Technology’s Role in Feeding a Soaring Population Raises This Dilemma

When farmer Terry Wanzek walks out in his fields, he sometimes sees a grove of trees, which reminds him of his grandfather, who planted those trees. Or he looks out over the pond, which deer, ducks and pheasant use for water, and he knows that his grandfather made a decision to drain land and put the pond in that exact spot.
Growing more with fewer resources is becoming increasingly urgent as the Earth's population is expected to hit 9.1 billion by 2050.
"There is a connection that goes beyond running a business and making a profit," says Wanzek, a fourth-generation North Dakota farmer who raises spring wheat, corn, soybeans, barley, dry edible beans and sunflowers. "There is a connection to family, to your ancestors and there is a connection to your posterity and your kids."
Wanzek's corn and soybeans are genetically modified (GM) crops, which means that they have been altered at the DNA level to create desirable traits. This intervention, he says, allows him to start growing earlier and to produce more food per acre.
Growing more with fewer resources is becoming increasingly urgent as the Earth's population is expected to hit 9.1 billion by 2050, with nearly all of the rise coming from developing countries, according to the Food and Agriculture Organization of the United Nations. This population will be urban, which means they'll likely be eating fewer grains and other staple crops, and more vegetables, fruits, meat, dairy, and fish.
Whether those foods will be touched in some way by technology remains a high-stakes question. As for GM foods, the American public is somewhat skeptical: in a recent survey, about one-third of Americans report that they are actively avoiding GMOs or seek out non-GMO labels when shopping and purchasing foods. These consumers fear unsafe food and don't want biotechnologists to tamper with nature. This disconnect—between those who consume food and those who produce it—is only set to intensify as major agricultural companies work to develop further high-tech farming solutions to meet the needs of the growing population.
"I don't think we have a choice going forward. The world isn't getting smaller. We have to come up with a means of using less."
In the future, it may be possible to feed the world. But what if the world doesn't want the food?
A Short History
Genetically modified food is not new. The first such plant (the Flavr Savr tomato) was approved for human consumption and brought to market in 1994, but people didn't like the taste. Today, nine genetically modified food crops are commercially available in the United States (corn, soybean, squash, papaya, alfalfa, sugar beets, canola, potato and apples). Most were modified to increase resistance to disease or pests, or tolerance to a specific herbicide. Such crops have in fact been found to increase yields, with a recent study showing grain yield was up to 24.5 percent higher in genetically engineered corn.
Despite some consumer skepticism, many farmers don't have a problem with GM crops, says Jennie Schmidt, a farmer and registered dietician in Maryland. She says with a laugh that her farm is a "grocery store farm - we grow the ingredients you buy in products at the grocery store." Schmidt's father-in-law, who started the farm, watched the adoption of hybrid corn improve seeds in the 1930s and 1940s.
"It wasn't a difficult leap to see how well these hybrid corn seeds have done over the decades," she says. "So when the GMOs came out, it was a quicker adoption curve, because as farmers they had already been exposed to the first generation and this was just the next step."
Schmidt, for one, is excited about the gene-editing tool CRISPR and other ways biotechnologists can create food like apples or potatoes with a particular enzyme turned off so they don't go brown during oxidation. Other foods in the pipeline include disease-resistant citrus, low-gluten wheat, fungus-resistant bananas, and anti-browning mushrooms.
"We need to not judge our agriculture by yield per acre but nutrition per acre."
"I don't think we have a choice going forward," says Schmidt. "The world isn't getting smaller. We have to come up with a means of using less."
A Different Way Forward?
But others remain convinced that there are better ways to feed the planet. Andrew Kimball, executive director of the Center for Food Safety, a non-profit that promotes organic and sustainable agriculture, says the public has been sold a lie with biotech. "GMO technology is not proven as a food producer," he says. "It's just not being done anywhere at a large scale. Ninety-nine percent of GMOs are corn and soy, and they allow chemical companies to sell more chemicals. But that doesn't increase food or decrease hunger." Instead, Kimball advocates for a pivot from commodity agriculture to farms with crop diversity and animals.
Kimball also suggests a way to use land more appropriately: stop growing so much biofuel. Right now, in the U.S., more than 55 percent of our crop farmland is in corn and soy. About 40 percent of that goes into cars through ethanol, 40 percent is fed to animals and a good bit of the rest goes into high-fructose corn syrup. That leaves only a small amount to feed people, says Kimball. "If you want to feed the world, not just the U.S., you want to make sure to use that land to feed people," he says. "We need to not judge our agriculture by yield per acre but nutrition per acre."
Robert Streiffer, a bioethicist at the University of Wisconsin at Madison, agrees that GMOs haven't really helped alleviate hunger. Glyphosate resistance, one of the traits that is most commonly used in genetically engineered crops, doesn't improve yield or allow crops to be grown in areas where they weren't able to be grown before. "Insect resistance through the insertion of a Bt gene can improve yield, but is mostly used for cotton (which is not a food crop) and corn which goes to feed cattle, a very inefficient method of feeding the hungry, to say the least," he says. Important research is being done in crops such as cassava, which could help relieve global hunger. But in his opinion, these researchers lack the profit potential needed to motivate large private funding sources, so they require more public-sector funding.
"A substantial portion of public opposition is as much about the lack of any perceived benefits for the consumers as it is for outright fear of health or environmental dangers."
"Public opposition to biotech foods is certainly a factor, but I expect this will slowly decline as labels indicating the presence of GE (genetically engineered) ingredients become more common, and as we continue to amass reassuring data on the comparative environmental safety of GE crops," says Streiffer. "A substantial portion of public opposition is as much about the lack of any perceived benefits for the consumers as it is for outright fear of health or environmental dangers."
One sign that the public may be willing to embrace some non-natural foods is the recent interest in cultured meat, which is grown in a lab from animal cells but doesn't require raising or killing animals. A study published last year in PLOS One found that 65 percent of 673 surveyed U.S. individuals would probably or definitely try cultured meat, while only 8.5 percent said they definitely would not. In the future, lab-grown food may become another way to create more food with fewer resources.
Danielle Nierenberg, president of the Food Tank, a nonprofit organization focused on building a global community of safe and healthy food, points to an even more immediate problem: food waste. Globally, about a third of food is thrown out or goes bad before it has a chance to be eaten. She says simply fixing roads and infrastructure in developing countries would go a long way toward ensuring that food reaches the hungry. Focusing on helping small farmers (who grow 70 percent of food around the globe), especially female farmers, would go a long way, she says.
Innovation on the Farm
In addition to good roads, those farmers need fertilizer. Nitrogen-based fertilizers may get a boost in the future from technologies that release nutrients slowly over time, like slow-release medicines based on nanotechnology. In field trials on rice in Sri Lanka, one such nanotech fertilizer increased crop yields by 10 percent, even though it delivered only half the amount of urea compared with traditional fertilizer, according to a study last year.
"I'm not afraid of the food I grow. We live in the same environment, and I feel completely safe."
One startup, the San-Francisco-based Biome Makers, is profiling microbial DNA to give farmers an idea of what their soil needs to better support crops. Joyn Bio, another new startup based in Boston and West Sacramento, is looking to engineer microbes that could reduce farming's reliance on nitrogen fertilizer, which is expensive and harms the environment. (Full disclosure: Joyn Bio and this magazine are funded by the same company, Leaps by Bayer, though leapsmag is editorially independent. Also, Bayer recently acquired Monsanto, the leading producer of genetically engineered seeds and the herbicide Roundup.)
Terry Wanzek, the farmer in North Dakota, says he'd be willing to try any new technology as long as it helps his bottom line – and increases sustainability. "I'm not afraid of the food I grow," he says of his genetically modified produce. "We eat the same food, we live in the same environment, and I feel completely safe."
Only time will tell if people several decades from now feel the same way. But no matter how their food is produced, one thing is certain: those people will need to eat.
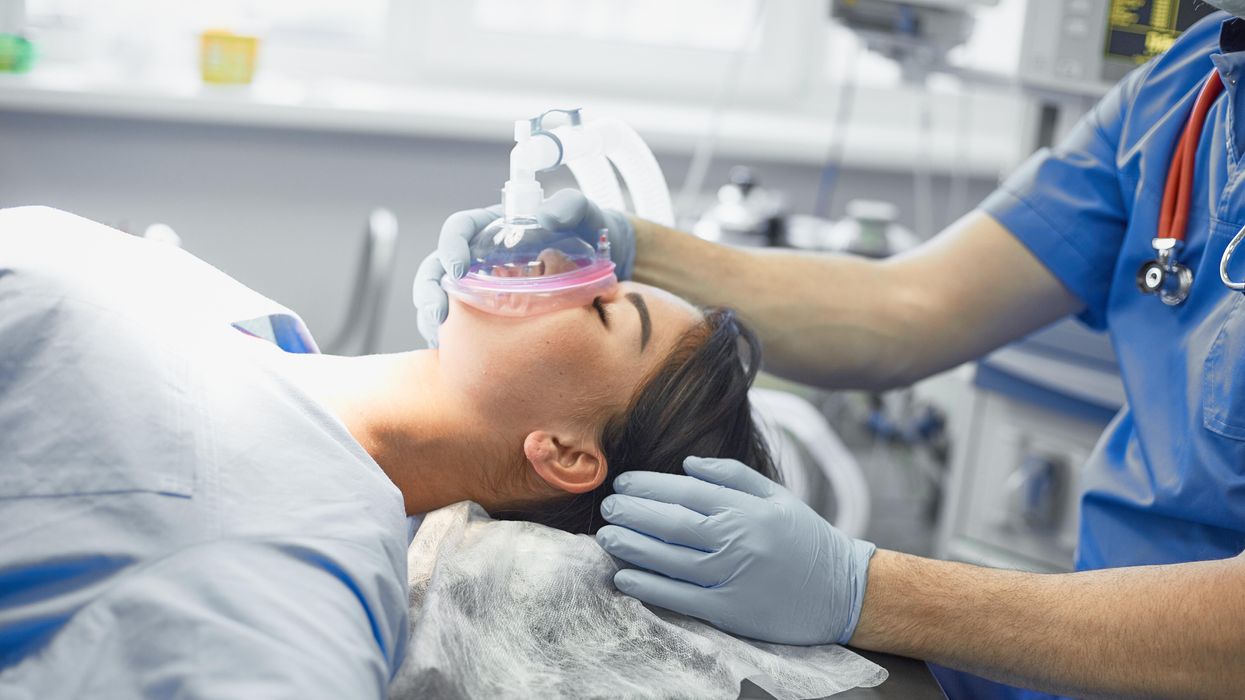
Your surgery could harm yourself and the planet. Here's what some doctors are doing about it.
Certain gases used for anesthesia are 3,000 times more damaging for the climate than CO2. Some anesthesiologists are pointing to other solutions.
This is part 1 of a three part series on a new generation of doctors leading the charge to make the health care industry more sustainable - for the benefit of their patients and the planet. Read part 2 here and part 3 here.
Susanne Koch, an anesthesiologist and neurologist, reached a pivot point when she was up to her neck in water, almost literally. The basement of her house in Berlin had flooded in the summer of 2018, when Berlin was pummeled by unusually strong rains. After she drained the house, “I wanted to dig into facts, to understand how exactly these extreme weather events are related to climate change,” she says.
Studying the scientific literature, she realized how urgent the climate crisis is, but the biggest shock was to learn that her profession contributed substantially to the problem: Inhalation gases used during medical procedures are among the most damaging greenhouse gases. Some inhalation gases are 3,000 times more damaging for the climate than CO2, Koch discovered. “Spending seven hours in the surgery room is the equivalent of driving a car for four days nonstop,” she says. Her job of helping people at Europe’s largest university hospital, the Charité in Berlin, was inadvertently damaging both the people and the planet.
“Nobody had ever even mentioned a word about that during my training,” Koch says.
On the whole, the medical sector is responsible for a disproportionally large percentage of greenhouse gas emissions, with the U.S. as the biggest culprit. According to a key paper published in 2020 in Health Affairs, the health industry “is among the most carbon-intensive service sectors in the industrialized world,” accounting for between 4.4 percent and 4.6 percent of greenhouse gas emissions. “It’s not just anesthesia but health care that has a problem,” says Jodi Sherman, anesthesiology professor and Medical Director of the Program on Healthcare Environmental Sustainability at Yale University as well as co-director of the Lancet Planetary Health Commission on Sustainable Healthcare. In the U.S., health care greenhouse gas emissions make up about 8.5 percent of domestic greenhouse gas emissions. They rose 6 percent from 2010 to 2018, to nearly 1,700 kilograms per person, more than in any other nation.
Of course, patients worry primarily about safety, not sustainability. Yet, Koch emphasizes that “as doctors, we have the responsibility to do no harm, and this includes making sure that we use resources as sustainably as possible.” Studies show that 2018 greenhouse gas and toxic air pollutant emissions resulted in the loss of 388,000 disability-adjusted life years in the U.S. alone. “Disease burden from health care pollution is of the same order of magnitude as deaths from preventable medical errors, and should be taken just as seriously,” Sherman cautions.
When Koch, the anesthesiologist, started discussing sustainable options with colleagues, the topic was immediately met with plenty of interest. Her experience is consistent with the latest representative poll of the nonprofit Foundation Health in Germany. Nine out of ten doctors were interested in urgently finding sustainable solutions for medical services but lacked knowhow and resources. For teaching purposes, Sherman and her team have developed the Yale Gassing Greener app that allows anesthesiologists to compare how much pollution they can avoid through choosing different anesthesia methods. Sherman also published professional guidelines intended to help her colleagues better understand how various methods affect carbon emissions.
Significant traces of inhalation gases have been found in Antarctica and the Himalayas, far from the vast majority of surgery rooms.
A solution espoused by both Sherman and Koch is comparatively simple: They stopped using desflurane, which is by far the most damaging of all inhalation gases to the climate. Its greenhouse effect is 2,590 times stronger than carbon dioxide. The Yale New Haven Hospital already stopped using desflurane in 2013, becoming the first known healthcare organization to eliminate a drug based on environmental grounds. Sherman points out that this resulted in saving more than $1.2 million in costs and 1,600 tons of CO2 equivalents, about the same as the exhaust from 360 passenger vehicles per year.
At the Charité, Koch claims that switching to other anesthesiology choices, such as propofol, has eliminated 90 percent of the climate gas emissions in the anesthesiology department since 2016. Young anesthesiologists are still taught to use desflurane as the standard because desflurane is absorbed less into the patients’ bodies, and they wake up faster. However, Koch who has worked as an anesthesiologist since 2006, says that with a little bit of experience, you can learn when to stop giving the propofol so it's timed just as well with a person’s wake-up process. In addition, “patients are less likely to feel nauseous after being given propofol,” Koch says. Intravenous drugs might require more skill, she adds, "but there is nothing unique to the drug desflurane that cannot be accomplished with other medications.”
Desflurane isn’t the only gas to be concerned about. Nitrous oxide is the second most damaging because it’s extremely long-lived in the environment, and it depletes the ozone layer. Climate-conscious anesthesiologists are phasing out this gas, too, or have implemented measures to decrease leaks.
Internationally, 192 governments agreed in the Kyoto protocol of 2005 to reduce halogenated hydrocarbons – resulting from inhalation gases, including desflurane and nitrous oxide – because of their immense climate-warming potential, and in 2016, they pledged to eliminate them by 2035. However, the use of inhalation anesthetics continues to increase worldwide, not least because more people access healthcare in developing countries, and because people in industrialized countries live longer and therefore need more surgeries. Significant traces of inhalation gases have been found in Antarctica and the Himalayas, far from the vast majority of surgery rooms.
Certain companies are now pushing new technology to capture inhalation gases before they are released into the atmosphere, but both Sherman and Koch believe marketing claims of 99 percent efficiency amount to greenwashing. After investigating the technology first-hand and visiting the company that is producing such filters in Germany, Koch concluded that such technology only reduces emissions by 25 percent. And Sherman believes such initiatives are akin to the fallacy of recycling plastic. In addition to questioning their efficiency, Sherman fears such technology “gives the illusion there is a magical solution that means I don’t need to change my behavior, reduce my waste and choose less harmful options.”
Financial interests are at play, too. “Desflurane is the most expensive inhalation gas, and some think, the most expensive must be the best,” Koch says. Both Koch and Sherman lament that efforts to increase sustainability in the medical sector are entirely voluntary in their countries and led by a few dedicated individual professionals while industry-wide standards and transparency are needed, a notion expressed in the American Hospital Association’s Sustainability Roadmap.

Susanne Koch, an anesthesiologist in Berlin, wants her colleagues to stop using a gas called desflurane, which is by far the most damaging of all inhalation gases to the climate.
Adobe Stock
Other countries have done more. The European Union recommends reducing inhalation gases and even contemplated a ban of desflurane, except in medical emergencies. In 2008, the National Health Service (NHS) created a Sustainable Development Unit, which measures CO2 emissions in the U.K. health sector. NHS is the first national health service that pledged to reach net zero carbon by 2040. The carbon footprint of the NHS fell by 26 percent from 1990 to 2019, mostly due to reduced use of certain inhalers and the switch to renewable energy for heat and power. “The evidence that the climate emergency is a health emergency is overwhelming,” said Nick Watts, the NHS Chief Sustainability Officer, in a press release, “with health professionals already needing to manage its symptoms.”
Sherman is a leading voice in demanding action in the U.S. To her, comprehensive solutions start with the mandatory, transparent measurement of emissions in the health sector to tackle the biggest sources of pollution. While the Biden administration highlighted its efforts to reduce these kinds of emissions during the United Nations Climate Conference (COP27) in November 2022 and U.S. delegates announced that more than 100 health care organizations signed the voluntary Health Sector Climate Pledge, with the aim to reduce emissions by 50 percent in the next eight years, Sherman is convinced that voluntary pledges are not enough. “Voluntary measures are insufficient,” she testified in congress. “The vast majority of U.S. health care organizations remain uncommitted to timely action. Those that are committed lack policies and knowledge to support necessary changes; even worse, existing policies drive inappropriate consumption of resources and pollution.”
Both Sherman and Koch look at the larger picture. “Health care organizations have an obligation to their communities to protect public health,” Sherman says. “We must lead by example. That includes setting ambitious, science-based carbon reduction targets to achieve net zero emissions before 2050. We must quantify current emissions and their sources, particularly throughout the health care supply chains.”
Have You Heard of the Best Sport for Brain Health?
In this week's Friday Five, research points to this brain healthiest of sports. Plus, the natural way to reprogram cells to a younger state, the network that could underlie many different mental illnesses, and a new test could diagnose autism in newborns. Plus, scientists 3D print an ear and attach it to woman
The Friday Five covers five stories in research that you may have missed this week. There are plenty of controversies and troubling ethical issues in science – and we get into many of them in our online magazine – but this news roundup focuses on scientific creativity and progress to give you a therapeutic dose of inspiration headed into the weekend.
Listen on Apple | Listen on Spotify | Listen on Stitcher | Listen on Amazon | Listen on Google
Here are the promising studies covered in this week's Friday Five:
- Reprogram cells to a younger state
- Pick up this sport for brain health
- Do all mental illnesses have the same underlying cause?
- New test could diagnose autism in newborns
- Scientists 3D print an ear and attach it to woman