Americans Fell for a Theranos-Style Scam 100 Years Ago. Will We Ever Learn?

Medical scams like Theranos are as American as America itself.
The huckster understands what people want – an easy route to good health -- and figures out just how to provide it as long as no one asks too many questions.
"Americans are very much prone to this sort of thinking: Give me a pill or give me a magical bean that can make me lose weight!"
The keys to success: Hoopla, fancy technology, and gullibility. And oh yes, one more thing: a blood sample. Well, lots and lots of blood samples. Every testing fee counts.
Sound familiar? It could be the story of the preternaturally persuasive Elizabeth Holmes, the disgraced founder of Theranos who stands accused of perpetrating a massive blood-testing fraud. But this is a different story from a different time, one that dates back 100 years but sounds almost like it could unfold on the front page of The Wall Street Journal today.
The main difference: Back then, watchdogs thought they'd be able to vanquish fake medicine and scam science. Fat chance, it turned out. It seems like we're more likely to lose-weight-quick than make much of a dent into quackery and health fraud.
Why? Have we learned anything at all over the past century? As we sweep into a new decade, experts says we're not as advanced as we'd like to think. But the fight against fraud and fakery continues.
Quackery: As American As America Itself
In the 17th century, British healers of questionable reputation got a new name -- "quack," from the Dutch word "quacksalver," which originally referred to someone who treats others with home remedies but developed a new meaning along the lines of "charlatan." And these quacks got a new place to sell their wares: the American colonies.
By 1692, a Boston newspaper advertised a patent medicine that promised to cure "the Griping of the Guts, and the Wind Cholick" and – for good measure – "preventeth that woeful Distemper of the Dry Belly Ach." A couple centuries later, the most famous woman in the United States wasn't a first lady or feminist but a hawker of nostrums named Lydia Estes Pinkham whose "vegetable compound" promised to banish "female complaints." One advertisement suggested that the "sure cure" would have saved the life of a Connecticut clergyman whose wife killed him after suffering from feminine maladies for 16 years.
By the early 20th century, Americans were fascinated by electricity and radiation, and both healers and hucksters embraced the new high-tech era. Men with flagging libidos, for example, could irradiate their private parts with the radioactive Radiendocrinator or buy battery-powered electric belts equipped with dangling bits to supercharge their, um, dangling bits.
The Rise of the Radio Wave 'Cure'
Enter radionics, the (supposed) science of better health via radio waves. The idea was that "healthy people radiate healthy energy," and sickness could be reversed through diagnosis and re-tuning, write Dr. Lydia Kang and Nate Pedersen in their 2017 book "Quackery: A Brief History of the Worst Ways to Cure Everything."
Detecting illness and fixing it required machinery -- Dynamizers, Radioclasts and Oscillocasts – that could cost hundreds of dollars each. Thousands of physicians bought them. Fortunately, they could work remotely, for a fee. The worried-and-potentially-unwell just needed to send a blood sample and, of course, a personal check.
Sting operations revealed radionics to be bogus. A skeptic sent a blood sample to one radionics practitioner in Albuquerque who reported back with news of an infected fallopian tube. In fact, the blood sample came from a male guinea pig. As an American Medical Association leader reported, the guinea pig "had shown no female characteristics up to that time, and a postmortem examination yielded no evidence of ladylike attributes."
When Quackery Refused to Yield
The rise of bogus medical technology in the early 20th century spawned a watchdog industry as organizations like the American Medical Association swept into action, said medical historian Eric Boyle, author of 2012's "Quack Medicine: A History of Combating Health Fraud in Twentieth-Century America."
"When quackery was recognized as a major problem, the people who campaigned for its demise were confident that they could get rid of it," he said. "A lot of people believed that increased education, the truths of science, and laws designed to protect consumers would ultimately drive quackery from the marketplace. And then throughout the century, as modern medicine developed, and more effectively treated one disease after another, many observers remained confident in that prediction."
There's a bid to "flood the information highway with truth to turn the storm of fake promotional stuff into a trickle."
But fake medicine persisted as Americans continued their quest to get- healthy-quick… or get-rich-quick by promising to help others to get- healthy-quick. Even radionics refused to die. It's still around in various forms. And, as the Theranos scandal reveals, we're still hoping our blood can offer the keys to longevity and good health.
Why Do We Still Fall for Scams?
In our own era, the Theranos company rose to prominence when founder and CEO Elizabeth Holmes convinced journalists and investors that she'd found a way to cheaply test drops of blood for hundreds of conditions. Then it all fell apart, famously, when the world learned that the technology didn't work. The company has folded, and Holmes faces a federal trial on fraud charges this year.
"There were a lot of prominent, very smart people who bought into the myth of Elizabeth Holmes," a former employee told "60 Minutes," even though the blood tests never actually worked as advertised.
Shouldn't "prominent, very smart people" know better? "People are gullible," said Dr. Stephen Barrett, a psychiatrist and leading quack-buster who runs the QuackWatch website. But there's more to the story. According to him, we're uniquely vulnerable as individuals to bogus medicine.
Scam artists specifically pinpoint their target audiences, such as "smart people," desperate people and alienated people, he said.
Smart people, for example, might be overconfident about their ability to detect fraud and fall for bogus medicine. Alienated people may distrust the establishment, whether it's the medical field or government watchdogs, and be more receptive to alternative sources of information.
Dr. Barrett also points a finger at magical thinking, which comes in different forms. It could mean a New Age-style belief that our minds can control the world around us. Or, as professional quack-buster Alex Berezow said, it could refer to "our cultural obsession with quick fixes."
"Americans are very much prone to this sort of thinking: Give me a pill or give me a magical bean that can make me lose weight! But complex problems need complex solutions," said Berezow, a microbiologist who debunks junk science in his job as a spokesman for the American Council on Science & Health.
American mistrust of expertise makes matters worse, he said. "When I tell people they need to get vaccinated, I'm called a shill for the pharmaceutical industry," he said. "If I say dietary supplements generally don't work, I'm a shill for doctors who want to keep people sick."
What can ordinary citizens do to protect themselves from fake medicine? "You have to have a healthy skepticism of everything," Berezow said. "When you come across something new, is someone trying to take advantage of you? It's a horrible way to think about the world, but there's some truth to it."
"Like any chronic disease, we will have to live with it while we do our best to fight it."
The government and experts have their own roles to play via regulation and education, respectively. For all the criticism it gets, the Food & Drug Administration does serve as a bulwark against fakery in prescription medicine. And while celebrities like Gwyneth "Goop" Paltrow hawk countless questionable medical products on the Internet, scientists and physicians are fighting back by using social media as a tool to promote the truth. There's a bid to "flood the information highway with truth to turn the storm of fake promotional stuff into a trickle," said Dr. Randi Hutter Epstein, a writer in residence at Yale School of Medicine and author of 2018's "Aroused: The History of Hormones and How They Control Just About Everything."
What's next? Like death, taxes and Cher, charlatans are likely to always be with us. Boyle quoted the late William Jarvis, a pioneering quack-buster in the late 20th century who believed health fraud would never be eradicated: "Like any chronic disease, we will have to live with it while we do our best to fight it."
Your surgery could harm yourself and the planet. Here's what some doctors are doing about it.
Certain gases used for anesthesia are 3,000 times more damaging for the climate than CO2. Some anesthesiologists are pointing to other solutions.
This is part 1 of a three part series on a new generation of doctors leading the charge to make the health care industry more sustainable - for the benefit of their patients and the planet. Read part 2 here and part 3 here.
Susanne Koch, an anesthesiologist and neurologist, reached a pivot point when she was up to her neck in water, almost literally. The basement of her house in Berlin had flooded in the summer of 2018, when Berlin was pummeled by unusually strong rains. After she drained the house, “I wanted to dig into facts, to understand how exactly these extreme weather events are related to climate change,” she says.
Studying the scientific literature, she realized how urgent the climate crisis is, but the biggest shock was to learn that her profession contributed substantially to the problem: Inhalation gases used during medical procedures are among the most damaging greenhouse gases. Some inhalation gases are 3,000 times more damaging for the climate than CO2, Koch discovered. “Spending seven hours in the surgery room is the equivalent of driving a car for four days nonstop,” she says. Her job of helping people at Europe’s largest university hospital, the Charité in Berlin, was inadvertently damaging both the people and the planet.
“Nobody had ever even mentioned a word about that during my training,” Koch says.
On the whole, the medical sector is responsible for a disproportionally large percentage of greenhouse gas emissions, with the U.S. as the biggest culprit. According to a key paper published in 2020 in Health Affairs, the health industry “is among the most carbon-intensive service sectors in the industrialized world,” accounting for between 4.4 percent and 4.6 percent of greenhouse gas emissions. “It’s not just anesthesia but health care that has a problem,” says Jodi Sherman, anesthesiology professor and Medical Director of the Program on Healthcare Environmental Sustainability at Yale University as well as co-director of the Lancet Planetary Health Commission on Sustainable Healthcare. In the U.S., health care greenhouse gas emissions make up about 8.5 percent of domestic greenhouse gas emissions. They rose 6 percent from 2010 to 2018, to nearly 1,700 kilograms per person, more than in any other nation.
Of course, patients worry primarily about safety, not sustainability. Yet, Koch emphasizes that “as doctors, we have the responsibility to do no harm, and this includes making sure that we use resources as sustainably as possible.” Studies show that 2018 greenhouse gas and toxic air pollutant emissions resulted in the loss of 388,000 disability-adjusted life years in the U.S. alone. “Disease burden from health care pollution is of the same order of magnitude as deaths from preventable medical errors, and should be taken just as seriously,” Sherman cautions.
When Koch, the anesthesiologist, started discussing sustainable options with colleagues, the topic was immediately met with plenty of interest. Her experience is consistent with the latest representative poll of the nonprofit Foundation Health in Germany. Nine out of ten doctors were interested in urgently finding sustainable solutions for medical services but lacked knowhow and resources. For teaching purposes, Sherman and her team have developed the Yale Gassing Greener app that allows anesthesiologists to compare how much pollution they can avoid through choosing different anesthesia methods. Sherman also published professional guidelines intended to help her colleagues better understand how various methods affect carbon emissions.
Significant traces of inhalation gases have been found in Antarctica and the Himalayas, far from the vast majority of surgery rooms.
A solution espoused by both Sherman and Koch is comparatively simple: They stopped using desflurane, which is by far the most damaging of all inhalation gases to the climate. Its greenhouse effect is 2,590 times stronger than carbon dioxide. The Yale New Haven Hospital already stopped using desflurane in 2013, becoming the first known healthcare organization to eliminate a drug based on environmental grounds. Sherman points out that this resulted in saving more than $1.2 million in costs and 1,600 tons of CO2 equivalents, about the same as the exhaust from 360 passenger vehicles per year.
At the Charité, Koch claims that switching to other anesthesiology choices, such as propofol, has eliminated 90 percent of the climate gas emissions in the anesthesiology department since 2016. Young anesthesiologists are still taught to use desflurane as the standard because desflurane is absorbed less into the patients’ bodies, and they wake up faster. However, Koch who has worked as an anesthesiologist since 2006, says that with a little bit of experience, you can learn when to stop giving the propofol so it's timed just as well with a person’s wake-up process. In addition, “patients are less likely to feel nauseous after being given propofol,” Koch says. Intravenous drugs might require more skill, she adds, "but there is nothing unique to the drug desflurane that cannot be accomplished with other medications.”
Desflurane isn’t the only gas to be concerned about. Nitrous oxide is the second most damaging because it’s extremely long-lived in the environment, and it depletes the ozone layer. Climate-conscious anesthesiologists are phasing out this gas, too, or have implemented measures to decrease leaks.
Internationally, 192 governments agreed in the Kyoto protocol of 2005 to reduce halogenated hydrocarbons – resulting from inhalation gases, including desflurane and nitrous oxide – because of their immense climate-warming potential, and in 2016, they pledged to eliminate them by 2035. However, the use of inhalation anesthetics continues to increase worldwide, not least because more people access healthcare in developing countries, and because people in industrialized countries live longer and therefore need more surgeries. Significant traces of inhalation gases have been found in Antarctica and the Himalayas, far from the vast majority of surgery rooms.
Certain companies are now pushing new technology to capture inhalation gases before they are released into the atmosphere, but both Sherman and Koch believe marketing claims of 99 percent efficiency amount to greenwashing. After investigating the technology first-hand and visiting the company that is producing such filters in Germany, Koch concluded that such technology only reduces emissions by 25 percent. And Sherman believes such initiatives are akin to the fallacy of recycling plastic. In addition to questioning their efficiency, Sherman fears such technology “gives the illusion there is a magical solution that means I don’t need to change my behavior, reduce my waste and choose less harmful options.”
Financial interests are at play, too. “Desflurane is the most expensive inhalation gas, and some think, the most expensive must be the best,” Koch says. Both Koch and Sherman lament that efforts to increase sustainability in the medical sector are entirely voluntary in their countries and led by a few dedicated individual professionals while industry-wide standards and transparency are needed, a notion expressed in the American Hospital Association’s Sustainability Roadmap.

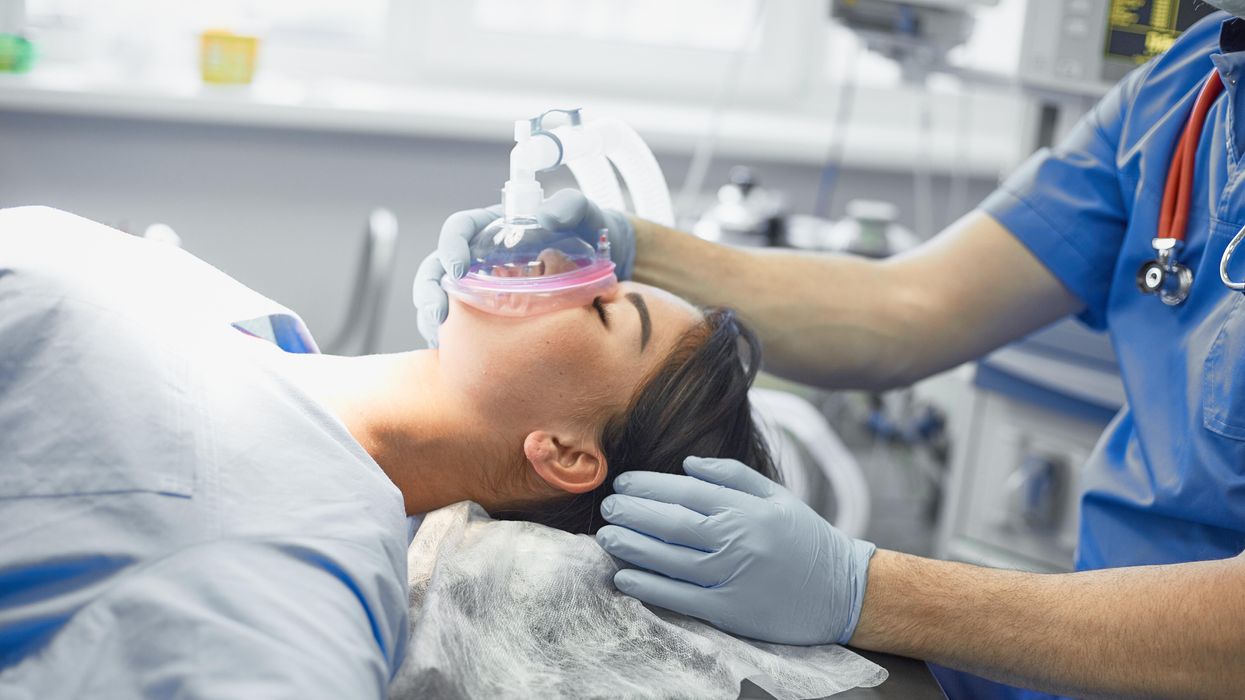
Susanne Koch, an anesthesiologist in Berlin, wants her colleagues to stop using a gas called desflurane, which is by far the most damaging of all inhalation gases to the climate.
Adobe Stock
Other countries have done more. The European Union recommends reducing inhalation gases and even contemplated a ban of desflurane, except in medical emergencies. In 2008, the National Health Service (NHS) created a Sustainable Development Unit, which measures CO2 emissions in the U.K. health sector. NHS is the first national health service that pledged to reach net zero carbon by 2040. The carbon footprint of the NHS fell by 26 percent from 1990 to 2019, mostly due to reduced use of certain inhalers and the switch to renewable energy for heat and power. “The evidence that the climate emergency is a health emergency is overwhelming,” said Nick Watts, the NHS Chief Sustainability Officer, in a press release, “with health professionals already needing to manage its symptoms.”
Sherman is a leading voice in demanding action in the U.S. To her, comprehensive solutions start with the mandatory, transparent measurement of emissions in the health sector to tackle the biggest sources of pollution. While the Biden administration highlighted its efforts to reduce these kinds of emissions during the United Nations Climate Conference (COP27) in November 2022 and U.S. delegates announced that more than 100 health care organizations signed the voluntary Health Sector Climate Pledge, with the aim to reduce emissions by 50 percent in the next eight years, Sherman is convinced that voluntary pledges are not enough. “Voluntary measures are insufficient,” she testified in congress. “The vast majority of U.S. health care organizations remain uncommitted to timely action. Those that are committed lack policies and knowledge to support necessary changes; even worse, existing policies drive inappropriate consumption of resources and pollution.”
Both Sherman and Koch look at the larger picture. “Health care organizations have an obligation to their communities to protect public health,” Sherman says. “We must lead by example. That includes setting ambitious, science-based carbon reduction targets to achieve net zero emissions before 2050. We must quantify current emissions and their sources, particularly throughout the health care supply chains.”
Have You Heard of the Best Sport for Brain Health?
In this week's Friday Five, research points to this brain healthiest of sports. Plus, the natural way to reprogram cells to a younger state, the network that could underlie many different mental illnesses, and a new test could diagnose autism in newborns. Plus, scientists 3D print an ear and attach it to woman
The Friday Five covers five stories in research that you may have missed this week. There are plenty of controversies and troubling ethical issues in science – and we get into many of them in our online magazine – but this news roundup focuses on scientific creativity and progress to give you a therapeutic dose of inspiration headed into the weekend.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
Here are the promising studies covered in this week's Friday Five:
- Reprogram cells to a younger state
- Pick up this sport for brain health
- Do all mental illnesses have the same underlying cause?
- New test could diagnose autism in newborns
- Scientists 3D print an ear and attach it to woman