New tools could catch disease outbreaks earlier - or predict them

A team at the Catalan Institution for Research and Advanced Studies is utilizing drones and weather stations to collect data on how mosquito breeding patterns are changing in response to climate shifts.
Every year, the villages which lie in the so-called ‘Nipah belt’— which stretches along the western border between Bangladesh and India, brace themselves for the latest outbreak. For since 1998, when Nipah virus—a form of hemorrhagic fever most common in Bangladesh—first spilled over into humans, it has been a grim annual visitor to the people of this region.
With a 70 percent fatality rate, no vaccine, and no known treatments, Nipah virus has been dubbed in the Western world as ‘the worst disease no one has ever heard of.’ Currently, outbreaks tend to be relatively contained because it is not very transmissible. The virus circulates throughout Asia in fruit eating bats, and only tends to be passed on to people who consume contaminated date palm sap, a sweet drink which is harvested across Bangladesh.
But as SARS-CoV-2 has shown the world, this can quickly change.
“Nipah virus is among what virologists call ‘the Big 10,’ along with things like Lassa fever and Crimean Congo hemorrhagic fever,” says Noam Ross, a disease ecologist at New York-based non-profit EcoHealth Alliance. “These are pretty dangerous viruses from a lethality perspective, which don’t currently have the capacity to spread into broader human populations. But that can evolve, and you could very well see a variant emerge that has human-human transmission capability.”
That’s not an overstatement. Surveys suggest that mammals harbour about 40,000 viruses, with roughly a quarter capable of infecting humans. The vast majority never get a chance to do so because we don’t encounter them, but climate change can alter that. Recent studies have found that as animals relocate to new habitats due to shifting environmental conditions, the coming decades will bring around 300,000 first encounters between species which normally don’t interact, especially in tropical Africa and southeast Asia. All these interactions will make it far more likely for hitherto unknown viruses to cross paths with humans.
That’s why for the last 16 years, EcoHealth Alliance has been conducting ongoing viral surveillance projects across Bangladesh. The goal is to understand why Nipah is so much more prevalent in the western part of the country, compared to the east, and keep a watchful eye out for new Nipah strains as well as other dangerous pathogens like Ebola.
"There are a lot of different infectious agents that are sensitive to climate change that don't have these sorts of software tools being developed for them," says Cat Lippi, medical geography researcher at the University of Florida.
Until very recently this kind of work has been hampered by the limitations of viral surveillance technology. The PREDICT project, a $200 million initiative funded by the United States Agency for International Development, which conducted surveillance across the Amazon Basin, Congo Basin and extensive parts of South and Southeast Asia, relied upon so-called nucleic acid assays which enabled scientists to search for the genetic material of viruses in animal samples.
However, the project came under criticism for being highly inefficient. “That approach requires a big sampling effort, because of the rarity of individual infections,” says Ross. “Any particular animal may be infected for a couple of weeks, maybe once or twice in its lifetime. So if you sample thousands and thousands of animals, you'll eventually get one that has an Ebola virus infection right now.”
Ross explains that there is now far more interest in serological sampling—the scientific term for the process of drawing blood for antibody testing. By searching for the presence of antibodies in the blood of humans and animals, scientists have a greater chance of detecting viruses which started circulating recently.
Despite the controversy surrounding EcoHealth Alliance’s involvement in so-called gain of function research—experiments that study whether viruses might mutate into deadlier strains—the organization’s separate efforts to stay one step ahead of pathogen evolution are key to stopping the next pandemic.
“Having really cheap and fast surveillance is really important,” says Ross. “Particularly in a place where there's persistent, low level, moderate infections that potentially have the ability to develop into more epidemic or pandemic situations. It means there’s a pathway that something more dangerous can come through."
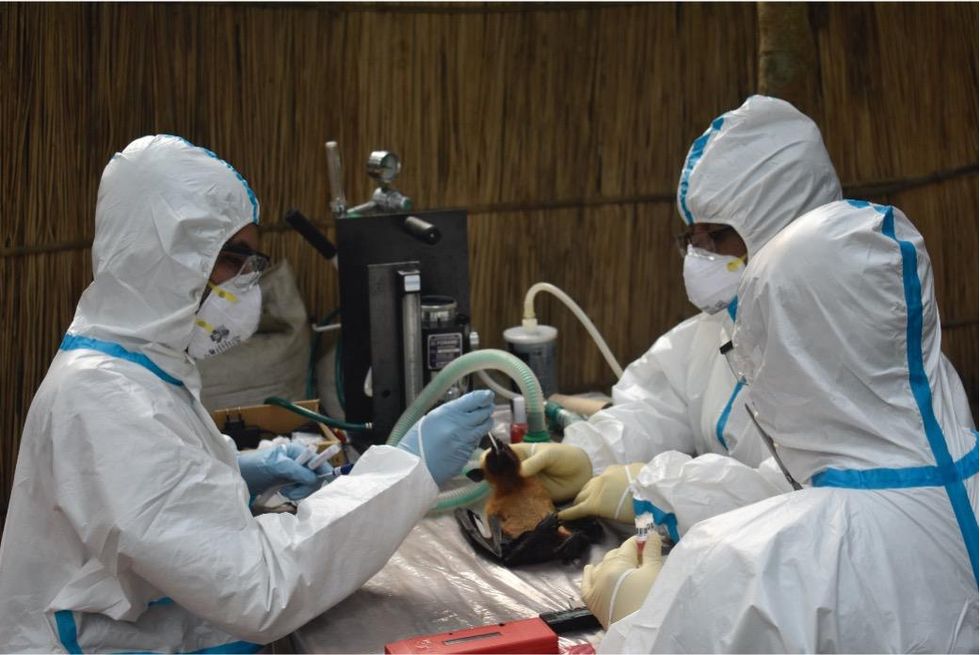
Scientists are searching for the presence of antibodies in the blood of humans and animals in hopes to detect viruses that recently started circulating.
EcoHealth Alliance
In Bangladesh, EcoHealth Alliance is attempting to do this using a newer serological technology known as a multiplex Luminex assay, which tests samples against a panel of known antibodies against many different viruses. It collects what Ross describes as a ‘footprint of information,’ which allows scientists to tell whether the sample contains the presence of a known pathogen or something completely different and needs to be investigated further.
By using this technology to sample human and animal populations across the country, they hope to gain an idea of whether there are any novel Nipah virus variants or strains from the same family, as well as other deadly viral families like Ebola.
This is just one of several novel tools being used for viral discovery in surveillance projects around the globe. Multiple research groups are taking PREDICT’s approach of looking for novel viruses in animals in various hotspots. They collect environmental DNA—mucus, faeces or shed skin left behind in soil, sediment or water—which can then be genetically sequenced.
Five years ago, this would have been a painstaking work requiring bringing collected samples back to labs. Today, thanks to the vast amounts of money spent on new technologies during COVID-19, researchers now have portable sequencing tools they can take out into the field.
Christopher Jerde, a researcher at the UC Santa Barbara Marine Science Institute, points to the Oxford Nanopore MinION sequencer as one example. “I tried one of the early versions of it four years ago, and it was miserable,” he says. “But they’ve really improved, and what we’re going to be able to do in the next five to ten years will be amazing. Instead of having to carefully transport samples back to the lab, we're going to have cigar box-shaped sequencers that we take into the field, plug into a laptop, and do the whole sequencing of an organism.”
In the past, viral surveillance has had to be very targeted and focused on known families of viruses, potentially missing new, previously unknown zoonotic pathogens. Jerde says that the rise of portable sequencers will lead to what he describes as “true surveillance.”
“Before, this was just too complex,” he says. “It had to be very focused, for example, looking for SARS-type viruses. Now we’re able to say, ‘Tell us all the viruses that are here?’ And this will give us true surveillance – we’ll be able to see the diversity of all the pathogens which are in these spots and have an understanding of which ones are coming into the population and causing damage.”
But being able to discover more viruses also comes with certain challenges. Some scientists fear that the speed of viral discovery will soon outpace the human capacity to analyze them all and assess the threat that they pose to us.
“I think we're already there,” says Jason Ladner, assistant professor at Northern Arizona University’s Pathogen and Microbiome Institute. “If you look at all the papers on the expanding RNA virus sphere, there are all of these deposited partial or complete viral sequences in groups that we just don't know anything really about yet.” Bats, for example, carry a myriad of viruses, whose ability to infect human cells we understand very poorly.
Cultivating these viruses under laboratory conditions and testing them on organoids— miniature, simplified versions of organs created from stem cells—can help with these assessments, but it is a slow and painstaking work. One hope is that in the future, machine learning could help automate this process. The new SpillOver Viral Risk Ranking platform aims to assess the risk level of a given virus based on 31 different metrics, while other computer models have tried to do the same based on the similarity of a virus’s genomic sequence to known zoonotic threats.
However, Ladner says that these types of comparisons are still overly simplistic. For one thing, scientists are still only aware of a few hundred zoonotic viruses, which is a very limited data sample for accurately assessing a novel pathogen. Instead, he says that there is a need for virologists to develop models which can determine viral compatibility with human cells, based on genomic data.
“One thing which is really useful, but can be challenging to do, is understand the cell surface receptors that a given virus might use,” he says. “Understanding whether a virus is likely to be able to use proteins on the surface of human cells to gain entry can be very informative.”
As the Earth’s climate heats up, scientists also need to better model the so-called vector borne diseases such as dengue, Zika, chikungunya and yellow fever. Transmitted by the Aedes mosquito residing in humid climates, these blights currently disproportionally affect people in low-income nations. But predictions suggest that as the planet warms and the pests find new homes, an estimated one billion people who currently don’t encounter them might be threatened by their bites by 2080. “When it comes to mosquito-borne diseases we have to worry about shifts in suitable habitat,” says Cat Lippi, a medical geography researcher at the University of Florida. “As climate patterns change on these big scales, we expect to see shifts in where people will be at risk for contracting these diseases.”
Public health practitioners and government decision-makers need tools to make climate-informed decisions about the evolving threat of different infectious diseases. Some projects are already underway. An ongoing collaboration between the Catalan Institution for Research and Advanced Studies and researchers in Brazil and Peru is utilizing drones and weather stations to collect data on how mosquitoes change their breeding patterns in response to climate shifts. This information will then be fed into computer algorithms to predict the impact of mosquito-borne illnesses on different regions.

The team at the Catalan Institution for Research and Advanced Studies is using drones and weather stations to collect data on how mosquito breeding patterns change due to climate shifts.
Gabriel Carrasco
Lippi says that similar models are urgently needed to predict how changing climate patterns affect respiratory, foodborne, waterborne and soilborne illnesses. The UK-based Wellcome Trust has allocated significant assets to fund such projects, which should allow scientists to monitor the impact of climate on a much broader range of infections. “There are a lot of different infectious agents that are sensitive to climate change that don't have these sorts of software tools being developed for them,” she says.
COVID-19’s havoc boosted funding for infectious disease research, but as its threats begin to fade from policymakers’ focus, the money may dry up. Meanwhile, scientists warn that another major infectious disease outbreak is inevitable, potentially within the next decade, so combing the planet for pathogens is vital. “Surveillance is ultimately a really boring thing that a lot of people don't want to put money into, until we have a wide scale pandemic,” Jerde says, but that vigilance is key to thwarting the next deadly horror. “It takes a lot of patience and perseverance to keep looking.”
This article originally appeared in One Health/One Planet, a single-issue magazine that explores how climate change and other environmental shifts are increasing vulnerabilities to infectious diseases by land and by sea. The magazine probes how scientists are making progress with leaders in other fields toward solutions that embrace diverse perspectives and the interconnectedness of all lifeforms and the planet.
Leaps.org spoke with Holden Thorp, Editor-in-Chief of the prestigious Science family of journals, about ways to improve science journalism, the challenges faced by experts, the lab leak theory and much more.
This month, Leaps.org had a chance to speak with Holden Thorp, Editor-in-Chief of the Science family of journals. We talked about the best ways to communicate science to the public, mistakes by public health officials during the pandemic, the lab leak theory, and bipartisanship for funding science research.
Before becoming editor of the Science journals, Thorp spent six years as provost of Washington University in St. Louis, where he is Rita Levi-Montalcini Distinguished University Professor and holds appointments in both chemistry and medicine. He joined Washington University after spending three decades at the University of North Carolina at Chapel Hill, where he served as the UNC's 10th chancellor from 2008 through 2013.
A North Carolina native, Thorp earned a doctorate in chemistry in 1989 at the California Institute of Technology and completed postdoctoral work at Yale University. He is a fellow of the National Academy of Inventors and the American Association for the Advancement of Science.
Read his full bio here.
This conversation was lightly edited by Leaps.org for style and format.
Matt Fuchs: You're a musician. It seems like many scientists are also musicians. Is there a link between the scientist brain and the musician brain?
Holden Thorp: I think [the overlap is] relatively common. I'm still a gigging bass player. I play in the pits for lots of college musicals. I think that it takes a certain discipline and requires you to learn a lot of rules about how music works, and then you try to be creative within that. That's similar to scientific research. So it makes sense. Music is something I've been able to sustain my whole life. I wouldn't be the same person if I let it go. When you're playing, especially for a musical, where the music is challenging, you can't let your mind wander. It’s like meditation.
MF: I bet it helps to do something totally different from your editing responsibilities. Maybe lets the subconscious take care of tough problems at work.
HT: Right.
MF: There's probably never been a greater need for clear and persuasive science communicators. Do we need more cross specialty training? For example, journalism schools prioritizing science training, and science programs that require more time learning how to communicate effectively?
HT: I think we need both. One of the challenges we've had with COVID has been, especially at the beginning, a lot of reporters who didn’t normally cover scientific topics got put on COVID—and ended up creating things that had to be cleaned up later. This isn't the last science-oriented crisis we're going to have. We've already got climate change, and we'll have another health crisis for sure. So it’d be good for journalism to be a little better prepared next time.
"Scientists are human beings who have ego and bravado and every other human weakness."
But on the other side, maybe it's even more important that scientists learn how to communicate and how likely it is that their findings will be politicized, twisted and miscommunicated. Because one thing that surprised me is how shocked a lot of scientists have been. Every scientific issue that reaches into public policy becomes politicized: climate change, evolution, stem cells.
Once one side decided to be cautious about the pandemic, you could be certain the other side was going to decide not to do that. That's not the fault of science. That’s just life in a political world. That, I think, caught people off guard. They weren't prepared to shape and process their messages in a way that accounted for that—and for the way that social media has intensified all of this.
MF: Early in the pandemic, there was a lack of clarity about public health recommendations, as you’d expect with a virus we hadn’t seen before. Should public officials and scientists have more humility in similar situations in the future? Public officials need to be authoritative for their guidance to be followed, so how do they lead a crisis response while displaying humility about what we don't know?
HS: I think scientists are people who like to have the answer. It's very tempting and common for scientists to kind of oversell what we know right now, while not doing as much as we should to remind people that science is a self-correcting process. And when we fail to do that – after we’ve collected more data and need to change how we're interpreting it – the people who want to undermine us have a perfect weapon to use against us. It's challenging. But I agree that scientists are human beings who have ego and bravado and every other human weakness.
For example, we wanted to tell everybody that we thought the vaccines would provide sterilizing immunity against infection. Well, we don't have too many other respiratory viruses where that's the case. And so it was more likely that we were going to have what we ended up with, which is that the vaccines were excellent in preventing severe disease and death. It would have been great if they provided sterilizing immunity and abruptly ended the pandemic a year ago. But it was overly optimistic to think that was going to be the case in retrospect.
MF: Both in terms of how science is communicated and received by the public, do we need to reform institutions or start new ones to instill the truth-seeking values that are so important to appreciating science?
HS: There are a whole bunch of different factors. I think the biggest one is that the social media algorithms reward their owners financially when they figure out how to keep people in their silos. Users are more likely to click on things that they agree with—and that promote conflict with people that they disagree with. That has caused an acceleration in hostilities that attend some of these disagreements.
But I think the other problem is that we haven’t found a way to explain things to people when it’s not a crisis. So, for example, a strong indicator of whether someone who might otherwise be vaccine hesitant decided to get their vaccine is if they understood how vaccines worked before the pandemic started. Because if you're trying to tell somebody that they're wrong if they don't get a vaccine, at the same time you're trying to explain how it works, that's a lot of explaining to do in a short period of time.
Lack of open-mindedness is a problem, but another issue is that we need more understanding of these issues baked into the culture already. That's partly due the fact that there hasn't been more reform in K through 12 and college teaching. And that scientists are very comfortable talking to each other, and not very comfortable talking to people who don't know all of our jargon and have to be persuaded to spend time listening to and thinking about what we're trying to tell them.
"We're almost to the point where clinging to the lab leak idea is close to being a fringe idea that almost doesn't need to be included in stories."
MF: You mentioned silos. There have been some interesting attempts in recent years to do “both sides journalism,” where websites like AllSides put different views on high profile issues side-by-side. Some people believe that's how the news should be reported. Should we let people see and decide for themselves which side is the most convincing?
HS: It depends if we're talking about science. On scientific issues, when they start, there's legitimate disagreement about among scientists. But eventually, things go back and forth, and people compete with each other and work their way to the answer. At some point, we reach more of a consensus.
For example, on climate change, I think it's gotten to the point now where it's irresponsible, if you're writing a story about climate change, to run a quote from somebody somewhere who's still—probably because of their political views—clinging to the idea that anthropogenic global warming is somehow not damaging the planet.
On things that aren't decided yet, that makes sense to run both. It's more a question of judgment of the journalists. I don't think the solution to it is put stark versions of each side, side-by-side and let people choose. The whole point of journalism is to inform people. If there's a consensus on something, that's part of what you're supposed to be informing them about.
MF: What about reporting on perspectives about the lab leak theory at various times during the pandemic?
HS: We’re the outlet that ran the letter that really restarted the whole debate. A bunch of well-known scientists said we should consider the lab leak theory more carefully. And in the aftermath of that, a bunch of those scientists who signed that letter concluded that the lab leak was very, very unlikely. Interestingly, publishing that letter actually drove us to more of a consensus. I would say now, we're almost to the point where clinging to the lab leak idea is close to being a fringe idea that almost doesn't need to be included in stories. But I would say there's been a lot of evolution on that over the last year since we ran that letter.
MF: Let's talk about bipartisanship in Congress. Research funding for the National Institutes of Health was championed for years by influential Republicans who supported science to advance health breakthroughs. Is that changing? Maybe especially with Sen. Roy Blunt retiring? Has bipartisanship on science funding been eroded by political battles during COVID?
HS: I'm optimistic that that won't be the case. Republican Congresses have usually been good for science funding. And that's because (former Sen.) Arlen Specter and Roy Blunt are two of the political figures who have pushed for science funding over the last couple decades. With Blunt retiring, we don't know who's going to step in for him. That's an interesting question. I hope there will be Republican champions for science funding.
MF: Is there too much conservatism baked into how we research new therapies and bring them to people who are sick, bench-to-bedside? I'm thinking of the criticisms that NIH or the FDA are overly bureaucratic. Are you hopeful about ARPA-H, President Biden’s proposed new agency for health innovation?
HS: I think the challenge hasn't been cracked by the federal government. Maybe DARPA has done this outside of health science, but within health science, the federal government has had limited success at funding things that can be applied quickly, while having overwhelming success at funding basic research that eventually becomes important in applications. Can they do it the other way around? They’ll need people running ARPA-H who are application first. It’s ambitious. The way it was done in Operation Warp Speed is all the money was just given to the companies. If the hypothesis on ARPA-H is for the federal government to actually do what Moderna and BioNTech did for the vaccine, themselves, that's a radical idea. It's going to require thinking very differently than the way they think about dispersing grants for basic research.
MF: You’ve written a number of bold op-eds as editor of the Science journals. Are there any op-eds you're especially proud of as voicing a view that was important but not necessarily popular?
HS: I was one of the first people to come out hard against President Trump['s handling of] the pandemic. Lots of my brothers and sisters came along afterwards. To the extent that I was able to catalyze that, I'm proud of doing it. In the last few weeks, I published a paper objecting to the splitting of the OSTP director from the science advisor and, especially, not awarding the top part of the job to Alondra Nelson, who is a distinguished scientist at black female. And instead, giving part of it to Francis Collins. He’s certainly the most important science policy figure of my lifetime, but somebody who’s been doing this now for decades. I just think we have to push as hard as we can to get a cadre of young people leading us in Washington who represent the future of the country. I think the Biden administration leaned on a lot of figures from the past. I’m pushing them hard to try to stop it.
MF: I want to circle back to the erosion of the public’s trust in experts. Most experts are specialists, and specialists operate in silos that don’t capture the complexity of scientific knowledge. Are some pushbacks to experts and concerns about the perils of specialization valid?
HS: You're on the right track there. What we need is more respect for the generalist. We can't help the fact that you have to be very specialized to do a lot of stuff. But what we need is more partnership between specialists and people who can cross fields, especially into communication and social sciences. That handoff is just not really there right now. It's hard to get a hardcore scientist to respect people who are interested in science, education and science communication, and to treat them as equals. The last two years showed that they're at least as important, if not more so.
MF: I’m grateful that you’re leading the way in this area, Holden. Thank you for sharing your thoughts and your work.
A recent study by researchers at the University of Pennsylvania examined how CAR-T therapy helped Doug Olson beat a cancer death sentence for over a decade - and how it could work for more people.
Doug Olson was 49 when he was diagnosed with chronic lymphocytic leukemia, a blood cancer that strikes 21,000 Americans annually. Although the disease kills most patients within a decade, Olson’s case progressed more slowly, and courses of mild chemotherapy kept him healthy for 13 years. Then, when he was 62, the medication stopped working. The cancer had mutated, his doctor explained, becoming resistant to standard remedies. Harsher forms of chemo might buy him a few months, but their side effects would be debilitating. It was time to consider the treatment of last resort: a bone-marrow transplant.
Olson, a scientist who developed blood-testing instruments, knew the odds. There was only a 50 percent chance that a transplant would cure him. There was a 20 percent chance that the agonizing procedure—which involves destroying the patient’s marrow with chemo and radiation, then infusing his blood with donated stem cells—would kill him. If he survived, he would face the danger of graft-versus-host disease, in which the donor’s cells attack the recipient’s tissues. To prevent it, he would have to take immunosuppressant drugs, increasing the risk of infections. He could end up with pneumonia if one of his three grandchildren caught a sniffle. “I was being pushed into a corner,” Olson recalls, “with very little room to move.”
Soon afterward, however, his doctor revealed a possible escape route. He and some colleagues at the University of Pennsylvania’s Abramson Cancer Center were starting a clinical trial, he said, and Olson—still mostly symptom-free—might be a good candidate. The experimental treatment, known as CAR-T therapy, would use genetic engineering to turn his T lymphocytes (immune cells that guard against viruses and other pathogens) into a weapon against cancer.
In September 2010, technicians took some of Olson’s T cells to a laboratory, where they were programmed with new molecular marching orders and coaxed to multiply into an army of millions. When they were ready, a nurse inserted a catheter into his neck. At the turn of a valve, his soldiers returned home, ready to do battle.
“I felt like I’d won the lottery,” Olson says. But he was only the second person in the world to receive this “living drug,” as the University of Pennsylvania investigators called it. No one knew how long his remission would last.
Three weeks later, Olson was slammed with a 102-degree fever, nausea, and chills. The treatment had triggered two dangerous complications: cytokine release syndrome, in which immune chemicals inflame the patient’s tissues, and tumor lysis syndrome, in which toxins from dying cancer cells overwhelm the kidneys. But the crisis passed quickly, and the CAR-T cells fought on. A month after the infusion, the doctor delivered astounding news: “We can’t find any cancer in your body.”
“I felt like I’d won the lottery,” Olson says. But he was only the second person in the world to receive this “living drug,” as the University of Pennsylvania investigators called it. No one knew how long his remission would last.
An Unexpected Cure
In February 2022, the same cancer researchers reported a remarkable milestone: the trial’s first two patients had survived for more than a decade. Although Olson’s predecessor—a retired corrections officer named Bill Ludwig—died of COVID-19 complications in early 2021, both men had remained cancer-free. And the modified immune cells continued to patrol their territory, ready to kill suspected tumor cells the moment they arose.
“We can now conclude that CAR-T cells can actually cure patients with leukemia,” University of Pennsylvania immunologist Carl June, who spearheaded the development of the technique, told reporters. “We thought the cells would be gone in a month or two. The fact that they’ve survived 10 years is a major surprise.”
Even before the announcement, it was clear that CAR-T therapy could win a lasting reprieve for many patients with cancers that were once a death sentence. Since the Food and Drug Administration approved June’s version (marketed as Kymriah) in 2017, the agency has greenlighted five more such treatments for various types of leukemia, lymphoma, and myeloma. “Every single day, I take care of patients who would previously have been told they had no options,” says Rayne Rouce, a pediatric hematologist/oncologist at Texas Children’s Cancer Center. “Now we not only have a treatment option for those patients, but one that could potentially be the last therapy for their cancer that they’ll ever have to receive.”

Immunologist Carl June, middle, spearheaded development of the CAR-T therapy that gave patients Bill Ludwig, left, and Doug Olson, right, a lengthy reprieve on their terminal cancer diagnoses.
Penn Medicine
Yet the CAR-T approach doesn’t help everyone. So far, it has only shown success for blood cancers—and for those, the overall remission rate is 30 to 40 percent. “When it works, it works extraordinarily well,” says Olson’s former doctor, David Porter, director of Penn’s blood and bone marrow transplant program. “It’s important to know why it works, but it’s equally important to know why it doesn’t—and how we can fix that.”
The team’s study, published in the journal Nature, offers a wealth of data on what worked for these two patients. It may also hold clues for how to make the therapy effective for more people.
Building a Better T Cell
Carl June didn’t set out to cure cancer, but his serendipitous career path—and a personal tragedy—helped him achieve insights that had eluded other researchers. In 1971, hoping to avoid combat in Vietnam, he applied to the U.S. Naval Academy in Annapolis, Maryland. June showed a knack for biology, so the Navy sent him on to Baylor College of Medicine. He fell in love with immunology during a fellowship researching malaria vaccines in Switzerland. Later, the Navy deployed him to the Fred Hutchinson Cancer Research Center in Seattle to study bone marrow transplantation.
There, June became part of the first research team to learn how to culture T cells efficiently in a lab. After moving on to the National Naval Medical Center in the ’80s, he used that knowledge to combat the newly emerging AIDS epidemic. HIV, the virus that causes the disease, invades T cells and eventually destroys them. June and his post-doc Bruce Levine developed a method to restore patients’ depleted cell populations, using tiny magnetic beads to deliver growth-stimulating proteins. Infused into the body, the new T cells effectively boosted immune function.
In 1999, after leaving the Navy, June joined the University of Pennsylvania. His wife, who’d been diagnosed with ovarian cancer, died two years later, leaving three young children. “I had not known what it was like to be on the other side of the bed,” he recalls. Watching her suffer through grueling but futile chemotherapy, followed by an unsuccessful bone-marrow transplant, he resolved to focus on finding better cancer treatments. He started with leukemia—a family of diseases in which mutant white blood cells proliferate in the marrow.
Cancer is highly skilled at slipping through the immune system’s defenses. T cells, for example, detect pathogens by latching onto them with receptors designed to recognize foreign proteins. Leukemia cells evade detection, in part, by masquerading as normal white blood cells—that is, as part of the immune system itself.
June planned to use a viral vector no one had tried before: HIV.
To June, chimeric antigen receptor (CAR) T cells looked like a promising tool for unmasking and destroying the impostors. Developed in the early ’90s, these cells could be programmed to identify a target protein, and to kill any pathogen that displayed it. To do the programming, you spliced together snippets of DNA and inserted them into a disabled virus. Next, you removed some of the patient’s T cells and infected them with the virus, which genetically hijacked its new hosts—instructing them to find and slay the patient’s particular type of cancer cells. When the T cells multiplied, their descendants carried the new genetic code. You then infused those modified cells into the patient, where they went to war against their designated enemy.
Or that’s what happened in theory. Many scientists had tried to develop therapies using CAR-T cells, but none had succeeded. Although the technique worked in lab animals, the cells either died out or lost their potency in humans.
But June had the advantage of his years nurturing T cells for AIDS patients, as well as the technology he’d developed with Levine (who’d followed him to Penn with other team members). He also planned to use a viral vector no one had tried before: HIV, which had evolved to thrive in human T cells and could be altered to avoid causing disease. By the summer of 2010, he was ready to test CAR-T therapy against chronic lymphocytic leukemia (CLL), the most common form of the disease in adults.
Three patients signed up for the trial, including Doug Olson and Bill Ludwig. A portion of each man’s T cells were reprogrammed to detect a protein found only on B lymphocytes, the type of white blood cells affected by CLL. Their genetic instructions ordered them to destroy any cell carrying the protein, known as CD19, and to multiply whenever they encountered one. This meant the patients would forfeit all their B cells, not just cancerous ones—but regular injections of gamma globulins (a cocktail of antibodies) would make up for the loss.
After being infused with the CAR-T cells, all three men suffered high fevers and potentially life-threatening inflammation, but all pulled through without lasting damage. The third patient experienced a partial remission and survived for eight months. Olson and Ludwig were cured.
Learning What Works
Since those first infusions, researchers have developed reliable ways to prevent or treat the side effects of CAR-T therapy, greatly reducing its risks. They’ve also been experimenting with combination therapies—pairing CAR-T with chemo, cancer vaccines, and immunotherapy drugs called checkpoint inhibitors—to improve its success rate. But CAR-T cells are still ineffective for at least 60 percent of blood cancer patients. And they remain in the experimental stage for solid tumors (including pancreatic cancer, mesothelioma, and glioblastoma), whose greater complexity make them harder to attack.
The new Nature study offers clues that could fuel further advances. The Penn team “profiled these cells at a level where we can almost say, ‘These are the characteristics that a T cell would need to survive 10 years,’” says Rouce, the physician at Texas Children’s Cancer Center.
One surprising finding involves how CAR-T cells change in the body over time. At first, those that Olson and Ludwig received showed the hallmarks of “killer” T-cells (also known as CD8 cells)—highly active lymphocytes bent on exterminating every tumor cell in sight. After several months, however, the population shifted toward “helper” T-cells (or CD4s), which aid in forming long-term immune memory but are normally incapable of direct aggression. Over the years, the numbers swung back and forth, until only helper cells remained. Those cells showed markers suggesting they were too exhausted to function—but in the lab, they were able not only to recognize but to destroy cancer cells.
June and his team suspect that those tired-looking helper cells had enough oomph to kill off any B cells Olson and Ludwig made, keeping the pair’s cancers permanently at bay. If so, that could prompt new approaches to selecting cells for CAR-T therapy. Maybe starting with a mix of cell types—not only CD8s, but CD4s and other varieties—would work better than using CD8s alone. Or perhaps inducing changes in cell populations at different times would help.
Another potential avenue for improvement is starting with healthier cells. Evidence from this and other trials hints that patients whose T cells are more robust to begin with respond better when their cells are used in CAR-T therapy. The Penn team recently completed a clinical trial in which CLL patients were treated with ibrutinib—a drug that enhances T-cell function—before their CAR-T cells were manufactured. The response rate, says David Porter, was “very high,” with most patients remaining cancer-free a year after being infused with the souped-up cells.
Such approaches, he adds, are essential to achieving the next phase in CAR-T therapy: “Getting it to work not just in more people, but in everybody.”

Doug Olson enjoys nature - and having a future.
Penn Medicine
To grasp what that could mean, it helps to talk with Doug Olson, who’s now 75. In the years since his infusion, he has watched his four children forge careers, and his grandkids reach their teens. He has built a business and enjoyed the rewards of semi-retirement. He’s done volunteer and advocacy work for cancer patients, run half-marathons, sailed the Caribbean, and ridden his bike along the sun-dappled roads of Silicon Valley, his current home.
And in his spare moments, he has just sat there feeling grateful. “You don’t really appreciate the effect of having a lethal disease until it’s not there anymore,” he says. “The world looks different when you have a future.”

