and rivers – and yet we are missing it completely while contributing to it daily. In fact, we exacerbate it multiple times a day—every time we use the bathroom.
It is the way we do our sewage.
Most of us don’t think much about what happens after we flush the toilet. Most of us probably assume that the substances we flush go “somewhere” and are dealt with safely. But we typically don’t think about it beyond that.
Most of us also probably don’t think about what’s in the ocean or lakes we swim in. Since others are swimming, jumping in is just fine. But our waterways are far from clean. In fact, at times they are incredibly filthy. In the US, we are dumping 1.2 trillion of gallons of untreated sewage into the environment every year. Just New York City alone discharges 27 billion gallons into the Hudson River basin annually.
How does this happen? Part of it is the unfortunate side effect of our sewage system design that dates back to over a century ago when cities were smaller and fewer people were living so close together.
Back then, engineers designed the so-called “combine sewer overflow systems,” or CSOs, in which the storm water pipes are connected to the sanitary sewer pipes. In normal conditions, the sewage effluent from homes flows to the treatment plants where it gets cleaned and released into the waterways. But when it rains, the pipe system becomes so overwhelmed with water that the treatment plant can’t process it fast enough. So the treatment plant has to release the excess water through its discharge pipes—directly, without treatment, into streams, rivers and the ocean.
The 1.2 trillion gallons of CSO releases isn’t even the full picture. There are also discharges from poorly maintained septic systems, cesspools and busted pipes of the aging wastewater infrastructure. The state of Hawaii alone has 88,000 cesspools that need replacing and are currently leaking 53 million gallons of raw sewage daily into their coastal waters. You may think twice about swimming on your Hawaii vacations.
Overall, the US is facing a $271 billion backlog in wastewater infrastructure projects to update these aging systems. Across the Western world, countries are facing similar challenges with their aging sewage systems, especially the UK and European Union.
That’s not to say that other parts of the planet are in better shape. Out of the 7+ billion people populating our earth, 4.2 billion don’t have access to safe sanitation. Included in this insane number are roughly 2 billion people who have no toilet at all. Whether washed by rains or dumped directly into the waterways, a lot of this sludge pollutes the environment, the drinking water, and ultimately the ocean.

Pipes pour water onto a rocky shore in Jakarta, Indonesia.
Tom Fisk
What complicates this from an ocean health perspective is that it’s not just poop and pee that gets dumped into nearby waterways. It is all the things we put in and on our bodies and flush down our drains. That vicious mix of chemicals includes caffeine, antibiotics, antidepressants, painkillers, hormones, microplastics, cocaine, cooking oils, paint thinners, and PFAS—the forever chemicals present in everything from breathable clothing to fire retardant fabrics of our living room couches. Recent reports have found all of the above substances in fish—and then some.
Why do we allow so much untreated sewage spill into the sea? Frankly speaking, for decades scientists and engineers thought that the ocean could handle it. The mantra back then was “dilution is the solution to pollution,” which might’ve worked when there were much fewer people living on earth—but not now. Today science is telling us that this old approach doesn’t hold. That marine habitats are much more sensitive than we had expected and can’t handle the amount of wastewater we are discharging into them.
The excess nitrogen and phosphorus that the sewage (and agricultural runoff) dumps into the water causes harmful algal blooms, more commonly known as red or brown tides. The water column is overtaken by tiny algae that sucks up all the oxygen from the water, creating dead zones like the big fish kills in the Gulf of Mexico. These algae also cause public health issues by releasing gases toxic to people and animals, including dementia, neurological damage, and respiratory illness. Marshes and mangroves end up with weakened root systems and start dying off. In a wastewater modeling study I published last year, we found that 31 percent of salt marshes globally were heavily polluted with human sewage. Coral reefs get riddled with disease and overgrown by seaweed.
We could convert sewage into high-value goods. It can be used to generate electricity, fertilizer, and drinking water. The technologies not only exist but are getting better and more efficient all the time.
Moreover, by way of our sewage, we managed to transmit a human pathogen—Serratia marcescens, which causes urinary, respiratory and other infections in people—to corals! Recent reports from the Florida Keys are showing white pox disease popping up in elk horn corals caused by S.marcescens, which somehow managed to jump species. Many recent studies have documented just how common this type of pollution is across the globe.
Yet, there is some good news in that abysmal sewage flow. Just like with plastic pollution, realizing that there’s a problem is the first step, so awareness is key. That’s exactly why I co-founded Ocean Sewage Alliance last year—a nonprofit that aims to “re-potty train the world” by breaking taboos in talking about the poop and pee problem, as well as uniting experts from various key sectors to work together to end sewage pollution in coastal areas.
To end this pollution, we have to change the ways we handle our sewage. Even more exciting is that by solving the sewage problem we can create all sorts of economic benefits. In 2015, human poop was valued at $9.5 billion a year globally, which today would be $11.5 billion per year.
What would one do with that sh$t?
We could convert it into high-value goods. Sewage can be used to generate electricity, fertilizer, and drinking water. The technologies not only exist but are getting better and more efficient all the time. Some exciting examples include biodigesters and urine diversion (or peecycling) systems that can produce fertilizer and biogas, essentially natural gas. The United Nations estimates that the biogas produced from poop could provide electricity for 138 million homes. And the recovered and cleaned water can be used for irrigation, laundry and flushing toilets. It can even be refined to the point that it is safe for drinking water – just ask the folks in Orange County, CA who have been doing so for the last few decades.
How do we deal with all the human-made pollutants in our sewage? There is technology for that too. Called pyrolysis, it heats up sludge to high temperatures in the absence of oxygen, which causes most of the substances to degrade and fall apart.
There are solutions to the problems—as long as we acknowledge that the problems exist. The fact that you are reading this means that you are part of the solution already. The next time you flush your toilet, think about where this output may flow. Does your septic system work properly? Does your local treatment plant discharge raw sewage on rainy days? Can that plant implement newer technologies that can upcycle waste? These questions are part of re-potty training the world, one household at a time. And together, these households are the force that can turn back the toxic sewage tide. And keep our oceans blue.
The U.S. must fund more biotech innovation – or other countries will catch up faster than you think
In the coming years, U.S. market share in biotech will decline unless the federal government makes investments to improve the quality and quantity of U.S. research, writes the author.
The U.S. has approximately 58 percent of the market share in the biotech sector, followed by China with 11 percent. However, this market share is the result of several years of previous research and development (R&D) – it is a present picture of what happened in the past. In the future, this market share will decline unless the federal government makes investments to improve the quality and quantity of U.S. research in biotech.
The effectiveness of current R&D can be evaluated in a variety of ways such as monies invested and the number of patents filed. According to the UNESCO Institute for Statistics, the U.S. spends approximately 2.7 percent of GDP on R&D ($476,459.0M), whereas China spends 2 percent ($346,266.3M). However, investment levels do not necessarily translate into goods that end up contributing to innovation.
Patents are a better indication of innovation. The biotech industry relies on patents to protect their investments, making patenting a key tool in the process of translating scientific discoveries that can ultimately benefit patients. In 2020, China filed 1,497,159 patents, a 6.9 percent increase in growth rate. In contrast, the U.S. filed 597,172, a 3.9 percent decline. When it comes to patents filed, China has approximately 45 percent of the world share compared to 18 percent for the U.S.
So how did we get here? The nature of science in academia allows scientists to specialize by dedicating several years to advance discovery research and develop new inventions that can then be licensed by biotech companies. This makes academic science critical to innovation in the U.S. and abroad.
Academic scientists rely on government and foundation grants to pay for R&D, which includes salaries for faculty, investigators and trainees, as well as monies for infrastructure, support personnel and research supplies. Of particular interest to academic scientists to cover these costs is government support such as Research Project Grants, also known as R01 grants, the oldest grant mechanism from the National Institutes of Health. Unfortunately, this funding mechanism is extremely competitive, as applications have a success rate of only about 20 percent. To maximize the chances of getting funded, investigators tend to limit the innovation of their applications, since a project that seems overambitious is discouraged by grant reviewers.
Considering the difficulty in obtaining funding, the limited number of opportunities for scientists to become independent investigators capable of leading their own scientific projects, and the salaries available to pay for scientists with a doctoral degree, it is not surprising that the U.S. is progressively losing its workforce for innovation.
This approach affects the future success of the R&D enterprise in the U.S. Pursuing less innovative work tends to produce scientific results that are more obvious than groundbreaking, and when a discovery is obvious, it cannot be patented, resulting in fewer inventions that go on to benefit patients. Even though there are governmental funding options available for scientists in academia focused on more groundbreaking and translational projects, those options are less coveted by academic scientists who are trying to obtain tenure and long-term funding to cover salaries and other associated laboratory expenses. Therefore, since only a small percent of projects gets funded, the likelihood of scientists interested in pursuing academic science or even research in general keeps declining over time.
Efforts to raise the number of individuals who pursue a scientific education are paying off. However, the number of job openings for those trainees to carry out independent scientific research once they graduate has proved harder to increase. These limitations are not just in the number of faculty openings to pursue academic science, which are in part related to grant funding, but also the low salary available to pay those scientists after they obtain their doctoral degree, which ranges from $53,000 to $65,000, depending on years of experience.
Thus, considering the difficulty in obtaining funding, the limited number of opportunities for scientists to become independent investigators capable of leading their own scientific projects, and the salaries available to pay for scientists with a doctoral degree, it is not surprising that the U.S. is progressively losing its workforce for innovation, which results in fewer patents filed.
Perhaps instead of encouraging scientists to propose less innovative projects in order to increase their chances of getting grants, the U.S. government should give serious consideration to funding investigators for their potential for success -- or the success they have already achieved in contributing to the advancement of science. Such a funding approach should be tiered depending on career stage or years of experience, considering that 42 years old is the median age at which the first R01 is obtained. This suggests that after finishing their training, scientists spend 10 years before they establish themselves as independent academic investigators capable of having the appropriate funds to train the next generation of scientists who will help the U.S. maintain or even expand its market share in the biotech industry for years to come. Patenting should be given more weight as part of the academic endeavor for promotion purposes, or governmental investment in research funding should be increased to support more than just 20 percent of projects.
Remaining at the forefront of biotech innovation will give us the opportunity to not just generate more jobs, but it will also allow us to attract the brightest scientists from all over the world. This talented workforce will go on to train future U.S. scientists and will improve our standard of living by giving us the opportunity to produce the next generation of therapies intended to improve human health.
This problem cannot rely on just one solution, but what is certain is that unless there are more creative changes in funding approaches for scientists in academia, eventually we may be saying “remember when the U.S. was at the forefront of biotech innovation?”

