The Sickest Babies Are Covered in Wires. New Tech Is Changing That.
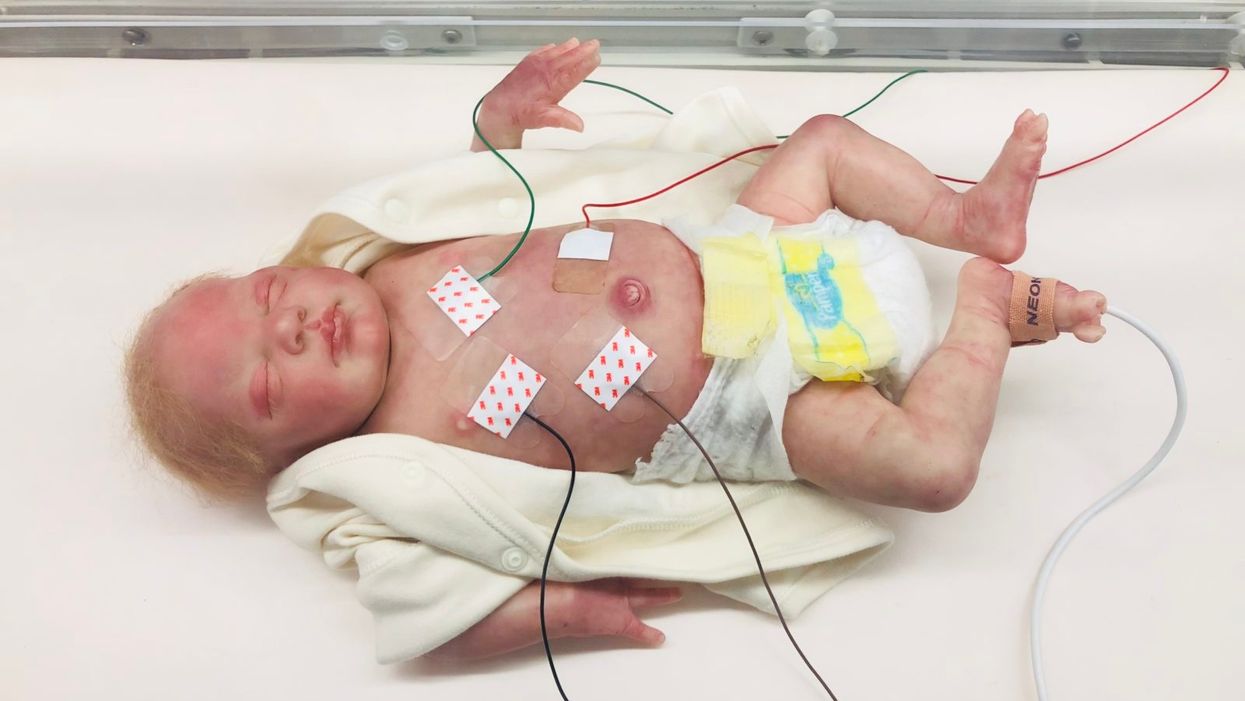
A wired baby in a neonatal intensive care unit.
I'll never forget the experience of having a child in the neonatal intensive care unit (NICU).
Now more than ever, we're working to remove the barriers between new parents and their infants.
It was another layer of uncertainty that filtered into my experience of being a first-time parent. There was so much I didn't know, and the wires attached to my son's small body for the first week of his life were a reminder of that.
I wanted to be the best mother possible. I deeply desired to bring my son home to start our lives. More than anything, I longed for a wireless baby whom I could hold and love freely without limitations.
The wires suggested my baby was fragile and it left me feeling severely unprepared, anxious, and depressed.
In recent years, research has documented the ways that NICU experiences take a toll on parents' mental health. But thankfully, medical technology is rapidly being developed to help reduce the emotional fallout of the NICU. Now more than ever, we're working to remove the barriers between new parents and their infants. The latest example is the first ever wireless monitoring system that was recently developed by a team at Northwestern University.
After listening to the needs of parents and medical staff, Debra Weese-Mayer, M.D., a professor of pediatric autonomic medicine at Feinberg School of Medicine, along with a team of materials scientists, engineers, dermatologists and pediatricians, set out to develop this potentially life-changing technology. Weese-Mayer believes wireless monitoring will have a significant impact for people on all sides of the NICU experience.
"With elimination of the cumbersome wires," she says, "the parents will find their infant more approachable/less intimidating and have improved access to their long-awaited but delivered-too-early infant, allowing them to begin skin-to-skin contact and holding with reduced concern for dislodging wires."
So how does the new system work?
Very thin "skin like" patches made of silicon rubber are placed on the surface of the skin to monitor vitals like heart rate, respiration rate, and body temperature. One patch is placed on the chest or back and the other is placed on the foot.
These patches are safer on the skin than previously used adhesives, reducing the cuts and infections associated with past methods. Finally, an antenna continuously delivers power, often from under the mattress.
The data collected from the patches stream from the body to a tablet or computer.

New wireless sensor technology is being studied to replace wired monitoring in NICUs in the coming years.
(Northwestern University)
Weese-Mayer hopes that wireless systems will be standard soon, but first they must undergo more thorough testing. "I would hope that in the next five years, wireless monitoring will be the standard in NICUs, but there are many essential validation steps before this technology will be embraced nationally," she says.
Until the new systems are ready, parents will be left struggling with the obstacles that wired monitoring presents.
Physical intimacy, for example, appears to have pain-reducing qualities -- something that is particularly important for babies who are battling serious illness. But wires make those cuddles more challenging.
There's also been minimal discussion about how wired monitoring can be particularly limiting for parents with disabilities and mobility aids, or even C-sections.
"When he was first born and I was recovering from my c-section, I couldn't deal with keeping the wires untangled while trying to sit down without hurting myself," says Rhiannon Giles, a writer from North Carolina, who delivered her son at just over 31 weeks after suffering from severe preeclampsia.
"The wires were awful," she remembers. "They fell off constantly when I shifted positions or he kicked a leg, which meant the monitors would alarm. It felt like an intrusion into the quiet little world I was trying to mentally create for us."
Over the last few years, researchers have begun to dive deeper into the literal and metaphorical challenges of wired monitoring.
For many parents, the wires prompt anxiety that worsens an already tense and vulnerable time.
I'll never forget the first time I got to hold my son without wires. It was the first time that motherhood felt manageable.
"Seeing my five-pound-babies covered in wires from head to toe rendered me completely overwhelmed," recalls Caila Smith, a mom of five from Indiana, whose NICU experience began when her twins were born pre-term. "The nurses seemed to handle them perfectly, but I was scared to touch them while they appeared so medically frail."
During the nine days it took for both twins to come home, the limited access she had to her babies started to impact her mental health. "If we would've had wireless sensors and monitors, it would've given us a much greater sense of freedom and confidence when snuggling our newborns," Smith says.
Besides enabling more natural interactions, wireless monitoring would make basic caregiving tasks much easier, like putting on a onesie.
"One thing I noticed is that many preemie outfits are made with zippers," points out Giles, "which just don't work well when your baby has wires coming off of them, head to toe."
Wired systems can pose issues for medical staff as well as parents.
"The main concern regarding wired systems is that they restrict access to the baby and often get tangled with other equipment, like IV lines," says Lamia Soghier, Medical Director of the Neonatal Intensive Care Unit at Children's National in Washington, D.C , who was also a NICU parent herself. "The nurses have to untangle the wires, which takes time, before handing the baby to the family."
I'll never forget the first time I got to hold my son without wires. It was the first time that motherhood felt manageable, and I couldn't stop myself from crying. Suddenly, anything felt possible and all the limitations from that first week of life seemed to fade away. The rise of wired-free monitoring will make some of the stressors that accompany NICU stays a thing of the past.
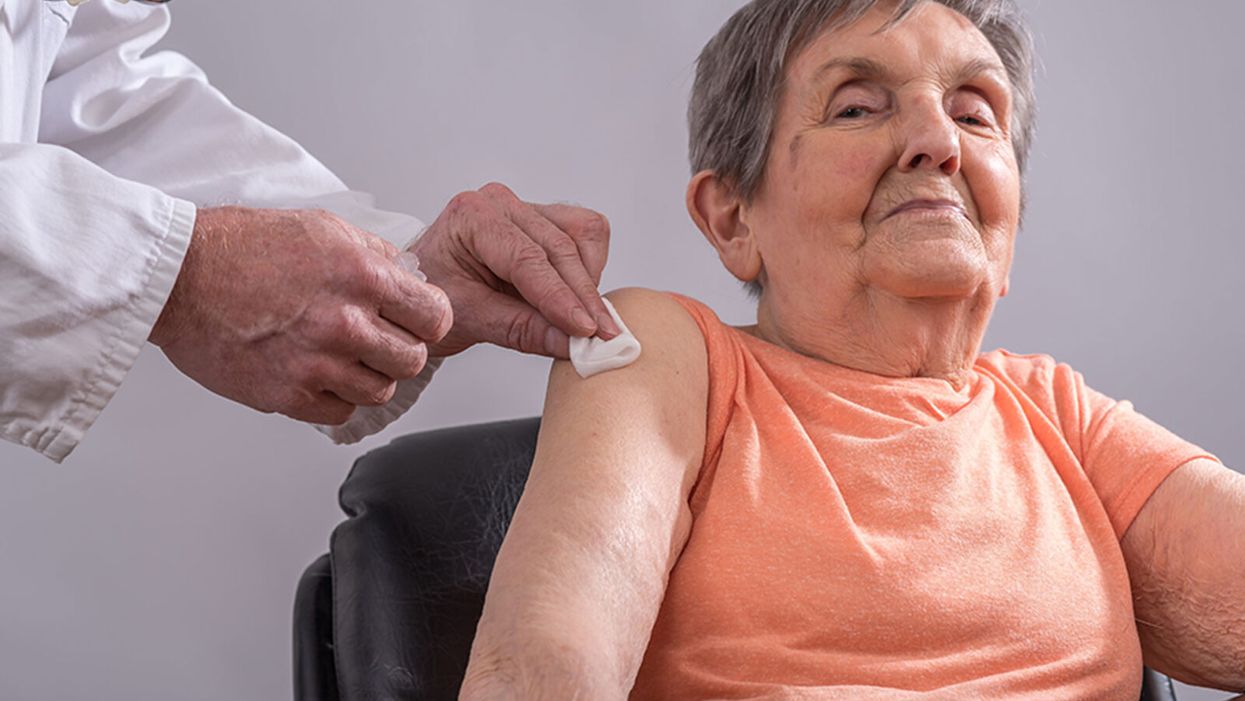
Drugs That Trick Older People’s Bodies to Behave Younger Might Boost the Effectiveness of a COVID-19 Vaccine
Because vaccination may be less effective in older people, it is imperative to test now whether immune boosters could help the efficacy of a COVID-19 vaccine in the elderly.
In our April 23rd editorial for this magazine, we argued that addressing the COVID-19 pandemic requires that we both fight the SARS-CoV-2 virus and fortify the human hosts who are most vulnerable to it.
Two recent phase 2 studies in older adults have suggested that a new category of drugs called rapalogues can in some cases increase the immunization capacity of older adults.
Because people over 70 account for more than 80 percent of reported COVID-19 deaths globally, this means we must do everything possible to protect our elders.
A range of recent studies have suggested that systemic knobs might metaphorically be turned to slow the cellular aging process, making us better able to fight off the many diseases correlated with aging. These types of systemic changes might be used to stem the specific decline in immunity caused by aging and to increases the biological capacity of elderly people to effectively fight viral infection.
But while helping make older people more resilient in the face of a viral infection is critical, that's not the only way geroscience can help in our fight against this deadly pandemic.
As we move toward hopefully developing one or more COVID-19 vaccines, researchers must more fully appreciate the ways in which traditional vaccines can be less effective in older people than in younger ones.
Repeated studies have shown that the flu vaccine, for example, has lower efficacy in older people than in younger ones. Older people tend to develop fewer antibodies after being vaccinated because a subset of their white blood cells, called T cells, have become less responsive over time. Some inflammatory peptides that increase with aging are also preventing the action of those T cells.
This is why there's a distinct possibility that a future COVD-19 vaccine, particularly one utilizing the traditional attenuated virus approach, could be less effective in older people than in younger ones.
Given the extreme urgency of developing vaccines that work well for everyone, we need to make sure that researchers are exploring all of the ways our elders can be best protected. While generating a vaccine that works equally well for people of all ages would be ideal, we can't count on that.
One way to bridge this gap might be to trick the bodies of older people into behaving as if they are younger just at the moment what a vaccine is delivered by giving them pre-immunization boosters.
Two recent phase 2 studies in older adults have suggested that a new category of drugs called rapalogues can in some cases increase the immunization capacity of older adults. Use of the drug for a short time period before flu shot immunization increased the antibody production for the flu and resulted in a 52 percent decrease in the occurrence of severe diseases needing medical help or hospitalization. This short-term pre-immunization intervention can also decrease the severity of serious respiratory tract infections, the deadliest manifestations of COVID-19, by similar magnitude. These patients also had almost half the incidence of the non-COVID-19 coronaviruses associated with the common cold.
The fact that those people were protected by treatment before hospitalization suggests metformin may have a role in boosting the vaccination of older people.
An inexpensive generic drug called metformin similarly targets the decline in immunity and inflammation (and extends health span and lifespan) in animals and has been used for decades to protect against the flu. A recent paper from a hospital in Wuhan, China showed that mortality of elderly COVID-19 diabetic patients on metformin was 25 percent less than that of patients with diabetes but not on metformin.
Another study from the U.S. showed that COVID-19 patients on metformin had a 20 percent decrease in mortality and lower inflammation. The fact that those people were protected by treatment before hospitalization suggests metformin may have a role in boosting the vaccination of older people.
We don't yet know whether rapalogues or metformin could be used as COVID-19 immunization boosters, not least because we don't have those vaccines. But we can and should make sure that all vaccine trials including older subjects also consider offering a subset of those subjects appropriate doses of rapalogues or metformin to explore whether doing so can boost the efficacy of a given vaccine.
If we weren't in the middle of the worst pandemic in a century, we would have more time to test our vaccines slowly and sequentially. In the context of the current crisis, however, testing whether immunization boosters might increase the efficacy of potential COVID-19 vaccines for older adults is at the very least a hypothesis worth exploring.
How We Can Return to Normal Life in the COVID-19 Era
A crowded baseball stadium is the epitome of "getting back to normal."
I was asked recently when life might return to normal. The question is simple but the answer is complex, with many knowns, lots of known unknowns, and some unknown unknowns. But I'll give it my best shot.
To get the fatality rate down to flu-like levels would require that we cut Covid-19 fatalities down by a factor of 5.
Since I'm human (and thus want my life back), I might be biased toward optimism.
Here's one way to think about it: Is there another infection that causes sickness and death at levels that we tolerate? The answer, of course, is 'yes': influenza.
According to the Centers for Disease Control, from 2010 to 2019, an average of 30 million Americans had the flu each year, leading to an annual average of 37,000 deaths. This works out to an infection-fatality rate, or IFR, of 0.12 percent. We've tolerated that level of illness death from influenza for a century.
Before going on, let's get one thing out of the way: Back in March, Covid-19 wasn't, as some maintained, "like the flu," and it still isn't. Since then, the U.S. has had 3.9 million confirmed Covid-19 cases and 140,000 deaths, for an IFR of 3.6 percent. Taking all the cases — including asymptomatic patients and those with minimal symptoms who were never tested for Covid-19 — into account, the real IFR is probably 0.6 percent, or roughly 5 times that of the flu.
Nonetheless, even a partly effective vaccine, combined with moderately effective medications, could bring Covid-19 numbers down to a tolerable, flu-like, threshold. It's a goal that seems within our reach.
Chronic mask-wearing and physical distancing are not my idea of normal, nor, I would venture to guess, would most other Americans consider these desirable states in which to live. We need both now to achieve some semblance of normalcy, but they're decidedly not normal life. My notion of normal: daily life with no or minimal mask wearing, open restaurants and bars, ballparks with fans, and theaters with audiences.
My projection for when we might get there: perhaps a year from now.
To get the fatality rate down to flu-like levels would require that we cut Covid-19 fatalities down by a factor of 5, via some combination of fewer symptomatic cases and a lower chance that a symptomatic patient will go on to die. How might that happen?
First, we have to make some impact on young people – getting them to follow the public health directives at higher rates than they are currently. The main reason we need to push younger people to stay safe is that they can spread Covid-19 to vulnerable people (those who are older, with underlying health problems). But, once the most vulnerable are protected (through the deployment of some combination of effective medications and a vaccine), the fact that some young people aren't acting safely – or maybe won't take a vaccine themselves – wouldn't cause so much concern. The key is whether the people at highest risk for bad outcomes are protected.
Then there's the vaccine. The first principle: We don't need a 100 percent-effective vaccine injected into 320 million deltoid muscles (in the U.S. alone). Thank God, since it's fanciful to believe that we can have a vaccine that's 100 percent effective, universally available by next summer, and that each and every American agrees to be vaccinated.
How are we doing in our vaccine journey? We've been having some banner days lately, with recent optimistic reports from several of the vaccine companies. In one report, the leading candidate vaccine, the one effort being led by Oxford University, led to both antibodies and a cellular immune response, a very helpful belt-and-suspenders approach that increases the probability of long-lasting immunity. This good news comes on the heels of the positive news regarding the American vaccine being made by Moderna earlier in July.
While every article about vaccines sounds the obligatory cautionary notes, to date we've checked every box on the path to a safe and effective vaccine. We might not get there, but most experts are now predicting an FDA-approvable vaccine (more than 50 percent effective with no show-stopping side effects) by early 2021.
It is true that we don't know how long immunity will last, but that can be a problem to solve later. In this area, time is our friend. If we can get to an effective vaccine that lasts for a year or two, over time we should be able to discover strategies (more vaccine boosters, new and better medications) to address the possibility of waning immunity.
All things considered, I'm going to put my nickel down on the following optimistic scenario: we'll have one, and likely several, vaccines that have been proven to be more than 50 percent effective and safe by January, 2021.
If only that were the finish line.
Once we vaccinate a large fraction of high-risk patients, having a moderate number of unvaccinated people running around won't pose as much threat.
The investments in manufacturing and distribution should pay off, but it's still inconceivable that we'll be able to get vaccines to 300 million people in three to six months. For the 2009 Swine Flu, we managed to vaccinate about 1 in 4 Americans over six months.
So we'll need to prioritize. First in line will likely be the 55 million Americans over 65, and the six to eight million patient-facing healthcare workers. (How to sort priorities among people under 65 with "chronic diseases" will be a toughie.) Vaccinating 80-100 million vulnerable people, plus clinicians, might be achievable by mid-21.
If we can protect vulnerable people with an effective vaccine (with the less vulnerable waiting their turn over a subsequent 6-12 month period), that may be enough to do the trick. (Of course, vulnerable people may also be least likely to develop immunity in response to a vaccine. That could be an Achilles' heel – time will tell.)
Why might that be enough? Once we vaccinate a large fraction of high-risk patients, having a moderate number of unvaccinated people running around won't pose as much threat. Since they're at lower risk, they have a lower chance of getting sick and dying than those who received the vaccine first.
We're likely to have better meds by then, too. Since March, we've discovered two moderately effective medications for Covid-19 — remdesivir and dexamethasone. It seems likely that we'll find others by next summer, perhaps even a treatment that prevents patients from getting ill in the first place. There are many such therapies, ranging from zinc to convalescent plasma, currently being studied.
Moreover, we know that hospitals that are not overrun with Covid-19 have lower mortality rates. If we've gotten a fairly effective vaccine into most high-risk people, the hospitals are unlikely to be overwhelmed – another factor that may help lower the mortality rate to flu-like levels.
All of these factors – vaccination of most vulnerable people, one or two additional effective medications, hospitals and ICU's that aren't overwhelmed – could easily combine to bring the toll of Covid-19 down to something that resembles that of the flu. Then, we should be able to return to normal life.
Whatever the reason, if enough people refuse the vaccine, all bets are off.
What do I worry about? There's the growing anti-vaxxer movement, for one. On top of that, it seems that many Americans worry that a vaccine discovered in record speed won't be safe, or that the FDA approval process will have been corrupted by political influences. Whatever the reason, if enough people refuse the vaccine, all bets are off.
Assuming only high-risk people do get vaccinated, there will still be cases of Covid-19, maybe even mini-outbreaks, well into 2021 and likely 2022. Obviously, that's not ideal, and we should hope for a vaccine that results in the complete eradication of Covid-19. But the point is that, even with flu-like levels of illness and death, we should still be able to achieve "normal."
Hope is not a strategy, as the saying goes. But it is hope, which is more than we've had for a while.