The Sickest Babies Are Covered in Wires. New Tech Is Changing That.
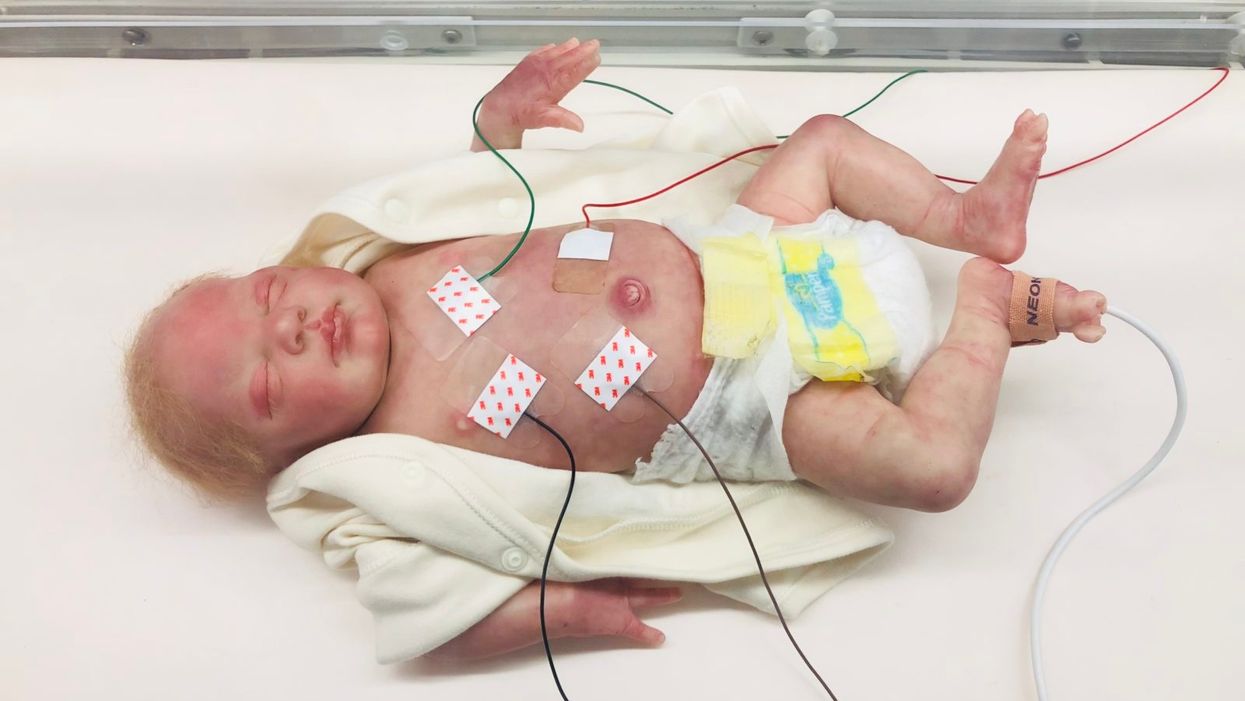
A wired baby in a neonatal intensive care unit.
I'll never forget the experience of having a child in the neonatal intensive care unit (NICU).
Now more than ever, we're working to remove the barriers between new parents and their infants.
It was another layer of uncertainty that filtered into my experience of being a first-time parent. There was so much I didn't know, and the wires attached to my son's small body for the first week of his life were a reminder of that.
I wanted to be the best mother possible. I deeply desired to bring my son home to start our lives. More than anything, I longed for a wireless baby whom I could hold and love freely without limitations.
The wires suggested my baby was fragile and it left me feeling severely unprepared, anxious, and depressed.
In recent years, research has documented the ways that NICU experiences take a toll on parents' mental health. But thankfully, medical technology is rapidly being developed to help reduce the emotional fallout of the NICU. Now more than ever, we're working to remove the barriers between new parents and their infants. The latest example is the first ever wireless monitoring system that was recently developed by a team at Northwestern University.
After listening to the needs of parents and medical staff, Debra Weese-Mayer, M.D., a professor of pediatric autonomic medicine at Feinberg School of Medicine, along with a team of materials scientists, engineers, dermatologists and pediatricians, set out to develop this potentially life-changing technology. Weese-Mayer believes wireless monitoring will have a significant impact for people on all sides of the NICU experience.
"With elimination of the cumbersome wires," she says, "the parents will find their infant more approachable/less intimidating and have improved access to their long-awaited but delivered-too-early infant, allowing them to begin skin-to-skin contact and holding with reduced concern for dislodging wires."
So how does the new system work?
Very thin "skin like" patches made of silicon rubber are placed on the surface of the skin to monitor vitals like heart rate, respiration rate, and body temperature. One patch is placed on the chest or back and the other is placed on the foot.
These patches are safer on the skin than previously used adhesives, reducing the cuts and infections associated with past methods. Finally, an antenna continuously delivers power, often from under the mattress.
The data collected from the patches stream from the body to a tablet or computer.

New wireless sensor technology is being studied to replace wired monitoring in NICUs in the coming years.
(Northwestern University)
Weese-Mayer hopes that wireless systems will be standard soon, but first they must undergo more thorough testing. "I would hope that in the next five years, wireless monitoring will be the standard in NICUs, but there are many essential validation steps before this technology will be embraced nationally," she says.
Until the new systems are ready, parents will be left struggling with the obstacles that wired monitoring presents.
Physical intimacy, for example, appears to have pain-reducing qualities -- something that is particularly important for babies who are battling serious illness. But wires make those cuddles more challenging.
There's also been minimal discussion about how wired monitoring can be particularly limiting for parents with disabilities and mobility aids, or even C-sections.
"When he was first born and I was recovering from my c-section, I couldn't deal with keeping the wires untangled while trying to sit down without hurting myself," says Rhiannon Giles, a writer from North Carolina, who delivered her son at just over 31 weeks after suffering from severe preeclampsia.
"The wires were awful," she remembers. "They fell off constantly when I shifted positions or he kicked a leg, which meant the monitors would alarm. It felt like an intrusion into the quiet little world I was trying to mentally create for us."
Over the last few years, researchers have begun to dive deeper into the literal and metaphorical challenges of wired monitoring.
For many parents, the wires prompt anxiety that worsens an already tense and vulnerable time.
I'll never forget the first time I got to hold my son without wires. It was the first time that motherhood felt manageable.
"Seeing my five-pound-babies covered in wires from head to toe rendered me completely overwhelmed," recalls Caila Smith, a mom of five from Indiana, whose NICU experience began when her twins were born pre-term. "The nurses seemed to handle them perfectly, but I was scared to touch them while they appeared so medically frail."
During the nine days it took for both twins to come home, the limited access she had to her babies started to impact her mental health. "If we would've had wireless sensors and monitors, it would've given us a much greater sense of freedom and confidence when snuggling our newborns," Smith says.
Besides enabling more natural interactions, wireless monitoring would make basic caregiving tasks much easier, like putting on a onesie.
"One thing I noticed is that many preemie outfits are made with zippers," points out Giles, "which just don't work well when your baby has wires coming off of them, head to toe."
Wired systems can pose issues for medical staff as well as parents.
"The main concern regarding wired systems is that they restrict access to the baby and often get tangled with other equipment, like IV lines," says Lamia Soghier, Medical Director of the Neonatal Intensive Care Unit at Children's National in Washington, D.C , who was also a NICU parent herself. "The nurses have to untangle the wires, which takes time, before handing the baby to the family."
I'll never forget the first time I got to hold my son without wires. It was the first time that motherhood felt manageable, and I couldn't stop myself from crying. Suddenly, anything felt possible and all the limitations from that first week of life seemed to fade away. The rise of wired-free monitoring will make some of the stressors that accompany NICU stays a thing of the past.
Should We Use Technologies to Enhance Morality?
Should we welcome biomedical technologies that could enhance our ability to tell right from wrong and improve behaviors that are considered immoral such as dishonesty, prejudice and antisocial aggression?
Our moral ‘hardware’ evolved over 100,000 years ago while humans were still scratching the savannah. The perils we encountered back then were radically different from those that confront us now. To survive and flourish in the face of complex future challenges our archaic operating systems might need an upgrade – in non-traditional ways.
Morality refers to standards of right and wrong when it comes to our beliefs, behaviors, and intentions. Broadly, moral enhancement is the use of biomedical technology to improve moral functioning. This could include augmenting empathy, altruism, or moral reasoning, or curbing antisocial traits like outgroup bias and aggression.
The claims related to moral enhancement are grand and polarizing: it’s been both tendered as a solution to humanity’s existential crises and bluntly dismissed as an armchair hypothesis. So, does the concept have any purchase? The answer leans heavily on our definition and expectations.
One issue is that the debate is often carved up in dichotomies – is moral enhancement feasible or unfeasible? Permissible or impermissible? Fact or fiction? On it goes. While these gesture at imperatives, trading in absolutes blurs the realities at hand. A sensible approach must resist extremes and recognize that moral disrupters are already here.
We know that existing interventions, whether they occur unknowingly or on purpose, have the power to modify moral dispositions in ways both good and bad. For instance, neurotoxins can promote antisocial behavior. The ‘lead-crime hypothesis’ links childhood lead-exposure to impulsivity, antisocial aggression, and various other problems. Mercury has been associated with cognitive deficits, which might impair moral reasoning and judgement. It’s well documented that alcohol makes people more prone to violence.
So, what about positive drivers? Here’s where it gets more tangled.
Medicine has long treated psychiatric disorders with drugs like sedatives and antipsychotics. However, there’s short mention of morality in the Diagnostic and Statistical Manual of Mental Disorders (DSM) despite the moral merits of pharmacotherapy – these effects are implicit and indirect. Such cases are regarded as treatments rather than enhancements.
It would be dangerously myopic to assume that moral augmentation is somehow beyond reach.
Conventionally, an enhancement must go beyond what is ‘normal,’ species-typical, or medically necessary – this is known as the ‘treatment-enhancement distinction.’ But boundaries of health and disease are fluid, so whether we call a procedure ‘moral enhancement’ or ‘medical treatment’ is liable to change with shifts in social values, expert opinions, and clinical practices.
Human enhancements are already used for a range of purported benefits: caffeine, smart drugs, and other supplements to boost cognitive performance; cosmetic procedures for aesthetic reasons; and steroids and stimulants for physical advantage. More boldly, cyborgs like Moon Ribas and Neil Harbisson are pushing transpecies boundaries with new kinds of sensory perception. It would be dangerously myopic to assume that moral augmentation is somehow beyond reach.
How might it work?
One possibility for shaping moral temperaments is with neurostimulation devices. These use electrodes to deliver a low-intensity current that alters the electromagnetic activity of specific neural regions. For instance, transcranial Direct Current Stimulation (tDCS) can target parts of the brain involved in self-awareness, moral judgement, and emotional decision-making. It’s been shown to increase empathy and valued-based learning, and decrease aggression and risk-taking behavior. Many countries already use tDCS to treat pain and depression, but evidence for enhancement effects on healthy subjects is mixed.
Another suggestion is targeting neuromodulators like serotonin and dopamine. Serotonin is linked to prosocial attributes like trust, fairness, and cooperation, but low activity is thought to motivate desires for revenge and harming others. It’s not as simple as indiscriminately boosting brain chemicals though. While serotonin is amenable to SSRIs, precise levels are difficult to measure and track, and there’s no scientific consensus on the “optimum” amount or on whether such a value even exists. Fluctuations due to lifestyle factors such as diet, stress, and exercise add further complexity. Currently, more research is needed on the significance of neuromodulators and their network dynamics across the moral landscape.
There are a range of other prospects. The ‘love drugs’ oxytocin and MDMA mediate pair bonding, cooperation, and social attachment, although some studies suggest that people with high levels of oxytocin are more aggressive toward outsiders. Lithium is a mood stabilizer that has been shown to reduce aggression in prison populations; beta-blockers like propranolol and the supplement omega-3 have similar effects. Increasingly, brain-computer interfaces augur a world of brave possibilities. Such appeals are not without limitations, but they indicate some ways that external tools can positively nudge our moral sentiments.
Who needs morally enhancing?
A common worry is that enhancement technologies could be weaponized for social control by authoritarian regimes, or used like the oppressive eugenics of the early 20th century. Fortunately, the realities are far more mundane and such dystopian visions are fantastical. So, what are some actual possibilities?
Some researchers suggest that neurotechnologies could help to reactivate brain regions of those suffering from moral pathologies, including healthy people with psychopathic traits (like a lack of empathy). Another proposal is using such technology on young people with conduct problems to prevent serious disorders in adulthood.
Most of us aren’t always as ethical as we would like – given the option of ‘priming’ yourself to act in consistent accord with your higher values, would you take it?
A question is whether these kinds of interventions should be compulsory for dangerous criminals. On the other hand, a voluntary treatment for inmates wouldn’t be so different from existing incentive schemes. For instance, some U.S. jurisdictions already offer drug treatment programs in exchange for early release or instead of prison time. Then there’s the difficult question of how we should treat non-criminal but potentially harmful ‘successful’ psychopaths.
Others argue that if virtues have a genetic component, there is no technological reason why present practices of embryo screening for genetic diseases couldn’t also be used for selecting socially beneficial traits.
Perhaps the most immediate scenario is a kind of voluntary moral therapy, which would use biomedicine to facilitate ideal brain-states to augment traditional psychotherapy. Most of us aren’t always as ethical as we would like – given the option of ‘priming’ yourself to act in consistent accord with your higher values, would you take it? Approaches like neurofeedback and psychedelic-assisted therapy could prove helpful.
What are the challenges?
A general challenge is that of setting. Morality is context dependent; what’s good in one environment may be bad in another and vice versa, so we don’t want to throw out the baby with the bathwater. Of course, common sense tells us that some tendencies are more socially desirable than others: fairness, altruism, and openness are clearly preferred over aggression, dishonesty, and prejudice.
One argument is that remoulding ‘brute impulses’ via biology would not count as moral enhancement. This view claims that for an action to truly count as moral it must involve cognition – reasoning, deliberation, judgement – as a necessary part of moral behavior. Critics argue that we should be concerned more with ends rather than means, so ultimately it’s outcomes that matter most.
Another worry is that modifying one biological aspect will have adverse knock-on effects for other valuable traits. Certainly, we must be careful about the network impacts of any intervention. But all stimuli have distributed effects on the body, so it’s really a matter of weighing up the cost/benefit trade-offs as in any standard medical decision.
Is it ethical?
Our values form a big part of who we are – some bioethicists argue that altering morality would pose a threat to character and personal identity. Another claim is that moral enhancement would compromise autonomy by limiting a person’s range of choices and curbing their ‘freedom to fall.’ Any intervention must consider the potential impacts on selfhood and personal liberty, in addition to the wider social implications.
This includes the importance of social and genetic diversity, which is closely tied to considerations of fairness, equality, and opportunity. The history of psychiatry is rife with examples of systematic oppression, like ‘drapetomania’ – the spurious mental illness that was thought to cause African slaves’ desire to flee captivity. Advocates for using moral enhancement technologies to help kids with conduct problems should be mindful that they disproportionately come from low-income communities. We must ensure that any habilitative practice doesn’t perpetuate harmful prejudices by unfairly targeting marginalized people.
Human capacities are the result of environmental influences, and external conditions still coax our biology in unknown ways. Status quo bias for ‘letting nature take its course’ may actually be worse long term – failing to utilize technology for human development may do more harm than good.
Then, there are concerns that morally-enhanced persons would be vulnerable to predation by those who deliberately avoid moral therapies. This relates to what’s been dubbed the ‘bootstrapping problem’: would-be moral enhancement candidates are the types of individuals that benefit from not being morally enhanced. Imagine if every senator was asked to undergo an honesty-boosting procedure prior to entering public office – would they go willingly? Then again, perhaps a technological truth-serum wouldn’t be such a bad requisite for those in positions of stern social consequence.
Advocates argue that biomedical moral betterment would simply offer another means of pursuing the same goals as fixed social mechanisms like religion, education, and community, and non-invasive therapies like cognitive-behavior therapy and meditation. It’s even possible that technological efforts would be more effective. After all, human capacities are the result of environmental influences, and external conditions still coax our biology in unknown ways. Status quo bias for ‘letting nature take its course’ may actually be worse long term – failing to utilize technology for human development may do more harm than good. If we can safely improve ourselves in direct and deliberate ways then there’s no morally significant difference whether this happens via conventional methods or new technology.
Future prospects
Where speculation about human enhancement has led to hype and technophilia, many bioethicists urge restraint. We can be grounded in current science while anticipating feasible medium-term prospects. It’s unlikely moral enhancement heralds any metamorphic post-human utopia (or dystopia), but that doesn’t mean dismissing its transformative potential. In one sense, we should be wary of transhumanist fervour about the salvatory promise of new technology. By the same token we must resist technofear and alarmist efforts to balk social and scientific progress. Emerging methods will continue to shape morality in subtle and not-so-subtle ways – the critical steps are spotting and scaffolding these with robust ethical discussion, public engagement, and reasonable policy options. Steering a bright and judicious course requires that we pilot the possibilities of morally-disruptive technologies.
Podcast: The Friday Five - your health research roundup
The Friday Five is a new series in which Leaps.org covers five breakthroughs in research over the previous week that you may have missed.
The Friday Five is a new podcast series in which Leaps.org covers five breakthroughs in research over the previous week that you may have missed. There are plenty of controversies and ethical issues in science – and we get into many of them in our online magazine – but there’s also plenty to be excited about, and this news roundup is focused on inspiring scientific work to give you some momentum headed into the weekend.
Covered in this week's Friday Five:
- Puffer fish chemical for treating chronic pain
- Sleep study on the health benefits of waking up multiples times per night
- Best exercise regimens for reducing the risk of mortality aka living longer
- AI breakthrough in mapping protein structures with DeepMind
- Ultrasound stickers to see inside your body

