Why you should (virtually) care

Virtual-first care, or V1C, could increase the quality of healthcare and make it more patient-centric by letting patients combine in-person visits with virtual options such as video for seeing their care providers.
As the pandemic turns endemic, healthcare providers have been eagerly urging patients to return to their offices to enjoy the benefits of in-person care.
But wait.
The last two years have forced all sorts of organizations to be nimble, adaptable and creative in how they work, and this includes healthcare providers’ efforts to maintain continuity of care under the most challenging of conditions. So before we go back to “business as usual,” don’t we owe it to those providers and ourselves to admit that business as usual did not work for most of the people the industry exists to help? If we’re going to embrace yet another period of change – periods that don’t happen often in our complex industry – shouldn’t we first stop and ask ourselves what we’re trying to achieve?
Certainly, COVID has shown that telehealth can be an invaluable tool, particularly for patients in rural and underserved communities that lack access to specialty care. It’s also become clear that many – though not all – healthcare encounters can be effectively conducted from afar. That said, the telehealth tactics that filled the gap during the pandemic were largely stitched together substitutes for existing visit-based workflows: with offices closed, patients scheduled video visits for help managing the side effects of their blood pressure medications or to see their endocrinologist for a quarterly check-in. Anyone whose children slogged through the last year or two of remote learning can tell you that simply virtualizing existing processes doesn’t necessarily improve the experience or the outcomes!
But what if our approach to post-pandemic healthcare came from a patient-driven perspective? We have a fleeting opportunity to advance a care model centered on convenient and equitable access that first prioritizes good outcomes, then selects approaches to care – and locations – tailored to each patient. Using the example of education, imagine how effective it would be if each student, regardless of their school district and aptitude, received such individualized attention.
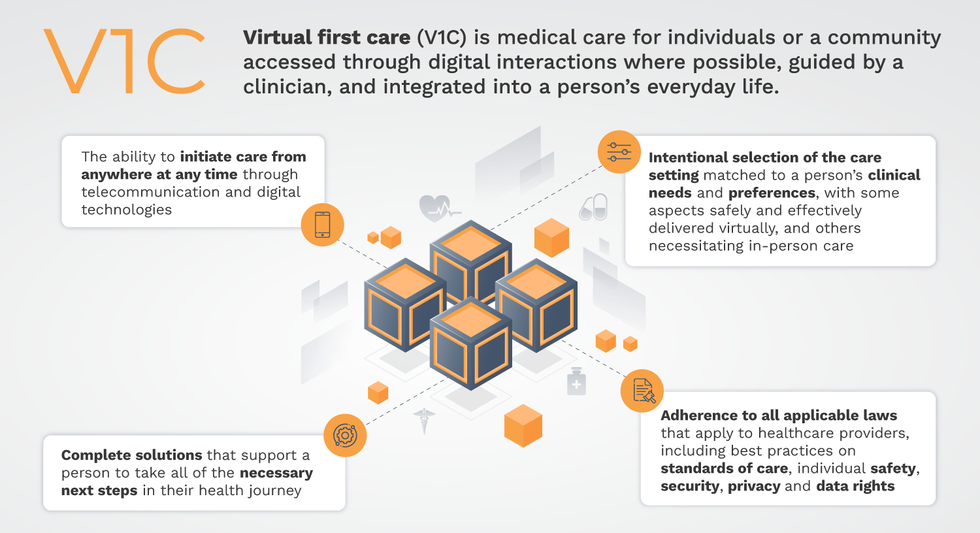
That’s the idea behind virtual-first care (V1C), a new care model centered on convenient, customized, high-quality care that integrates a full suite of services tailored directly to patients’ clinical needs and preferences. This package includes asynchronous communication such as texting; video and other live virtual modes; and in-person options.
V1C goes beyond what you might think of as standard “telehealth” by using evidence-based protocols and tools that include traditional and digital therapeutics and testing, personalized care plans, dynamic patient monitoring, and team-based approaches to care. This could include spit kits mailed for laboratory tests and complementing clinical care with health coaching. V1C also replaces some in-person exams with ongoing monitoring, using sensors for more ‘whole person’ care.
Amidst all this momentum, we have the opportunity to rethink the goals of healthcare innovation, but that means bringing together key stakeholders to demonstrate that sustainable V1C can redefine healthcare.
Established V1C healthcare providers such as Omada, Headspace, and Heartbeat Health, as well as emerging market entrants like Oshi, Visana, and Wellinks, work with a variety of patients who have complicated long-term conditions such as diabetes, heart failure, gastrointestinal illness, endometriosis, and COPD. V1C is comprehensive in ways that are lacking in digital health and its other predecessors: it has the potential to integrate multiple data streams, incorporate more frequent touches and check-ins over time, and manage a much wider range of chronic health conditions, improving lives and reducing disease burden now and in the future.
Recognizing the pandemic-driven interest in virtual care, significant energy and resources are already flowing fast toward V1C. Some of the world’s largest innovators jumped into V1C early on: Verily, Alphabet’s Life Sciences Company, launched Onduo in 2016 to disrupt the diabetes healthcare market, and is now well positioned to scale its solutions. Major insurers like Aetna and United now offer virtual-first plans to members, responding as organizations expand virtual options for employees. Amidst all this momentum, we have the opportunity to rethink the goals of healthcare innovation, but that means bringing together key stakeholders to demonstrate that sustainable V1C can redefine healthcare.
That was the immediate impetus for IMPACT, a consortium of V1C companies, investors, payers and patients founded last year to ensure access to high-quality, evidence-based V1C. Developed by our team at the Digital Medicine Society (DiMe) in collaboration with the American Telemedicine Association (ATA), IMPACT has begun to explore key issues that include giving patients more integrated experiences when accessing both virtual and brick-and-mortar care.
Digital Medicine Society
V1C is not, nor should it be, virtual-only care. In this new era of hybrid healthcare, success will be defined by how well providers help patients navigate the transitions. How do we smoothly hand a patient off from an onsite primary care physician to, say, a virtual cardiologist? How do we get information from a brick-and-mortar to a digital portal? How do you manage dataflow while still staying HIPAA compliant? There are many complex regulatory implications for these new models, as well as an evolving landscape in terms of privacy, security and interoperability. It will be no small task for groups like IMPACT to determine the best path forward.
None of these factors matter unless the industry can recruit and retain clinicians. Our field is facing an unprecedented workforce crisis. Traditional healthcare is making clinicians miserable, and COVID has only accelerated the trend of overworked, disenchanted healthcare workers leaving in droves. Clinicians want more interactions with patients, and fewer with computer screens – call it “More face time, less FaceTime.” No new model will succeed unless the industry can more efficiently deploy its talent – arguably its most scarce and precious resource. V1C can help with alleviating the increasing burden and frustration borne by individual physicians in today’s status quo.
In healthcare, new technological approaches inevitably provoke no shortage of skepticism. Past lessons from Silicon Valley-driven fixes have led to understandable cynicism. But V1C is a different breed of animal. By building healthcare around the patient, not the clinic, V1C can make healthcare work better for patients, payers and providers. We’re at a fork in the road: we can revert back to a broken sick-care system, or dig in and do the hard work of figuring out how this future-forward healthcare system gets financed, organized and executed. As a field, we must find the courage and summon the energy to embrace this moment, and make it a moment of change.
Fast for Longevity, with Less Hunger, with Dr. Valter Longo
Valter Longo, a biogerontologist at USC, and centenarian Rocco Longo (no relation) appear together in Italy in 2021. The elder Longo is from a part of Italy where people have fasted regularly and are enjoying long lifespans.
You’ve probably heard about intermittent fasting, where you don’t eat for about 16 hours each day and limit the window where you’re taking in food to the remaining eight hours.
But there’s another type of fasting, called a fasting-mimicking diet, with studies pointing to important benefits. For today’s podcast episode, I chatted with Dr. Valter Longo, a biogerontologist at the University of Southern California, about all kinds of fasting, and particularly the fasting-mimicking diet, which minimizes hunger as much as possible. Going without food for a period of time is an example of good stress: challenges that work at the cellular level to boost health and longevity.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
If you’ve ever spent more than a few minutes looking into fasting, you’ve almost certainly come upon Dr. Longo's name. He is the author of the bestselling book, The Longevity Diet, and the best known researcher of fasting-mimicking diets.
With intermittent fasting, your body might begin to switch up its fuel type. It's usually running on carbs you get from food, which gets turned into glucose, but without food, your liver starts making something called ketones, which are molecules that may benefit the body in a number of ways.
With the fasting-mimicking diet, you go for several days eating only types of food that, in a way, keep themselves secret from your body. So at the level of your cells, the body still thinks that it’s fasting. This is the best of both worlds – you’re not completely starving because you do take in some food, and you’re getting the boosts to health that come with letting a fast run longer than intermittent fasting. In this episode, Dr. Longo talks about the growing number of studies showing why this could be very advantageous for health, as long as you undertake the diet no more than a few times per year.
Dr. Longo is the director of the Longevity Institute at USC’s Leonard Davis School of Gerontology, and the director of the Longevity and Cancer program at the IFOM Institute of Molecular Oncology in Milan. In addition, he's the founder and president of the Create Cures Foundation in L.A., which focuses on nutrition for the prevention and treatment of major chronic illnesses. In 2016, he received the Glenn Award for Research on Aging for the discovery of genes and dietary interventions that regulate aging and prevent diseases. Dr. Longo received his PhD in biochemistry from UCLA and completed his postdoc in the neurobiology of aging and Alzheimer’s at USC.
Show links:
Create Cures Foundation, founded by Dr. Longo: www.createcures.org
Dr. Longo's Facebook: https://www.facebook.com/profvalterlongo/
Dr. Longo's Instagram: https://www.instagram.com/prof_valterlongo/
Dr. Longo's book: The Longevity Diet
The USC Longevity Institute: https://gero.usc.edu/longevity-institute/
Dr. Longo's research on nutrition, longevity and disease: https://pubmed.ncbi.nlm.nih.gov/35487190/
Dr. Longo's research on fasting mimicking diet and cancer: https://pubmed.ncbi.nlm.nih.gov/34707136/
Full list of Dr. Longo's studies: https://pubmed.ncbi.nlm.nih.gov/?term=Longo%2C+Valter%5BAuthor%5D&sort=date
Research on MCT oil and Alzheimer's: https://alz-journals.onlinelibrary.wiley.com/doi/f...
Keto Mojo device for measuring ketones
Silkworms with spider DNA spin silk stronger than Kevlar
Silkworm silk is fragile, which limits its uses, but a few extra genes can help.
Story by Freethink
The study and copying of nature’s models, systems, or elements to address complex human challenges is known as “biomimetics.” Five hundred years ago, an elderly Italian polymath spent months looking at the soaring flight of birds. The result was Leonardo da Vinci’s biomimetic Codex on the Flight of Birds, one of the foundational texts in the science of aerodynamics. It’s the science that elevated the Wright Brothers and has yet to peak.
Today, biomimetics is everywhere. Shark-inspired swimming trunks, gecko-inspired adhesives, and lotus-inspired water-repellents are all taken from observing the natural world. After millions of years of evolution, nature has quite a few tricks up its sleeve. They are tricks we can learn from. And now, thanks to some spider DNA and clever genetic engineering, we have another one to add to the list.
The elusive spider silk
We’ve known for a long time that spider silk is remarkable, in ways that synthetic fibers can’t emulate. Nylon is incredibly strong (it can support a lot of force), and Kevlar is incredibly tough (it can absorb a lot of force). But neither is both strong and tough. In all artificial polymeric fibers, strength and toughness are mutually exclusive, and so we pick the material best for the job and make do.
Spider silk, a natural polymeric fiber, breaks this rule. It is somehow both strong and tough. No surprise, then, that spider silk is a source of much study.The problem, though, is that spiders are incredibly hard to cultivate — let alone farm. If you put them together, they will attack and kill each other until only one or a few survive. If you put 100 spiders in an enclosed space, they will go about an aggressive, arachnocidal Hunger Games. You need to give each its own space and boundaries, and a spider hotel is hard and costly. Silkworms, on the other hand, are peaceful and productive. They’ll hang around all day to make the silk that has been used in textiles for centuries. But silkworm silk is fragile. It has very limited use.
The elusive – and lucrative – trick, then, would be to genetically engineer a silkworm to produce spider-quality silk. So far, efforts have been fruitless. That is, until now.
We can have silkworms creating silk six times as tough as Kevlar and ten times as strong as nylon.
Spider-silkworms
Junpeng Mi and his colleagues working at Donghua University, China, used CRISPR gene-editing technology to recode the silk-creating properties of a silkworm. First, they took genes from Araneus ventricosus, an East Asian orb-weaving spider known for its strong silk. Then they placed these complex genes – genes that involve more than 100 amino acids – into silkworm egg cells. (This description fails to capture how time-consuming, technical, and laborious this was; it’s a procedure that requires hundreds of thousands of microinjections.)
This had all been done before, and this had failed before. Where Mi and his team succeeded was using a concept called “localization.” Localization involves narrowing in on a very specific location in a genome. For this experiment, the team from Donghua University developed a “minimal basic structure model” of silkworm silk, which guided the genetic modifications. They wanted to make sure they had the exactly right transgenic spider silk proteins. Mi said that combining localization with this basic structure model “represents a significant departure from previous research.” And, judging only from the results, he might be right. Their “fibers exhibited impressive tensile strength (1,299 MPa) and toughness (319 MJ/m3), surpassing Kevlar’s toughness 6-fold.”
A world of super-materials
Mi’s research represents the bursting of a barrier. It opens up hugely important avenues for future biomimetic materials. As Mi puts it, “This groundbreaking achievement effectively resolves the scientific, technical, and engineering challenges that have hindered the commercialization of spider silk, positioning it as a viable alternative to commercially synthesized fibers like nylon and contributing to the advancement of ecological civilization.”
Around 60 percent of our clothing is made from synthetic fibers like nylon, polyester, and acrylic. These plastics are useful, but often bad for the environment. They shed into our waterways and sometimes damage wildlife. The production of these fibers is a source of greenhouse gas emissions. Now, we have a “sustainable, eco-friendly high-strength and ultra-tough alternative.” We can have silkworms creating silk six times as tough as Kevlar and ten times as strong as nylon.
We shouldn’t get carried away. This isn’t going to transform the textiles industry overnight. Gene-edited silkworms are still only going to produce a comparatively small amount of silk – even if farmed in the millions. But, as Mi himself concedes, this is only the beginning. If Mi’s localization and structure-model techniques are as remarkable as they seem, then this opens up the door to a great many supermaterials.
Nature continues to inspire. We had the bird, the gecko, and the shark. Now we have the spider-silkworm. What new secrets will we unravel in the future? And in what exciting ways will it change the world?
This article originally appeared on Freethink, home of the brightest minds and biggest ideas of all time.


