When doctors couldn’t stop her daughter’s seizures, this mom earned a PhD and found a treatment herself.

Savannah Salazar (left) and her mother, Tracy Dixon-Salazaar, who earned a PhD in neurobiology in the quest for a treatment of her daughter's seizure disorder.
Twenty-eight years ago, Tracy Dixon-Salazaar woke to the sound of her daughter, two-year-old Savannah, in the midst of a medical emergency.
“I entered [Savannah’s room] to see her tiny little body jerking about violently in her bed,” Tracy said in an interview. “I thought she was choking.” When she and her husband frantically called 911, the paramedic told them it was likely that Savannah had had a seizure—a term neither Tracy nor her husband had ever heard before.
Over the next several years, Savannah’s seizures continued and worsened. By age five Savannah was having seizures dozens of times each day, and her parents noticed significant developmental delays. Savannah was unable to use the restroom and functioned more like a toddler than a five-year-old.
Doctors were mystified: Tracy and her husband had no family history of seizures, and there was no event—such as an injury or infection—that could have caused them. Doctors were also confused as to why Savannah’s seizures were happening so frequently despite trying different seizure medications.
Doctors eventually diagnosed Savannah with Lennox-Gaustaut Syndrome, or LGS, an epilepsy disorder with no cure and a poor prognosis. People with LGS are often resistant to several kinds of anti-seizure medications, and often suffer from developmental delays and behavioral problems. People with LGS also have a higher chance of injury as well as a higher chance of sudden unexpected death (SUDEP) due to the frequent seizures. In about 70 percent of cases, LGS has an identifiable cause such as a brain injury or genetic syndrome. In about 30 percent of cases, however, the cause is unknown.
Watching her daughter struggle through repeated seizures was devastating to Tracy and the rest of the family.
“This disease, it comes into your life. It’s uninvited. It’s unannounced and it takes over every aspect of your daily life,” said Tracy in an interview with Today.com. “Plus it’s attacking the thing that is most precious to you—your kid.”
Desperate to find some answers, Tracy began combing the medical literature for information about epilepsy and LGS. She enrolled in college courses to better understand the papers she was reading.
“Ironically, I thought I needed to go to college to take English classes to understand these papers—but soon learned it wasn’t English classes I needed, It was science,” Tracy said. When she took her first college science course, Tracy says, she “fell in love with the subject.”
Tracy was now a caregiver to Savannah, who continued to have hundreds of seizures a month, as well as a full-time student, studying late into the night and while her kids were at school, using classwork as “an outlet for the pain.”
“I couldn’t help my daughter,” Tracy said. “Studying was something I could do.”
Twelve years later, Tracy had earned a PhD in neurobiology.
After her post-doctoral training, Tracy started working at a lab that explored the genetics of epilepsy. Savannah’s doctors hadn’t found a genetic cause for her seizures, so Tracy decided to sequence her genome again to check for other abnormalities—and what she found was life-changing.
Tracy discovered that Savannah had a calcium channel mutation, meaning that too much calcium was passing through Savannah’s neural pathways, leading to seizures. The information made sense to Tracy: Anti-seizure medications often leech calcium from a person’s bones. When doctors had prescribed Savannah calcium supplements in the past to counteract these effects, her seizures had gotten worse every time she took the medication. Tracy took her discovery to Savannah’s doctor, who agreed to prescribe her a calcium blocker.
The change in Savannah was almost immediate.
Within two weeks, Savannah’s seizures had decreased by 95 percent. Once on a daily seven-drug regimen, she was soon weaned to just four, and then three. Amazingly, Tracy started to notice changes in Savannah’s personality and development, too.
“She just exploded in her personality and her talking and her walking and her potty training and oh my gosh she is just so sassy,” Tracy said in an interview.
Since starting the calcium blocker eleven years ago, Savannah has continued to make enormous strides. Though still unable to read or write, Savannah enjoys puzzles and social media. She’s “obsessed” with boys, says Tracy. And while Tracy suspects she’ll never be able to live independently, she and her daughter can now share more “normal” moments—something she never anticipated at the start of Savannah’s journey with LGS. While preparing for an event, Savannah helped Tracy get ready.
“We picked out a dress and it was the first time in our lives that we did something normal as a mother and a daughter,” she said. “It was pretty cool.”
Could Biologically Enhancing Our Morality Save Our Species?
A human head pictured with a red heart in the place of a brain.
As a species, we are prone to weaponizing. There is a famous anecdote from Wulf Schievenhovel, a German anthropologist who was working in the highlands of New Guinea studying a local tribe. One day, he offered two tribesmen a flight in an airplane. They duly accepted but showed up with two large stones. When he asked why, they told him that they wanted to drop them on a neighboring village. Ethologist Frans de Waal later remarked on this story that Schievenhovel had effectively "witnessed the invention of the bomb."
Today you don't have to be Putin or Kim Jong Un to pose an existential threat.
Modern technology has given us access to more than just rocks. In 2011, a Swedish man was arrested after attempting a nuclear fission in his kitchen. And in the inaugural issue of this magazine, my colleague Hank Greely raised a terrifying prospect:
"do-it-yourself hobbyists can use CRISPR [gene editing]… to change the genomes of whole species of living things – domestic or wild; animal, vegetable, or microbial – cheaply, easily, and before we even know it is happening."
In science fiction, it is typically governments that take over technologies and use them for evil. That risk is of course no fiction. It is an ongoing problem that we have addressed through institutions: democracies, constitutions, legal systems and international treaties, and groups working together as checks and balances. It isn't perfect, but it has worked (so far).
Today you don't have to be Putin or Kim Jong Un to pose an existential threat. We are rapidly acquiring the technological ability for individuals and groups not just to cause major harm, but to do so exactly as Hank said: "cheaply, easily, and before we even know it is happening."
How should we address this problem? Together with Ingmar Persson, a fellow philosophy professor at Gothenburg, Sweden, I have argued that while education, institutions and good policing are important, we may need to think more radically.
We could adapt our biology so that we can appreciate the suffering of foreign or future people in the same instinctive way we do our friends and neighbors.
We evolved, along with the New Guinea tribesmen, to care about our small group and to be suspicious of outsiders. We evolved to cooperate well within our group, at a size where we could keep an eye on free riders. And we evolved to have the ability, and occasionally the desire to harm others, but with a natural limit on the amount of harm we could do—at least before others could step in to prevent, punish or kill us.
Our limitations have also become apparent in another form of existential threat: resource depletion. Despite our best efforts at educating, nudging, and legislating on climate change, carbon dioxide emissions in 2017 are expected to come in at the highest ever following a predicted rise of 2 percent. Why? We aren't good at cooperating in larger groups where freeriding is not easily spotted. We also deal with problems in order of urgency. A problem close by is much more significant to us than a problem in the future. That's why even if we accept there is a choice between economic recession now or natural disasters and potential famine in the future, we choose to carry on drilling for oil. And if the disasters and famine are present day, but geographically distant, we still choose to carry on drilling.
So what is our radical solution? We propose that there is a need for what we call moral bioenhancement. That is, for seeking a biological intervention that can help us overcome our evolved moral limitations. For example, adapting our biology so that we can appreciate the suffering of foreign or future people in the same instinctive way we do our friends and neighbors. Or, in the case of individuals, in addressing the problem of psychopathy from a biological perspective.
There is no reason in principle why humans could not be genetically modified...to make them kinder, happier, more conscientious, altruistic and just.
We have been dramatically successful at modifying various moral characteristics of non-human animals. Over ten thousand years or so, we have turned wolves into dogs by selective breeding, and those dogs into breeds with behavioural as well as physical characteristics: certain breeds can be faithful, hard working, good tempered and intelligent (or the opposite). Scientists have manipulated the expression of genes in prairie voles to cause them to form a mate bond more quickly, and in monkeys to make them work harder. There is no reason in principle why humans could not be genetically modified using gene editing, or their brains modified in other ways, to make them kinder, happier, more conscientious, altruistic and just.
One objection is that this is a pipe dream: even if it is acceptable to do this, it is so unlikely to be achievable, it is not worth pursuing. However, research has shown that we are already morally modified. This is widely accepted when it comes to negative effects. For example, we all know that alcohol can lead people to aggressive or other destructive behaviours that they would not have countenanced sober. In a 2008 case, a retired UK teacher was cleared of child pornography charges after he successfully argued his behaviour was caused by a drug prescribed for his Parkinson's disease. There is also evidence that we can be morally modified in a more positive direction. For example, SSRIs like Prozac, a class of drugs widely used to treat depression, have been shown to act on healthy volunteers to make them more cooperative and less critical.
Another objection is that we need the negative aspects of our human character. We need people who can fight wars. We need to be able to blot out the suffering of the wider world: to experience it as we would if it applied to our nearest and dearest would be unbearable. This might be so. If aggressiveness and denial, or strong bonding to small communities, are important traits, it is important that we understand how, and to what degree, they should be controlled. It is unlikely that nature has dished out exactly the right levels of all morally relevant characteristics on an individual or population level. We don't claim to have all the answers to what characteristics we need to enhance, and what characteristics we need to diminish. But we see no reason to believe that the status quo is the optimum.
We haven't argued that we should go blindly in now with half-baked moral enhancers, or that we should forget about moral education, or legal solutions. Evolution has a built-in response to existential threats through adaptation. But adaptation takes generations and can't deal with threats that take out a whole population. Some threats are too important —and too urgent—to be left to chance.
Deep Brain Stimulation for Mental Illnesses Raises Ethical Concerns
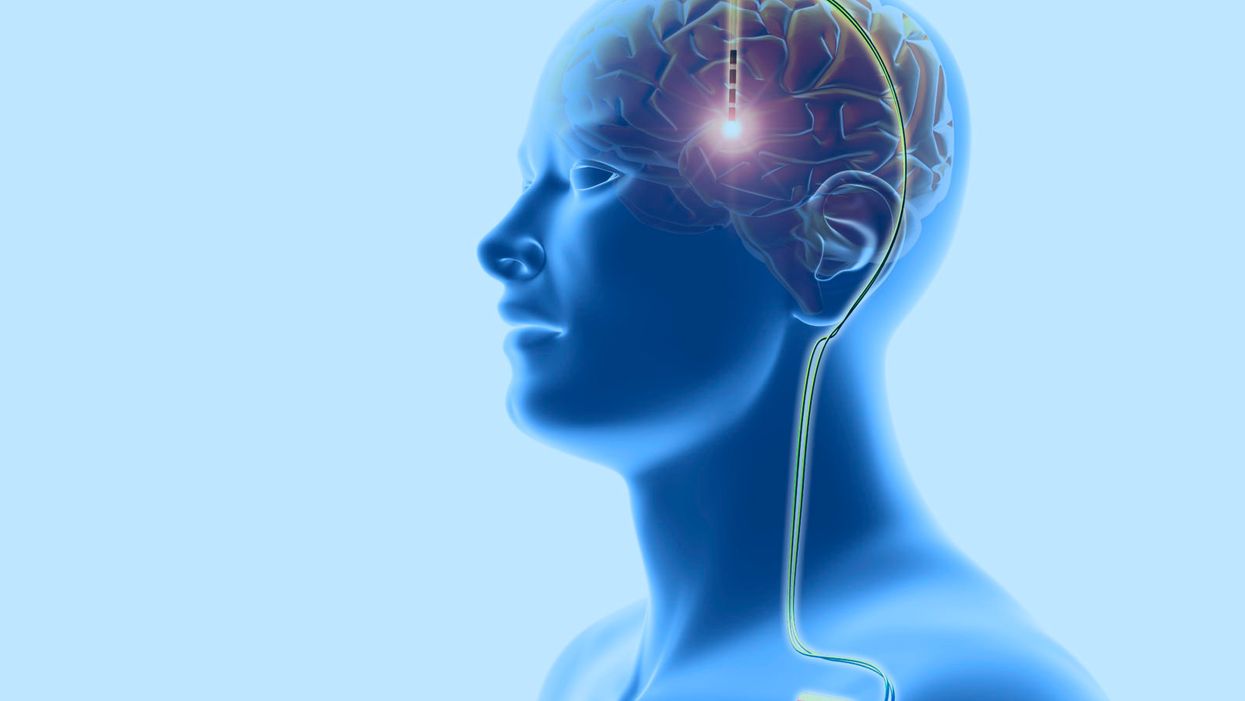
Deep brain stimulation: This neurosurgical treatment involves the implantation of electrodes in the cerebral lobes of the brain, linked through the scalp (top) to wires (down right) leading to a battery implanted below the skin. This sends electrical impulses to specific areas of the brain. DBS was developed for the treatment of Parkinson's disease, but is being investigated for use in other conditions.
Imagine that you are one of the hundreds of millions of people who suffer from depression. Medication hasn't helped you, so you're looking for another treatment option. Something powerful enough to change your mood as soon as you need a lift.
"If a participant experiences a personality change, does this change who they are or dehumanize them by altering their nature?"
Enter deep brain stimulation: a type of therapy in which one or more electrodes are inserted into your brain and connected to a surgically implanted, battery-operated medical device in your chest. This device, which is approximately the size of a stopwatch, sends electric pulses to a targeted region of your brain. The idea is to control a variety of neurological symptoms that can't be adequately managed by drugs.
Over the last twenty years, deep brain stimulation, known as DBS, has become an efficient and safe alternative for the treatment of chronic neurological diseases such as epilepsy, Parkinson's disease and neuropathic pain. According to the International Neuromodulation Society, there have been more than 80,000 deep brain stimulation implants performed around the world.
The Food and Drug Administration approved DBS as a treatment for essential tremor and Parkinson's in 1997, dystonia in 2003 and obsessive compulsive disorder in 2009. Since doctors can use drugs and treatments "off-label" (not approved by the FDA) to treat patients with any disease, DBS is now also being investigated as a treatment for chronic pain, PTSD and major depression.
And these new applications are raising profound ethical questions about individuality, personality, and even what it means to be human.
"These patients are essentially having a computer that can modify and influence emotional processing, mood and motor outputs inserted into the brain," said Gabriel Lazaro-Munoz, an assistant professor at The Center for Medical Ethics and Health Policy at Baylor College of Medicine. "These responses define us as human beings and dictate our autonomy. If a participant experiences a personality change, does this change who they are or dehumanize them by altering their nature? These are some of the questions we have to consider."
"When we are not in control of ourselves, are we ourselves?"
The U.S. government has similar concerns about DBS. The National Institutes of Health recently awarded grants to study the neuroethical issues surrounding the use of DBS in neuropsychiatric and movement disorders and appropriate consent for brain research. The grants are part of the Brain Research through Advancing Innovative Neurotechnologies (BRAIN) Initiative. Walter Koroshetz, director of NIH's National Institute of Neurological Disorders and Stroke said, "Neuroscience is rapidly moving toward a new frontier of research on human brains that may have long-lasting and unforeseen effects. These new awards signal our commitment to research conducted in a responsible way as to anticipate all potential consequences, and to ensure that research subjects have a clear understanding of the potential benefits and risks of participating in studies."
Dr. Lazaro-Munoz's Center was awarded one of the grants to identify and evaluate the ethical, legal and social concerns with adaptive deep brain stimulation (aDBS) technologies. Adaptive DBS is a relatively new version of the technology that enables recording of brain cell activity that is then used to regulate the brain in real time. He and his team will closely observe researchers conducting aDBS studies and administering in-depth interviews to trial participants, their caregivers, and researchers, as well as individuals who declined to participate in such studies. The goal is to gain a better understanding of the ethical concerns at stake in order to guide responsible research.
Dr. Lazaro-Munoz said one of the concerns is dehumanization. "By using this technology are we compromising what makes us human? When we are not in control of ourselves, are we ourselves?" He notes that similar concerns were raised about pharmaceutical treatments for illnesses. "Both change behaviors and emotional processing. However, there is a difference. Culturally we are more used to using drugs, not implanting devices into brain and computer interfaces. Many people think of it as science fiction."
The changes in behavior due to DBS can be dramatic, perhaps none more so than with Parkinson's disease; patients may see their chronic tremors suddenly vanish.
Pills for OCD and depression take longer than DBS to see significant improvement, sometimes months. "A DBS device is either on or off. And patients and families see changes immediately," Dr. Lazaro-Munoz said. "Family members are often startled by these changes, as are the patients." He's observed that patients feel more in control with pills because they can alter and "play" with the dose or even skip a dose.
The changes in behavior due to DBS can be dramatic, perhaps none more so than with Parkinson's disease; patients may see their chronic tremors suddenly vanish, like in this must-see video.
But surgical procedures to treat motor symptoms are also increasingly being implicated as a cause of behavioral changes, both positive and negative, in patients with Parkinson's. The personality changes reported in patients who undergo DBS include hypermania, pathological gambling, hypersexuality, impulsivity and aggressiveness. One patient who suffered from OCD fell in love with the music of Johnny Cash when his brain was stimulated. On the positive side, patients report memory enhancement.
One patient who is pleased with DBS is Greg Barstead, who was diagnosed with Parkinson's in 2003, when he was the president of Colonial Penn Life Insurance Company. He also has dystonia, which affects his neck and shoulders. Barstead said that DBS has been helpful for a range of symptoms: "My shoulder is a lot less stiff and my neck hurts less. And my tremors are under control. It is not perfect, as it doesn't relieve all the Parkinson's symptoms, but it does enough of a good job that both my wife and I are very happy I had DBS."
"We are not exactly sure what part of the brain causes depression. Doctors have not identified where to implant the device."
He said he hasn't noticed any personality changes, but noted that the disease itself can cause such changes. In fact, studies have shown that it can cause many psychiatric problems including depression and hallucinations. And, approximately a third of Parkinson's patients develop dementia.
Arthur L. Caplan, founding head of the Division of Medical Ethics at NYU School of Medicine, notes that unlike psychosurgery, DBS can be turned on and off and the device can be removed. "There are less ethical concerns around treating patients with Parkinson's disease than other illnesses because surgeons know exactly where to implant the device and have many years of experience with it," he said, adding that he is concerned about using DBS for other illnesses, such as depression. "We are not exactly sure what part of the brain causes depression. Doctors have not identified where to implant the device. And I would certainly not advocate its use in patients with mild depression."
Dr. Lazaro-Munoz said of the personality changes possible with DBS, physicians need to consider how the patients were functioning without it. "Patients who are candidates for DBS typically used many medications as well as psychotherapy before opting for DBS," he explained. "To me, the question is what is the net result of using this technology? Does the patient have regrets? Are the changes in personality significant or not? Although most DBS patients report being happy they underwent the procedure, some say they don't feel like themselves after DBS. Others feel they are more like themselves, especially if there are dramatic improvements in movement problems or relief of OCD symptoms."
And then there is the question of money. The costs of DBS are covered by most insurance companies and Medicare only for FDA-approved targets like Parkinson's. Off-label uses are not covered, at least for now.
Caplan reminds people that DBS devices are manufactured by companies that are interested in making money and the average cost per treatment is around $50,000. "I am interested in seeing DBS move forward," he said. "But we must be careful and not allow industry to make it go too fast, or be used on too many people, before we know it is effective."