Will COVID-19 Pave the Way For Home-Based Precision Medicine?

n artist rendering of a "smart toilet" that gathers biometric data to monitor a person's health in real time.
It looks like an ordinary toilet but it is anything but. The "smart toilet" is the diagnostic tool of the future, equipped with cameras that take snapshots of the users and their waste, motion sensors to analyze what's inside the urine and stool samples, and software that automatically sends data to a secure, cloud-based system that can be easily accessed by your family doctor.
"It's a way of doing community surveillance. If there is a second wave of infections in the future, we'll know right away."
Using urine "dipstick tests" similar to the home pregnancy strips, the smart toilet can detect certain proteins, immune system biomarkers and blood cells that indicate the presence of such diseases as infections, bladder cancer, and kidney failure.
The rationale behind this invention is that some of the best ways of detecting what's going on in our bodies is by analyzing the substances we excrete every day, our sweat, urine, saliva and yes, our feces. Instead of getting sporadic snapshots from doctor's visits once or twice a year, the smart toilet provides continuous monitoring of our health 24/7, so we can catch the tell-tale molecular signature of illnesses at their earliest and most treatable stages. A brainchild of Stanford University researchers, they're now working to add a COVID-19 detection component to their suite of technologies—corona virus particles can be spotted in stool samples—and hope to have the system available within the year.
"We can connect the toilet system to cell phones so we'll know the results within 30 minutes," says Seung-min Park, a lead investigator on the research team that devised this technology and a senior research scientist at the Stanford University School of Medicine. "The beauty of this technology is that it can continuously monitor even after this pandemic is over. It's a way of doing community surveillance. If there is a second wave of infections in the future, we'll know right away."
Experts believe that the COVID-19 pandemic will accelerate the widespread acceptance of in-home diagnostic tools such as this. "Shock events" like pandemics can be catalysts for sweeping changes in society, history shows us. The Black Death marked the end of feudalism and ushered in the Renaissance while the aftershocks of the Great Depression and two world wars in the 20th century led to the social safety net of the New Deal and NATO and the European Union. COVID-19 could fundamentally alter the way we deliver healthcare, abandoning the outdated 20th century brick and mortar fee-for-service model in favor of digital medicine. At-home diagnostics may be the leading edge of this seismic shift and the pandemic could accelerate the product innovations that allow for home-based medical screening.
"That's the silver lining to this devastation," says Dr. Leslie Saxon, executive director of the USC Center for Body Computing at the Keck School of Medicine in Los Angeles. As an interventional cardiologist, Saxon has spent her career devising and refining the implantable and wearable wireless devices that are used to treat and diagnose heart conditions and prevent sudden death. "This will open up innovation—research has been stymied by a lack of imagination and marriage to an antiquated model," she adds. "There are already signs this is happening—relaxing state laws about licensure, allowing physicians to deliver health care in non-traditional ways. That's a real sea change and will completely democratize medical information and diagnostic testing."
Ironically, diagnostics have long been a step-child of modern medicine, even though accurate and timely diagnostics play a crucial role in disease prevention, detection and management. "The delivery of health care has proceeded for decades with a blind spot: diagnostic errors—inaccurate or delayed diagnoses—persist throughout all settings of care and continue to harm an unacceptable number of patients," according to a 2015 National Academy of Medicine report. That same report found as many as one out of five adverse events in the hospital result from these errors and they contribute to 10 percent of all patient deaths.
The pandemic should alter the diagnostic landscape. We already have a wealth of wearable and implantable devices, like glucose sensors to monitor blood sugar levels for diabetics, Apple's smart watch, electrocardiogram devices that can detect heart arrythmias, and heart pacemakers.
The Food and Drug Administration is working closely with in-home test developers to make accurate COVID-19 diagnostic tools readily available and has so far greenlighted three at-home collection test kits. Two, LabCorp's and Everlywell's, use nasal swabs to take samples. The third one is a spit test, using saliva samples, that was devised by a Rutgers University laboratory in partnership with Spectrum Solutions and Accurate Diagnostic Labs.
The only way to safely reopen is through large scale testing, but hospitals and doctors' offices are no longer the safest places.
In fact, DIY diagnostic company Everlywell, an Austin, Texas- based digital health company, already offers more than 30 at-home kits for everything from fertility to food sensitivity tests. Typically, consumers collect a saliva or finger-prick blood sample, dispatch it in a pre-paid shipping envelope to a laboratory, and a physician will review the results and send a report to consumers' smartphones.
Thanks to advances in technology, samples taken at home can now be preserved long enough to arrive intact at diagnostic laboratories. The key is showing the agency "transport and shipping don't change or interfere with the integrity of the samples," says Dr. Frank Ong, Everlywell's chief medical and scientific officer.
Ong is keenly aware of the importance of saturation testing because of the lessons learned by colleagues fighting the SARS pandemic in his family's native Taiwan in 2003. "In the beginning, doctors didn't know what they were dealing with and didn't protect themselves adequately," he says. "But over two years, they learned the hard way that there needs to be enough testing, contact tracing of those who have been exposed, and isolation of people who test positive. The value of at-home testing is that it can be done on the kind of broad basis that needs to happen for our country to get back to work."
Because of the pandemic, new policies have removed some of the barriers that impeded the widespread adoption of home-based diagnostics and telemedicine. Physicians can now practice across state lines, get reimbursed for telemedicine visits and use FaceTime to communicate with their patients, which had long been considered taboo because of privacy issues. Doctors and patients are becoming more comfortable and realizing the convenience and benefits of being able to do these things virtually.
Added to this, the only way to safely reopen for business without triggering a second and perhaps even more deadly wave of sickness is through large-scale testing, but hospitals and doctors' offices are no longer the safest places. "We don't want people sitting in a waiting room who later find out they're positive, and potentially infected everyone, including doctors and nurses," says Dr. Kavita Patel, a physician in Washington, DC who served as a policy director in the Obama White House.
In-home testing avoids the risks of direct exposure to the virus for both patients and health care professionals, who can dispense with cumbersome protective gear to take samples, and also enables people without reliable transportation or child-care to learn their status. "At home testing can be a critical component of our country's overall testing strategy," says Dr. Shantanu Nundy, chief medical officer at Accolade Health and on the faculty of the Milken Institute School of Public Health at George Washington University. "Once we're back at work, we need to be much more targeted, and have much more access to data and controlling those outbreaks as tightly as possible. The best way to do that is by leapfrogging clinics and being able to deliver tests at home for people who are disenfranchised by the current system."
In the not-too-distant future, in-home diagnostics could be a key component of precision medicine, which is customized care tailored specifically to each patient's individual needs. Like Stanford's smart toilet prototype, these ongoing surveillance tools will gather health data, ranging from exposures to toxins and pollutions in the environment to biochemical activity, like rising blood pressure, signs of inflammation, failing kidneys or tiny cancerous tumors, and provide continuous real-time information.
"These can be deeply personalized and enabled by smart phones, sensors and artificial intelligence," says USC's Leslie Saxon. "We'll be seeing the floodgates opening to patients accessing medical services through the same devices that they access other things, and leveraging these tools for our health and to fine tune disease management in a model of care that is digitally enabled."
[Editor's Note: This article was originally published on June 8th, 2020 as part of a standalone magazine called GOOD10: The Pandemic Issue. Produced as a partnership among LeapsMag, The Aspen Institute, and GOOD, the magazine is available for free online.]
Urinary tract infections account for more than 8 million trips to the doctor each year.
Few things are more painful than a urinary tract infection (UTI). Common in men and women, these infections account for more than 8 million trips to the doctor each year and can cause an array of uncomfortable symptoms, from a burning feeling during urination to fever, vomiting, and chills. For an unlucky few, UTIs can be chronic—meaning that, despite treatment, they just keep coming back.
But new research, presented at the European Association of Urology (EAU) Congress in Paris this week, brings some hope to people who suffer from UTIs.
Clinicians from the Royal Berkshire Hospital presented the results of a long-term, nine-year clinical trial where 89 men and women who suffered from recurrent UTIs were given an oral vaccine called MV140, designed to prevent the infections. Every day for three months, the participants were given two sprays of the vaccine (flavored to taste like pineapple) and then followed over the course of nine years. Clinicians analyzed medical records and asked the study participants about symptoms to check whether any experienced UTIs or had any adverse reactions from taking the vaccine.
The results showed that across nine years, 48 of the participants (about 54%) remained completely infection-free. On average, the study participants remained infection free for 54.7 months—four and a half years.
“While we need to be pragmatic, this vaccine is a potential breakthrough in preventing UTIs and could offer a safe and effective alternative to conventional treatments,” said Gernot Bonita, Professor of Urology at the Alta Bro Medical Centre for Urology in Switzerland, who is also the EAU Chairman of Guidelines on Urological Infections.
The news comes as a relief not only for people who suffer chronic UTIs, but also to doctors who have seen an uptick in antibiotic-resistant UTIs in the past several years. Because UTIs usually require antibiotics, patients run the risk of developing a resistance to the antibiotics, making infections more difficult to treat. A preventative vaccine could mean less infections, less antibiotics, and less drug resistance overall.
“Many of our participants told us that having the vaccine restored their quality of life,” said Dr. Bob Yang, Consultant Urologist at the Royal Berkshire NHS Foundation Trust, who helped lead the research. “While we’re yet to look at the effect of this vaccine in different patient groups, this follow-up data suggests it could be a game-changer for UTI prevention if it’s offered widely, reducing the need for antibiotic treatments.”
MILESTONE: Doctors have transplanted a pig organ into a human for the first time in history
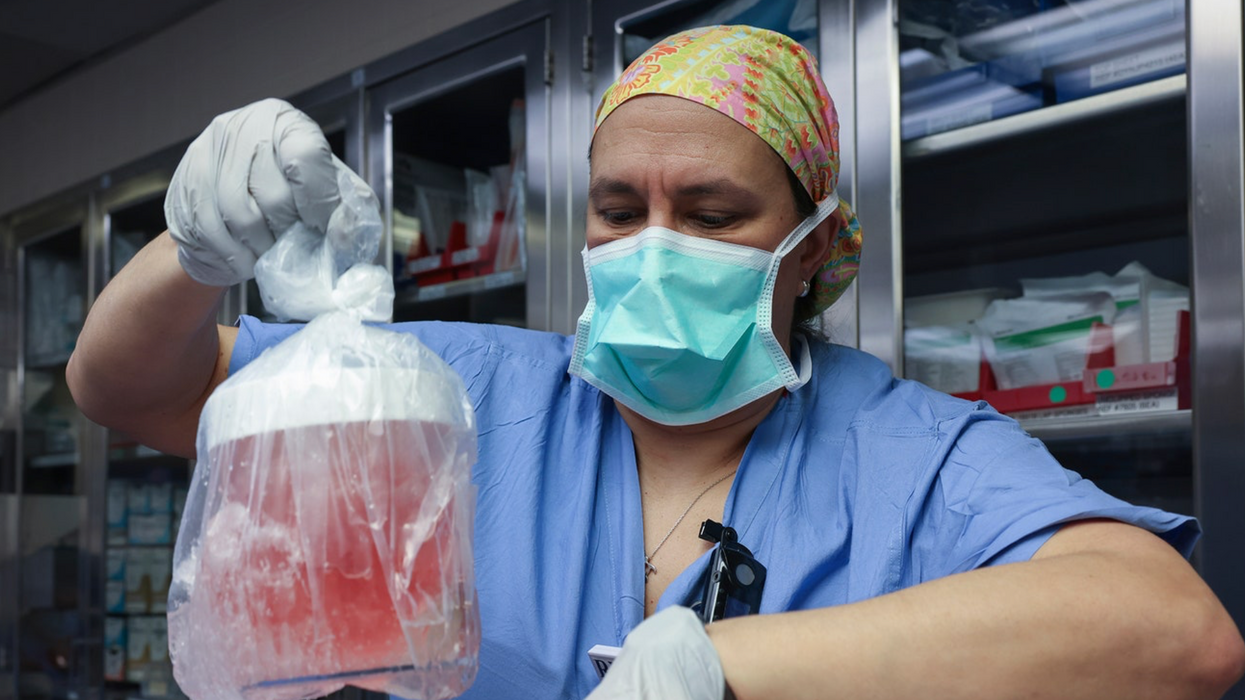
A surgeon at Massachusetts General Hospital prepares a pig organ for transplant.
Surgeons at Massachusetts General Hospital made history last week when they successfully transplanted a pig kidney into a human patient for the first time ever.
The recipient was a 62-year-old man named Richard Slayman who had been living with end-stage kidney disease caused by diabetes. While Slayman had received a kidney transplant in 2018 from a human donor, his diabetes ultimately caused the kidney to fail less than five years after the transplant. Slayman had undergone dialysis ever since—a procedure that uses an artificial kidney to remove waste products from a person’s blood when the kidneys are unable to—but the dialysis frequently caused blood clots and other complications that landed him in the hospital multiple times.
As a last resort, Slayman’s kidney specialist suggested a transplant using a pig kidney provided by eGenesis, a pharmaceutical company based in Cambridge, Mass. The highly experimental surgery was made possible with the Food and Drug Administration’s “compassionate use” initiative, which allows patients with life-threatening medical conditions access to experimental treatments.
The new frontier of organ donation
Like Slayman, more than 100,000 people are currently on the national organ transplant waiting list, and roughly 17 people die every day waiting for an available organ. To make up for the shortage of human organs, scientists have been experimenting for the past several decades with using organs from animals such as pigs—a new field of medicine known as xenotransplantation. But putting an animal organ into a human body is much more complicated than it might appear, experts say.
“The human immune system reacts incredibly violently to a pig organ, much more so than a human organ,” said Dr. Joren Madsen, director of the Mass General Transplant Center. Even with immunosuppressant drugs that suppress the body’s ability to reject the transplant organ, Madsen said, a human body would reject an animal organ “within minutes.”
So scientists have had to use gene-editing technology to change the animal organs so that they would work inside a human body. The pig kidney in Slayman’s surgery, for instance, had been genetically altered using CRISPR-Cas9 technology to remove harmful pig genes and add human ones. The kidney was also edited to remove pig viruses that could potentially infect a human after transplant.
With CRISPR technology, scientists have been able to prove that interspecies organ transplants are not only possible, but may be able to successfully work long term, too. In the past several years, scientists were able to transplant a pig kidney into a monkey and have the monkey survive for more than two years. More recently, doctors have transplanted pig hearts into human beings—though each recipient of a pig heart only managed to live a couple of months after the transplant. In one of the patients, researchers noted evidence of a pig virus in the man’s heart that had not been identified before the surgery and could be a possible explanation for his heart failure.
So far, so good
Slayman and his medical team ultimately decided to pursue the surgery—and the risk paid off. When the pig organ started producing urine at the end of the four-hour surgery, the entire operating room erupted in applause.
Slayman is currently receiving an infusion of immunosuppressant drugs to prevent the kidney from being rejected, while his doctors monitor the kidney’s function with frequent ultrasounds. Slayman is reported to be “recovering well” at Massachusetts General Hospital and is expected to be discharged within the next several days.